What Is a Dental Fistula and How Can It Be Treated?

Written and verified by the dentist Vanesa Evangelina Buffa
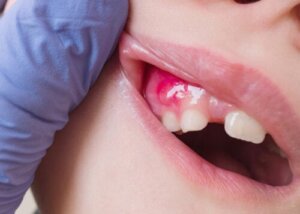
If you notice a reddened area or a lump in the gum with pus coming out, you most likely have a dental fistula. This condition is infectious in origin and requires immediate dental treatment.
A dental fistula is a fairly common condition. But sometimes it can go unnoticed.
In this article, we’ll tell you what this oral condition is and why it occurs. We also detail the treatments available to solve the problem. Read on and find out more.
What is a dental fistula?
A dental fistula is an abnormal drainage pathway that the body creates to release the contents of an internal infection to the outside. It’s usually a small channel that passes through the bone and makes its way over the surface of the gums or palate.
Therefore, the presence of a dental fistula in the mouth is an indication of an infectious process. It’s a duct that links a dental abscess with the outside.
It’s worth clarifying that a dental abscess is a collection of pus in the vicinity of a tooth. This process develops as a consequence of a bacterial infection in the dental or periodontal tissues. Its most common location is in the area of the roots or on the sides of the teeth.
Dental fistulas try to move the putrefied contents of the abscesses to the outside. And in this way, they prevent the infectious material from continuing to accumulate inside the jaws.
Therefore, the outflow of pus into the mouth is one of the characteristic signs of this phenomenon. However, it isn’t the only one. We’ll explain it in more detail below.
Symptoms of a dental fistula
When a dental fistula appears in the mouth, it may be accompanied by pain. It’s a sharp and penetrating discomfort in the affected area.
However, the outflow of pus can actually become a relief for the patient. The drainage releases internal pressures and this can reduce the pain associated with abscesses. And there are even cases where the person may not feel anything and the process goes unnoticed.
Another manifestation of a dental fistula is inflammation and redness of the tissue where it’s located. It usually appears on the gum, on the sides of the affected tooth or on the palate. Although, in more severe cases, it can be observed on the skin of the face.
In some cases, the area may increase in volume and form a lump that then bursts and begins to ooze. Or a small whitish or yellowish, pimple-like spot may be seen on the gum. Pus will come out of it.
In addition, it’s common for the patient to have a bitter taste in the mouth. Another symptomatology that may accompany dental fistulas is sensitivity or pain in the affected tooth and in other areas of the face, neck, or ear.
The lymph nodes in the neck and jaw may also enlarge (adenomegaly), the face may swell and fever may occur. And, in the most severe cases, the patient may have difficulty speaking, swallowing, and breathing.
In the face of these manifestations, it’s important to see a doctor urgently. They indicate the complication of the infection and could endanger the patient’s life.

Find out about 7 Symptoms that Signal a Dental Infection
Causes
As we’ve already mentioned, the cause of a dental fistula is an infectious process in the tooth that starts with a dental abscess. However, this bacterial colonization can be due to different situations:
- Deep caries: This is the most frequent cause. The bacteria that cause cavities and destroy the tooth reach the pulp. This causes the death and infection of the nerve.
- Periodontal disease: Periodontitis not treated in a timely manner can cause a dental abscess on the supporting tissues of the tooth.
- Poorly performed root canals or defective fillings: If a cavity hasn’t been properly treated or a root canal has failed, bacteria can take its course and cause a dental fistula.
- Wisdom teeth: Third molars or wisdom teeth are the last teeth to erupt and they do so in adulthood. Many times, their eruption is associated with complications, such as difficulty in cleaning them, bad position, lack of space and retention of the tooth. With these issues, infections are common and therefore, the appearance of fistulas is also common.
- Trauma: Blows to the teeth can cause cracks or fractures through which bacteria can enter. Traumatisms can also cause the rupture of the vascular nerve bundle of the tooth, depriving it of irrigation. With this, the pulp dies and becomes easily infected.
Diagnosis of a dental fistula
The diagnosis of a dental fistula is usually made through an oral examination and oral radiographs. During the inspection, erythema and swelling of the gum can be observed in the mouth, as well as the presence of a point that exudes pus.
Sometimes the patient has pain when touching the area. In addition, when pressing, more pus usually comes out into the mouth.
X-rays can be taken to visualize the area of the abscessed tooth, its size, and the nearby structures involved.
Often, when the cause of the infection is doubtful, a dentist will use a test called a fistulography. This allows them to find out where the dental fistula comes from.
It consists of probing and placing a radiopaque material inside the canal until it stops. Then an X-ray is taken to observe the place where it reaches and thus define the origin of the problem.
From the exhaustive study of the case, the dentist can reach a precise diagnosis. Based on this, he/she will plan the most appropriate treatment.
Find out more: Dental Curettage: Procedure, Results and Care
Treatment of a dental fistula
In order to solve a dental fistula problem, it’s necessary to eliminate the infection that causes it. In order to do this, as we have already mentioned, it’s important to make a correct diagnosis that allows us to know the extent and seriousness of the matter.
Going to see a dentist is fundamental. Without treatment, the fistula won’t heal by itself. Moreover, the risk of the infection that causes it to spread to the jaws and other parts of the mouth and body increases.
To treat the infection, the dentist prescribes antibiotics that act systemically on the germs. But, in addition, local treatment inside the mouth will be necessary. These procedures will resolve the cause of the problem.
The choice of approach will depend on the size of the infection, the parts of the mouth involved, the degree of tooth destruction, and the long-term prognosis. These are the usual procedures to treat a dental fistula:
- Endodontics or root canal retreatment: This is the most conservative treatment and the first choice if the case allows it. The inside of the teeth is cleaned, the infected material is removed and the element is sealed, without having to remove it.
- Periodontal treatment: If the cause of the dental fistula is periodontitis, root curettage will be necessary to eliminate and treat the problem.
- Exodontia: When the dental damage is very extensive, or the abscess has spread to important areas, then tooth extraction may be the solution. When the problematic tooth is removed, a curettage and a deep cleaning of the area is also performed to remove all the infected material present. Rehabilitation with dentures or implants will then be necessary to restore function and aesthetics to the mouth.
Once the infection has been eliminated with any of the procedures we mentioned, the tissues regenerate and recover. Thus, after a few days, the gum will return to normal and the fistula will no longer exist.
However, some appointments will be necessary to monitor how the situation evolves. The dentist will decide whether it’s necessary to plan further treatment.
Home remedies
There are some measures that can be practiced at home to help to reduce the symptoms of dental fistulas. Especially if there’s discomfort.
However, this doesn’t replace definitive treatment. It will always be necessary to go to the dentist to solve the cause of the condition.
These are some of the methods that you can implement at home until you receive the corresponding dental care, as well as after the treatment has been carried out:
- Apply a cold compress on the cheek near the abscess, especially if there’s pain. This is also helpful once the corresponding treatment has been received in order to reduce inflammation and promote recovery.
- Consult the dentist to take an over-the-counter pain reliever.
- Rinse your mouth with warm water and salt.
- Avoid tobacco, alcohol and hot, acidic or spicy foods to prevent irritation of the area.
- Rinse with an antiseptic mouthwash if recommended by the dentist.
- Take the medication prescribed by the dentist, respecting the schedules and completing the entire medication plan.
Even if the dental fistula is caused by a bacterial infection, you should never take antibiotics without a prescription. You should know that depending on the situation, the dentist will choose the medication that best suits your needs.
Self-medicating is dangerous and can complicate future evolution.
Prevent the problem
Having a dental fistula in the mouth is an indication of an infection somewhere deeper. And, even though the body will be working to fight against more serious complications, these are still a possibility.
As we told you, when faced with this problem, it’s essential to receive dental treatment as soon as possible. It’s also important to realize that dental fistulas can be prevented. And, by taking certain precautions, you’ll prevent the discomfort and risks of this condition and the need to undergo uncomfortable and expensive treatments.
The best way to prevent abscesses and dental fistulas is to take care of your oral health responsibly. Oral hygiene by brushing teeth, gums, and your tongue after every meal for at least 2 minutes is one of the habits to sustain. It’s also of utmost importance to floss daily and to complement the cleaning with fluoride toothpastes and mouthwashes.
Taking care of your diet and avoiding very sweet foods, ultra-processed foods, and carbonated beverages will help you control harmful bacteria. Eating healthy and varied foods will bring health to the tissues of the mouth and the rest of your body.
In addition, visiting the dentist every 6 months completes your oral care. The dentist is an ally when it comes to taking care of your oral health.
Now that you know what a dental fistula is, why it appears and how it’s treated, you’ll surely want to prevent this problem. With simple, consistent care, you’ll be able to forget about infections in your mouth!
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Melo, S. L., Da Silva, T. T., de Sousa Lima, S., & Salomão, M. B. (2022). TRATAMENTO ENDODÔNTICO COM PRESENÇA DE FÍSTULA-REVISÃO DE LITERATURA. Revista Cathedral, 4(1), 71-84.
- Luque-Luna, M., Alamon-Reig, F., & Morgado-Carrasco, D. (2022). Odontogenic Fistula. JAMA dermatology.
- Silva, F. A., de Sousa Santos, K., & de Vasconcelos Neves, G. (2018). O rastreamento de fistula como recurso diagnóstico no tratamento endodôntico. ARCHIVES OF HEALTH INVESTIGATION, 7.
- Pérez Gorrín, A. (2019). Microbiología de los abscesos dentales.
- Alcántara-Ramírez, V. D., Gutiérrez-Ayala, D., Gutiérrez-Ávila, S. A., & Arenas, R. (2022). Odontogenic Fistula. Cutaneous Manifestation of an Odontologic Disease. Dermatología Cosmética, Médica y Quirúrgica, 19(4), 345-347.
- Rimoldi, M. A., Gubiani, M. L., Boldrini, M. P., Pinardi, B. A., & Juarez, R. (2021). Fístula cutánea odontogénica: a propósito de un caso. Revista argentina de dermatología, 102(1), 76-82.
- Domínguez Domínguez, L. (2020). Prescripción de antibióticos en endodoncia por odontólogos generales.
- Jiménez, J. C. C., & Esqueda, G. P. A. Cirugía endodóntica apical.
- González, E. E. M., Rodríguez, H. P. C., & Llamas, M. B. 26. Relación endodoncia y periodoncia. principios básicos de endodoncia clínica, 283.
- Vera Medina, M. M. (2020). Valoración de éxitos y fracasos en endodoncia (Bachelor’s thesis).
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








