Pyramidal Syndrome or False Sciatica, What Does it Consist Of?


Written and verified by the doctor Leonardo Biolatto
Pyramidal syndrome is also called false sciatica because it causes symptoms that are confused with low back pain. It occurs due to an overload of the pyramidal muscle that ends in contracture of the same, with the consequent compression of the sciatic nerve.
This pathology is more frequent among women and its greater incidence takes place around 40 and 50 years of age. However, it can appear at any age. In fact, even though it is associated with runners and athletes, poor posture is another possible cause.
The difference between pyramidal syndrome and real sciatica is very important. Both the complications and the treatment will be different in relation to one entity or the other.
What is pyramidal syndrome or false sciatica?
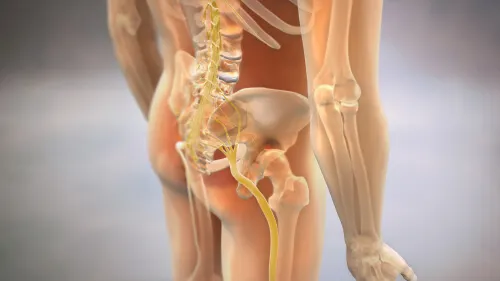
The pyramidal muscle is a small anatomical structure located in the pelvis. It is so named because it has the shape of a triangle, which begins at the sacrum and extends to the femur. It’s part of the gluteus and is responsible for the movement of the external rotation of the leg.
The sciatic nerve, for its part, has a path that leads to the leg contacting this muscle. In fact, there are people with a particular constitution, in whom the nerve crosses the pyramidal muscle. So much so, that the space between both structures is very small.
In pyramidal syndrome, the muscle increases in size and compresses the sciatic nerve. This increase may be due to muscle overload, for example, due to exercise. Contractures are also to blame.
On the other hand, in true sciatica, the nerve is actually compressed in the upper part of its course, generally with contact over the vertebrae of the spine. Sciatic pain is more permanent, insidious, and persistent.
As a difference, pyramidal syndrome or false sciatica tends to be transitory. Since it’s a contracture or muscular overload, time resolves it. But in low back pain, herniated discs are the main cause, and therefore become chronic.

You might like to read: 5 Ways to Relieve Sciatica Symptoms
What are the symptoms of pyramidal syndrome?
Pyramidal syndrome manifests itself with pain in the buttock and leg. Sometimes it extends to the groin or around the hip. However, the pressure of the muscle must be very high for it to spread.
In sciatica, on the other hand, the pain spreads and radiates away from the point of origin, reaching as far as the foot. In pyramidal syndrome, or false sciatica, the discomfort is more localized, over the buttock.
In addition, there’s often some swelling in the area. This will be perceived from the outside as an enlargement in some region of the buttock, sometimes as a palpable area that increases the pain when it comes into contact with a chair, for example. In extreme situations, even the very rubbing of clothing is painful.
Pain usually occurs when walking or sitting for a long time. One of the most typical signs of pyramidal syndrome or false sciatica is that the sufferer cannot cross the affected leg over the other.
In order to establish the diagnosis, it’s important for the physician to determine the characteristics of the patient’s pain through a series of questions. It’s difficult to establish the presence of alterations in the pyramidal muscle by means of images.
However, tests can be requested to rule out real sciatica. Magnetic resonance imaging and X-rays are used to check for alterations at the lumbar level or in the path of the nerve.
You may be interested in: Infusions and Tips To Relieve Sciatica Symptoms
How is false sciatica treated?
Pyramidal syndrome, or false sciatica, is usually treated with physiotherapy. Stretching and exercises that improve muscle contractures are recommended. It’s also important to correct posture, especially when sitting.
Analgesics and non-steroidal anti-inflammatory drugs can be taken to relieve pain. In case these measures don’t work, corticosteroid or botulinum toxin injections in the muscle area have been used on a trial basis, still with debatable results.
There are few cases that require surgery. However, the final decision will be made by a specialist. The first steps are to rule out other pathologies that may be behind the symptoms, and to initiate a conservative approach, with physiotherapy and lifestyle changes.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Sánchez, VE Ortiz, et al. “Síndrome piramidal y variaciones anatómicas como causa de dolor ciático insidioso.” Revista Española de Anestesiología y Reanimación 61.9 (2014): 521-524.
- Maslo, Philippe. Las dolencias de espalda: hernia, lumbago, ciática, tortícoles. Editorial Paidotribo, 2001.
- Limonta Cruzata, María Emilia, Carlos Mario Alejandrez Leyva, and Yuneisys Coronados Valladares. “¿ Quiénes padecen el síndrome del piramidal?.” Revista Cubana de Medicina Física y Rehabilitación 11.2 (2019): 1-5.
- Ruiz-Arranz, J. L., I. Alfonso-Venzalá, and J. Villalón-Ogayar. “Síndrome del músculo piramidal. Diagnóstico y tratamiento. Presentación de 14 casos.” Revista Española de Cirugía Ortopédica y Traumatología 52.6 (2008): 359-365.
- Acuña Morales, Sara. “Tratamiento lumbociatalgia inespecífica y síndrome del piriforme. Revisión bibliográfica.” (2016).
- Mendoza, Israel Gutiérrez, et al. “Síndrome del piramidal (piriforme).” HISTORIA 10.2 (2014).
- Castro, M., et al. “Tratamiento del síndrome de dolor miofascial con toxina botulínica tipo A.” Revista de la Sociedad Española del Dolor 13.2 (2006): 96-102.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








