The Dental Nerve and Toothaches: Causes and Treatments


Written and verified by the dentist Vanesa Evangelina Buffa
Toothaches can have their origin in the dental nerve. That annoying and irritable sensation that can make us desperate and take away our sleep arises in the deepest part of the dental pieces.
The dental pieces are formed by hard tissues that are found in the external area of the crown and the root. Inside, in the center of the teeth, is the pulp, which is what we know as the dental nerve. This soft area, which has nerve endings and blood vessels, is responsible for toothaches.
When the pulp becomes inflamed or infected, the person will feel sensitivity or pain in their teeth. That is why it’s necessary to receive treatment as soon as possible and resolve the situation. This is not only because of the discomfort and the alteration in the sufferer’s quality of life, but also because of the possibility of developing dangerous complications.
There are several factors that can lead to the dental nerve causing toothache. In this article, we’ll tell you about the most frequent causes and the possible treatments that can resolve this annoying situation.
The dental nerve: Responsible for toothaches
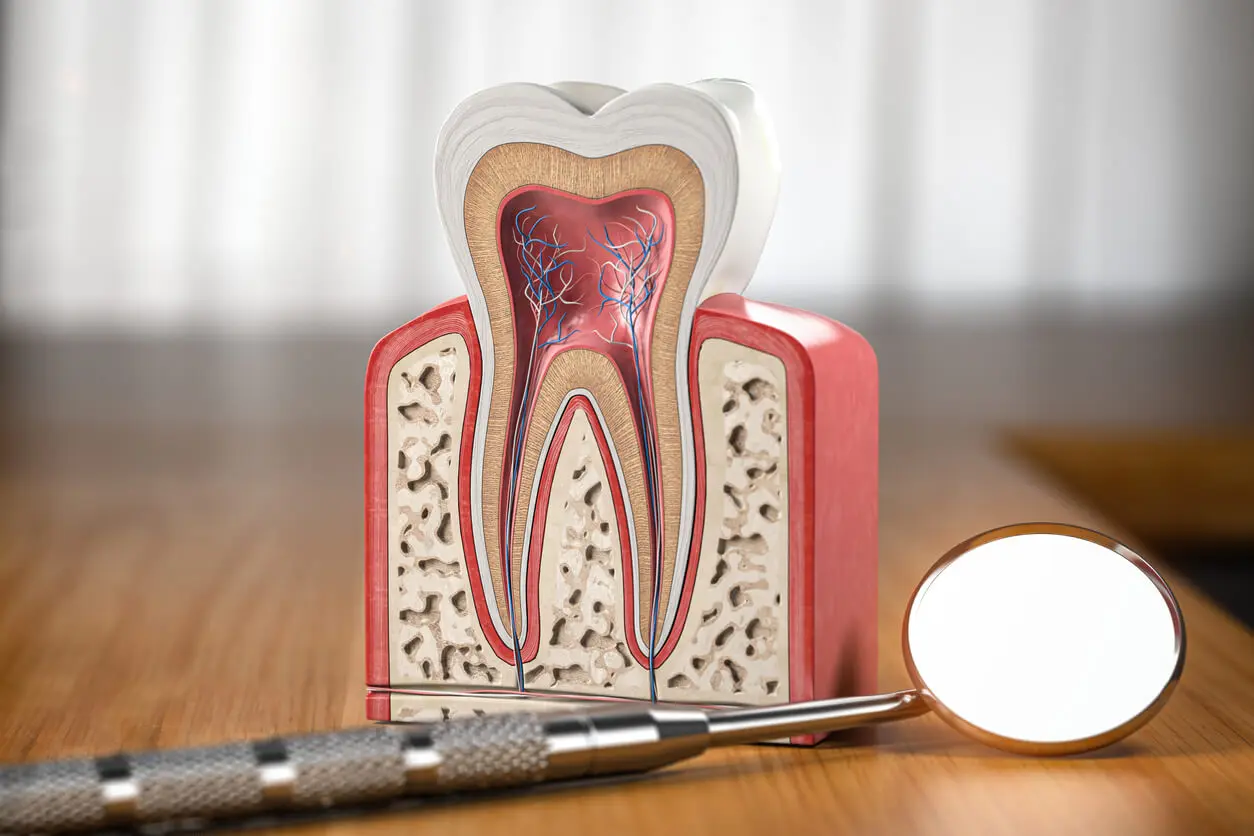
As we’ve already mentioned, what we know colloquially as the dental nerve is what anatomically corresponds to the pulp of the tooth. It is the soft tissue found in the innermost part of the teeth.
It consists of an area of connective tissue containing specialized cells, blood vessels, and nerve endings. The latter are responsible for the painful sensations we feel in the teeth when there’s a problem.
The dental pulp is contained and, therefore, surrounded by hard walls. The nerve is surrounded by dentin and then by the enamel in the crown, followed by cementum in the dental root. The strongest tissues protect the inner area of the teeth.
Dentin has thousands of microtubules inside it that connect it to the pulp. Thus, as wel’l tell you later in this article, when the dentin is unprotected and exposed, the nerve endings inside the tooth can be stimulated by external factors and cause pain.
We think you may also enjoy reading this article: How to Easily Whiten Your Teeth with Natural Products
How does a toothache occur?
In healthy teeth, the enamel and dentin protect the dental pulp and thus prevent discomfort. However, when these outer layers are affected by various alterations, the dental nerve is compromised, and a toothache appears.
The destruction of the enamel by blows, cavities, wear, or erosion leaves the dentin exposed. The presence of microscopic tubules inside the dentin is responsible for the fact that some external factors can stimulate the dental nerve and cause sensitivity and toothaches. Certain chemical substances, temperature changes, and even pressure can lead to this uncomfortable sensation.
If the destruction is greater and involves the dentin, bacteria reach the pulp, or harmful stimuli are prolonged over time, the pulp will react with an inflammatory process. This is what we know as pulpitis.
As in all cases of inflammation, increased vascularization and exudates lead to a tendency for the tissue to swell. However, as the pulp is enclosed in a hard cavity, it can’t do this. So, a lot of pressure is generated inside the tooth. This causes toothache and progresses to an infection of the dental nerve.
Infection of the dental nerve leads to the death of the pulp and the production of pus. These waste substances also exert pressure on the hard tissues and cause pain. They can even spread to other nearby sectors, forming dental abscesses.
Types of pulpitis
You should know that there are two types of pulpitis: reversible and irreversible. This is important at the time of diagnosis, as it will determine the therapy your dentist will recommend.
Reversible pulpitis is one in which the inflammation is mild and the pulp remains healthy enough to be saved. With the appropriate treatments, the vitality of the tooth can be maintained.
On the other hand, irreversible pulpitis is one in which the inflammation is very severe, the pain is intense, and prolonged. Therefore, the pulp cannot be preserved. This type of condition can progress to an infection of the nerve and cause dental abscesses.
Causes
We’ve already told you that a toothache is often caused by damage to the dental nerve. However, there are several situations that can lead to pulp damage. Here are some of them:
- Cavities: This is a loss of enamel and dentin that exposes the deepest area of the tooth. In this case, bacteria, thermal, and chemical changes irritate, inflame, and infect the pulp.
- Trauma: A blow to a tooth can break it, leaving dentin or even the pulp exposed. Trauma can also injure the vascular bundle of the tooth. Without blood supply, the nerve becomes necrotic and more susceptible to infections.
- Tooth wear and tear: Certain harmful habits can wear away the protective layer of enamel and expose the underlying dentin. Bruxism is the most obvious example. Frequent biting on objects can also cause this type of injury.
- Gingivitis and periodontal disease: The bacteria that cause lesions in the supporting tissues of the teeth can reach the pulp area through the periodontium. This causes inflammation and infection of the dental nerve and toothache. In these cases, it’s necessary to treat both conditions.
- Gingival recession: If the gums are located in a more apical area, they leave part of the root exposed, and this causes the tooth to hurt. The gingival tissue can be retracted by gingivitis or by very traumatic tooth brushing.
- Fillings: The placement of a new filling can cause sensitivity and toothaches. Deep cleaning and the use of certain chemicals during treatment irritate the pulp. Old and large fillings can deteriorate over time and have leaks through which bacteria and external agents affect the dental nerve.
- Erosion: This is the loss of enamel due to the action of chemical substances. Carbonated beverages, acidic foods, and the use of tooth whitening products can cause this type of damage.
The characteristics of a toothache due to damage to the dental nerve
When the origin of the toothache is in the dental nerve, the intensity of the discomfort will vary according to the condition that’s causing it. The sensitivity caused by reversible pulpitis isn’t the same as the pain generated by an irreversible process or infection.
In the stage in which the pulp damage is still mild, the pain is usually characterized by being acute and temporary. It’s common for patients to report sensitivity when eating something cold, hot, or sweet.
If pulpitis isn’t treated in time, the inflammation continues and causes more intense, throbbing, and constant radiating pain. The person then often reports that the discomfort intensifies when lying down and with hot foods; on the contrary, cold may alleviate the situation.
When the nerve becomes infected and a periapical abscess is generated, the pain increases when biting and touching the area near the tooth. In the mouth, swelling and redness of the gum and nearby areas may also appear. In these cases, a fever, swollen lymph nodes, bad breath and bad taste in the mouth may also appear.
Diagnosis
When a person has a toothache, the best idea is to go immediately to the dentist. The professional will perform a series of examinations and tests that will allow him/her to know what the problem is. Based on this, they’re be able to choose the appropriate therapy.
The dentist will examine the teeth to determine the type of condition that’s affecting the tooth. He/she will also take one or more X-rays.
In addition, in these cases, it’s common to perform a tooth sensitivity test. It consists of taking hot and cold stimuli to the tooth to observe its response.
Percussion is performed on the teeth using a light, blunt instrument, such as a mirror handle. The crown of the affected element is tapped horizontally and vertically.
Treatments for toothache due to problems in the dental nerve
When treating the dental nerve and resolving toothache, diagnosis is fundamental. The treatment chosen depends on the state of the pulp and the severity of the process.
Fillings and pulp protection
If the toothache is caused by cavities or a simple fracture and the dental nerve is healthy, a filling is the most common solution. It consists of cleaning the diseased area and then filling the cavity with a filling. In this way, the dentin and pulp will no longer have contact with the outside.
In cases where the inflammation is mild and the damage is reversible, special materials can be used in the deep areas to help the pulp recover.
The dentist will proceed in the same way as with fillings, removing the cavities and cleaning the diseased area. Then, before obturation, they place medicinal substances that favor nerve recovery.
If the pulp has not been exposed, an indirect pulp protection is usually performed, placing a special filling on the deep dentin. Then, the rest of the cavity is filled with a temporary material or a filling, depending on the case.
In cases of trauma, if there’s a small and aseptic exposure of the pulp, a direct pulp protection can be performed. In this case, the paste is placed directly on the nerve. Then, the dentist will also likely proceed just like the indirect technique.
Endodontics
If the damage to the dental nerve is more severe, endodontic treatments will be necessary. That is, it will be necessary to use procedures that clean the internal area of the teeth.
In general, endodontics consist of extracting the damaged nerve, cleaning the area, and sealing it with special materials. The techniques vary according to the type of damage, whether it’s a temporary or permanent tooth, and in the latter case, whether it’s completely formed or not.
Thus, in children, pulpotomies or pulpectomies can be performed. The dentist will fill them with special pastes that can be reabsorbed by the permanent teeth when they develop.
In cases of damaged permanent teeth that haven’t finished developing their roots, dentists may use apexification treatments. The inside of the teeth will be cleaned and periodically filled with pastes that stimulate root closure. Another alternative is revascularization, which attempts to regenerate the necrotic pulp so that it can finish forming the root.
Finally, in adults with fully developed teeth, the procedure is the classic root canal treatment. The dentist removes the damaged nerve, cleans and disinfects the inside of the tooth, and fills it with a biocompatible material that seals the cavity.
We think you may be interested in reading this, too: Mouth Piercing Could Have Oral Health Consequences
Exodontia
If the tooth is badly destroyed and can’t be reconstructed, or the infection is very severe, the dentist may decide to extract the tooth. In this case, after the exodontia, it will be necessary to rehabilitate the function and esthetics of the mouth with a prosthesis or an implant.
How to relieve the pain
The best way to eliminate a toothache caused by dental nerve damage is to go to the dentist. APart from the treatment that the professional deems appropriate, there are some other immediate measures that would help.
Maintaining proper oral hygiene and avoiding sweet, very cold, and hot foods is a good strategy to avoid discomfort.
The professional may indicate the use of anti-inflammatory drugs to relieve pain and symptoms of pulpitis. In addition, in the case of infection, antibiotics will be necessary to reverse the problem and soothe the symptoms. Warm salt water rinses are also often helpful.
In the case of adult patients, drainage is a very common dental practice, especially in emergency consultations. It consists of anesthetizing the patient and making a cavity in the tooth until it reaches the nerve. This way, the pressure caused by inflammation or infection can be relieved.
It’s important not to self-medicate and not to let time pass with this type of mouth problem. Infections can spread to other parts of the body and lead to serious complications such as Ludwig’s angina or septicemia.
Prevent dental nerve damage and toothaches
Dental nerve damage and the resulting toothache can be prevented with simple preventive measures. Maintaining proper oral hygiene through proper brushing and using fluoride toothpaste and floss every day will prevent many of the common problems that can destroy your teeth.
Eating a balanced diet, protecting your teeth when playing sports, and using splints if you suffer from bruxism are also of utmost importance. Finally, last but not least, don’t forget check-ups and professional cleanings with your dentist every 6 months. With this simple habit, you’ll be able to enjoy your smile and prevent discomfort in your mouth.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Simancas-Escorcia, V. H. (2019). Fisiopatología de los odontoblastos: una revisión. Duazary, 16(3), 87-103.
- Alva, M. A. C., Santos, A. A. C., & Moreira, A. C. (2018). Sensibilidad dentaria: causas y tratamiento. Revista Mexicana de Estomatología, 5(1), 65-67.
- Valladarez Olvera, E. N. (2021). Sensibilidad dental post-tratamiento aclarante: revisión sistemática.
- Belén, E., & Medina, G. (2020). Factores asociados a la sensibilidad dental en procedimientos de aclaramiento vital (Bachelor’s thesis, Universidad Nacional de Chimborazo).
- Pérez Ruiz, A. O., Roseñada Cepero, R., Grau León, I., & González Ramos, R. M. (2005). Interpretación fisiopatológica de los diferentes estadios de una pulpitis. Revista Cubana de Estomatología, 42(2), 0-0.
- Muñiz López, K. I. (2021). Protectores pulpares directos e indirectos (Bachelor’s thesis, Universidad de Guayaquil. Facultad Piloto de Odontología).
- Montoya Chalen, K. V. (2021). Materiales biocerámicos como protección pulpar (Bachelor’s thesis, Universidad de Guayaquil. Facultad Piloto de Odontología).
- Centeno, J. E. O., & Hernández, D. G. (2020). Pulpotomia o Pulpectomia: Éxito clínico y radiográfico en dientes temporales. Revista de Salud Pública, 24(3), 8-17.
- Cabrera Merlo, A. (2021). Apicoformación con plasma rico en plaquetas: reporte de un caso.
- Yáñez Pérez, E. (2020). Tratamiento en dientes con ápice inmaduro. Revascularización vs apicoformación.
- Troilo, L., Kohan, M., Chinen, M., & Santángelo, G. V. (2020). Nuevas tendencias en técnicas de apicoformación utilizando biomateriales. In IV Jornadas de Actualización en Prácticas Odontológicas Integradas PPS-SEPOI (La Plata, 7 de julio de 2020).
- Martínez-González, J. M., & Dorado, C. B. (2019). Tratamiento de las infecciones odontógenas. Donado. Cirugía bucal: Patología y técnica, 293.
- Sorrel Medina, G. F. (2018). Drenaje en endodoncia: revisión sistemática (Doctoral dissertation, Universidad del Desarrollo. Facultad de Ciencias de la Salud).
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








