Causes and Prevention of Prostatitis


Written and verified by the doctor María Irene Benavides Guillém
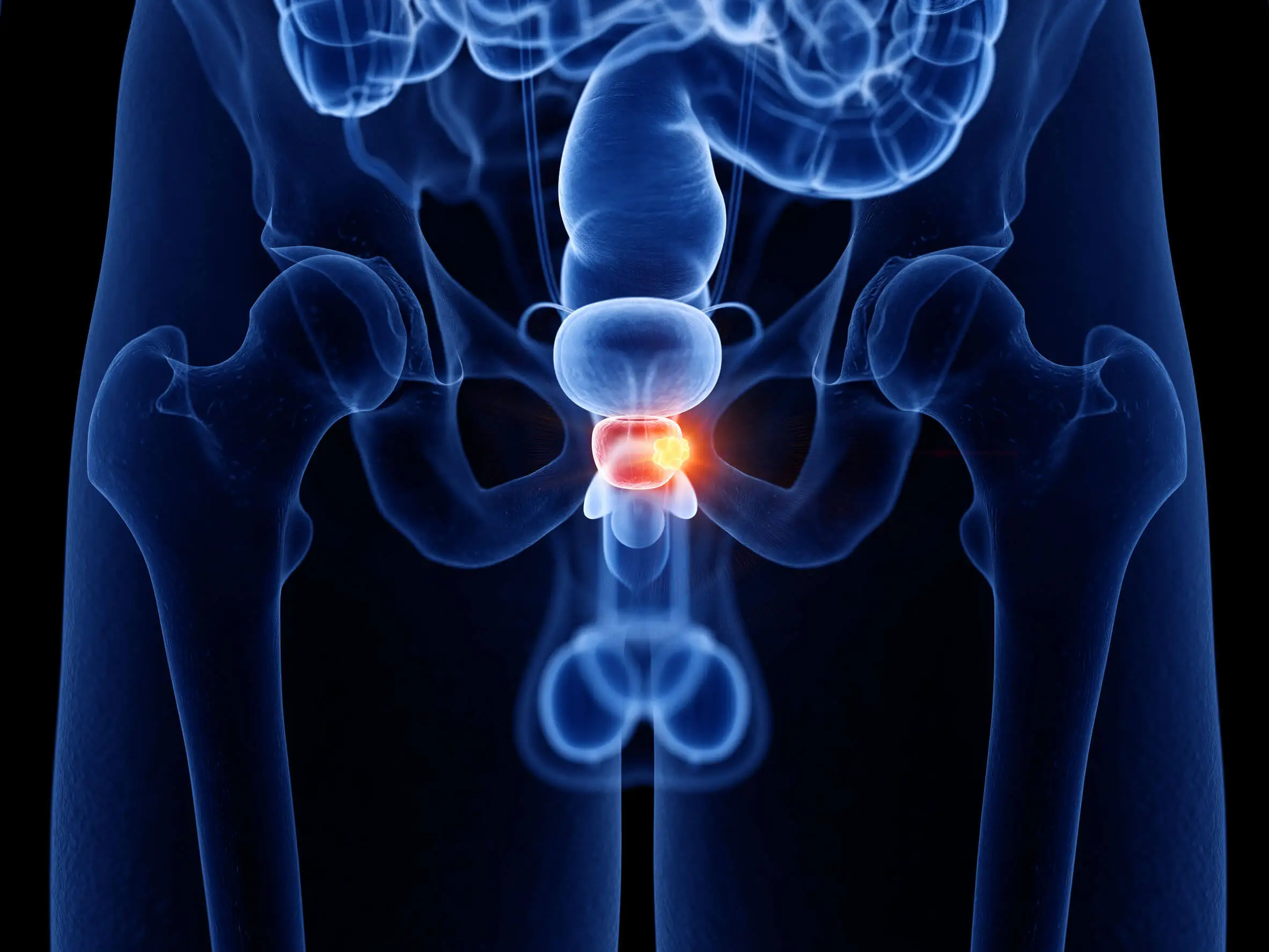
Prostatitis is the inflammation of the prostate gland. It’s part of the male reproductive system, and is located below the bladder, next to the rectum, and surrounding the urethra.
Prostatitis most commonly occurs between the ages of 20 and 40. This doesn’t mean it can’t occur at any time though. In fact, it affects 10 to 14 out of every 100 men.
Causes of prostatitis
Prostatitis has different causes, and delayed diagnosis and non-specific treatment are a real problem.
Although there are several classifications of the pathology, the most commonly used one is the division into bacterial and non-bacterial. Let’s have a closer look.
Acute bacterial prostatitis
Acute bacterial prostatitis is an infection of the prostate caused by bacteria that travel up the lower urinary tract or take the lymphatic route from the rectum. In these cases, the infection is said to be retrograde, as the bacterial elements ascend from outside the urogenital tract.
Bacterial prostatitis due to urinary tract infections
In men, unlike women, the urethra is part of the reproductive system. The prostate gland has several mechanisms to defend itself against infections. These range from its emptying during urination and ejaculation, to the production of antimicrobial substances.
However, poor drainage of secretions or reflux of urine into the prostate gland leads to inflammation of the gland. Thus, most bacterial prostatitis is caused by recurrent urinary tract infections.
Generally, only one type of microorganism causes the infection. In 50% to 87% of the cases, this bacterium will be Escherichia coli.
You might be interested in: How Antibiotics Work for Urinary Tract Infections
Bacterial prostatitis and sexually transmitted infections
Bacterial prostatitis can also result from sexually transmitted diseases. Bacteria such as Gardnerella vaginalis, Chlamydia trachomatis, and Neisseria gonorrhoeae are involved.
In addition, these germs can trigger autoimmune events, aggravating the picture. Such is the case of C. trachomatis infection in which antibodies that attack sperm are generated.
Non-bacterial prostatitis
As for non-bacterial prostatitis, its origin is less clear. There are several theories.
One theory is that there’s a backflow of urine causing chronic irritation and inflammation of the prostate. Another is that microorganisms or substances produced by them stimulate an autoimmune response.
Another theory links chronic prostatitis to hemorrhoids and varicocele. All due to a malfunction of the veins in the pelvic area.
Risk factors
There are different factors that can favor the appearance of prostatitis. These include medical conditions such as bladder catheter use and dialysis treatment. Also, having diabetes and HIV infection are additional factors that will increase the risk.
In addition to this, sexual habits are substantial determinants for the development of prostatitis. Thus, having multiple sexual partners without the use of condoms is considered high-risk behavior.
Read more: The Foley Catheter: Use and Technique
Depression as a risk factor for prostatitis
According to some theories, chronic prostatitis may behave as a psychosomatic disease. This entity has been linked to stress, anxiety, and increased sensitivity to pain.
Along these lines, Lien et al. conducted a study in which they found that men with depression had almost twice the risk of developing acute and chronic prostatitis compared to those who didn’t have it. The reasons why this happens are still under investigation.
Symptoms
Men with prostatitis have a series of non-specific symptoms of the lower genitourinary system. These include pain between the scrotum and rectum that radiates to the groin and even to the genitals. In some cases, there may even be pain in the lower back.
Other frequent symptoms are fever, general malaise, increased urination or urinary retention, as well as discomfort when urinating. There can even be pain during sexual intercourse and premature ejaculation.
In some patients, the most noticeable symptoms are urinary, while in others the manifestations become evident in a person’s sex life.
Asymptomatic prostatitis
Many men with prostatitis are asymptomatic. This leads to the condition becoming chronic. Sometimes, in men over 50 years of age, the diagnosis is made accidentally, due to abnormal findings in a urine test.
Diagnosis
The diagnosis of prostatitis isn’t simple. A complete medical history and a detailed physical examination will always be important. The prostatitis symptom survey proposed by the US National Institutes of Health may be helpful.
Acute prostatitis
In acute bacterial prostatitis, the prostate is enlarged, tender, and very painful on palpation. The Asian Association of Urinary Tract Infection and Sexually Transmitted Infection (AAUS) recommends a urinalysis that would show leukocytes and bacteria, as well as a urine culture.
Prostate antigen (PSA) determination isn’t a routine test for the diagnosis of prostatitis. However, if doctors carry one out, high readings will be found. In such circumstances, post-treatment follow-up should be carried out.
Chronic prostatitis
In chronic prostatitis, a digital rectal examination isn’t helpful. Minimally high magnification and sensitivity will be found.
In this case, other tests such as a sperm or semen culture are helpful. Occasionally, a biopsy may be required to make the diagnosis.
In conjunction with this, a prostate ultrasound is key in the diagnosis of acute and chronic prostatitis. It’ll help to rule out the presence of complications, such as a prostatic abscess.
Possible complications
There is a wide range of complications with prostatitis. A poorly treated bacterial variant can have serious consequences, such as abscesses, testicular infections, or sepsis.
Meanwhile, when the problem becomes chronic, it brings with it chronic pain and sexual dysfunction. Even infertility is an expected outcome.
Sexual dysfunction and psychological problems resulting from prostatitis
Failure to deal with it in time leads to chronic and worsening symptoms. The intensity of pain due to prostatitis can be such that it compromises male sexual performance. Relationships can become a traumatic and painful experience.
Since this is a taboo subject, men hardly ever share it with anyone. Such a situation leads to psychological disorders.
Prostatitis and male infertility
The prostate secretes a prostatic fluid rich in zinc, which represents between 25% to 30% of the ejaculation liquid. Accessory glands secrete proteins such as semenogelin, which, when released by the seminal vesicle, creates viscosity in the semen.
This is why prostatitis can prevent or hinder fertilization, as semen quality must be excellent in order to increase the chances of fertilization.
Prostatitis and prostate cancer
According to the American Cancer Society, several researchers have found an association between prostatitis and prostate cancer. Thus, cancer cells have been found in inflamed prostate tissue.
Although further studies are needed to confirm this hypothesis, this makes us think about the care and dedication with which we must diagnose patients. Good management and treatment of prostatitis will be the basis for avoiding fatal outcomes.
Many men don’t go to see a doctor when they have prostatitis symptoms out of fear. This makes proper treatment difficult.3 tips to prevent prostatitis
Some simple measures can help to prevent prostatitis. They’re easy to implement and don’t require too many complications.
1. Wash your hands
Washing your hands before and after urinating reduces the number of microorganisms found in the extremities, and infections are prevented.
2. Healthy sexual life
All steps to help prevent sexually transmitted infections also prevent urinary tract infections and prostatitis. Among them is the correct use of condoms.
3. Healthy body, healthy prostate
To care for your prostate, try to do everything you can to promote well-being. Avoid stress, do physical activity, and have a balanced diet.
Overcome embarrassment
The most important message is to go and see a doctor as soon as you notice any relevant symptoms. Overlooking, hiding, or ignoring the discomfort will only aggravate the problem. It’s crucial that you put your embarrassment to one side and go and see your doctor as soon as you can.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Matsumoto M, Yamamoto S. AAUS guideline for acute bacterial prostatitis 2021. J Infect Chemother. 2021;27(9):1277-1283.
- Puerta-Suárez J., Cardona-Maya W. D. La próstata desde una perspectiva inmunológica. Medicina y Laboratorio 2020;24(1):13-35.
- Magri V, Boltri M, Cai T, Colombo R, Cuzzocrea S, De Visschere P et al. Multidisciplinary approach to prostatitis. Arch Ital Urol Androl. 2019;90(4):227-248.
- Robles A, Garibay T. R., Acosta E, Morales S. La próstata: generalidades y patologías más frecuentes. Revista de la Facultad de Medicina (México), 2019;62(4):41-54.
- Repetto E, Sosa A, Colla R, Metrebian E, Metrebian S. Relación de prostatitis en la aparición del cáncer de próstata y la hiperplasia benigna prostática. Revista Cubana de Urología 2019;8(1):22-33.
- Puerta J., Cardona W. Prostatitis: revisión de una patología enigmática y su relación con la fertilidad masculina. Urol Colomb 2018;27(3):233–242.
- Torres K. L. Prostatitis. Revista Médica Sinergia 2018;2(1):26-31.
- Reyes N., Correa Ó. Inflamación y cáncer de próstata: implicaciones biológicas y posible utilidad clínica. Iatreia 2914;27(1):73-84.
- Jiménez-Cruz J. F., Broseta-Rico E. Clasificación, etiología, diagnóstico y tratamiento de las prostatitis. Otros tipos de prostatitis. Enferm Infecc Microbiol Clin 2005;23(Supl. 4):47-56.
- Lien CS, Chung CJ, Lin CL, Chang CH. Increased risk of prostatitis in male patients with depression. World J Biol Psychiatry. 2020;21(2):111-118.
- Collins MM, O’Leary MP, Calhoun EA, Pontari MA, Adler A, Eremenco S et al; Chronic Prostatitis Collaborative Research Network. The Spanish National Institutes of Health-Chronic Prostatitis Symptom Index: translation and linguistic validation. J Urol. 2001;166(5):1800-3.
- En la referencia de la Bibliografía Reyes N., Correa Ó. Inflamación y cáncer de próstata: implicaciones biológicas y posible utilidad clínica. Iatreia 2014;27(1):73-84
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








