Treatments for Vascular Lesions

Written and verified by the dermatologist Maria del Carmen Hernandez
Nowadays, laser technology is the gold standard for the treatment of vascular lesions. Practices such as sclerotherapy, which consists of injecting a solution into the affected blood vessel, used to be the treatment of choice for these lesions.
Sclerotherapy post-treatment requires more post-treatment care than a laser session. Are you interested in learning more? Below, we’ll talk about the benefits of laser treatment for different skin conditions.
The causes of vascular lesions
Almost everyone has some type of spot on their skin. These lesions can be either vascular or pigmented. They’re caused by the accumulation of blood vessels that are, in turn, caused by various factors, such as the following:
- Sun damage
- Skin aging
- The intake of some type of medicine
- Pregnancy
- Congenital causes
You should also read: How to Make a Garlic and Lemon Ointment for Varicose Veins
How do lasers work to treat vascular lesions?
Vascular lasers have helped patients improve their quality of life, as they’re non-ablative and outpatient treatments.
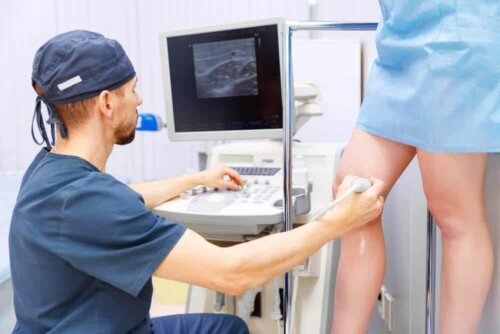
Laser technology is based on the principle of precise heating and subsequent closure of blood vessels. The transformation of the energy that caused the absorption of the light the laser emitted produces this heat.
It helps treat these types of injuries in a precise and safe way by reducing or eliminating them, without damaging the surrounding tissue. It may take several months to completely remove the lesion. This depends on the size and extent of the vascular condition, and the number of blood vessels treated.
Vascular lesions that can be treated
- Port wine stains
- Telangiectasias
- Hemangiomas
- Erythema
- Poikiloderma of civatte
- Venous lakes
- Ruby nevus
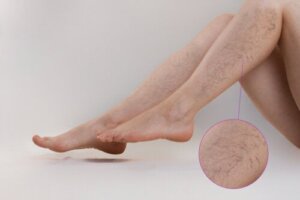
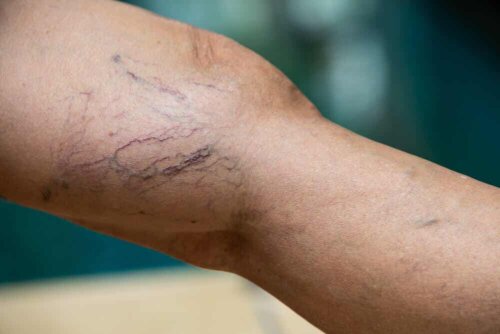
Vascular lesions, varicose veins, or spider veins, which occur mainly in the lower limbs, are common conditions in adults. They’re more prevalent in women and, for aesthetic reasons, they tend to consult medical professionals for their removal.
Read on to learn more: How to Make an Ointment to Reduce Spider Veins
The main advantages of using laser
- Firstly, it’s a non-surgical, minimally invasive treatment. This means that it doesn’t require direct contact with the area to be treated.
- Secondly, it’s very fast, as they’re 30-minute sessions.
- Safe and effective for this common aesthetic problem.
- It doesn’t incapacitate the patient to carry out their usual tasks and they can even put on makeup.
- The patient doesn’t need to apply compression bandages on the treated area.
- The entire leg or body can be treated in one session.
- It has a low risk of hypopigmentation, as it interferes very little with melanin.
Does it have any side effects?
Although it usually doesn’t have complications, the most common side effects are usually first and second-degree burns, which disappear without leaving any scars in about one to two weeks.
Hemosiderotic pigmentations will require more time and sessions to disappear completely.
After the session, edema or erythema can appear on the skin due to the intervention. Both disappear in a short period of time.
Is the treatment painful?
The patient may feel mild discomfort during the procedure. However, if the medical professional applies topical anesthesia to the area, they may eliminate this discomfort.
Post-session recommendations
- Firstly, the patient should wait 3 to 4 weeks to get the treatment if they’ve been exposed to the sun in recent days.
- It’s best not to wear overly tight clothes.
- Don’t expose yourself to very hot showers, swimming pools, stoves, or saunas and don’t exercise in the hours prior to the procedure. This will prevent vasodilation.
- Don’t expose yourself to the sun. If you do, use a high sun protection factor until the area of the treated lesion recovers its normal tone. Experts also advise against exposing the treated skin to the sun without proper photoprotection during the first summer after the treatment.
It should be noted that it isn’t a definitive treatment in itself as, if you maintain bad habits, have a genetic predisposition, or lead a sedentary lifestyle, among other factors, it’s very likely that you’ll get new vascular lesions.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Jahnke MN. Vascular Lesions. Pediatr Ann. 2016;45(8):e299‐e305. doi:10.3928/19382359-20160720-08
-
Astner S, Anderson RR. Treating vascular lesions. Dermatol Ther. 2005;18(3):267‐281. doi:10.1111/j.1529-8019.2005.05025.x
- Elluru RG. Cutaneous vascular lesions. Facial Plast Surg Clin North Am. 2013;21(1):111‐126. doi:10.1016/j.fsc.2012.11.001
-
Railan D, Parlette EC, Uebelhoer NS, Rohrer TE. Laser treatment of vascular lesions. Clin Dermatol. 2006;24(1):8‐15. doi:10.1016/j.clindermatol.2005.10.026
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








