Chalazion: Everything You Need to Know

Reviewed and approved by the nurse Leidy Mora Molina
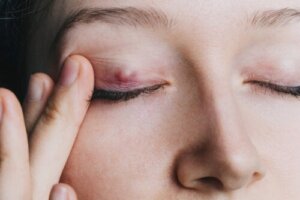
Eyelid swellings are often very annoying and make daily life difficult. In this sense, a chalazion is one of the two conditions that in most cases cause these small eyelid lumps. Here’s everything you should know about it.
This alteration is described as a small inflammatory process originating in the eyelid that is usually accompanied by redness. Likewise, it is the result of occlusion or non-infectious obstruction of the drainage ducts of the Meibomian glands.
The Meibomian glands are small sebaceous structures located behind the eyelid and responsible for the secretion of lipids that lubricate the eye. Therefore, any alteration that increases the quantity or viscosity will increase the risk of developing a chalazion.
Differences between a chalazion and a stye
A stye is an acute and painful protuberance in the eyelid resulting from an infectious process or the complication of another pathology, such as blepharitis. On the other hand, patients with a chalazion rarely feel pain or tenderness around it and its origin is usually non-infectious.
Similarly, styes are located at the level of the palpebral margin, due to occlusion of Zeiss or Moll’s glands. However, the chalazion is usually located in the body of the eyelid due to occlusion of the Meibomian glands.
Styes often cause the inflammation of the entire eyelid and resolve spontaneously in less than a week. On the other hand, a chalazion rarely causes generalized swelling of the eyelid and resolves in 2 to 8 weeks.
Causes of chalazions
The protrusion of a chalazion is formed by the retention of lipid secretions from the Meibomian glands due to an obstruction of their excretory ducts. This occlusion is of inflammatory origin, due to a direct alteration or dysfunction of the glands.
The main causes include the following:
- Dusty environment
- Acne rosacea
- Dysfunction of the glands
- Seborrhea
- Anxiety
- Dyslipidemia
- Diabetes
- Allergies
However, infectious etiology shouldn’t be ruled out, despite its low frequency. It is estimated that the main agents responsible for eye infections belong to the staphylococcus family.
Symptoms of a chalazion
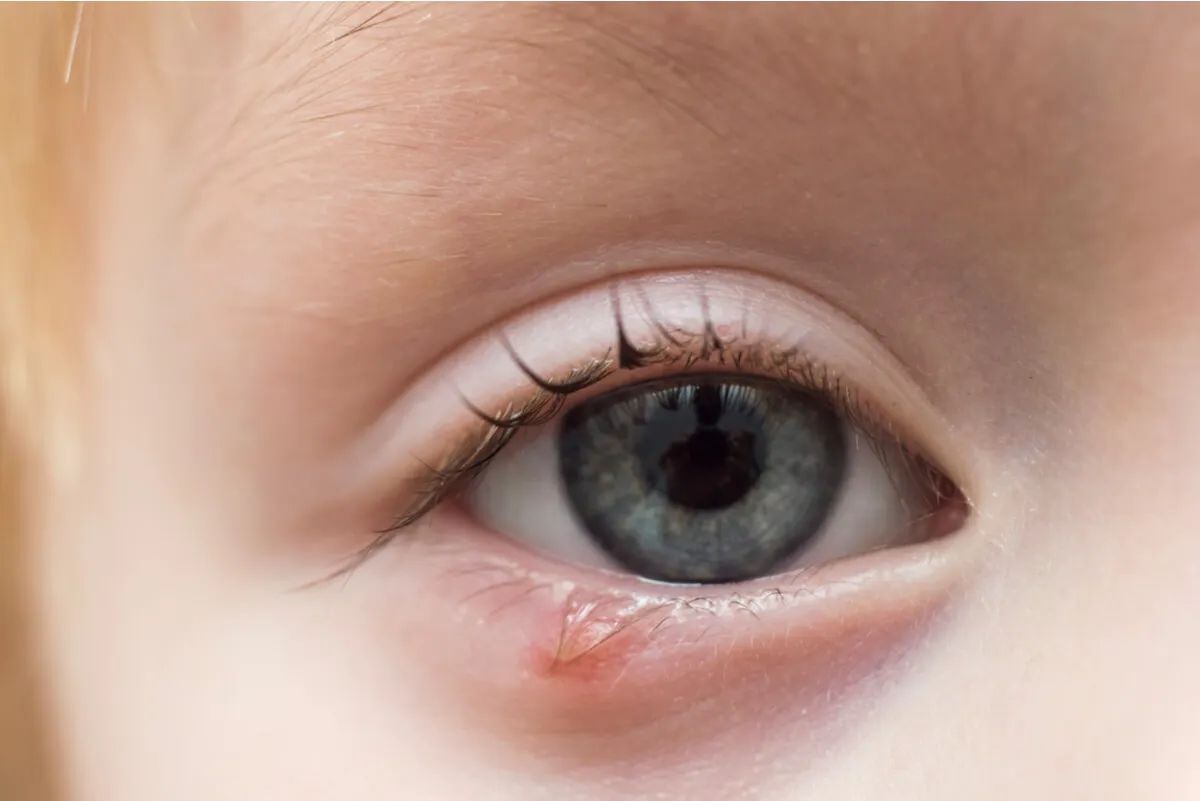
A chalazion is characterized by the presentation of a palpable and non-painful nodule or lump in the upper or lower eyelid. Initially, it usually appears as a generalized swelling of the eyelid and then settles in the center or body of the eyelid after a couple of days.
It’s also usually accompanied by redness and a sensation of warmth in the area. In addition, depending on its size and location, it can enter the cornea and alter vision, causing eye fatigue and blurred vision.
You may be interested in: 19 Common Eyelid Disorders and their Treatment
Medical treatment
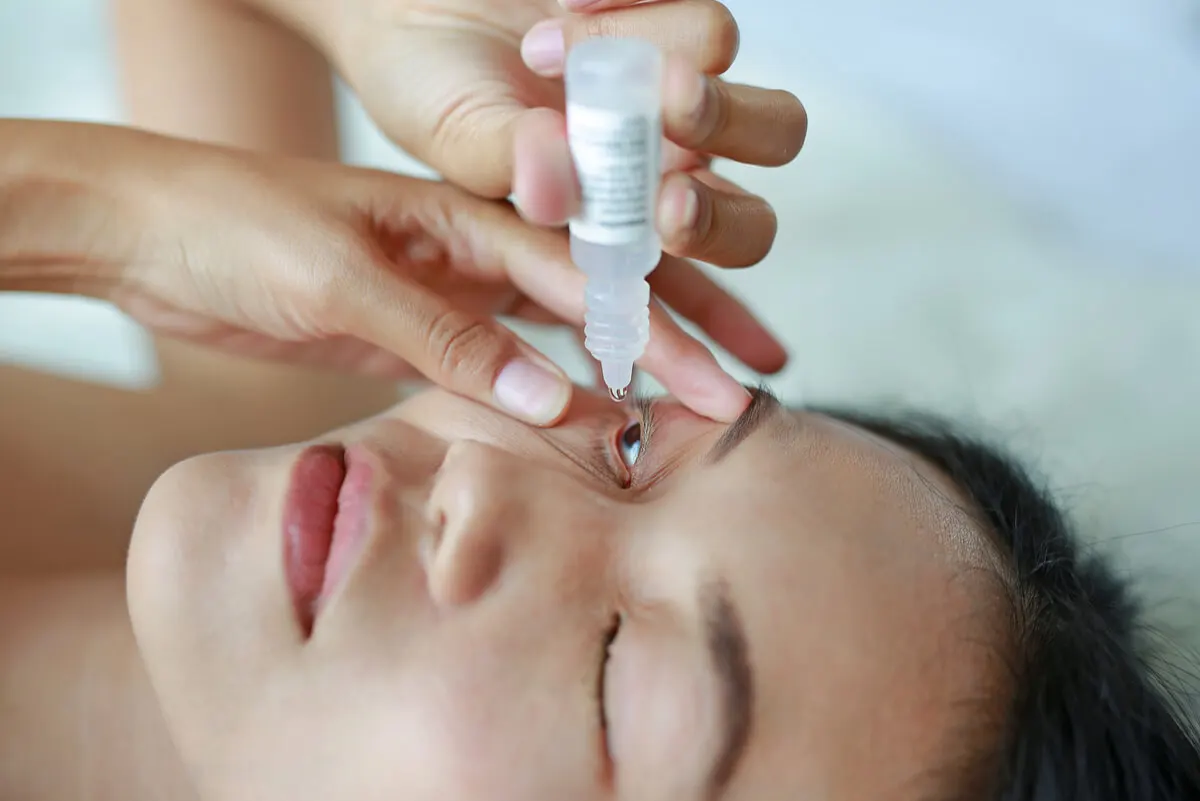
Therapeutic management is aimed at controlling the symptoms and guiding the favorable evolution of the chalazion. In this sense, specialists recommend the use of hot compresses on the area for 5 to 15 minutes, 2 to 3 times a day, to try to eliminate the obstruction.
On the other hand, the doctor may opt for the administration of corticosteroids, such as cortisone or triamcinolone if it’s large, not very aesthetic, and lasts for more than 2 weeks. In addition, if it doesn’t remit and the visual symptoms get worse, then curettage and surgical drainage under local anesthesia may be used.
The use of antibiotics should be at the discretion of the specialist if the lesion is of infectious etiology. Only the physician is able to determine the benefits and disadvantages of each medication.
Tips for the care of a chalazion
Home care is focused on maintaining eyelid hygiene and using methods that help to unblock the occluded glandular ducts. In order to do this, we can apply wet compresses a couple of times a day and massage techniques on the lump.
The first thing to do is to wash both hands thoroughly with soap and water before touching the area. Then proceed to make small circular movements with the fingertips of the index or middle fingers for up to 5 minutes.
It’s important to avoid applying pressure or rubbing for a long time, as it may favor inflammation and infection of the area, worsening the symptoms. Similarly, the use of any topical or oral pharmacological substance should be under strict medical supervision.
Read also: 5 Easy Tricks for Treating Styes
Tips for prevention
The appearance of this condition can’t always be prevented, especially if you have a predisposition to this type of pathology. However, it’s important to apply preventive measures. Among the indications are the following:
- Proper hand hygiene
- Periodic face cleaning
- Ensure the healthiness of all elements in contact with the eyes, such as eyeglasses
- Follow a diet rich in omega-3 fatty acids
Similarly, in case of suffering from glandular pathologies of the eyeball, it’s important to keep it under the supervision, management and treatment of a medical specialist.
Chalazions are common
Ocular pathologies are usually a very frequent reason for consultation in ophthalmology, so it’s important not to underestimate the appearance of lumps or bumps on the eyelid. A chalazion may be indicative of a systemic process or a complication of another disorder.
The specialist is the only one qualified to identify, differentiate and adequately treat eye conditions and their repercussions. For this reason, it’s advisable to see a specialist as soon as possible in case of any symptoms.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Özdal P, Codère F, Callejo S, Caissie A, Burnier M. Accuracy of the clinical diagnosis of chalazion. Eye. 2004;18(2):135-138.
- Arbabi E, Kelly R, Carrim Z. Chalazion. BMJ. 2010;341(aug04 1):c4044-c4044.
- Unal M. Chalazion Treatment. Orbit. 2008;27(6):397-398.
- Jordan GA, Beier K. Chalazion. 2020 Aug 8. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan–.
- López-Cerero L, Etxebarria J, Mensa J. Diagnóstico microbiológico de las infecciones oculares. Enfermedades Infecciosas y Microbiología Clínica. 2009;27(9):531-535.
- Fano Machín Yey. Complicaciones de la Blefaritis. Presentación de caso. Rev haban cienc méd [Internet]. 2016; 15( 1 ).
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








