Mandibular Prognathism: What Is It and How Is It Corrected?

Written and verified by the dentist Vanesa Evangelina Buffa
There are several situations and disorders that can affect people’s bite and the harmony of their smile and face. Mandibular prognathism is one of these alterations. What is it? What are its main causes?
This is a condition that’s characterized by the presence of a lower jaw that’s too large or too far forward in relation to the upper jaw. The jaw protrudes and affects occlusion and facial aesthetics. We’ll tell you more about it in this article.
What is mandibular prognathism?
The word “prognathism” comes from the Greek “pro,” which means “forward,” and “gnathos,” which means “jaw.” This disorder is also known as “skeletal class III malocclusion.”
As we already told you, it’s the extension or protrusion of the lower jaw forward. This protrusion causes the chin to protrude excessively and noticeably on the face. Often, this is due to excessive growth of the lower jaw.
However, it can also be caused by the lack of development of the upper bone that is located far behind. Thus, the upper and lower teeth cannot relate properly.
The causes of mandibular prognathism
The most common origin of mandibular prognathism is usually genetic and hereditary. It’s common for people born with a larger lower jaw to have relatives with the same problem.
Therefore, if there’s a family history, it’s important to take children to the dentist and orthodontist at an early age. In this way, it will be possible to detect the problem in order to address it early.
In any case, some external situations may favor the appearance of this condition. Premature loss of milk teeth is an example. Tonsil or adenoid hypertrophy and mouth breathing are other factors that increase the chances of prognathism.
Sometimes it can also be a symptom of other systemic diseases. Acromegaly, for example, is a disorder in which there’s excessive growth hormone production and the jaw is usually larger.
People with Down syndrome and other rarer disorders, such as Crouzon syndrome, Nevus syndrome, and conditions such as acrodysostosis also often have prognathism.
The symptoms of mandibular prognathism
The most notable feature of this condition is a protruding chin. However, this disorder generates several other symptoms, such as the following:
- Malocclusion: The incorrect relationship of the jaws to each other affects the bite and the position of the teeth in the mouth. The teeth of the lower arch close outside and in front of the upper teeth. Sometimes, an open bite can be generated when the person fails to close their jaw correctly.
- An alteration of oral functions: A person with mandibular prognathism often has problems when biting, chewing, eating, and speaking. Diction problems, such as lisping, tend to be frequent.
- Problems in the temporomandibular joint.
- Frequent headaches.
- Aesthetic problems: A pronounced chin can be an aesthetic inconvenience for some people who don’t feel comfortable with its appearance. This can lead to feelings of insecurity, low self-esteem, and difficulties relating to others.
How is mandibular prognathism diagnosed?
The diagnosis of mandibular prognathism is usually suspected by the dentist and confirmed by an orthodontist. When the general dentist discovers signs of this condition, he/she makes an referral to the specialist for the resolution of the problem.
The physical examination and the clinical history data – such as family history and certain oral habits – are important when arriving at the diagnosis. However, other resources are also necessary to help the professional confirm the diagnosis.
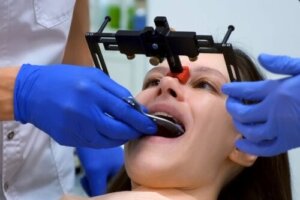
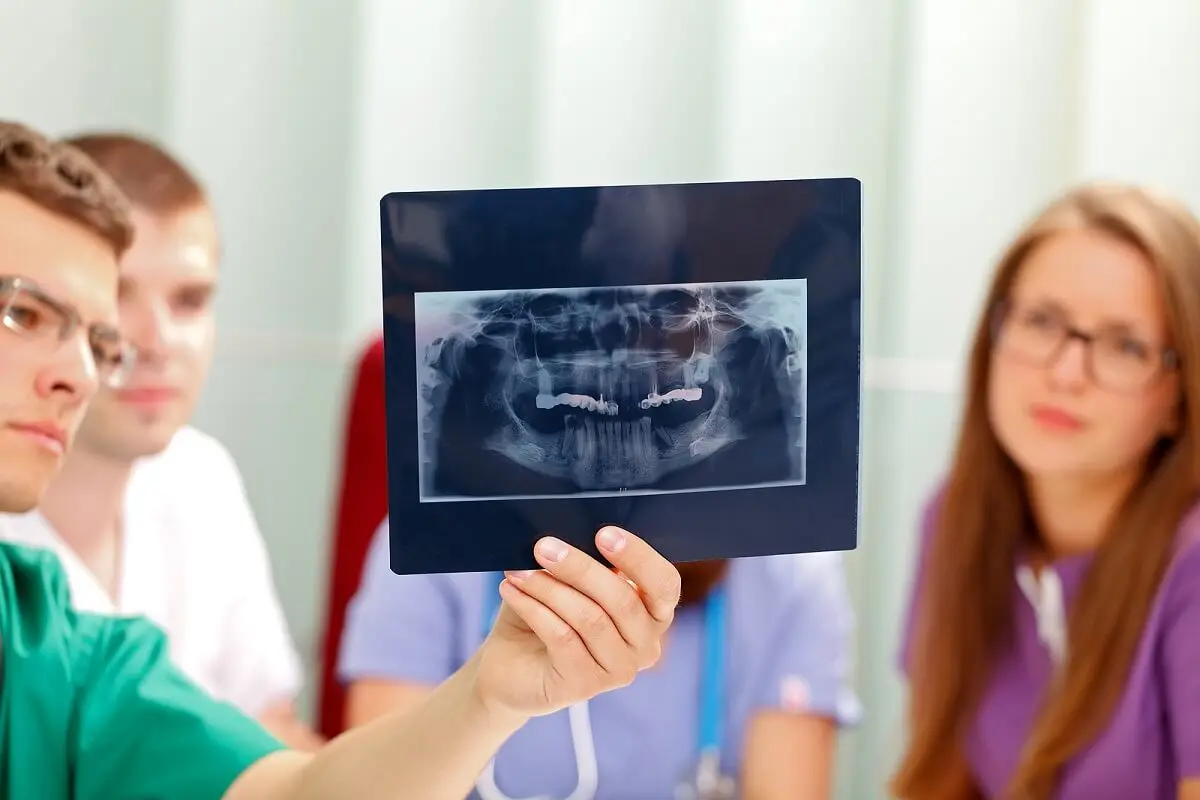
Dental and cranial radiographs, such as orthopantomography and cephalometry, contribute to the study of the problem. Intra- and extra-oral photographs also provide valuable information.
Bite impressions and obtaining a study cast complete the diagnostic process. The practitioner can plan the most appropriate treatment for each individual patient from this.
If an underlying medical condition causes mandibular prognathism, the dentist will suggest timely treatment for that condition with the appropriate specialist.
We think you may also enjoy reading this article: How to Easily Whiten Your Teeth with Natural Products
How is it treated?
The therapeutic alternatives when addressing a skeletal class III occlusion problem depend on the age of the patient. It’s not the same to treat it in a child or an adolescent – whose bones have not yet finished growing – as in an adult who’s already completed this formative process.
It’s less invasive and more conservative when treatment is carried out during childhood. In addition, it prevents the symptoms of this condition and its functional, aesthetic, and psychological effects from being prolonged over time.
For this reason, it’s recommended to take children to a pediatric dentist from the first year of life and to have a consultation with the orthodontist between 6 and 7 years of age – or even earlier if the dentist suggests it – for an evaluation of the bite.
As soon as the first signs are detected, beginning treatment in childhood is much more beneficial. However, you should know that there are also therapeutic alternatives for adults. Here, we’ll tell you how the problem is usually solved in both age groups.
The treatment of mandibular prognathism in children
During childhood and adolescence, it’s possible to correct the increased growth of the jaws. At this stage, it’s possible to take advantage of the fact that bone formation is still active. This promotes the advancement of the upper jaw or slows down the advancement of the lower jaw in search of a harmonious relationship.
Interceptive orthodontics, a procedure that acts on the growth of the bony bases at a very early age, is used for this purpose. In the case of mandibular prognathism, expander appliances are used to stimulate the development of the upper jaw.
Also, chin braces and orthodontic masks that slow down the growth of the jaw will likely be recommended. Once these procedures have been performed, it may be necessary to supplement with corrective orthodontic treatment to improve dental alignment. When the bones are in the right position, the malposition of the teeth is corrected to achieve a good bite.
We think you may be interested in reading this, too: Mouth Piercing Could Have Oral Health Consequences
The treatment of mandibular prognathism in adults
In the case of adults, in whom bone growth has already finished and mandibular prognathism has already been established, the treatment is more complex. If this is your case, you shouldn’t be discouraged, because it’s still possible to achieve good results.
In mild cases, you can opt for orthodontic treatment to correct the misalignment of the teeth. This can improve the bite and the appearance of the smile and the relationship between the upper and lower elements. However, it doesn’t change the appearance of the face and isn’t always indicated.
In more serious situations, when functional and esthetic problems are very evident, it’s necessary to combine orthodontic treatment with orthognathic surgery.
The latter is a type of maxillofacial surgery that makes it possible to restore symmetry and harmony to the face by putting the jaw bones in place.
Orthognathic surgery to correct mandibular prognathism
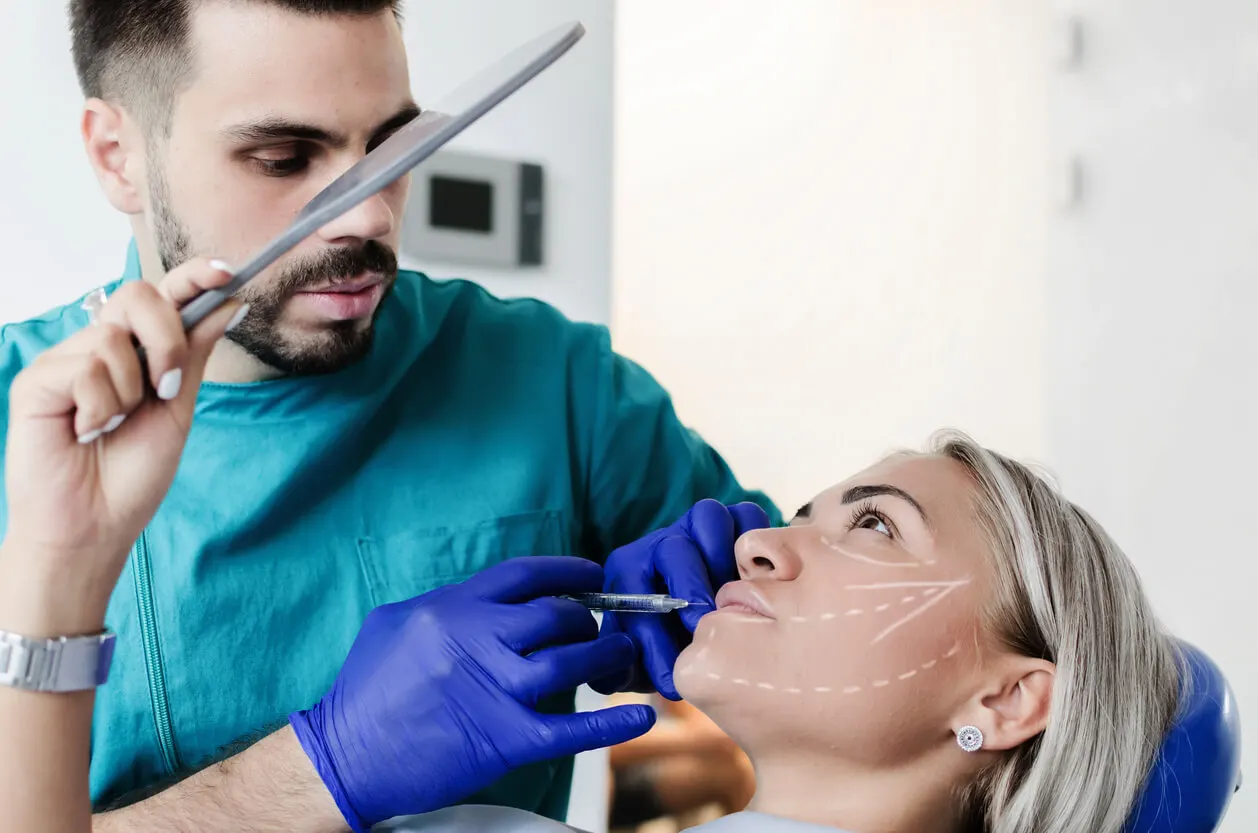
Before the person undergoes such surgery, various morphological and esthetic studies with X-rays and photographs are necessary. This helps to plan the treatment, to consider the aspects to be corrected, and to determine the most appropriate techniques.
It also allows the person to be shown the possible result, which makes it easier for him/her to accept the change and resolve any associated questions and concerns before the procedure. In any case, prior to this, it’s necessary to wear orthodontic devices for a period of time.
This makes the oral situation more favorable for the intervention. In particular, the teeth are positioned in the best possible areas.
The surgery is performed in an operating room and under general anesthesia, so it requires hospitalization. It’s performed by a multidisciplinary team, in which the maxillofacial surgeon plays a key role. The duration of the procedure can take about 2 hours, although this depends on the complexity of the case.
The process is done through the oral cavity, so there will be no visible scar on the face. Depending on the type of mandibular prognathism of the patient, the upper jaw, the lower jaw, or both bones will be mobilized.
During the procedure, the surgeon performs an osteotomy of the maxilla, which consists of fracturing it and placing it backward. If necessary, excess bone is removed. Also, to keep the two bone fragments together, they’re fixed with titanium plates and pins.
This type of surgery can only be performed once the person’s growth has been completed. In the case of girls, this usually occurs around the age of 16; in boys, it tends to occur between 17 and 18. Anyway, this depends on each particular person.
What happens after corrective jaw surgery?
After the surgery, it’s necessary to follow certain care procedures to favor the recovery of the tissues and to prevent complications. It will be necessary to follow a liquid diet and then a soft diet to avoid mobilizing the jaw while it heals.
The surgeon will prescribe medication for pain and to avoid infections. She or he will also suggest rest for 1 to 3 weeks. It’s not advisable to exert yourself, exercise, or smoke during this time.
Once the recovery time has passed, it may be necessary to return to braces for a period of time. Your teeth can be positioned in the right place with the braces to achieve the desired smile.
Can prognathism be prevented?
When mandibular prognathism is due to hereditary or genetic issues or is part of a syndrome, it’s not possible to prevent it. However, it is possible to act on the external factors that favor the appearance of this disorder.
Parents, for example, play a fundamental role in taking care of their children’s mouths and thus can help prevent the loss of milk teeth before their time. Detecting and controlling harmful habits (such as mouth breathing) and seeking a solution in time is also part of prevention.
Early and frequent dental check-ups also make it possible to detect any problems in the mouth early, even when everything seems to be going well. Visiting the dentist is a simple but fundamental action to prevent major problems in the future.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Sauhing Muñoz, I. J. (2012). Diagnóstico y tratamiento de pacientes clase III por prognatismo mandibular (Bachelor’s thesis, Universidad de Guayaquil. Facultad Piloto de Odontología).
- Cartuche, L. P. G., Cruz, V. S., Bravo, M. E., & Manuel, E. C. (2019). MALOCLUSION DE CLASE III, TRATAMIENTO ORTODONCICO. REVISIÓN DE LA LITERATURA. Evidencias en Odontología Clínica, 4(2).
- Alina, R. A., & Yosvany, H. S. (2021, June). CARACTERÍSTICAS MORFOLÓGICAS DEL SÍNDROME CLASE III. In cibamanz2021.
- Carrasco-Sierra, M., Mendoza-Castro, A. M., & Andrade-Vera, F. M. (2018). Implementación de la ortodoncia interceptiva. Dominio de las Ciencias, 4(1), 332-340.
- Caro, M., & Awuapara, S. (2021). Revisión de los principales manejos ortodónticos interceptivos y correctivos no quirúrgicos de la maloclusión clase III. Revista de la Asociación Odontológica Argentina, 109(3), 207-212.
- Torres Rodríguez, M. S. (2022). Cambios cefalométricos en pacientes con prognatismo y pseudo prognatismo mandibular pre y postquirúrgicos.
- Aquino Hilares, G. (2019). Ortodoncia y cirugía ortognática.
- Disla Abreu, R., & Cabral Monte de Oca, C. (2021). Cirugía ortognática primero en el tratamiento combinado de ortodoncia-cirugía ortognática en maloclusiones esqueletales de Clase III (Doctoral dissertation, Universidad Nacional Pedro Henriquez Ureña).
- Amit, K., Premkumar, S., & Palone, M. R. T. La maloclusión clase III esquelética grave mediante abordaje primario de cirugía ortognática: informe de caso Severe skeletal class III malocclusion by surgery-first orthognathic approach: a case report.
- Parejas Sánchez, K. X. (2022). Protocolos y plan de tratamiento ortodóntico preventivo.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








