Swimmer's Itch: Causes, Symptoms and Treatment

Written and verified by the doctor María Irene Benavides Guillém
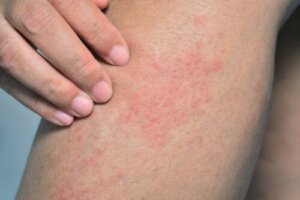
Swimmer’s itch, cercarial or schistosome dermatitis, is an allergic skin reaction to cercariae, which are the larvae of a waterfowl parasite (bird schistosomes).
It’s a condition that has few studies, but recently there has been growing interest since the World Health Organization (WHO) lists it as an emerging disease. There are reports of cases and outbreaks of swimmer’s itch in all parts of the world, including North and South America, Europe, and Asia.
In research by Lashaki et al. reviewing 41 studies conducted between 1937 and 2017 in different countries, they determined that at least 34% of waterfowl worldwide are infected with schistosomes.
The main symptoms
As mentioned, swimmer’s itch is, in essence, an allergy. So there’s an initial phase in which contact with the parasite is made and sensitization to the parasite occurs.
In later episodes, the dermatitis itself will occur, due to the reaction of the immune system against something it recognizes, i.e. cercariae.
As the name suggests, the main symptom of swimmer’s itch is itching. It ranges from tolerable to unbearable, to the point of sleeplessness.
Continue reading: Living with Dust Allergy
Chronology of skin lesions
Swimmer’s itch produces a series of rashes that follow one after the other at characteristic times:
- Immediately after contact there may be itching, tingling, and burning at the site where the cercariae penetrated.
- Then, a spot or macule of 1 to 2 millimeters in diameter appears at this same site, which may persist for several hours.
- After 10 to 15 hours there’s a cutaneous eruption with welts, small pimples, blisters, and papules, three to five millimeters in diameter.
- Between the second and third day, vesicles appear.
- One week after penetration the papules disappear and a small red spot remains.
Scratching causes symptoms to increase. Scratching releases more histamine and the itching increases. In addition, the lesions can become infected by bacteria, making the situation worse.

Is it a serious disease?
The presence and intensity of the symptoms of swimmer’s itch depend on three factors:
- Whether it’s the first contact with cercariae or the person who was previously exposed. The greater the exposure, the more significant the sensitization and the more florid the symptoms.
- The number of cercariae contacted.
- The genetic and immunological susceptibility of the person.
- When many cercariae have penetrated, there may be fever, swelling or inflammation of the joints, nausea, and diarrhea. If the episode of dermatitis is very severe or is repeated continuously, it may become a chronic condition.
What causes swimmer’s itch?
Cercariae are known as duck bites or duck lice. But they aren’t actually lice, but larvae of different species of flatworms or flatworms called bird schistosomes.
The parasite develops in any aquatic environment where certain species of snails are present and act as intermediate hosts. Birds are the definitive hosts; most frequently ducks, geese, and swans.
Macháček et al. reported the presence of cercariae in small artificial water bodies at a university in Prague, Czech Republic. In other words, these parasites are present in natural or artificial, rural or urban areas.
Infection
The larvae emerge from the snails in search of birds’ feet, heading for the surface, responding to sunlight. The infection occurs in humans when they come into contact with water, but aren’t the target of cercariae.
Our body temperature, similar to that of birds, attracts the parasite. However, when it penetrates the human skin, it ends up dying, generating a reaction that is what causes swimmer’s itch.
The release of larvae is higher in the morning hours, when birds are usually in the water. Also, in warmer temperatures. For this reason, outbreaks usually occur in spring and summer. However, it doesn’t spread from human to human.
Who’s at risk for swimmer’s itch?
Swimmer’s itch affects people who are exposed to cercariae for recreational or occupational reasons. It’s most often described in children, as they bathe shallower, closer to shore, and for longer periods of time.
In addition, it’s common in rice farmers and may appear after cleaning aquariums containing snails with the parasite.
How can it be diagnosed?
Although swimmer’s itch usually follows a characteristic pattern, with specific times of appearance of the lesions, the disease may go unnoticed.
On the other hand, specialists and patients easily confuse it with other issues, such as contact dermatitis, insect bites, and bacterial skin infections.
The appearance of lesions limited to areas of the body immersed in water and a history of swimming in a lake or pond in the previous 96 hours are usually the key data that make us think of cercarial dermatitis or swimmer’s itch.
Find out more: Tips to Prevent Skin Diseases
Are there laboratory tests for the diagnosis of swimmer’s itch?
There aren’t any laboratory tests that are diagnostic of the disease. Alterations may occur in routine blood tests, such as those seen in other parasitic or allergic issues, but they aren’t always there.
Moreover, they aren’t very useful in the absence of medical suspicion and a clear history of exposure. Additionally, tests that detect the parasite in blood or other body fluids aren’t available either.

Treatments available
Treatment of swimmer’s itch focuses on symptom relief. For example, antiparasitic drugs aren’t indicated because, as we explained, the parasite dies in contact with the dermis.
You should take the following measures into account in case of cercarial dermatitis:
- Avoid scratching, as it aggravates the condition and favors infection by bacteria.
- Use cold compresses to relieve itching.
- In case the allergic reaction is very strong or the itching is unbearable, we suggest going to the doctor. They may prescribe allergy medications.
- Be very careful with applying creams, natural herbal products, and oily substances without medical indication. Specialists don’t recommend these practices because they may increase dermatitis.
Preventing swimmer’s itch
In conclusion, to protect yourself against contact with cercariae, we recommend you avoid swimming on shallow shores, places with abundant vegetation, and early in the morning. As described above, these circumstances facilitate exposure to the parasite.
Wearing appropriate swimsuits that leave the least amount of skin uncovered is also a good practice, as well as sunbathing after getting out of the water.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Lashaki EK, Teshnizi SH, Gholami S, Fakhar M, Brant SV, Dodangeh S. Global prevalence status of avian schistosomes: A systematic review with meta-analysis. Parasite Epidemiol Control. 2020;9:e00142.
- Macháček T, Turjanicová L, Bulantová J, Hrdý J, Horák P, Mikeš L. Cercarial dermatitis: a systematic follow-up study of human cases with implications for diagnostics. Parasitol Res. 2018;117(12):3881-3895.
- Veleizán A. A. y Flores V. El piojo de pato, la cercaria y la dermatitis cercarial. Desde la patagonia difundiendo saberes 2017;14(23):2-7.
- Horák P, Mikeš L, Lichtenbergová L, Skála V, Soldánová M, Brant SV. Avian schistosomes and outbreaks of cercarial dermatitis. Clin Microbiol Rev. 2015;28(1):165-90.
- Kolářová L, Horák P, Skírnisson K, Marečková H, Doenhoff M. Cercarial dermatitis, a neglected allergic disease. Clin Rev Allergy Immunol. 2013;45(1):63-74.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








