What Is Therapeutic Apheresis?

Written and verified by the doctor Mariel Mendoza
Therapeutic apheresis is an extracorporeal circulation procedure that filters blood through a device for therapeutic purposes. Its purpose is to remove and eliminate the components considered to be responsible for a pathology, without modifying the rest of the blood substances.
It’s part of the purification procedures and, in addition, there are many therapeutic apheresis procedures that can be carried out. It’s used as a therapeutic alternative in certain diseases in which conventional treatment fails.
It’s also known as therapeutic plasma exchange, because it separates the plasma from the blood cells by filtration or centrifugation. The former is generally used.
It resembles the hemodialysis procedure, except that it’s capable of removing toxins bound to plasma proteins.
What is required?
The following is required to perform therapeutic apheresis:
- Vascular access providing high blood flow: Generally, vascular accesses similar to hemodialysis are used, such as arteriovenous fistulas or central catheters. Only in some cases can a peripheral line be used.
- Anticoagulation: with heparin or citrate.
- Continuous monitoring: When the therapeutic apheresis procedure is performed, there must be constant monitoring of the person’s vital signs. It requires trained personnel and the use of monitors.
How does therapeutic apheresis work?
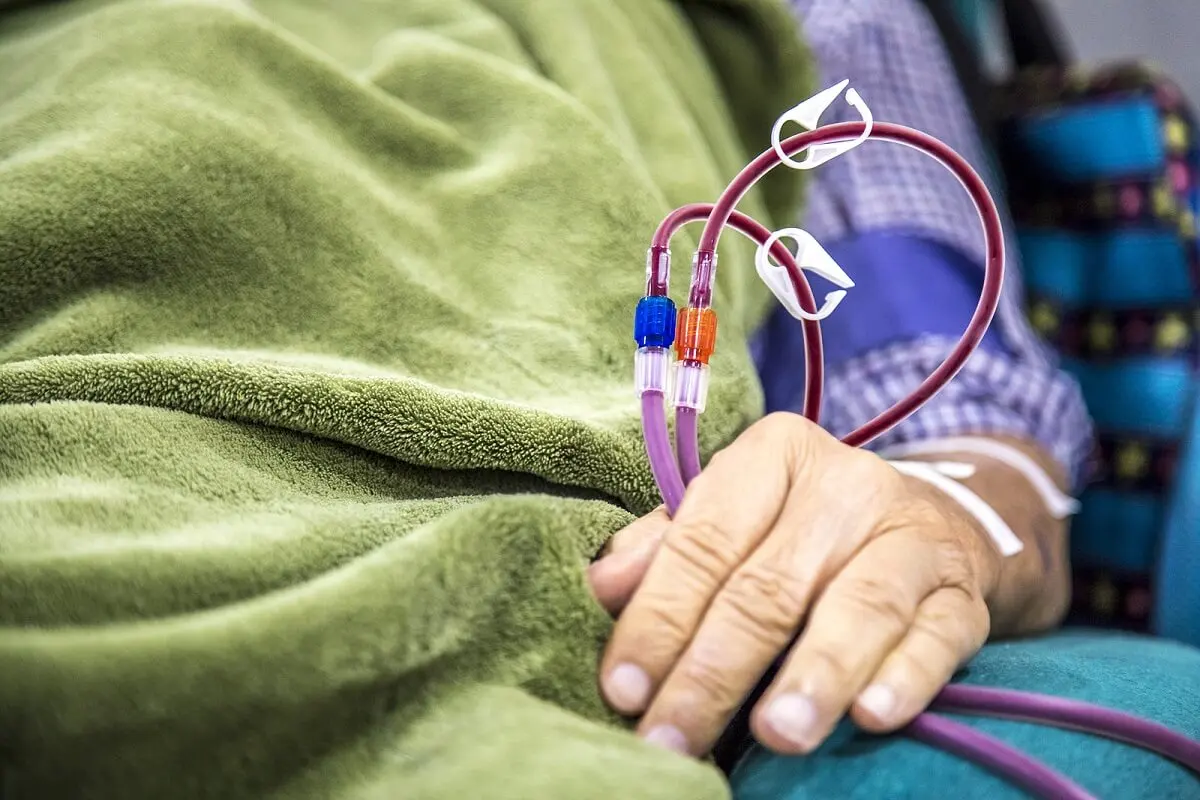
In therapeutic apheresis, two vascular accesses are used; one in and one out. This makes it possible to produce a sterile circuit that circulates the blood extracorporeally. This circuit is connected to a special device that filters the components.
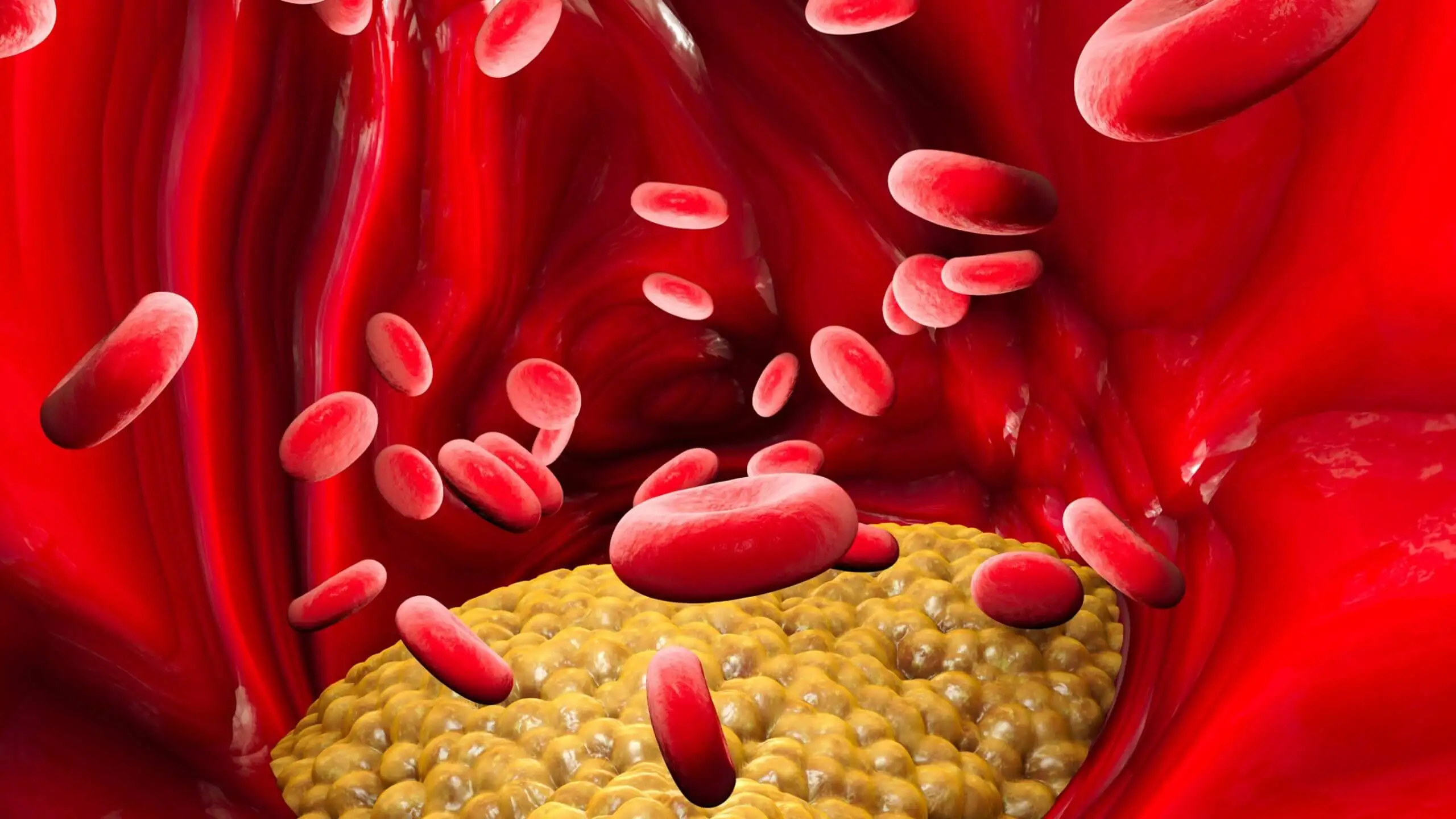
The harmful components remain in the filter, while the rest return to the person through the other vascular access. In this way, immune complexes, autoantibodies, proinflammatory cytokines, heavy metals, toxins, harmful proteins, excess cholesterol, among others, are trapped and eliminated from the blood.
Risks associated with its implementation
The risks of therapeutic apheresis are related to vascular access, anticoagulation, and the element that replaces the extracted plasma. Venous access requires the use of large caliber catheters, which sometimes result in complications such as bleeding, infections at the puncture site, thrombosis, or even pneumothorax.
In addition, anticoagulation generates a propensity to bleed and, when citrate is used, the serum ionic calcium concentration is reduced. This leads to symptoms of hypocalcemia, such as paresthesia, nausea, vomiting, a cold sensation, and cardiac arrhythmias.
On the other hand, when having to replace the extracted plasma with a replacement solution, in order to maintain volume and oncotic pressure, two solutions are usually used: fresh frozen plasma or 5% albumin. This doesn’t replace the immunoglobulins, which makes them prone to infection.
Transfusion reactions with fever and allergy may also occur.
Considering that a large volume of circulating plasma is removed during plasma exchange, hypotension related to hypovolemia may occur. As well as other symptoms of hypoperfusion, such as dizziness, distal coldness or tachycardia.
Find out more here: Symptoms of Hypocalcemia and its Treatment
Indications for therapeutic apheresis
Therapeutic apheresis is used to treat those pathologies that have the following characteristics:
- They’re caused by a pathogenic component found in the blood.
- This pathogenic component can be eliminated efficiently.
- The elimination of the pathogenic component is faster than the production of the pathogen.
- Removal or decrease of the pathogenic component in the blood resolves or improves symptoms.
In addition, although most of the time its indications are of an acute type, in some cases its periodic implementation is needed. It’s recommended in conditions such as the following:
- Familial hypercholesterolemia
- Cryoglobulinemia
- Multiple myeloma
- Waldenström’s macroglobulinemia
- Guillain Barré syndrome
- Raynaud’s disease
- Poisonous or drug intoxication
- Multiple sclerosis
- Lyme disease.
- Antibody-mediated organ transplant rejection
- Idiopathic thrombocytopenic purpura
Find our more about: What Are the Normal Values of Leukocytes?
There are different types of therapeutic apheresis
The main therapeutic apheresis treatments are plasmapheresis and cytapheresis. However, they aren’t the only ones, as the following are also included:
- Immunoadsorption: an antibody or antigen is removed from plasma by combining with another
- Double filtration
- Plasmadsorption
- Hemoadsorption
- Photoapheresis: immunomodulatory therapy in which mononuclear cells are treated with photoactivatable drugs and then activated with ultraviolet light
- Rheapheresis
- LDL-apheresis: selective removal of low-density lipoprotein
- DALI: selective absorption of lipoproteins from the blood through ligands
- MARS: removal of albumin-bound substances
- Prometheus: removal of albumin-bound toxins
Plasmapheresis is the most common and separates plasma components from blood cells. On the other hand, cytapheresis lowers the specific blood cell count by removing white cells (leukocytapheresis), platelets (thrombocytapheresis), or red blood cells (erythroapheresis).
An excellent alternative
Therapeutic apheresis is a therapeutic alternative in various diseases in which conventional treatment has failed. It’s considered suitable as long as it’s capable of eliminating the harmful component at a faster rate than that produced by the body.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Anaya F. Por qué la aféresis terapéutica debe pertenecer a la especialidad de nefrología. Nefrología (Madr.) 2011; 31(4):379-381. Disponible en http://scielo.isciii.es/scielo.php?script=sci_arttext&pid=S0211-69952011000400001&lng=es
- Medina M. Aféresis terapéutica. Recambio plasmático terapéutico. Citaféresis. Rev Med Inst Mex Seguro Soc 2005;43(1):47-52. Disponible en https://www.redalyc.org/pdf/4577/457745546013.pdf.
- Rodríguez E, et al. Aféresis Terapéutica en Patología Renal. Nefrología al día 2020. Disponible en https://www.nefrologiaaldia.org/es-articulo-aferesis-terapeutica-patologia-renal-219.
- Schwartz J, et al. Guías sobre el uso de la Aféresis Terapéutica en la práctica clínica – enfoque basado en la evidencia del Comité de Redacción de la Sociedad Americana de Aféresis: Sexta Edición Especial. Revista de Aféresis Clínica 2013;28. Disponible en https://www.ammtac.org/docs/articulos/Guia%20ASFA%202013%20Espanol.pdf.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








