Major neurocognitive disorder
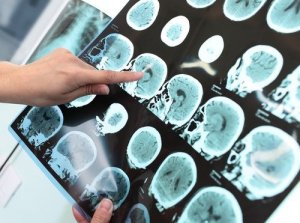
Major neurocognitive disorder, also known as dementia, is a condition in which higher brain functions are impaired as a result of neuronal damage. Over time, the patient will lose their autonomy even in the most menial tasks.
Today, as life expectancy increases with the consequent aging of the population, the major neurocognitive disorder is considered a global problem. There’s no cure for this disease, but the symports are treatable.
Major neurocognitive disorder
Neurocognitive disorders mainly take a toll on a person’s memory, perception, and problem-solving abilities. These are what many doctors refer to as “neurocognitive functions.”
The most direct neurocognitive disorders are amnesia, dementia, and delirium. Dementia, or major neurocognitive disorder, typically appears in people over 60 years of age.
According to data from the World Health Organization, there are approximately 50 million people afflicted by this condition in the world.
Symptoms and stages
When it comes to major neurocognitive disorder, the main symptoms manifest as afflictions to different areas of a person’s mental function. The patient will experience a degenerative process in their autonomy and ability to perform certain activities. The following serious impairments are common:
- Shifts in language abilities and perception.
- The decline of memory, thought, and judgment.
- Changes in emotional behavior and/or personality.
Besides these, there are several other symptoms related to this disorder that a person may experience. These include hallucinations, depression, aggressiveness, or delusions. In the evolutionary process of major neurocognitive disorder, three stages can be differentiated, which we will describe below.
You might be interested in: The Differences between Dementia and Alzheimer’s
The initial stage of the disease
The first symptoms consist of mild and gradual issues. Above all, a person begins to experiences forgetfulness and episodes of disorientation in time or space. However, such episodes aren’t too frequent.
The intermediate stage of major neurocognitive disorder
Next, as time goes by, the condition matures and the symptoms become more evident. In time, the person afflicted starts requiring help, especially with simple tasks such as grooming, shopping, or paying bills.
Also, lapses of memory become more serious and frequent. Patients may become disoriented in their own homes and experience mild episodes of amnesia. Also, they may experience difficulties in communication.
Advanced stage
Finally, a person becomes progressively worse after reaching the most advanced stages of major neurocognitive disorder. The person afflicted will have increasingly more problems with their daily routine. They may even display aggressive behavior. Then, in the end, they’ll become entirely dependent and inactive.
Alzheimer’s as a form of major neurocognitive disorder

Alzheimer’s is the most common form of dementia. In fact, this disease appears in 60-80% of the cases with a major neurocognitive disorder diagnosis. Currently, there’s no cure for either Alzheimer’s or any type of major neurocognitive disorder.
However, there are a series of treatments that focus on decreasing the symptoms that improve the quality of life of a person with this diagnosis. These treatments can also slow down the development of the disease. Currently, Alzheimer’s is one of the main priorities in biomedical research.
Discover: Non-Alzheimer’s Types of Dementia
Treatment for major neurocognitive disorder
As we said before, there’s no current cure for major neurocognitive disorder. Therefore, the progressive development of the disease is inevitable and treatments are solely focused on improving quality of life.
Firstly, we should mention how important teamwork is between nurses, doctors, and social workers are because this is a multifactorial disorder.
The role of the main caregiver is fundamental in the treatment of this disorder as they handle the evolution of the disease. It’s very important to prevent complications due to the treatment or its side effects.
Family support is also essential, as a person with Alzheimer’s should never be alone. Also, occupational therapies and support networks are very beneficial for patients.
In many cases, it’s important to prevent certain secondary causes of the disease such as hypertension, high cholesterol, or obesity. The idea is to act against any risk factors that may predispose someone to this condition.
In addition, there’s a series of treatments for the symptoms of major cognitive disorder. These symptoms may include hallucinations, delusions, depression or aggression, among others. The types of drugs used in these cases are antipsychotics, antidepressants, and anticonvulsants.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
-
Bartoloni, L. C. (2019). Deterioro cognitivo. Diagnosis, Retrieved from http://revistadiagnosis.org.ar/index.php/diagnosis/article/view/227
-
Demencia. Retrieved from https://www.who.int/es/news-room/fact-sheets/detail/dementia
- Crespo-Santiago D, Fernández-Viadero C. Bases biomolecurares del envejecimiento neurocognitivo. www.viguera.com/sepg Psicogeriatría. 2011;
-
de Azpiazu P, Salamero M, Pujol J, Cuevas R. Conductas agresivas en la demencia. Escala RAGE, validación de la versión en castellano [Aggressive behaviour in dementia. RAGE scale, validation of the version in Spanish]. Rev Neurol. 2001;33(10):928-930.
- Orejarena-Ballestas M-C, Quiñonez-Pérez AM, Marín-Gutiérrez A. Estimulación cognitiva para pacientes con trastorno neurocognitivo mayor por enfermedad de alzheimer: revisión sistemática. Búsqueda. 2017;
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








