Red Spots on the Skin: 25 Possible Causes and Treatments

Reviewed and approved by the nurse Leidy Mora Molina
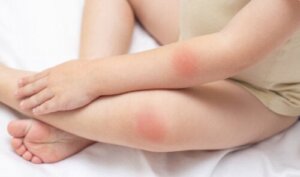
Occasionally, red spots appear on the skin. These can be caused by a wide variety of factors. These range from allergic reactions to medications or contact with certain substances to temporary illnesses.
They’re not always a symptom to worry about. In fact, sometimes they disappear on their own. Nevertheless, sometimes they do require treatment for an underlying condition.
What do red spots on the skin look like?
The skin is not only the largest organ of the body, but it’s also exposed to the outside world. In this sense, it constitutes the first and main protective barrier.
Because of this, it’s extremely sensitive to any changes, both those related to stimuli coming from the outside, as well as those of the body itself, for physiological or even emotional reasons. In fact, there’s a strong relationship between the skin and emotions.
In response to such changes, it tends to show or manifest various reactions. The appearance of red spots on the skin is one of the common responses to environmental or body transformations.
There’s great variety in terms of red spots; different shades, extensions, zones or locations, durations, or permanence of the same on the skin. Some present with bumps, changes in texture, itching, or pain.
We think you may be interested in reading this, too: 5 Tips to Protect the Skin Against the Effects of Air Conditioning
The possible causes of red spots on the skin
The reasons why red spots appear on the skin are not necessarily serious. However, it’s important to know what these causes are, in order to recognize how we should act.
1. Heat rash
In the case of a heat rash, the sweat glands are blocked. In addition to redness, small bumps usually appear. Itching is also experienced.
Heat rash usually appears where there are creases, such as the:
- Underarms
- Groin
- Neck
- Buttocks
This is not serious and subsides on its own in a few days. Just keep the area cool, dry, and free of irritating elements.
Some home treatments for rashes can also be applied, such as chamomile baths, oatmeal, or aloe vera creams, and cold compresses. However, it may be related to fungi, mites, or contact with irritating substances. In these cases, antihistamines, antibiotics, or antifungals may be prescribed.
2. Pityriasis
Pityriasis rosea is another form of a rash. It’s most common in adolescents and young adults.
This type of rash is characterized by a large red spot, accompanied by smaller ring-shaped spots. It may be on the chest, torso, or back.
These red spots are scaly and itchy. In addition, other symptoms such as headache, sore throat, and fever often occur.
The exact cause is not known. Experts think it may be related to viruses or bacteria, as it often occurs after an infection.
Sometimes it goes away in a few weeks. Sometimes corticosteroids, antihistamines, or antivirals are recommended to help with the symptoms.
3. Contact dermatitis
Contact dermatitis is a fairly common set of skin conditions. It’s caused by grabbing, touching, or rubbing against something that is irritating or allergic to the person. The skin often becomes dry, cracked, and scaly.
In some cases, it may disappear on its own within a few days or weeks, especially if contact with the offending substance is avoided. The treatment is symptomatic plus some hydrocortisone creams.

4. Atopic dermatitis
Atopic dermatitis, also known as atopic dermatitis or eczema, is a disease of the skin. Eczema is a relatively common disease. It’s characterized by the presence of red patches on the skin, accompanied by itching.
The causes are genetic in origin. Atopic dermatitis conditions the skin, in the sense that it can’t protect itself well from certain conditions, making it more sensitive and prone to irritation.
There is no cure. Treatment consists of steroid creams or ointments to relieve itching and burning. Oral antihistamines are also recommended, as well as keeping the skin well hydrated.
5. Psoriasis
Psoriasis is a chronic autoimmune disorder. In this disease, the body overproduces skin cells, which accumulate, forming layers that flake off.
Medications are available to help relieve symptoms. These include creams and immunosuppressive drugs. Ultraviolet light therapy is also available.
Also, certain factors (stress, medications, infections) help trigger flare-ups.
6. Rosacea
Rosacea is a dermatological disease of genetic origin that’s more common in white women. Reddened areas appear on the skin of the face and blood vessels become visible. There are also often outbreaks of pimples with pus and there is a burning sensation and eye irritation.
Treatments are aimed at reducing the symptoms. On the other hand, it’s recommended to avoid factors that enhance rosacea:
- Hot or alcoholic beverages
- Spicy food
- Very high or low temperatures
- Excessive sun or wind
- Medications that cause vasodilation
- Irritating cosmetic products
7. Ringworm
Ringworm or tinea corporis is a fairly common infection caused by fungi that colonize the skin. It produces lesions that are evident in the form of red spots. There’s also scaling.
It’s not painful or serious. However, it is contagious and can affect a person’s quality of life. It usually subsides with ointment treatment.
8. Allergic reactions
A large number of people suffer from allergic reactions to some element (called an allergen). There can be food, respiratory, and skin allergies.
Although the latter is less frequent, allergic reactions usually involve the appearance of red spots. In addition to being treated with antihistamines, they can be prevented by avoiding exposure.
9. Reactions to a medication or drug
There are some drugs that cause, as a side effect, the appearance of red spots on the skin. These may be raised or flat, scaly or blistered. They also vary in tone from scarlet to purple.
The redness disappears when the drug is stopped. Occasionally, though, another drug, such as epinephrine, diphenhydramine, or a corticosteroid, may be required.
10. Scabies
Scabies is caused by a mite called Sarcoptes scabiei. This parasite is transmitted by direct contact.
It produces hyperkeratotic lesions (thickening of the outer layer of the skin), with redness, burning, itching, and ulcers (from scratching). Treatment is based on the use of scabicides and ointments to mitigate symptoms, as well as the adoption of hygienic and personal hygiene measures.
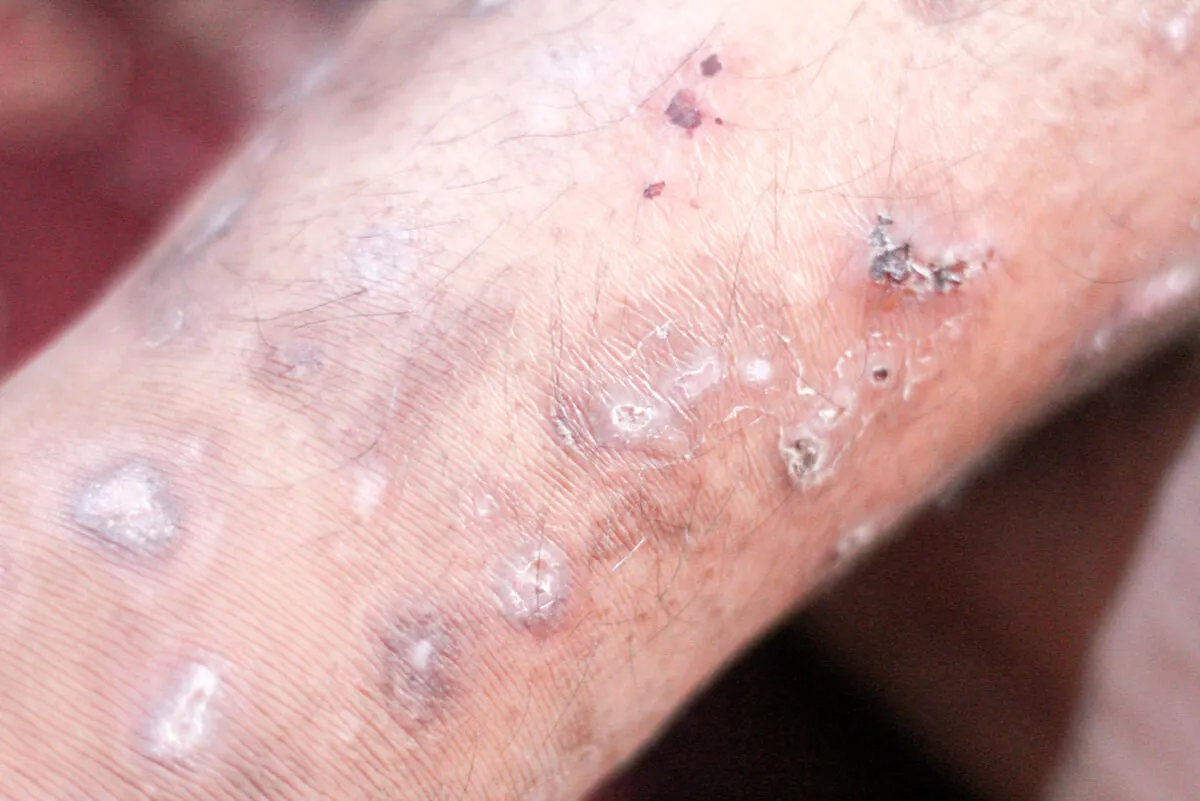
11. Cellulitis
Cellulitis occurs when bacteria enter the skin. The affected area becomes inflamed and red; it also often feels hot and very tender.
It can spread rapidly and is potentially serious. Treatment is antibiotic-based.
12. Candidiasis
Candidiasis is caused by a fungus called Candida albicans. Although this bacteria normally inhabit the body, it sometimes behaves as a pathogen, causing skin rashes.
Among other areas, red patches may appear on the glans, accompanied by itching. Treatment consists of antifungal creams (e.g. clotrimazole).
13. Impetigo
Impetigo causes sores around the mouth and nose, which then crust over. It also causes inflammatory reactions with red patches on the affected skin.
This is a very contagious bacterial infection that’s most common in children. Antibiotic treatment is usually effective.
14. Lichen planus
This is an autoimmune condition. In this case, the red spots are flat and appear in the mouth, throat, nails, scalp, or genitals.
It’s most common in women aged 30 to 60 years. It’s not well understood what causes it, although researchers suspect a genetic component.
It’s not contagious and goes away on its own. However, it can also become a chronic disease. Treatment options consist of topical corticosteroids or retinoids and oral antihistamines.
Like this article? You may also like to read: Mandelic Acid: What Is It and What Are its Benefits for the Skin?
15. Chickenpox
This is a highly contagious disease. It’s caused by the varicella-zoster virus. It affects children the most, although after their first exposure, a lifelong immunity develops.
The most obvious symptom is a rash with red papules. Chicken pox is preventable because a vaccine is available. However, there is no treatment for the virus once a person has contracted it.
16. Measles
Measles remains a potentially deadly disease. It’s caused by a virus of the paramyxovirus family.
The most obvious symptom is a red rash. It can lead to serious complications and has a case fatality rate of about 10%. There is no treatment, but it can be prevented by vaccination.
17. Rubella
This is a contagious disease that’s more common in children. The virus is airborne and enters through the respiratory tract.
Symptoms include fever, nausea, and a skin rash (pink rash). There’s also no cure, but a vaccine is available.
18. Skin cancer
Red spots are often a clinical sign of skin cancer. In this case, treatment may include various procedures, such as excision, Mohs surgery, curettage, electrodesiccation, freezing, or cryotherapy, as well as radiation and chemotherapy.
19. Lupus
Lupus is an autoimmune disease in which the body’s own defense system attacks healthy cells. Lupus can affect various organs (kidneys, brain, heart, lungs), as well as joints and skin. On the face, it causes rashes in the form of reddish spots.
There is no cure for lupus. Treatments are aimed at improving the patient’s quality of life by seeking to reduce symptoms and outbreaks.
This includes lifestyle changes, as well as anti-inflammatory drugs, immunosuppressants, and corticosteroids.
20. Petechiae
Small, round, reddish, or brownish spots are called petechiae. They may be due to the following:
- An infection.
- An injury
- An allergic reaction
- Hemorrhagic coagulation disorder
These red spots are not itchy or lumpy; however, they may spread and form larger spots. Treatment depends on the cause. Antibiotics are sometimes required.
21. Blood moles
Blood moles, cherry angiomas, or cherry hemangioma is the name for these small skin growths, which appear as a round red or purple spot. Sometimes, they can be raised. They are most common in people over 30 years of age.
They can be diagnosed with a simple visual examination and do not require any treatment. If the person is uncomfortable with their appearance or bleeding, however, they can be treated or removed with laser, nitrogen, or other methods.
They are not usually a cause for alarm. However, there is a possibility that they may be due to a clotting disorder.
22. Acne
Acne can also lead to red spots on the skin, whether on the face, chest, or back. There are a variety of drugs and cosmetic products, and even home remedies, to treat acne. However, the main recommendation is to avoid touching pimples or blackheads.
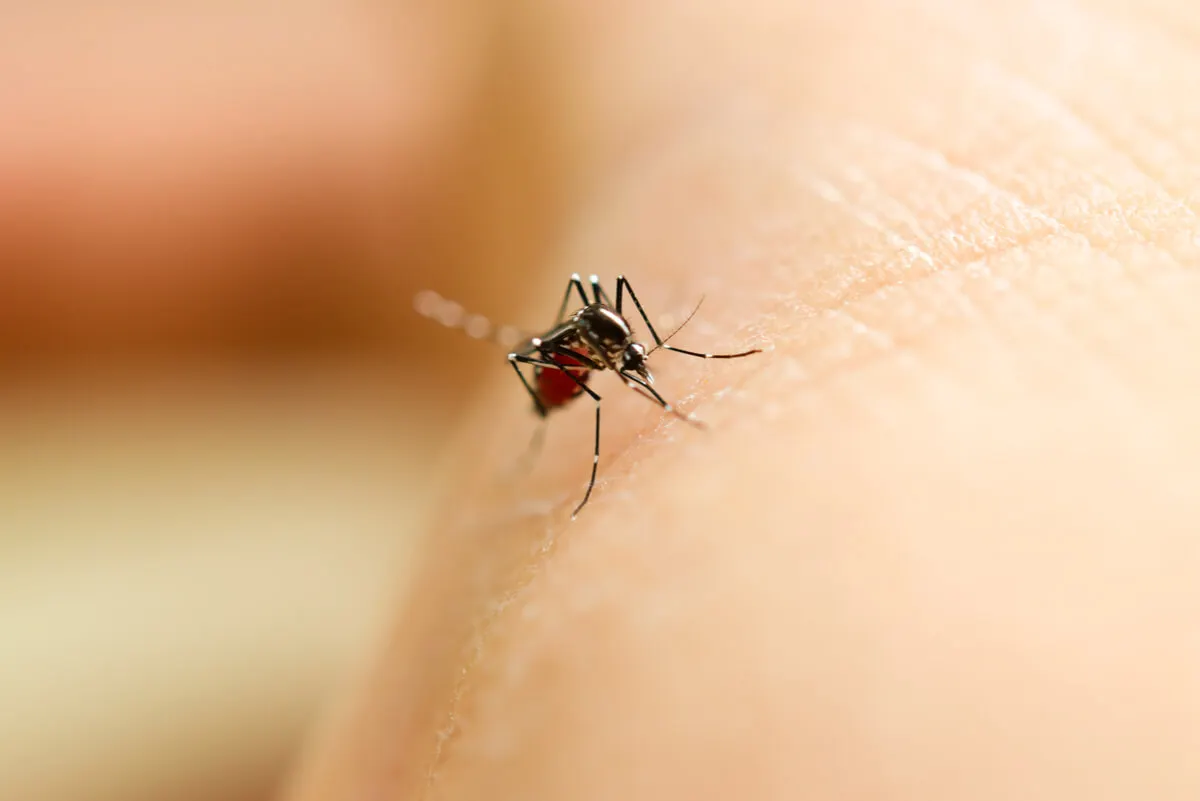
23. Insect bites
A very common reaction to insect bites is the appearance of red spots on or around the area where the bite occurred. This may be accompanied by an inflammatory reaction and itching.
The stinging effects are relieved with ointments. If the person is allergic to the insect, an antihistamine should be administered. In any case, it’s advisable to avoid exposure by covering up well and using instect repellents.
24. Swimmer’s itch
Swimmer’s itch, or cercariae dermatitis, is also called jock itch. It’s the name given to the larval forms of trematodes (specifically, schistosomes). This is an itchy rash caused by immersion in water contaminated with these parasites.
It’s not contagious. Treatment is with corticosteroids and antihistamines. On occasion, it may require antibiotics.
25. Stress
Experiencing stressful situations, in the short or long term, results in the appearance of various physical symptoms. Therefore, stress can also cause red spots to appear on the skin in some people.
When to consult a doctor
Depending on the area where they are, red spots on the skin are either a noticeable symptom or not. At least for the person affected, they do not usually go unnoticed.
If the spots disappear in a short time, there’s no need to worry. However, if they persist for some time, it’s always a good idea to make an appointment with a physician to evaluate them and recommend treatment.
Immediate attention should be sought if, in addition to persisting, the spots are accompanied by other symptoms, such as the following:
- Fever
- Palpitations
- Intense pain
- Extreme fatigue
- Shortness of breath or choking sensation
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Alonso, M. C., Leonard, D. D., Cruz, Y. B., & Rodríguez, A. E. S. (2020). Cáncer de piel no melanoma y radiaciones ultravioletas. Folia Dermatológica Cubana, 12(1).
- Armstrong, A. W., & Read, C. (2020). Pathophysiology, clinical presentation, and treatment of psoriasis: a review. Jama, 323(19), 1945-1960.
- García-Bravo B, Conde-Salazar L, De la Cuadra J, et al. Estudio epidemiológico de la dermatitis alérgica de contacto en España. Actas Dermo-Sifiliográficas. 2004; 95(1): 14-24.
- Johnston G, Exton L, Mohd Mustapa M, et al. British Association of Dermatologists’ guidelines for the management of contact dermatitis. Br J Dermatol. 2017; 176(2): 317-329.
- Le Cleach L, Chosidow O. Lichen planus. N Engl J Med. 2012; 366(8): 723-32.
- Lyons J, Milner J, Stone K. Atopic dermatitis in children: clinical features, pathophysiology, and treatment. Immunol Allergy Clin North Am. 2015; 35(1): 161-183.
- Morgado-Carrasco, D., Piquero-Casals, J., & Podlipnik, S. (2022). Tratamiento de la escabiosis. Atención Primaria, 54(3), 102231.
- Pastrana, I. R. M. (2018). Prurigo por insecto y alergia a la picadura del mosquito: estudio de caso. Atención Familiar, 25(3), 129-131.
- Petit A. Pitiriasis rosada («pityriasis rosea»). EMC – Dermatología. 2015; 49(4): 1-7.
- Ranganathan D, John GT. Therapeutic plasma exchange in renal disorders. Indian J Nephrol. 2019; 29(3): 151-159.
- Tanghetti E. The role of inflammation in the pathology of acne. J Clin Aesthet Dermatol. 2013 Sep; 6(9): 27–35.
- Thomas A, Baird S, Anderson J. Purpuric and petechial rashes in adults and children: initial assessment. BMJ. 2016; 352: i1285.
- Urbina F, Das A, Sudy E. Clinical variants of pityriasis rosea. World J Clin Cases. 2017; 5(6): 203-211.
- Zaenglein, A. L. (2018). Acne vulgaris. New England Journal of Medicine, 379(14), 1343-1352.
- Trac, E. Et al. Outbreak of Swimmer’s Itch in Denmark. 2019. ActaDV. Doi: 10.2340/00015555-3309
- RICHARD P. USATINE, MD, AND MICHELLE TINITIGAN, MD. Diagnosis and Treatment of Lichen Planus. 2011. Disponible en: https://www.aafp.org/pubs/afp/issues/2011/0701/p53.html
- Baptista, L. Impetigo – review. 2012. DOI: http://dx.doi.org/10.1590/abd1806-4841.20142283
- Campillos Páez, S. Et al. Escabiosis: revisión y actualización. 2002. Medifam vol.12 no.7. Disponible en: https://scielo.isciii.es/scielo.php?script=sci_arttext&pid=s1131-57682002000700004
-
Aditya K Gupta, Maria Chaudhry, & Boni Elewski. Tinea corporis, tinea cruris, tinea nigra, and piedra. 2003. Dermatologic Clinics. Disponible en: https://www.derm.theclinics.com/article/S0733-8635(03)00031-7/fulltext
- Thomas J. Zuber. 2000. ROSACEA. Primary Care: Clinics in Office Practice. Disponible en: https://www.primarycare.theclinics.com/article/S0095-4543(05)70197-4/fulltext
- Ma. T. Bordel-Gómeza, A. Miranda-Romerob, J. Castrodeza-Sanzc. 2010. Epidemiología de la dermatitis de contacto: prevalencia de sensibilización a diferentes alérgenos y factores asociados. Actas Dermo-Sifiliográficas. Disponible en: https://www.sciencedirect.com/science/article/abs/pii/S0001731009000064
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








