Polycystic Ovarian Syndrome and its Treatment
Written and verified by the doctor Nelton Abdon Ramos Rojas
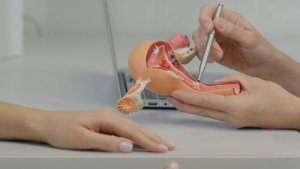
Generally, the medical community uses the term “polycystic ovarian syndrome” to refer to an alteration of the female reproductive system. It commonly afflicts women who are still within their reproductive age.
Those affected by polycystic ovarian syndrome have fibrous structures inside their ovaries and these produce hormonal alterations. Thus, their levels of androgens (Y-chromosome hormone), such as testosterone and androsterone, are usually high.
Besides, this hormonal imbalance produces a series of symptoms which, if not properly treated, could lead to more serious complications over time.
Polycystic Ovarian Syndrome
Symptoms

The most frequent symptoms associated with the polycystic ovarian syndrome are:
- Changes in menstrual cycles. These changes may affect intervals, duration, or intensity.
- Infertility or problems getting pregnant.
- Hirsutism, or an increase in facial hair. It may appear in body regions that were hairless before.
- Acne development that varies in severity.
- Loss of hair with all the characteristics of male baldness.
You may be interested: Seven Reasons You Might Feel Pain in Your Ovaries
In addition, polycystic ovarian syndrome is often present in women who are overweight or obese. These factors also contribute to the worsening of symptoms and new complications such as:
- Alterations during pregnancy. This is usually associated with gestational diabetes and hypertension.
- Sleeping disorders such as sleep apnea.
- Type 2 diabetes.
- Uterine bleeding.
- Changes in the behavior of a woman.
- Slight probability of developing other diseases such as uterine cancer or metabolic syndrome.
Researchers are yet to identify the exact trigger of this syndrome. However, there are several factors associated with its development.
In any case, there are several changes in the usual function of the ovaries. For example, this imbalance causes the ovaries to develop numerous small collections of fluid called follicles and it may fail to regularly release mature eggs during what should be the menstruation cycle.
Discover: Beets and Molasses, a Traditional Remedy for Ovarian Cysts
Treatments for Polycystic Ovarian Syndrome
Nowadays, medical professionals have many choices when it comes to selecting treatment. Therefore, they select the most appropriate method is according to the specific characteristics of a person and the impact of the syndrome in them.
Thus, it’s important that a woman diagnosed with polycystic ovaries informs her gynecologist about any medication she may be taking. In addition, she should also inform them about her lifestyle, allergies and any other health issues she may be dealing with or might’ve had in the past.
Treatment
These are some of the treatment guidelines that are most used today:
- Controlled weight reduction. The advice is to follow a balanced diet and maintain a daily physical routine.
- Administering medication. This is for treating symptoms of endocrine disorders related to the polycystic ovarian syndrome. Overall, these are some of the most commonly prescribed drugs to treat polycystic ovaries:
- Contraceptive pills. These are for regulating hormone levels due to their content of estrogen and progesterone. Not only that, but they can also regulate menstrual periods and uterine hemorrhages. Also, they reduce the chances of acquiring other diseases such as uterine cancer.
- Chemical compounds with progesterone. These, just like contraceptives, help regulate menstrual cycles and are a form of prevention against uterine cancer.
- Other treatments to cope with excessive hair growth or hirsutism.
3. Electrolysis. This is a technique to destroy the ovaries’ follicles. To do so, a needle sends a tiny electrical charge to the problem area. This kind of treatment requires a few sessions to complete.
We hope this article was useful. Perhaps it even answered some of your questions and solved and doubts you may have had. However, don’t hesitate to contact your gynecologist for any other questions you may still have on the subject.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Azziz, R. (2018). Polycystic ovary syndrome. Obstetrics & Gynecology, 132(2), 321-336. https://journals.lww.com/greenjournal/Fulltext/2018/08000/Polycystic_Ovary_Syndrome.9.aspx?context=FeaturedArticles&collectionId=4
- Bambhroliya, Z., Sandrugu, J., Lowe, M., et al. (2022). Diabetes, polycystic ovarian syndrome, obstructive sleep apnea, and obesity: a systematic review and important emerging themes. Cureus, 14(6), 1-11. https://www.cureus.com/articles/95667-diabetes-polycystic-ovarian-syndrome-obstructive-sleep-apnea-and-obesity-a-systematic-review-and-important-emerging-themes
- Chaves, F. O., Quirós, S. L. y Morera, M. R. (2021). Manejo de infertilidad por anovulación en síndrome de ovario poliquístico. Revista Médica Sinergia, 6(2), 1-13. https://dialnet.unirioja.es/servlet/articulo?codigo=8373582
- Chiliquinga, S., Aguirre, R., Agudo, M., Chú, Á. y Cuenca, S. (2017). Criterios diagnósticos y tratamiento integral terapéutico del síndrome de ovarios poliquísticos. Revista Cubana de Obstetricia y Ginecología, 43(3), 173-181. http://scielo.sld.cu/scielo.php?pid=S0138-600X2017000300018&script=sci_arttext&tlng=en
- Deswal, R., Narwal, V., Dang, A. & Pundir, C. S. (2020). The prevalence of polycystic ovary syndrome: a brief systematic review. Journal of human reproductive sciences, 13(4), 261–271. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7879843/
- Ding, H., Zhang, J., Zhang, F., Zhang, S., Chen, X., Liang, W. & Xie, Q. (2021). Resistance to the insulin and elevated level of androgen: a major cause of polycystic ovary syndrome. Frontiers in endocrinology, 12, 1-14. https://www.frontiersin.org/articles/10.3389/fendo.2021.741764/full
- Escobar-Morreale, H. F. (2018). Polycystic ovary syndrome: definition, aetiology, diagnosis and treatment. Nature Reviews Endocrinology, 14(5), 270-284. https://www.nature.com/articles/nrendo.2018.24
- Guzmán López, J. A., Robles Lara, P. D., Rivera Contreras, O. E., Ramírez Velandia, F., Sepúlveda Sanguino, A. J. & Sepúlveda Agudelo, J. (2020). Review of diagnostic criteria for polycystic ovary syndrome. Medicas UIS, 33(3), 21-28. http://www.scielo.org.co/scielo.php?pid=S0121-03192020000300002&script=sci_abstract&tlng=en
- Helvaci, N., Karabulut, E., Demir, A. U. & Yildiz, B. O. (2017). Polycystic ovary syndrome and the risk of obstructive sleep apnea: a meta-analysis and review of the literature. Endocrine Connections, 6(7), 437-445. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5574283/
- Jazani, A. M., Azgomi, H. N. D., Azgomi, A. N. D. & Azgomi, R. N. D. (2019). A comprehensive review of clinical studies with herbal medicine on polycystic ovary syndrome (PCOS). DARU Journal of Pharmaceutical Sciences, 27(2), 863–877. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6895349/
- Kim, C. H., Chon, S. J. & Lee, S. H. (2020). Effects of lifestyle modification in polycystic ovary syndrome compared to metformin only or metformin addition: a systematic review and meta-analysis. Scientific reports, 10(1), 1-13. https://link.springer.com/content/pdf/10.1038/s41598-020-64776-w.pdf
- Kovanci, E. & Buster, J. E. (2015). Polycystic ovary syndrome. Clin Gynecol. https://www.cambridge.org/core/services/aop-cambridge-core/content/view/9F82ABBA3DA35ACDC3F85B5CB4D301FB
- Livadas, S., Anagnostis, P., Bosdou, J. K., Bantouna, D. & Paparodis, R. (2022). Polycystic ovary syndrome and type 2 diabetes mellitus: A state-of-the-art review. World journal of diabetes, 13(1), 5. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8771268/
- Meier, R. K. (2018). Polycystic Ovary Syndrome. Nursing Clinics of North America. https://doi.org/10.1016/j.cnur.2018.04.008
- Mirzohidovna, H. E. Z. (2021). Obesity as a risk factor for recurrent polycystic ovary disease. Asian journal of pharmaceutical and biological research, 10(3). https://www.ajpbr.org/index.php/ajpbr/article/view/41
- Ong, M., Peng, J., Jin, X. & Qu, X. (2017). Chinese herbal medicine for the optimal management of polycystic ovary syndrome. The American Journal of Chinese Medicine, 45(03), 405-422. https://www.worldscientific.com/doi/abs/10.1142/S0192415X17500252
- Penzias, A., Bendikson, K., Butts, S., et al. (2017). Role of metformin for ovulation induction in infertile patients with polycystic ovary syndrome (PCOS): a guideline. Fertility and sterility, 108(3), 426-441. https://www.sciencedirect.com/science/article/pii/S0015028217304855
- Pérez Rojas, J. M. & Maroto Fernandez, K. E. (2018). Polycystic ovary syndrome (PCOS). Medicina Legal de Costa Rica, 35(1), 94-101. https://www.scielo.sa.cr/scielo.php?pid=S1409-00152018000100094&script=sci_arttext&tlng=en
- Winnykamien, I., Dalibón, A. & Knoblovits, P. (2017). Síndrome de ovario poliquístico. Rev. Hosp. Ital. B. Aires, 37(1), 10-20. https://www1.hospitalitaliano.org.ar/multimedia/archivos/noticias_attachs/47/documentos/31087_10-20-Winnykamien-D.pdf
- Woodward, A., Klonizakis, M. & Broom, D. (2020). Exercise and polycystic ovary syndrome. Physical Exercise for Human Health, 123-136. https://link.springer.com/chapter/10.1007/978-981-15-1792-1_8
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








