What is a Contraceptive Patch and How Does it Work?

Reviewed and approved by the pharmacist Franciele Rohor de Souza
The contraceptive patch is a method to prevent unwanted pregnancy. It can be placed on different parts of the body, either on the belly, buttocks, back, or arm. Its working principle is similar to that of the pill, as it releases hormones such as estrogen and progestin.
As long as it’s used properly, it’s considered effective. However, there are some factors that can affect its effectiveness. Do you want to know more about it? In this article, we’ll tell you how it works, its possible side effects, and when this method is contraindicated. Continue reading to learn more!
The contraceptive patch: What it’s used for and how it works
There are several methods to prevent unwanted pregnancies, both for use by men and women. Among the most commonly used are the following options:
- Condoms
- Diaphragms
- Pills
- Vaginal rings
- Copper IUDs
In particular, the “contraceptive patch” or “transdermal patch” is among the so-called “hormonal methods. “ This means that its principle of operation is based on the release of estrogen and progestin, which is a synthetic form of progesterone.
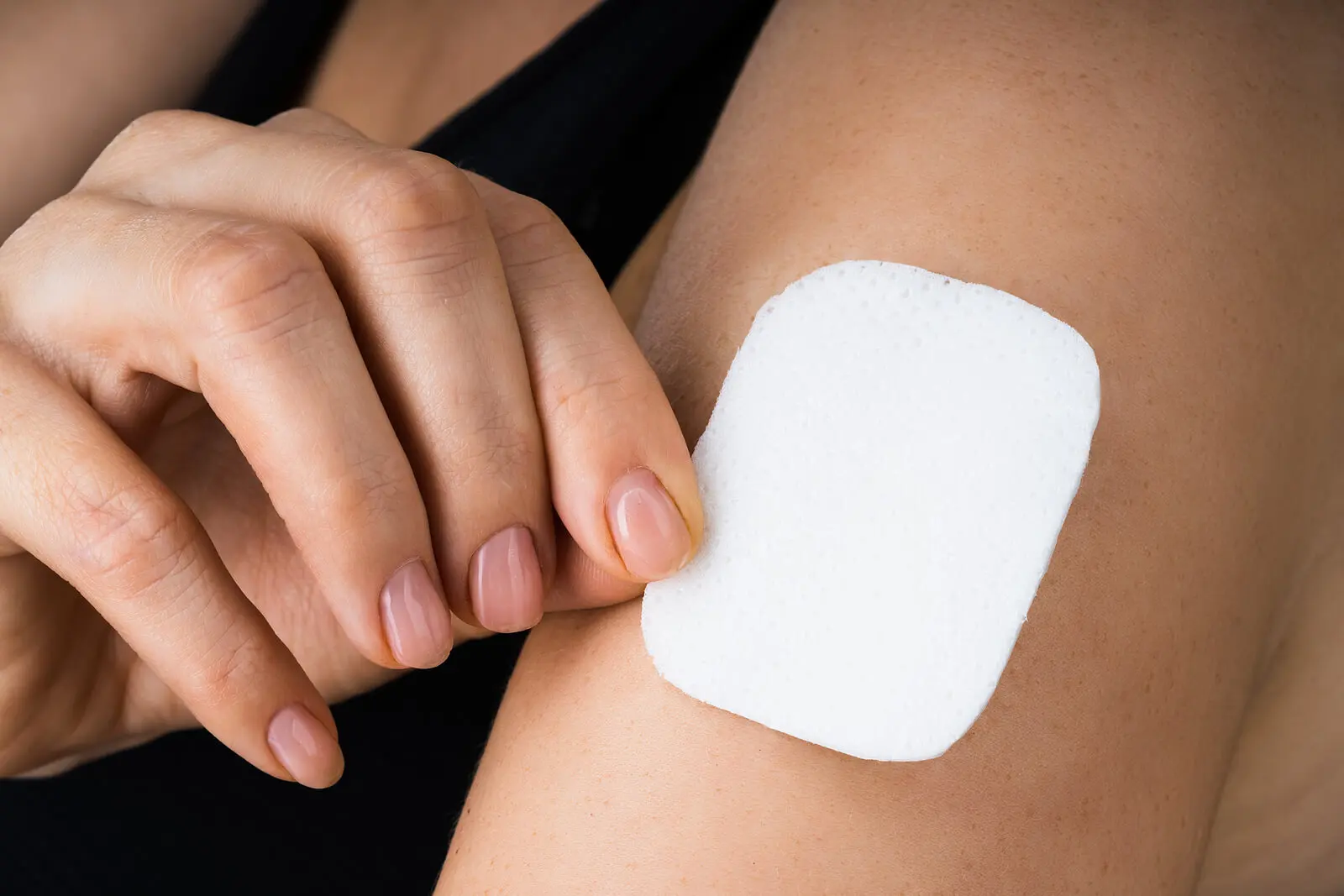
It’s a small square plate, composed of several layers. It can be placed on different parts of the body, such as the abdomen, buttocks, back, or arm. Once in contact with the body, the hormones are absorbed through the skin and pass into the bloodstream.
With all this, the following is sought:
- It prevents the ovaries from releasing eggs.
- There’s a thickening of the cervical mucus to make it difficult for sperm to travel to the ovaries.
- There’s a thinning of the walls of the uterus to prevent the implantation of a fertilized egg.
Therefore, this contraceptive method can help prevent an unwanted pregnancy. However, it should be clarified that it does not protect against sexually transmitted diseases.

We think you may also enjoy reading this article: The Billings or Cervical Mucus Method: What Is It and What are its Risks?
How is the contraceptive patch used?
Although it is apparently simple, the use of the contraceptive patch should not be taken lightly. In fact, it’s considered a prescription drug and should only be used with a doctor’s authorization.
If you’re interested in using it, you should know that its implantation process involves the following:
- A consultation with the gynecologist. During this consultation, you should express your interest in using the patch as a contraceptive method. If the professional agrees, the next step is to start using it on the first day of your menstrual period.
- Choose where to place it. It can be on one of the buttocks, biceps, abdomen, or back. You must avoid placing it in places where there’s friction.
- Clean the area. It’s necessary to sanitize the skin and dry it.
- Carefully remove the patch from its packaging. Make sure it is not damaged, cut, or soiled.
- Apply the adhesive part on the skin. Then, remove the protector it comes with.
- Press with your hand for a few seconds. This way, you make sure that it’s well adhered.
- Leave it on for a week. During this period, you should check its condition regularly to make sure that it is still fixed.
- Keep it on. Don’t remove it for showering, swimming, or exercising.
- Make the patch replacement. After the first week, replace the item with a new one. This should be done on exactly the same day of the week. Preferably, use the new one on another area of the skin to avoid irritation.
- Peel off one week. Do not apply the patch in the last week before your period.
The effectiveness and benefits of the birth control patch
If you follow the recommendations, the transdermal patch is effective in preventing pregnancy. However, if you’ve never used it before, you can supplement the first week with another method of contraception as a precaution.
Research reports that the overall annual chance of pregnancy is 0.8%, and method failure is estimated at 0.6%. That’s quite low, as it turns out. However, this may vary in overweight people. Compared to other methods, the following advantages stand out:
- It’s not necessary to interrupt sex to use it (as in the case of coitus interruptus);
- Since it’s a single weekly placement, and not a daily dose like the pill, it tends to be less likely to be forgotten.
- Unlike the implant, it’s not necessary to go to a doctor’s office to have it inserted.
- It doesn’t require the cooperation of the partner (as is the case of condoms).
- It can be discontinued at any time.
- It doesn’t cause weight gain.
- Like pills, it may help regulate your period and may control some PMS symptoms.
On the other hand, when there’s low hormone production, the use of the contraceptive patch can bring other health benefits related to problems such as acne, iron deficiency, cysts, and even the prevention of osteoporosis.
Like this article? You may also like to read: What Happens if I Vomit After Taking My Birth Control Pill?
What can affect its performance?
The effectiveness of the contraceptive patch can be affected by some factors, which could increase the possibility of getting pregnant. In this regard, the following recommendations should be taken into account.
Adherence
Ideally, it should be checked once a day to make sure it has adhered to the skin. If for some reason it comes off, do not try to put it back on again, even if you use reinforcement tape. In any case, it should be replaced with a new one.
As an added precaution, use a back-up method of contraception.
Irritation
Avoid placing the patches on irritated, reddened, or wounded skin. It’s advisable to change or alternate the area where it’s placed each time.
Clean the skin
In addition to cleaning the application area, lotions or creams should not be used, neither before applying the patch nor during the time it remains on the skin. This may affect its adherence.
Interaction
Certain medications or supplements may interact with the contraceptive patch, affecting its functioning. In this regard, the following are mentioned:
- Rifampin, rifampicin and rifamate (antibiotics)
- Griseofulvin (antifungal)
- HIV drugs (antiretrovirals)
- Anticonvulsants
- St. John’s wort
Obesity and the patch
As mentioned above, it is possible that effectiveness may decrease in women whose weight is greater than 90 kilograms or with a BMI close to or greater than 30.
Forgetting to change the patch
A mistake such as forgetting to put a new patch on time is usually one of the main reasons why a woman can become pregnant while using this method. If this happens, a backup contraceptive is needed.
Immersion in water
Being submerged in water for more than thirty minutes, whether at the beach, in a pool, hot tub, or in a bathtub, can affect adherence. If this happens, you should change it or use an additional method.
Scrapes or rubbing
Lastly, the patch should not be placed in an area where clothing is constantly rubbing against it. This contributes to the deterioration of the patch and decreases its ability to adhere well to the skin.
Contraindications of the contraceptive patch
When a woman wants to start using this type of method, she should inform her doctor if she is in any of the following situations:
- Pregnancy
- Lactation
- A recent abortion
- Use of medication for epilepsy or depression
- Diabetes
- High cholesterol
- Psoriasis or eczema
- Heart, kidney, or liver disease
The contraceptive patch is not recommended for all women. In this order of ideas, its use may be discouraged in the following cases:
- Smokers over 35 years of age
- Women with a history of heart attack or stroke
- Those who have problems such as angina pectoris, severe high blood pressure, or blood clots
- People with breast or cervical cancer.
- Complications with diabetes (such a neuropathy, diabetic retinopathy, or blood vessel damage)
- Jaundice during pregnancy or caused by hormonal contraceptives
Similarly, it’s recommended to discontinue use if you’re planning to undergo surgery.
Possible risks and side effects
The same side effects as oral hormonal contraceptives (pills) can occur with the patch. These include the following:
- Mood swings
- Acne
- Headaches
- Nausea
- The sensation of swollen breast
- Alterations in the menstrual cycle
- Bleeding or discharge
- Muscle spasms
In addition to this, there may be some skin reactions in the area where it is fixed or adhered. These include irritation, dryness, redness, itching, swelling, and rashes. Some of these effects may disappear within a few months, once the body gets used to the hormones.
However, some reviews mention other possible risks of hormonal contraception. The most frequent are mentioned below:
- Increased chances of clotting problems
- Vaginal infections
- High blood pressure
- Stroke
- Heart attacks
- Lliver cancer
- Gallbladder disease
When to see a doctor
If the following symptoms are observed, it is paramount to see a doctor or gynecologist as soon as possible.
- Chest pain
- Shortness of breath
- Leg pain
- Sudden loss of vision
- Jaundice
- Fever
- Changes in the appearance of urine
- Watery bowel movements
- Sleep disturbances
- Fatigue, discouragement.
- Acute abdominal pain
- The appearance of a breast lump
- Prolonged absence of the period
Discontinuation of use
If you wish to become pregnant or change your method of contraception, you can stop using the contraceptive patch at any time.
However, there may be some temporary side effects, such as headaches, irregular periods, etc. You should consult your doctor if you have any questions.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Courtney K. The Contraceptive Patch: Latest Developments. Nursing for Women’s Health, Volume 10, Issue 3, 250 – 254
- Etchepareborda J. Anticoncepción hormonal. Riesgos y beneficios. Revista SAEGRE. 2011; XVIII(3): 30-43.
- Galzote RM, Rafie S, Teal R, Mody SK. Transdermal delivery of combined hormonal contraception: a review of the current literature. Int J Womens Health. 2017 May 15;9:315-321. doi: 10.2147/IJWH.S102306. PMID: 28553144; PMCID: PMC5440026.
- Orizaba-Chávez B, Alba-Jasso G, Ocharán-Hernández M. Farmacocinética de la progesterona. Rev Hosp Jua Mex. 2013; 80(1): 59-66.
- Torres Serna C. Anticonceptivos hormonales y su interacción con otros medicamentos. En: Cifuentes Borrero R., Anticoncepción en situaciones especiales. Bogotá: Federación Colombiana de Asociaciones de Obstetricia y Ginecología, 2006. Capítulo 34
- Valdés-Bango M, Castelo-Branco C. Anticoncepción con solo progestina. Ginecol Obstet Mex. 2020; 88(Suppl: 1): 56-73.
- Zieman M, Guillebaud J, Weisberg E, et al. Contraceptive efficacy and cycle control with the Ortho Evra/Evra transdermal system: the analysis of pooled data. Fertil Steril. 2002; 77(2 Suppl 2): S13-8. doi: 10.1016/s0015-0282(01)03275-7.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








