Transdermal Patches: Characteristics and Uses

Transdermal patches have their origins in medicines that, since ancient times, people have applied through the skin. Liniments, plasters, and ointments were already used in ancient Greece, as a means of administering different medications.
In the 19th century, the idea emerged that the skin was impenetrable for certain medicines. Scientists held to this idea until the 20th century, when they proved that it was possible to administer various drugs through the skin. In time, they developed these so-called transdermal patches, and they proved to be very functional.
Transdermal patches are part of the so-called “Controlled Release Therapeutic Systems“. They’re based on a principle postulated by John Urquhart, creator of the first skin patch. According to him, the therapeutic efficacy of a substance doesn’t depend on the dose. Rather, it depends on the speed and degree of its absorption.
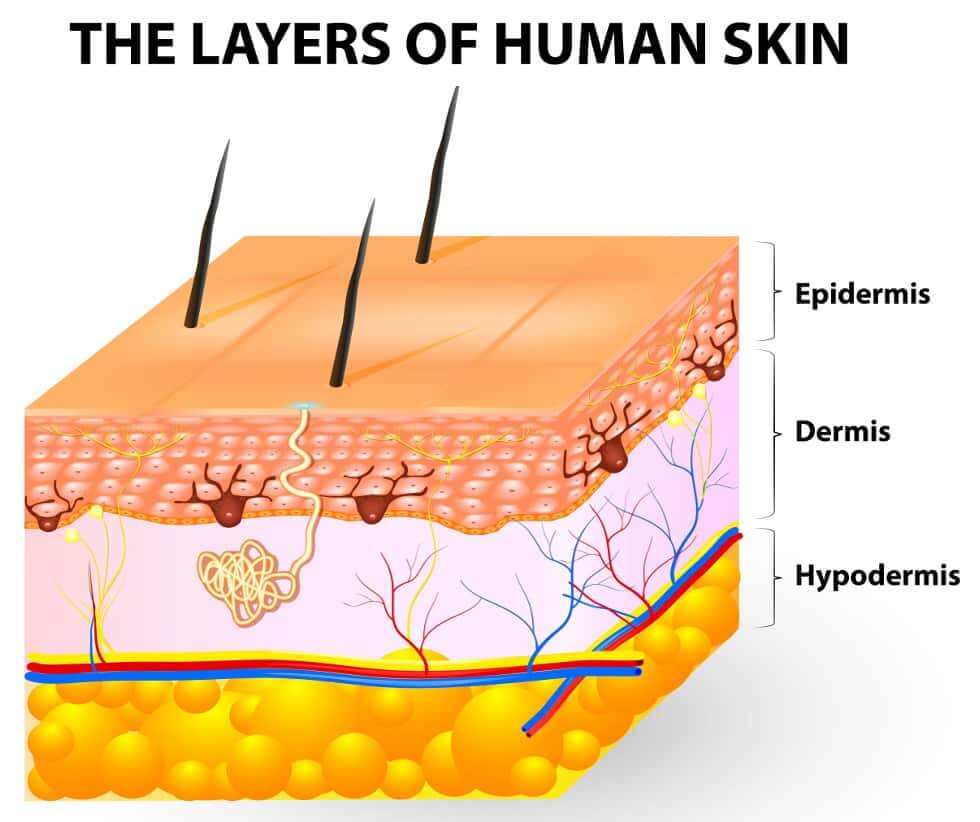
What are transdermal patches?
Transdermal patches are a way of administering medications. They attach to the skin with an adhesive and then release a drug continuously, ensuring that the skin absorbs it correctly. What we mean here is that it goes through the successive layers of skin, until it finally reaches the blood.
To administer a drug through the skin, it must have certain characteristics. The molecules that compose it must be lipophilic (that is, capable of being transported in lipids), and have a low molecular weight.
Likewise, they must have great pharmacological strength. This is because the body will only be able to absorb a small amount of product through the transdermal patches. At most, 10 milligrams per day.
Read also: Skin Memory: What You Should Know
Characteristics and use
Transdermal patches comprise four parts:
- A waterproof covering sheet
- A matrix or reservoir of the active ingredient, which houses the drug
- An adhesive
- A plastic sheet that doctors will remove before applying the patch
Some patches differ from others, mainly in the way the drug is stored and the way it’s released. Thus, there are basically three types of transdermal patches:
- Reservoir systems. The patch disperses the active ingredient through another substance and then releases it through a membrane. There are patches made of polypropylene, ethylene-vinyl-acetate copolymer, and also non-porous membrane.
- Matrix systems. The active ingredient is in a matrix and has a diffusing action, without the aid of a semi-permeable membrane.
- Mixed systems. These combine the two previous types.
Uses of transdermal patches
Currently, doctors can treat several diseases, symptoms, and problems by using transdermal patches. Among them, different types of pain, tobacco addiction, Alzheimer’s disease, Parkinson’s disease, and also several other applications.
Overall, the most commonly administered active ingredients in patch form are:
- Nitroglycerin. Mainly to prevent angina.
- Fentanyl and Buprenorphine. Doctors use these opiates for analgesic purposes.
- Nicotine. To help overcome addiction to tobacco.
- Ethinylestradiol + Norelgestromine. For contraceptive purposes.
- Estradiol, norethisterone. Used as a hormonal treatment during menopause.
- Testosterone. To treat the effects of surgical menopause.
- Rotigotine. For the treatment of Parkinson’s.
- Rivastigmine. For the treatment of Alzheimer’s disease.
Also, there are several transdermal patches for cosmetic purposes. Among them, we can find body fat reducers, skin tighteners, and anti-cellulite.
Here’s another interesting article for you: Prevent Cellulite and Get Firmer Skin: 11 Habits
Other information of interest
The Food and Drug Administration (FDA) has warned us about drugs that require special caution when administered transdermally. These are mainly contraceptives, opioid analgesics, and also rivastigmine.
Overall, the main advantages of these patches are:
- They facilitate the administration of drugs to people who have difficulty taking them orally.
- They offer more constant and sustained levels of the drug in the blood.
- Also, by using them, we prevent the metabolization of the drug through the liver, thus limiting several different potential side effects.
- Sometimes, they allow for a reduction in the frequency of administration and also improve compliance with the dosage.
Overall, the main disadvantage of these patches is that they sometimes produce an allergic reaction on the skin. Likewise, when an adverse reaction appears, it takes longer to disappear. They can also be aesthetically uncomfortable and are doctors are only able to use them with a small group of drugs.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Allevato, M. A. (2007). Sistemas terapéuticos transdérmicos. Act Terap Dermatol, 30, 154-165.
- Miyahira Yataco, C. S., Herrero Ballestar, J. V., & Tudela, L. L. (2011). Indicaciones de los parches transdérmicos de los derivados opioides. FMC Formacion Medica Continuada En Atencion Primaria. https://doi.org/10.1016/S1134-2072(11)70014-7
- Schulmeister, L. (2014). Parches transdérmicos: Medicamentos con músculo. Nursing (Ed. Española). https://doi.org/10.1016/s0212-5382(06)71019-6
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








