Dental Curettage: Procedure, Results and Care

Written and verified by the dentist Vanesa Evangelina Buffa
Gingivitis and periodontitis, along with cavities, are one of the most common oral problems in the adult population. Dental curettage is one of the treatments used to resolve conditions in the supporting tissues.
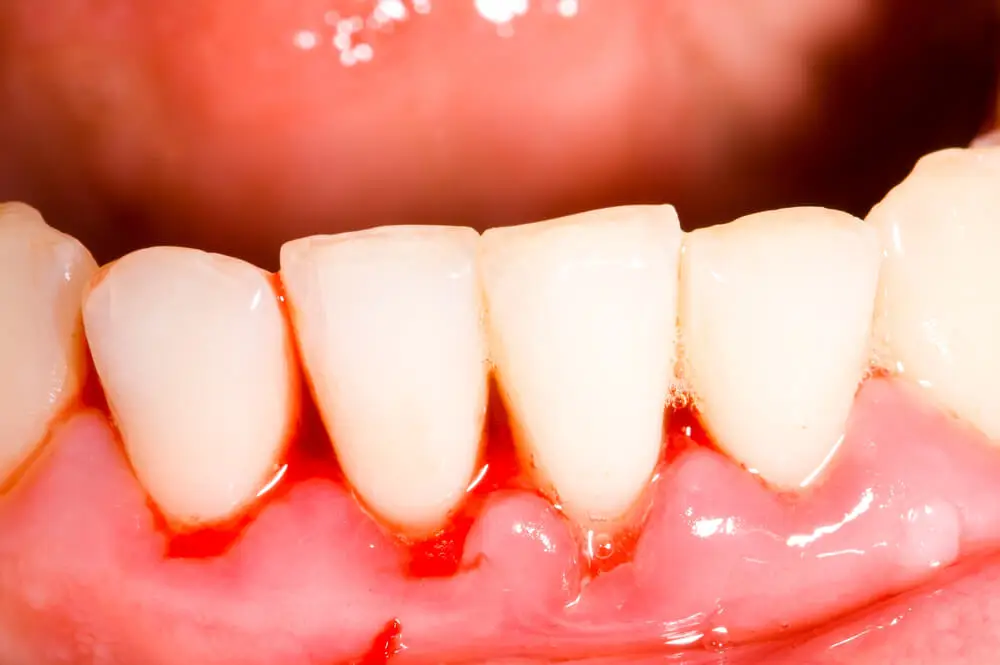
When gums become red, swollen, bleeding, and tender, it indicates a problem in the oral cavity. Seeking professional help immediately to resolve the situation will prevent more serious complications.
For if gingivitis isn’t treated in time it can progress to pyorrhea or periodontitis. Here, the damage to the tissues that support the teeth is more severe. This is why tooth mobility and even tooth loss is a possibility that should be avoided at all costs.
When dealing with periodontal problems, the dentist may recommend dental curettage. In this article, we’ll explain what this treatment consists of and what care should be taken once it has been performed.
What is dental curettage?
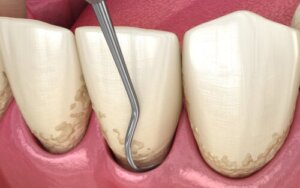
Dental curettage is a dental treatment performed to treat gingivitis and periodontitis problems. It consists of scaling, polishing, and smoothing the roots and periodontal pockets to remove deposits of tartar, bacteria, and inflammatory tissue accumulated under the gums.
When bacterial plaque isn’t adequately removed with dental hygiene, it accumulates on and under the gums. These deposits calcify and harden with the minerals present in the mouth, becoming tartar.
The accumulation of tartar and bacteria between the root and the gum gives rise to periodontal pockets. This situation is very characteristic of pyorrhea. The gingival margin is displaced and pockets are formed that retain more debris, making the situation worse and worse.
Dental curettage allows adequate cleaning of the areas that are inaccessible to toothbrushing. By removing debris and inflamed areas and leaving a smooth root surface, tissue recovery is promoted.
This technique can be performed by a trained general dentist or a periodontist. The latter are professionals specialized in the approach and treatment of the tissues that support the teeth.
When is dental curettage performed?
As we have already mentioned, dental curettage is used to treat problems in the supporting tissues. But it isn’t always necessary.
In cases of mild gingivitis, when periodontal pockets aren’t yet present, home care and professional cleaning are usually sufficient. On the other hand, when there’s periodontitis with a lot of accumulated tartar, deep pockets, and loss of bone tissue, dental curettage will be appropriate.
Even in the most severe cases, this technique is combined with special surgery to restore the patient’s periodontal health. It will be the dentist who’ll determine the need for a dental curettage.
Obvious symptoms
Some obvious symptoms may make you suspect that something is wrong with the periodontal tissues. These are manifestations you should pay attention to, and, if they appear, seek immediate professional help:
- Red, swollen, sensitive gums that bleed easily
- Tartar on teeth and gums
- Bad breath and a bad taste in the mouth
- Pus coming out between teeth and gingival tissue
- Tooth mobility
When you visit the dentist, the professional will do a thorough oral examination, look for the presence of pockets and measure their depth; likewise, he will check for tooth mobility. In addition, x-rays will be taken to observe the degree of bone involvement.
From this evaluation, the dentist will arrive at an accurate diagnosis of the problem and plan the best treatment accordingly. Dental curettage will be necessary when the damage can’t be reversed with conventional professional cleaning.
Find out more: Black Spots on Your Gums: Causes and Treatments
How is dental curettage performed?
Dental curettage seeks to eliminate bacterial plaque and tartar accumulations deposited in the periodontal tissues. It acts on deep and sensitive areas such as the gingival pocket and the dental root. For this reason, anesthesia is necessary before starting the treatment.
It’s performed in the dental clinic in one or several sessions, depending on the needs of each case. It’s usually performed by dividing the mouth into quadrants to clean all the sectors in order. Once the area has been desensitized, the treatment is divided into two stages.
1. Root scaling
The first part of the procedure begins with the scaling of the dental roots to remove bacterial plaque and tartar. This can be done manually, with ultrasonic instruments, or with a combination of both techniques:
- Manual: Curettes are used, which are thin instruments specially designed to efficiently access the affected area. They’re used to scrape the roots and dislodge adhering tartar in a controlled and precise manner.
- Ultrasonic: Sonic or ultrasonic devices are used to clean the area quickly through vibrations.
The combination of both techniques achieves a better finish. In general, it isn’t necessary to detach the gum in order to scrape the roots. But some more serious cases may require surgical separation of the gingival tissue in order to access the deep pockets better.
In addition, a microbiological analysis of tartar and plaque is performed at this stage. This allows the bacteria that cause the problem to be identified so that the appropriate antibiotic can be used.
2. Smoothing and polishing of the teeth
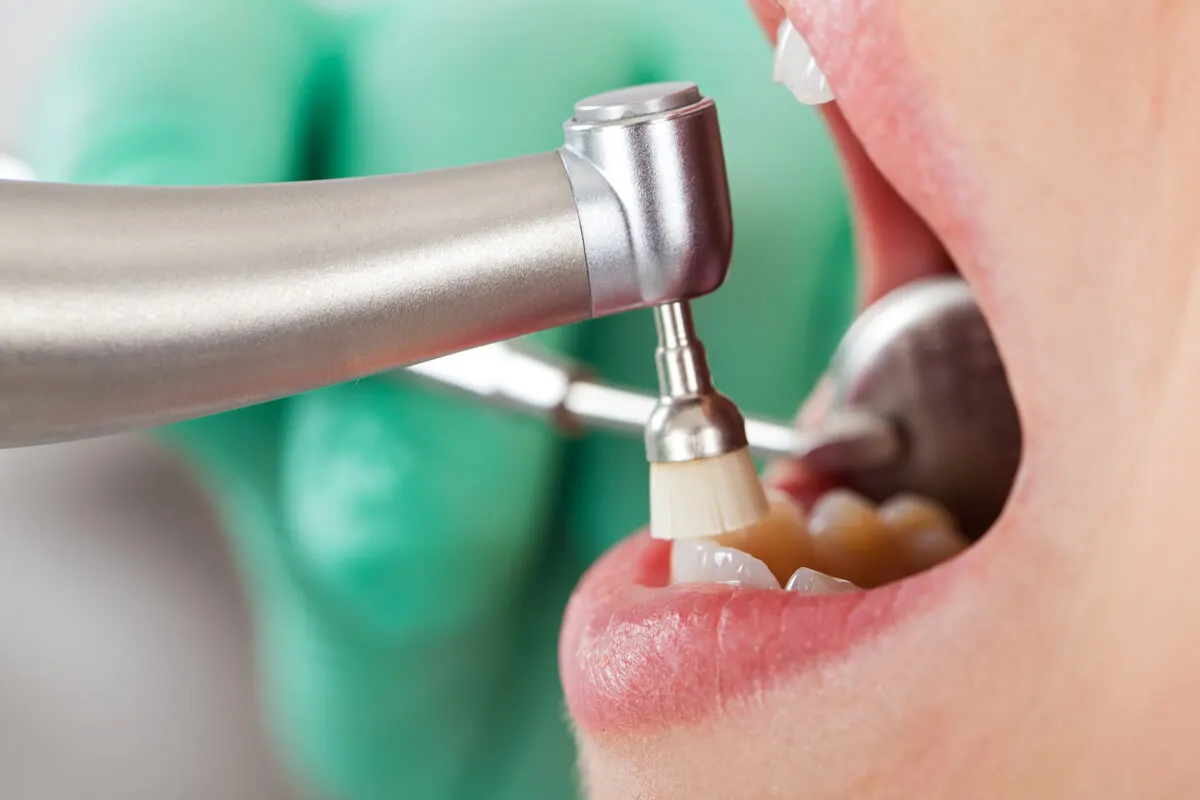
Once the roots have been scaled and all the debris present on and under the gums has been removed, the teeth are smoothed and polished. For this, rotary instruments with special brushes and pastes are used to remove pigments and irregularities from the tooth surfaces.
In this way, the teeth are left smooth and shiny. The aim is to eliminate all areas that may favor the retention of bacterial plaque and thus the reappearance of the problem.
At the end of the treatment, the periodontist will recommend certain hygienic measures to the patient, and what they need to carry out at home. He/she will also prescribe antibiotics, anti-inflammatory and antiseptic rinses specific for each case.
Every so often, the condition of the mouth should be reevaluated and maintenance treatments should be carried out. In this way, the results obtained are sustained, and relapses, complications, and the rapid accumulation of bacterial plaque are avoided.
Results of dental curettage
After dental curettage, the periodontal tissues will need some time to recover. For this reason, it’s common for the area to be tender and sore for a few days after the treatment.
Sensitivity to hot and cold foods and slight bleeding, especially on contact or during tooth brushing, is also common. The area where the dental curettage has been performed may look swollen and red for a few days, until the inflammation subsides.
The use of anti-inflammatory drugs recommended by the professional will be of great help in these cases. They’ll reduce discomfort and promote recovery.
With this treatment, the supporting tissues will recover, the inflammation will disappear and the teeth will be able to remain in the mouth. In addition, other systemic complications associated with periodontal disease will be prevented.
Discover more here: The Link Between Osteoporosis and Dental Health
How often are dental curettages performed?
Dental curettage treatment, as already mentioned, may require several sessions. Especially if the damage is severe, the pockets are deep, and a large part of the mouth is affected.
To avoid the patient’s discomfort, in these cases, the professional prefers to work by sector. The patient will be seen several times to complete the treatment in stages.
But once the whole process has been completed and the dental curettage has been completed in all the affected areas, new revisions will be necessary. The dentist will say how often to return for maintenance appointments. In general, these will be every 4 or 6 months, depending on the complexity of each case.
In these periodontal check-ups, the specialist will evaluate the condition of the mouth and will eliminate any new foci of bacterial plaque and tartar that have formed. They will especially focus on specific areas that tend to accumulate bacteria.
Thus, with regular check-ups and cleaning sessions, periodontal health can be maintained with simpler and less invasive therapies, thus avoiding having to repeat the dental curettage in the whole mouth.
If you don’t have the necessary aftercare, then periodontitis will reappear. That’s why scheduled visits to the dentist shouldn’t be postponed or suspended.
What are the differences between dental curettage and professional cleaning?
Both professional cleaning and dental curettage aim to remove plaque and tartar and improve periodontal health. However, they aren’t the same procedure.
Dental cleaning is a less invasive therapy that focuses on removing pigments, stains, plaque, and tartar accumulated on tooth surfaces. This is all above the gum line, in the visible area of the teeth.
It’s a preventive treatment that’s performed to control bacterial plaque and avoid complications. This is performed in almost all patients. In general, one or two dental cleanings a year are recommended, depending on the patient’s gingival health and oral hygiene.
On the other hand, as we have already mentioned, dental curettage is different because it involves cleaning deeper places, in what is called the subgingival area. Bacterial plaque and tartar deposited in the internal area of the gum are removed and the root of the tooth is reached. This is a more invasive procedure and, as we mentioned, it requires the use of anesthesia.
Dental curettage is a corrective treatment that’s only applied to patients suffering from periodontal problems. In this case, it’s the solution to a condition that is already present.
Dental curettage aftercare
Once dental curettage has been performed and the anesthesia has worn off, the patient can return to his or her daily activities without any problem. As we have already told you, there may be slight bleeding and minor discomfort that will diminish as the days go by.
In any case, some special care procedures will ensure that the tissues operated on recover better, more quickly, and that they don’t become infected again:
- Medication: The dentist will tell you if you need to take anti-inflammatory drugs, analgesics, and antibiotics. It’s essential to respect what’s prescribed in order to avoid complications.
- Oral hygiene: Toothbrushing should be done gently, but you shouldn’t stop doing it. It may produce slight bleeding that will disappear as the gums become swollen.
- Taking care of the diet: In the days following the intervention, hard and very hot foods should be avoided. Fresh, soft, and easy-to-chew foods are preferable.
- Do not smoke: Smoking is one of the worst enemies of periodontal tissue. You should avoid this habit. If you can’t do this, you should at least avoid smoking in the first 48 hours following the curettage.
- Pay attention to the symptoms: We have already told you what can happen after a dental curettage. If you notice that something isn’t going well during the recovery time, if your mouth swells, if the pain doesn’t subside with medication, or if there’s constant bleeding, then consult your dentist immediately.
Dental curettage can be prevented
Dental curettage is a simple intervention that’s performed under anesthesia and isn’t painful. However, it’s a procedure that’s carried out because there’s a potentially serious, or already serious, condition in the mouth.
Bacterial plaque and tartar, deep pockets, bone loss, and tooth mobility can be prevented with certain basic care tips.
To maintain healthy teeth, it’s essential to take care of dental hygiene responsibly. Daily brushing should be carried out three times a day for 2 minutes.
A soft bristle brush should be used to ensure cleanliness at the junction of the gum and teeth and all sides of all the teeth. You should also include tongue hygiene.
Daily flossing is also essential. This allows the removal of bacterial plaque that accumulates between the teeth, where brushing cannot reach. Toothpaste with fluoride and mouthwashes should be included to complement your mouth hygiene.
Dietary care is also very important. A healthy and balanced diet helps to maintain strong teeth and gums. In addition, smoking should be avoided. As we told you, this habit is very harmful for oral health and for the whole body in general.
Finally, don’t forget that, when it comes to taking care of your oral health, the dentist is your great ally. Visiting the dentist regularly, every 6 months, helps to detect any problem that may appear in time.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Mosquera Tacuri, M. J. (2019). Tratamiento de bolsas periodontales con raspado y alisado radicular campo abierto (Bachelor’s thesis, Universidad de Guayaquil. Facultad Piloto de Odontología).
- Herrera Mamani, J. N. (2021). Efecto de la terapia de raspado y alisado radicular sobre la hipersensibilidad dentaria en pacientes atendidos en un Centro Odontológico de la ciudad de Moquegua, 2020.
- Huamán Huamán, G. G. (2018). FRECUENCIA DE HIPERSENSIBILIDAD DENTINARIA POSTERIOR AL RASPADO Y ALISADO RADICULAR EN PACIENTES TRATADOS EN LA CLINICA ODONTOLOGICA DE LA UNIVERSIDAD NORBERT WIENER-2016-I.
- Pérez, A. J. S. (2008). Gingivectomia y curetaje gingival. Labor dental clínica: Avances clínicos en odontoestomatología, 9(1), 24-28.
- Pinargote, B. R., Bajaña, L. C., & Mera, D. V. (2020). EFICACIA DE LA TETRACICLINA COMO COADYUVANTE EN LA TERAPIA DE RASPADO Y ALISADO RADICULAR EN PACIENTE CON PERIODONTITIS CRÓNICA. REPORTE DE CASO. Revista Científica Especialidades Odontológicas UG, 3(2).
- Díaz-Caballero, A. J., Rivera-Peñates, D. M., & Anaya-Guzmán, L. I. (2022). Factores etiológicos de abscesos periodontales: Una patología emergente. Informe de tres casos. Universidad Y Salud, 24(2), 205-211.
- Cantos, V., & Steward, I. (2021). Diferencias clínicas en el tratamiento periodontal con y sin el uso de clorhexidina. Revisión sistemática.
- Bascones Martínez, A., Matesanz Pérez, P., & Escribano Bermejo, M. (2007). Análisis de la eficacia de la terapia antibiótica coadyuvante en el tratamiento básico de la periodontitis crónica en pacientes fumadores. Avances en Periodoncia e Implantología Oral, 19(1), 29-38.
- Delgado, J., & Ayo, A. M. (2021). Revisión sistemática de la utilización de clorhidrato de minociclina, Arestin®, como coadyuvante en pacientes periodontales durante el tratamiento periodontal (Doctoral dissertation, Santo Domingo: Universidad Iberoamericana (UNIBE)).
- Rodríguez Pulido, J. I., Martínez Sandoval, G., Garza Enríquez, M., Chapa Arizpe, M. G., Nakagoshi Cepeda, M. A. A., & Nakagoshi Cepeda, S. E. (2019). Acondicionamiento radicular en el tratamiento periodontal no quirúrgico y quirúrgico. Revista ADM, 76(5), 278-281.
- Peña, MARTA., Vaamonde, CANÒLICH., Vilarrasa, JAVI., Vallés, CRISTINA., Pascual, ANDRÉS., Shapira, LIOR, & Nart, JOSÉ (2018). Diagnóstico y tratamiento de las enfermedades periodontales: de lo imposible a lo posible. Revista científica de la Sociedad Española de Periodoncia, 4(11), 11-22.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








