7 Most Common Oral Diseases and Their Treatment


Written and verified by the dentist Vanesa Evangelina Buffa
It’s common to visit the dentist because of an urgent need, such as a toothache, a broken tooth, or just simply because we want to know what’s going on in our mouth! Although many common oral diseases are preventable, people often end up having to go to the dentist to get them sorted out.
According to the Global Burden of Disease Study 2019, oral diseases affect about 3.5 billion people worldwide. Untreated dental caries in permanent teeth is the most frequent health disorder.
Oral diseases cause pain and discomfort to the sufferer. The most serious ones can lead to facial deformities and even death.
Several of these disorders can be prevented with simple care or treated in their early stages. However, some people postpone their oral health, and the processes worsen and get more invasive, complex, and expensive treatments are necessary.
Knowing about the most common oral diseases will help you to focus on the factors that favor their development, in order to prevent them or to take action to avoid their progression. Discover here the most common oral health problems and their treatment.
The 7 most common oral diseases
1. Tooth decay
Tooth decay is the most common oral pathology. It affects people all over the world, regardless of gender and age.
According to the Global Burden of Disease Study 2019, tooth decay in permanent teeth is the most common oral disorder. Around 2 billion people suffer from it and 520 million children suffer from the disease in milk teeth.
Tooth decay is the deterioration of the hard tissues of the teeth. They lose their minerals due to the action of acids produced by bacteria in the mouth when metabolizing sugars in the diet.
Poor oral hygiene and a diet rich in simple carbohydrates are the main factors associated with the appearance of this disease. If there are many bacteria in the mouth and they have enough sugar to multiply and accumulate more and more, the acidity in the mouth will damage the teeth.
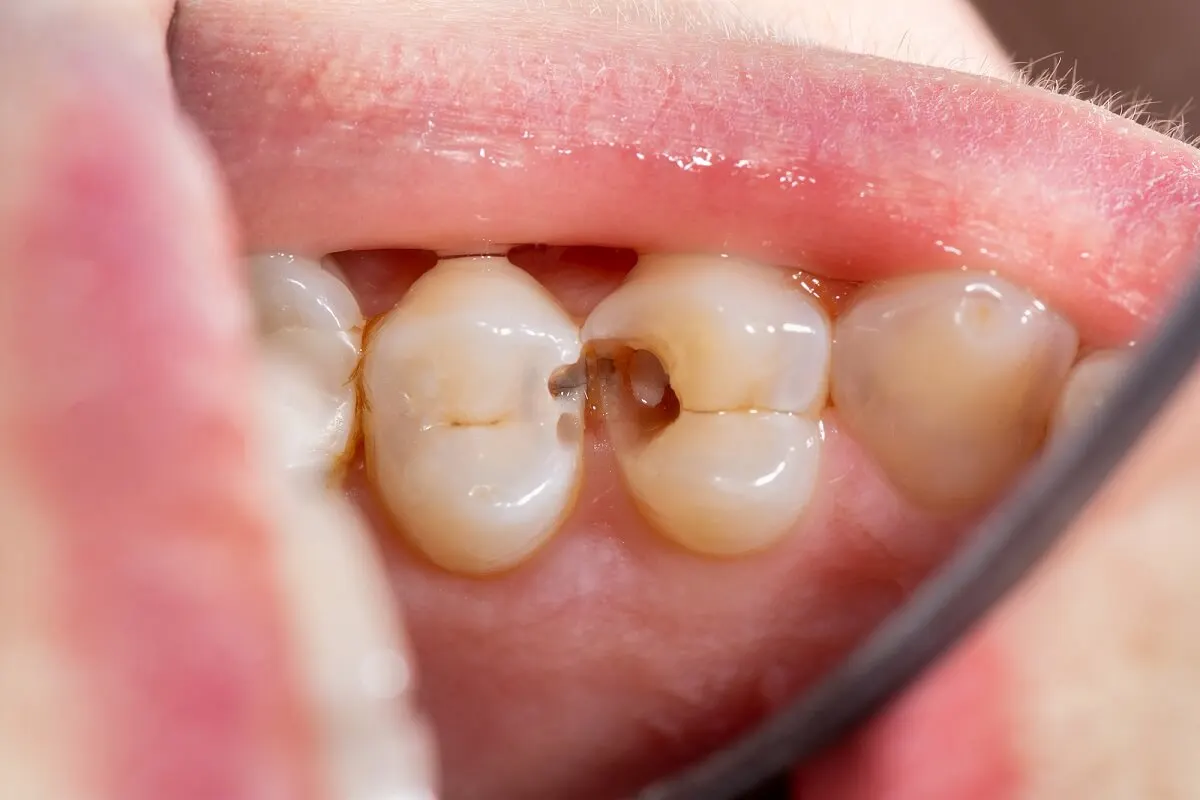
At the beginning of the disease, tooth decay looks like a dry white spot on the surface of the tooth enamel. As the process continues, the spots darken, the tissues break down, and gaps and cavities appear in the teeth.
If cavities aren’t treated in time, the destruction can affect the dental pulp. This causes pain and infections that aggravate the situation and require more complex treatments for their resolution.
In their early stages, tooth decay can be reversed with fluoride therapies. However, when there’s tissue loss, depending on the extent of the lesion and the severity of the case, fillings, root canals, or even tooth extraction will be necessary.
With healthy habits, tooth decay can be avoided. Practicing proper oral hygiene every day, using fluoride toothpaste, eating a low-sugar diet, and visiting the dentist every six months are effective ways to prevent this disease.
Find out more: Bacteria that Cause Cavities
2. Periodontal problems
Other of the most common oral diseases are those affecting the periodontium: gingivitis and periodontitis. These disorders are more common in adults, but can also develop in children and adolescents.
According to the World Health Organization (WHO), severe periodontal conditions are estimated to affect almost 14% of adults. This corresponds to more than 1 billion cases worldwide.
Gingivitis
Gingivitis is the inflammation of the gums and the beginning of periodontal problems. The lack of oral hygiene causes the accumulation of bacterial plaque and tartar that irritates the gingival tissue. Although there are other factors that also favor the picture, such as hormonal changes and pregnancy, smoking, or the presence of some systemic diseases.
Gingivitis can be recognized because the gingival tissue has an intense red color, swells, bleeds easily, and hurts. Spitting up blood when brushing teeth is one of the most common manifestations of this disorder and a wake-up call that shouldn’t be missed.
Treatment consists of thorough oral hygiene at home, including brushing teeth and gums, flossing, fluoride toothpastes, and antiseptic mouthwashes. Also, professional cleanings at the dentist’s clinic are necessary to remove tartar deposits.
Periodontitis
Periodontitis is also known as “periodontal disease” or “pyorrhea”. It’s what happens when gingivitis hasn’t been treated and has progressed and reached deeper tissues.
Bacteria from plaque and tartar reach the deepest areas of the gum, causing pockets where they accumulate and proliferate. This leads to infection and inflammation of the tissues that support the teeth.
Periodontitis affects the gums, the roots of the teeth, the periodontal ligament, and the alveolar bone. These structures are responsible for holding the teeth in place.
In periodontitis, the supporting tissues are damaged and the bone is destroyed. With this, the teeth lose their support and it’s very common for them to start to move or, in the most advanced cases, even to come out.
Tooth mobility is one of the characteristic symptoms of periodontitis. In addition, the patient will have gingival inflammation or recession, discomfort in the teeth, bad breath, pus, bleeding, and pain in the gums.
Periodontal disease is a disorder that needs to be treated as soon as it’s diagnosed, so that it doesn’t continue to progress. Not only because it can leave you without teeth, but also because this condition is associated with systemic conditions. Diabetes, heart disease, and respiratory and neurological diseases are some examples.
The treatment of periodontitis requires the intervention of the dentist. Depending on the severity of the condition and the extent of the damage, the professional will perform cleaning, scaling, root planing, and periodontal surgery, complemented by the use of local antiseptics and antibiotics.
Find out all about: Dental Curettage: Procedure, Results and Care
3. Canker sores
Canker sores are ulcerations that occur on the oral mucosa causing pain and discomfort in the mouth. Their causes aren’t entirely clear, although several factors favor their appearance: stress, hormonal changes, immune problems, trauma, food hypersensitivity, and some oral infections.
Canker sores are characterized by rounded, whitish lesions with red edges. They hurt when touched or when eating very salty or spicy foods.
They develop mainly on the cheeks, lips, or sides, and underside of the tongue. They also occur on the back of the roof of the mouth and gums.
Canker sores are not contagious. These lesions usually heal on their own within 10 to 14 days.
This means that no treatment is necessary, although some symptom-improving measures will alleviate the process. Soft and cool diets, avoiding spicy, acidic, and salty foods, and applying some local analgesic can soothe the annoying symptoms.
If the lesions persist after 2 weeks, it’s important to consult the dentist to rule out other problems.
4. Oral infections
Bacteria, fungi, and viruses can affect oral tissues and cause infections with manifestations in the mouth. We have already told you about caries, gingivitis, and periodontitis, pathologies caused by bacteria in the mouth.
Dental and periodontal abscesses are collections of pus, the product of infections in the teeth and gums that haven’t been treated. These processes cause pain and swelling in the area. In addition, there’s a risk that the condition may spread to other distant areas.
It’s important that dental abscesses are treated as soon as they’re detected. The use of antibiotics is necessary, in addition to eliminating the infectious focus through root canals, extractions, curettage, or periodontal surgery.
But not only the bacteria that attack the teeth and periodontium are responsible for infections in the mouth. Here are other common oral diseases caused by germs.
Candidiasis
Candidiasis or thrush is a common infection of the oral mucosa, especially in children and the elderly. It is caused by Candida albicans, a fungus that’s usually present in the mouth.
When certain favorable conditions occur, this microorganism grows excessively. This breaks the balance of the oral ecosystem and mycosis develops.
Exaggerated oral hygiene, the excessive or frequent use of antibiotics, some medical treatments, or certain systemic diseases favor its appearance. This infection is one of the main oral manifestations in HIV patients.
Thrush is characterized by the appearance of small white spots that look like coagulated milk and don’t come off when you try to remove them with gauze. They occur on the corners of the lips, tongue, cheeks, palate, and other areas of the mouth. It’s treated with local or systemic antifungal agents, depending on the case.
Hand, foot and mouth disease
Hand, foot and mouth disease is an infection caused by coxsackievirus A16 and enterovirus 71. The condition doesn’t only affect the mouth, as its name suggests, but also manifests itself in the hands and feet.
Painful blisters appear on the cheeks and tongue, palms of the hands, soles of the feet, and buttocks. In addition, the process is accompanied by sore throat and fever.
This pathology is typical of young children and school-age children. It’s very uncomfortable, but tends to disappear after 3 to 5 days.
Herpangina
Herpangina is another common oral disease caused by coxsackievirus A and enteroviruses. It most often affects children ages 3 to 10 years, during the summer and fall seasons.
Small red spots appear in the back of the mouth at the beginning of the infection. They fill with fluid and turn into blisters that burst, leaving small sores.
The ulcerations are very small, measuring 2 to 4 millimeters, and are very painful. The discomfort they cause leads the child to refuse food and water.
They are most frequently located on the soft palate, tonsils, and throat. The symptoms are usually accompanied by a sore throat, difficulty swallowing, and fever.
The sores usually disappear on their own after 5 to 10 days. Throughout the process, it’s important to keep the child hydrated. Pain medication can be used.
Cold sores
Infections with the herpes virus are another fairly common oral problem. The manifestations will change depending on the age of the patient.
The first infection of children with the herpes virus usually occurs between the ages of 0 and 3 years old and is known as gingivostomatitis herpeticum. It’s characterized by swollen and bleeding gums and the appearance of small blisters and painful ulcers throughout the mouth.
In addition, the child usually has a fever, excessive drooling, refuses hydration, and is fussy and tired. The process lasts about a week and disappears by itself without treatment. However, the pediatrician may prescribe pain medication and home care measures to soothe the child.
Recurrent cold sores are another variant of oral infection with herpes simplex virus type I. Once a person has been infected by this germ, it remains latent in the body forever.
When faced with situations that reduce the defenses, the virus finds an opportune scenario to appear and produce symptoms. Eating certain foods, exposure to the sun or extreme cold, colds, stress, or trauma are some factors that predispose to the appearance of the condition.
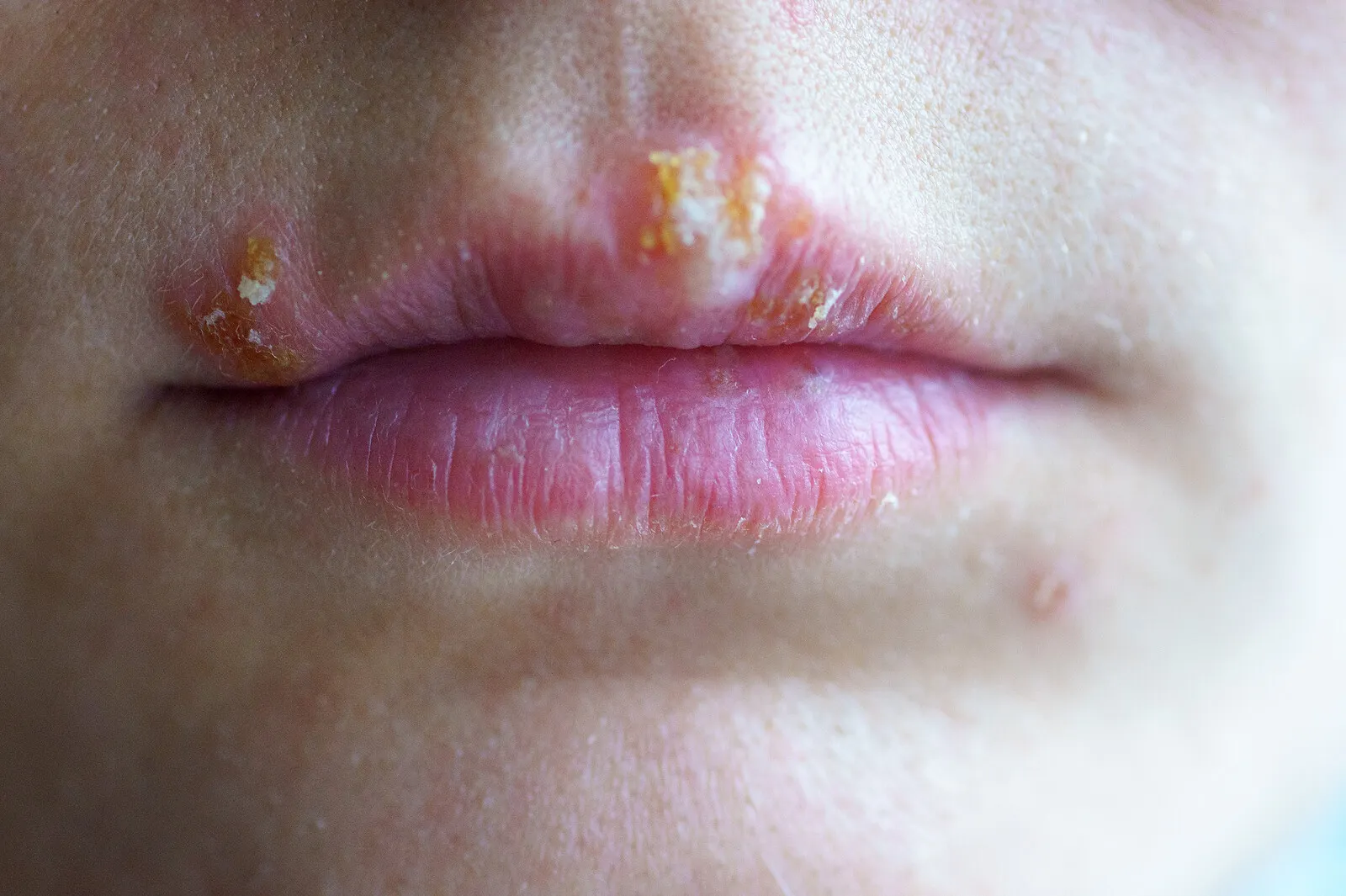
Oral herpes causes small fluid-filled blisters in the mouth or on the skin of the lips. They itch or hurt and, when they break, they leave yellowish crusts that heal after a few days.
The whole process lasts about 10 days and disappears without treatment. In any case, topical antivirals can be used to accelerate the healing of the lesions.
Herpes is contagious, so it’s important to take measures to avoid its transmission to other people and autoinoculation in other mucous membranes of the body.
6. Malocclusion
Bite problems and misaligned teeth are other common oral diseases. The lack of harmony and balance in the dentition prevents the correct relationship between the upper and lower teeth. This causes problems in chewing, eating, speaking, and esthetics.
Malocclusions can appear due to genetic problems that can’t be avoided. However, very often, they’re related to dysfunctional habits during childhood that could be prevented, such as thumb sucking, oral breathing, prolonged use of the bottle or pacifier, atypical swallowing.
To treat malocclusions, it’s necessary to resort to orthodontic treatments. Today there are several types of appliances that help improve a person’s bite.
Depending on the age of the patient, the problem to be treated, the severity of the malocclusion, and the needs of the person, the most appropriate option is chosen for each case.
7. Oral cancer
Oral cancer is among the most common and dangerous oral diseases. In fact, it is among the 10 most frequent types of cancer.
Oral cancer is detected more in people over 40 years of age. Between the ages of 60 and 62 is the diagnostic peak.
Malignization of oral cells is associated with several risk factors that accumulate throughout life:
- Tobacco
- Alcohol
- Infections with human papillomavirus
- Too much sun exposure
- Poor oral hygiene
- Dentures in bad condition
Manifestations vary depending on where in the mouth they’re located, and the type of cancer. They can be seen as red or white spots, ulcers that don’t heal, or lumps and tumors.
Depending on the type of cancer and the stage when it’s diagnosed, the treatment will be established. In any case, the prognosis is always better for cases that are detected as soon as symptoms begin. That’s why it’s very important to visit the dentist regularly and perform self-examinations to identify any suspicious changes.
Prevent oral diseases
Many of the most common oral diseases can be prevented. Simple practices and healthy lifestyle habits will help you avoid the discomfort of these conditions and the need for unpleasant, costly treatments.
Brushing, flossing, fluoride toothpastes, and oral rinses will help you control plaque problems. A healthy, low-sugar diet will also reduce germs and keep bones, teeth, and mucous membranes healthy.
Avoiding harmful habits such as smoking, alcohol, thumb sucking, or mouth breathing is another way to prevent oral disease. Frequent visits to the dentist complete our prevention methods.
Your dentist will help you keep your mouth healthy and help prevent the ailments we’ve told you about here. And, if they do occur, they’ll work to solve the problems as soon as they can.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Caiza, P., & Rubí, G. (2022). Remineralización del esmalte dental con flúor barniz y fluoruro diamino de plata. Estudio in vitro (Bachelor’s thesis, Quito: UCE).
- Perona, M. D. P. G., Gálvez, D. A., & Salinas, C. T. (2021). Developments in the use of varnish flúor. Reporte case. Revista de Odontopediatría Latinoamericana, 3(2), 111-117.
- Castillo, D. I. A. N. A., Chamorro, L. I. D. A., Díaz, J., Rosas, S. I. L. V. I. O., & Cabrera, C. R. I. S. T. I. A. N. (2019). Frecuencia de los factores de riesgo relacionados con la Gingivitis en la Clínica de Mediana Complejidad de la Universidad Cooperativa de Colombia campus Pasto, periodos 2017-II y 2018-I. San Juan de Pasto: Universidad Cooperativa de Colombia.
- Sojod, B., Périer, J. M., Zalcberg, A., Bouzegza, S., El Halabi, B., & Anagnostou, F. (2022). Enfermedad periodontal y salud general. EMC-Tratado de Medicina.
- Illescas, M. V. L., Soto, A. R., & González, B. G. (2019). Maloclusiones dentarias y su relación con los hábitos bucales lesivos. Revista Cubana de Estomatología, 56(2), 1-14.
- Solano, Y. H., & Molina, Y. A. (2019). Hábitos bucales deformantes y su relación etiológica con las maloclusiones. Multimed, 23(3), 580-591.
- Cárdenas, H. M. (2022). Identificación de cándida en cavidad bucal de pacientes con diabetes y VIH/SIDA. Estomatología, 30(1), NA-NA.
- Rivera, C. (2015). Essentials of oral cancer. International journal of clinical and experimental pathology, 8(9), 11884.
- Miguel Cruz, P. A., Niño Peña, A., Batista Marrero, K., & Miguel-Soca, P. E. (2016). Factores de riesgo de cáncer bucal. Revista Cubana de Estomatología, 53(3), 128-145.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








