8 Misunderstood Aspects of Alzheimer's Disease


Written and verified by the doctor Maryel Alvarado Nieto
Alzheimer’s disease (AD) is the leading cause of dementia of neurodegenerative origin in the world. It’s also the best known and most studied of the diseases that fall into this category, although there are still several aspects to be clarified.
It’s quite common that both patients and many of the people in their close environment have access to untruthful information about this disease. This complicates the picture of Alzheimer’s disease (AD).
The purpose of this article is to clarify the main questions that arise with the diagnosis in order to understand the disease and its progression more honestly. This is especially because the symptoms worsen with the passage of time since this is a degenerative disease.
It’s for this reason that it’s a part of a group of entities grouped under the term dementia. They lead to the patient’s inability to cope with everyday life tasks.
1. Genetics and Alzheimer’s disease
While it’s true that AD has a hereditary component, it’s also true that it’s considered a multifactorial disease. This implies that in order for it to develop, several factors involved in its occurrence must interact and not just one in isolation.
Among these risk factors, the most important is age. It’s more frequent after 65 years of age, in the female sex, and when Down syndrome is also present.
Due to this multiple origin, it’s not correct to assume that having a parent with Alzheimer’s disease implies a sentence of AD for the children. However, neither is it correct to underestimate the hereditary component observed in patients.
It’s estimated that about 40% of people with Alzheimer’s disease have a family history of this type of dementia after 65 years of age.

2. Alzheimer’s disease and senescence
Another common myth is that Alzheimer’s disease only appears in older people. This is because in most cases this is the form of presentation.
However, there’s a variant of dementia in which symptoms begin in young people. Although this group includes all patients under 65 years of age, clinical manifestations may debut as early as 30 years of age.
In addition, the clinical course of early-onset Alzheimer’s disease usually follows a torpid and devastating course. Therefore, it has a worse prognosis than the late-onset form. Furthermore, despite being a rare form of this disease, a clear genetic component has been demonstrated in early AD.
We think you may also enjoy reading this article: The Differences between Dementia and Alzheimer’s
3 Is Alzheimer’s disease a synonym for dementia?
Since AD is the most common cause of dementia of degenerative origin, it’s common to assume that they correspond to the same disease. However, not all types of dementia is caused by Alzheimer’s.
Apart from AD, other pathologies causing the major neurocognitive disorder known under the term dementia are the following:
- Dementia with Lewy bodies
- Frontotemporal dementia
- Dementia associated with Parkinson’s disease
In each of these conditions, the clinical manifestations are going to depend on the affected neuronal area. Likewise, the risk factors, characteristics, and pathophysiology are different for each of them.
However, they’re classified as dementia because they lead to progressive neurocognitive impairment, which interferes with the performance of daily activities for patients. All of them require the support of a caregiver.
Like this article? You may also like to read: Alzheimer’s Disease and Sleep Pattern Changes
4. Is the treatment for Alzheimer’s disease effective?
One of the most frightening aspects for patients and relatives is that there’s currently no cure for Alzheimer’s disease. Even so, there are drugs prescribed to minimize cognitive symptoms, but they don’t offer a definitive solution.
This has sometimes led to the postponement of early treatment. There’s a fatalistic assumption that the disease progressing is inevitable.
However, after diagnosis, it’s necessary to establish a timely therapeutic regimen. For this, it’s key to turn to these drugs, since they’ve proven effective in the management of manifestations by allowing a significant improvement in functionality.
Also, although their benefit is modest and much research remains to be done, it’s wrong to deny patients the possibility of treatment, especially knowing that it exists.
5. Is it possible to prevent Alzheimer’s disease?
The prevention of AD is a complex issue to address. There are multiple opinions on the subject.
Countless publications share miracle diets, physical exercises, and magical alternative therapies on how to prevent the development of the pathology. However, none of these options offers a realistic contribution to the prevention of Alzheimer’s because its origin is multifactorial.
For this reason, research on the individual risk factors involved has been difficult. However, studies have been conducted to establish preventive measures to at least postpone the age of onset.
The symptomatology is the result of neuronal involvement that occurs over decades. It’s not a condition with sudden onset.
Associated risk factors
Regardless of the complexity of studying each factor, some authors propose the incorporation of a healthier lifestyle in order to reduce the risk of Alzheimer’s disease. Despite these suggestions, there’s still no consensus that guarantees effective prevention.
Among the most widely accepted recommendations are the following:
- Maintain a stimulating intellectual development
- Include regular physical exercise routines
- Eat a balanced diet rich in fruits, vegetables, fish, and vegetable proteins
- Participate in social and cultural events at different stages of life
- Control blood pressure, obesity, and diabetes
- Reduce your alcohol and tobacco consumption
6. Definitive diagnosis of Alzheimer’s disease: An impossible task?
Another aspect of concern for newly diagnosed patients and their families is the accuracy of the diagnosis. The reason is that the histological brain changes that define the disease may only be evident in an autopsy.
This concept is still very relevant. However, nowadays, a better understanding of AD has led to the creation of valid criteria that decrease diagnostic errors.
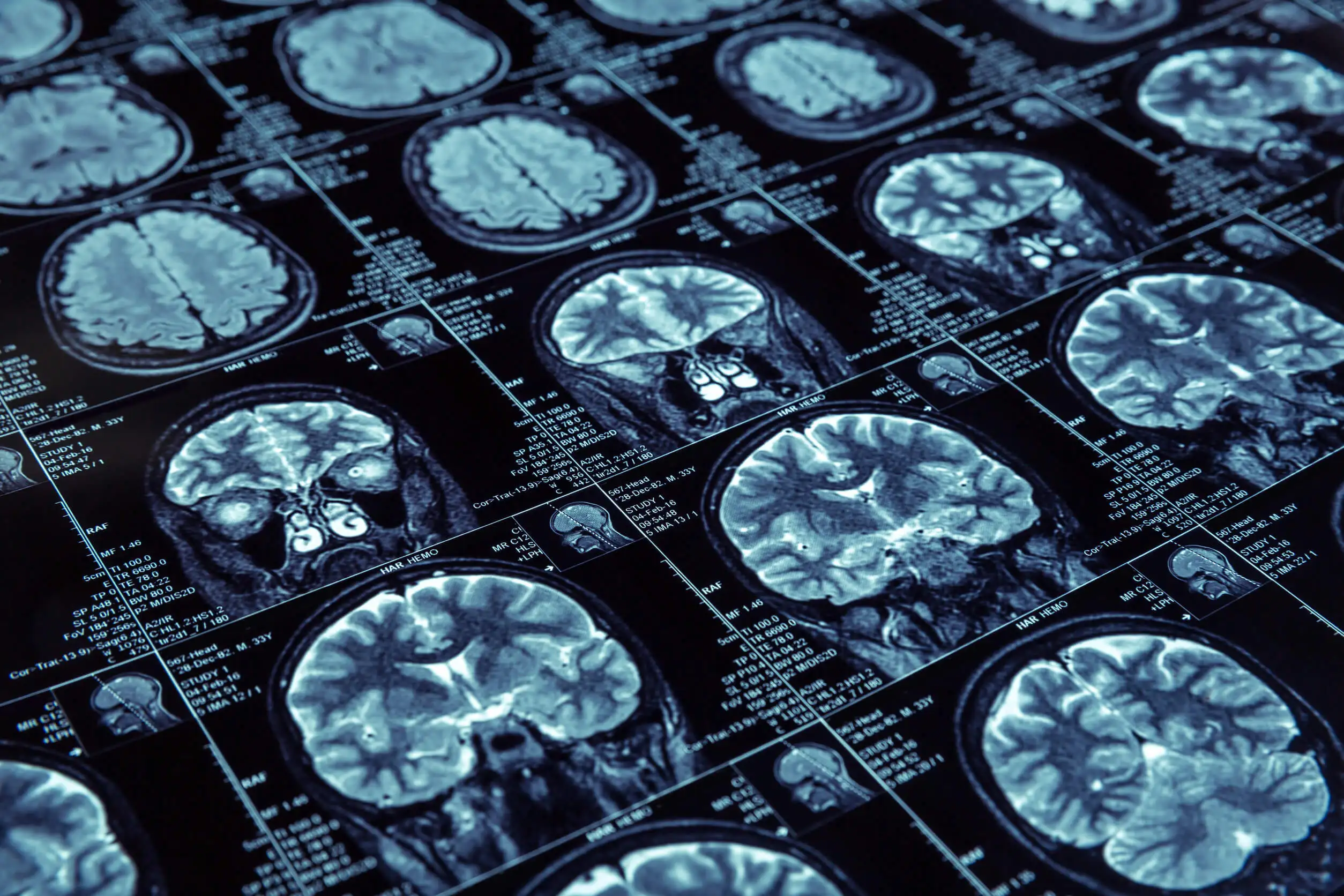
Furthermore, it’s possible to detect such histological changes without resorting to postmortem confirmation. This is done through biomarkers detected in complementary tests. Among these studies are lumbar puncture and imaging with magnetic resonance imaging (MRI) and positron emission tomography (PET).
7. Alzheimer’s disease doesn’t define a person
The person’s own perception of their disease is another relevant aspect. This has been examined in an article by the Alzheimer’s Association, with the aim of demystifying the disease and reducing the stigma attached to the diagnosis.
Something as burdensome as the diagnosis itself – which patients must deal in the early stages – often leads to the assumption by those close to them that AD means they’re going to stop being independent. Although this reaction may initially be reasonable, it should be avoided. Cognitive loss is progressive over time, so the patient’s personality doesn’t simply evaporate with the diagnosis.
8. Minimizing the symptoms of Alzheimer’s disease
It’s always important to consider the well-being of someone who deals with the disease on a daily basis, so certain comments should be avoided. Some people with the disease claim that many other people underestimate the diagnosis, often questioning the person’s age or assuming that their concepts about it aren’t correct.
Finally, although it’s possible that there’s no bad intention in doing so, the reality is that it doesn’t really help the person with this disease. Information is always the best tool.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Domarus, A.; Farreras, P.; Rozman, C.; Cardelach, F.; Nicolás, J; Cervera, R.; Farreras Rozman. Medicina Interna; 19na Edición; Elsevier; 2020.
- Sacristán, P.; Aspectos Genéticos de la Enfermedad de Alzheimer; Universidad de León – Facultad de Ciencias Biológicas y Ambientales; 2021.
- Tellechea, P.; Pujol, N.; Steve, P.; Echeveste, B.; García, M.; Arbizú, J.; Riverol, M.; Enfermedad de Alzheimer de Inicio Precoz y de Inicio Tardío: ¿Son la Misma Entidad?; Sociedad Española de Neurología; 2015.
- López, Ó.; Tratamiento Farmacológico de la Enfermedad de Alzheimer y otras Demencias; Archivos de Medicina Interna; 37 (2); 2015.
- Orueta Sánchez, Ramón. “Los medicamentos para la enfermedad de Alzheimer a debate. El papel del médico de familia.” Revista Clínica de Medicina de Familia 12.3 (2019): 113-114.
- Bermejo, F.; Llamas, S.; Villarejo, A.; Prevención de la Enfermedad de Alzheimer: un Camino a Seguir; Sociedad Española de Medicina Interna; 2016.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








