5 Types of Skin Fungus and How to Identify Them


Reviewed and approved by the doctor José Gerardo Rosciano Paganelli
Taking care of our skin is important for many reasons. First, it’s the protective layer of our body, and keeping it well cared for will also protect the rest of our body. In addition, any damage it suffers, whether from skin fungus or other causes, is easily visible, compromising our comfort and personal image.
That’s why it’s vital to protect ourselves from skin fungus and know how to identify if we suffer from any infection that needs medical attention. This way, we can cure it quickly and avoid consequences or permanent skin damage.
Are all skin fungi the same?
Just as there are no single animal or plant species, the kingdom of fungi is also made up of many different organisms. Some of them can affect humans and cause skin infections.
Overall, we can talk about the five types of fungi that commonly cause stains, itching, and even pain when it comes to skin infections.
Read this article: Learn How To Treat Foot Fungus With These Home Remedies
1. Tinea skin fungus

Dermatophytes grow best in a warm, moist environment and are most common in tropical and subtropical regions. They also multiply in enclosed or poorly ventilated spaces, clothing subject to excessive sweating, sports and exercise equipment, etc.
Dermatophytes generally grow only in tissues containing keratin or “dead tissue,” such as hair, nails, and the outer layer of the skin. They also stop spreading when they come into contact with living cells or areas of inflammation.
These fungi are transmitted by contact with the fungus on another host. Infection usually starts in the developing hair or the outermost part of the skin, known as the “stratum corneum,” and spreads from there.
Tinea is classified according to the area of the body it affects. For example, tinea torsorum or capitis affects the hair and scalp. Tinea corporis attacks the tissue of the trunk, limbs, and face. Ringworm of the hand is another common infection that affects the palms and is scaly.
A very common type of ringworm is ringworm of the foot, better known as “athlete’s foot.” Warm, humid environments: sports equipment and clothing, gym locker rooms are ideal for these skin fungi. However, anyone is prone to suffering from this infection.
How to identify this type of fungus?
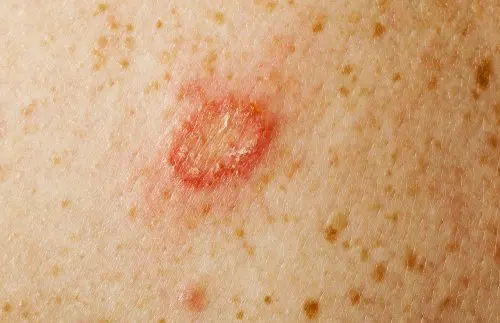
You can tell if you have ringworm problems if you present:
- Itching or burning
- Ring-shaped redness of the skin
- Blistering
- Scaly or peeling skin
- Breakdown or softening of the affected area
2. Candida
Candidiasis is an infection caused by yeast. It’s a very common fungus, present even in the human body.
The infection occurs when our body’s antibodies can’t defend us from these fungi on the skin. This can occur when we have low defenses or when we take antibiotics.
Although this type of infection can affect any part of the body, it appears mainly in areas of the skin with folds, such as the armpits, the lower part of the breasts, groin, etc. When it occurs on the skin, it’s called cutaneous candidiasis.
Yeast also affects the mucous membranes: the genitals, mouth, tongue, and even in extreme cases, the esophagus and lungs. Candida is the main cause of dermatitis in babies due to the moisture that remains in their diapers.
Discover: Two Ingredients That Can Inhibit Nail Fungus Growth and Spreading
How to identify this type of fungus:
- Redness and rash
- Itching or burning
- White discharge from the affected area
- Pain and discomfort
- Change of color, weakening, stretch marks, thickening, or loss of nails
3. Nail fungus
Fungal infections can also affect the nails, which they’re referred to as onychomycosis. Many of the etiological agents are dermatophytes, so they can be included in the tinea category and be called tinea unguium. However, it can also be due to other fungi that affect the skin, such as mold and yeast.
According to multiple studies, onychomycosis is the most common nail infection and accounts for up to 30% of all cases. Anyone can suffer from this infection. However, diabetics and those who are uncompromised are at a higher risk.
Fungi most often affect the toenails. They can be located in the nail unit itself, affect the surrounding skin, and spread to other nails. Unfortunately, treatment of this mycosis is difficult and often requires a combination of topical and oral therapy.
How to identify this type of fungus
Identification of onychomycosis is very simple, even in the early stages of the disease. The affected nail usually changes color, becoming whiter or yellowish.
The shape of the nail is also altered. In some cases, it’s possible to observe a nail weakening, which increases the likelihood of the nail breaking. However, some fungi are capable of causing a thickening of the nail. This type of infection does not usually cause pain in the affected nail unless the case is very severe.
4. Pityriasis versicolor
Pityriasis Versicolor is a fungal infection of the skin caused by yeasts. The most common etiological agent is a yeast known as Malassezia furfur. It can be found on the skin as part of the normal flora. However, it can become pathogenic under certain conditions.
The fungus can produce a special substance called azelaic acid, which prevents melanin production, causing the characteristic symptomatology. This disease has a universal distribution. However, studies show that it’s more frequent in tropical and subtropical countries.
The characteristic lesions of Pityriasis Versicolor can appear anywhere on the body. One of the most common locations is on the chest, but it can also be seen on the neck, face, and arms.
How to identify this type of fungus
The main symptom of this fungal skin infection is the presence of whitish or yellowish spots. The spots tend to increase in size gradually. The lesion may be round or oval, and slight scaling may be visible.
The condition does not usually cause other symptoms, although some people may experience itching or stinging the lesions. Fortunately, the state may disappear on its own by the end of the summer in countries with temperate climates.
5. Sporotrichosis
This common fungal infection from Latin America is caused by a mold called Sporothrix schenckii. The etiological agent inhabits different moss, rose bushes, manure, and hay bales. Its distribution means that the most affected population is gardeners and farmers.
The fungus penetrates the skin through small cuts, usually due to prickles with plant thorns. Fortunately, this fungus can’t be transmitted from person to person. In addition, hematogenous spread to other tissues is rare, so the lesions are usually confined to a specific area.
How to identify this type of fungus
The primary lesion manifests as a lump or abscess of variable size, located in the area where the fungus entered the body. It is painless and will progressively increase in size. The number of bumps may gradually increase and reach a variable number.
As the days go by, the lesions become necrotic and similar to a boil. Furthermore, they often evolve into ulcer-like lesions that take a long time to heal.
Prevention of skin fungus is essential
The best way to protect yourself from skin fungus is to avoid contact with other infected people, their clothes, and personal items.
It’s also essential to maintain excellent personal hygiene, as most fungi are part of the normal flora. If you notice that you’re suffering from a fungal skin infection, see your doctor for a prescription for an antifungal medication.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Molina de Diego, A. (2011). Aspectos clínicos, diagnósticos y terapéuticos de las dermatofitosis. Enfermedades Infecciosas y Microbiología Clínica, 29, 33-39. https://doi.org/10.1016/s0213-005x(11)70025-8
- Garrote, A. (2002). Micosis cutáneas. Revista Offarm, 21(8), 82-90. https://www.elsevier.es/es-revista-offarm-4-articulo-micosis-cutaneas-13035868
- Suárez, S. (2002). Dermatitis del pañal. Abordaje eficaz. Farmacia Profesional, 16(11), 52-57. https://www.elsevier.es/es-revista-farmacia-profesional-3-articulo-dermatitis-del-panal-abordaje-eficaz-13041486
- Mendoza, N., Palacios, C., Cardona, N., & Gómez, L. M. (2012). Onicomicosis: afección común de difícil tratamiento. Revista de la Asociación Colombiana de Dermatología y Cirugía Dermatológica, 20(2), 149-158. https://doi.org/10.29176/2590843x.224
- Walter Gubelin, H., Rodrigo de la Parra, C., & Laura Giesen, F. (2011). Micosis superficiales. Revista Médica Clínica Las Condes, 22(6), 804-812. https://doi.org/10.1016/s0716-8640(11)70493-x
- Rubio, G., Sánchez, G., Porras, L., & Alvarado, Z. (2010). Esporotricosis: prevalencia, perfil clínico y epidemiológico en un centro de referencia en Colombia. Revista Iberoamericana de Micología, 27(2), 75-79. https://doi.org/10.1016/j.riam.2010.01.001
- Ramírez-Godínez, J. B., Carreño-Gayosso, E. A., Soto-Ortiz, J. L., Tarango-Martínez, V. M., & Mayorga-Rodríguez, J. A. (2017). Pitiriasis versicolor: una actualización. Medicina cutánea ibero-latino-americana, 46(3), 166-175. https://www.medigraphic.com/pdfs/cutanea/mc-2018/mc183b.pdf
- Segundo-López LD, Sierra-Maeda KY, Arenas R. (2021). Onicomicosis en la población diabética: importancia de las complicaciones, tratamiento y prevención . Dermatología Cosmética, Médica y Quirúrgica;19(3):289-295. Consultado el 24 de marzo de 2023. https://www.medigraphic.com/cgi-bin/new/resumen.cgi?IDARTICULO=102292
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








