What is Osseointegration of Dental Implants?

Written and verified by the dentist Vanesa Evangelina Buffa
Osseointegration may seem new to you but the concept has been around since the middle of the 20th century. Therefore, it’s been around for at least 50 years.
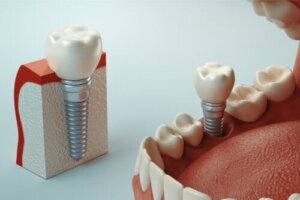
Osseointegration is the mechanism by which dental implants solidly attach to the patient’s natural bone. It’s the healing that gives these attachments the fixation and stability that characterizes them.
The success of dental implant treatments depends to a large extent on the osseointegration process. In this article, we’re going to tell you everything you need to know about this mechanism that takes place inside the bones.
The discovery of osseointegration
As has happened with several of the milestones in medicine, the discovery of osseointegration was fortuitous. The research of Swedish professor and physician Per-Ingvar Brånemark led to an understanding of this mechanism that is now used in dental rehabilitation.
The researcher was studying the healing of rabbits. It was by chance that he discovered that the titanium optical chambers that he inserted into their legs to record tissue changes eventually welded to the animals’ bones.
Upon discovering this reaction in the animals’ bone structures, some members of Brånemark’s team implanted titanium pieces in their own forearms. They were thus able to demonstrate that osseointegration was also possible in the human body.
In 1965, the first titanium dental implant was tested to replace a missing tooth. However, it was not until the mid-1980s that the practice became more widespread and gained greater importance in the dental sector. Since then, it has continued to grow.
Osseointegration is a key process for the success of dental implants. Currently, research continues on the conditions and materials that favor this type of healing and thus find new advances in this specialty.
Dental implants are considered to be the best solution for recovering dental functionality and aesthetics in the absence of teeth. Osseointegration is responsible for the trust that both professionals and patients place in this procedure.
What is osseointegration of dental implants?
Osseointegration is the biological mechanism through which dental implants are joined and integrated with bone tissue. The great fixation and stability of these attachments depend on the result of this process.
When performing a rehabilitation treatment with dental implants, the placement of these titanium screws inside the maxillary bone is one of the first steps. In the thickness of the bone tissue, the osseointegration process begins, which lasts between 3 and 4 months.
We can consider the osseointegration of dental implants as a special healing process, capable of joining the bone with the metal of the screws. The result of these chemical, organic, and physiological reactions is a bone structure bonded to the titanium that supports the future prosthetic rehabilitation.
Thanks to osseointegration, a strong fixation is achieved between the dental implants and the maxillary bone. This makes the prostheses that are placed on them more stable, functional, and comfortable.
The success of dental implant treatments depends to a large extent on osseointegration.
Achieving an adequate fixation between the screws and the maxillary bone is what makes the treatment long-lasting and effective. In fact, when the procedure is successful and the patient cooperates with specific care, dental implants can last a lifetime.
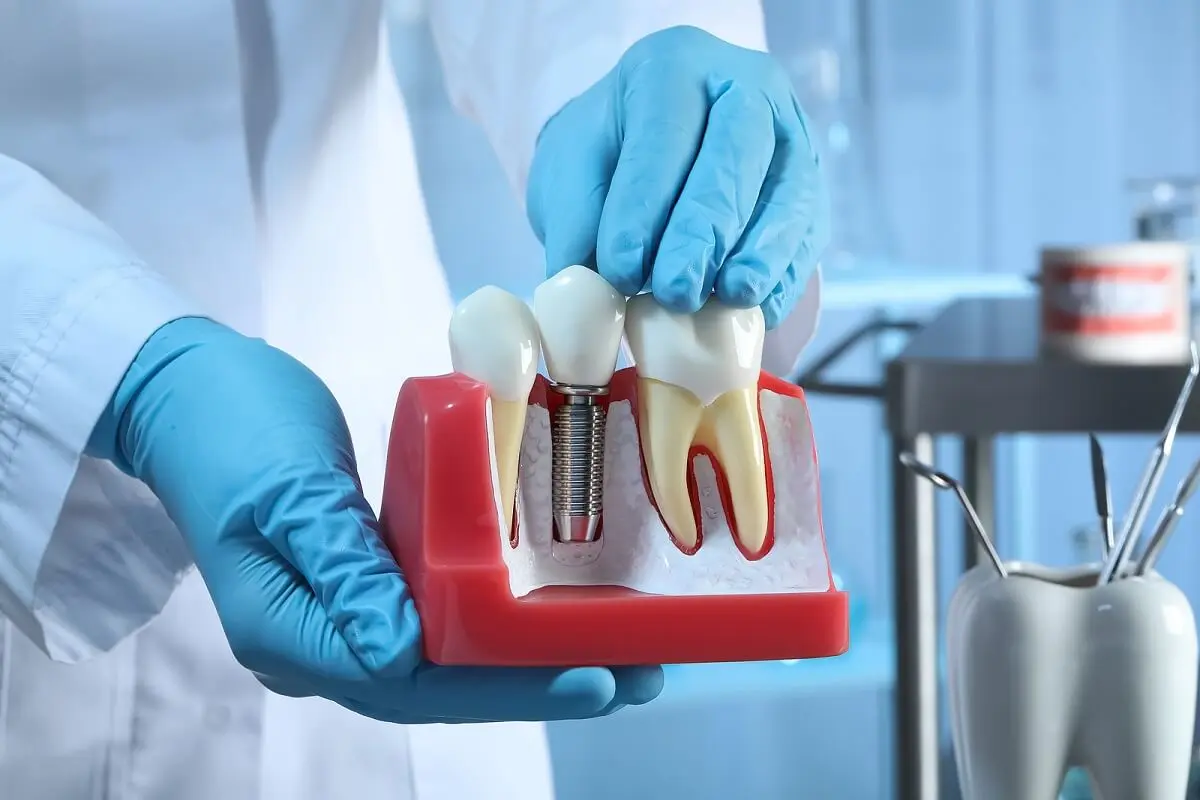
The osseointegration process of dental implants
When a person decides to have dental implants, there are some aspects that the surgeon must consider in order to achieve osseointegration. We tell you about the factors that influence the success of the process.
Remaining bone structure
After losing a tooth, the bone stops receiving the natural chewing stimuli and the body begins to reabsorb it. Therefore, it’s very important that before starting dental implant treatment, the surgeon assesses the quantity and quality of the bone in which to place the screws.
The jawbone must be thick enough to support the implants. If the bone structure has been resorbed and there is not enough bone, some surgical alternatives should be used to support the screw in the future. Bone grafts or lifting the floor of the maxillary sinus in the upper arch are some examples.
The amount of space available
When placing a dental implant, it’s important to have enough space for the insertion of the attachment. For this, the dentist must consider the type of tooth that occupied that place and how much time has passed since its loss.
When a tooth comes out, the space left by its root in the bone is different depending on the tooth. Anterior teeth have only one, while molars have two or three.
If a dental implant is to be placed in the space left by a molar, it is necessary to wait for the bone to regenerate. In this way, the site will be more uniform and osseointegration will take place without problems.
On the other hand, if a long time has passed since the loss of the teeth, it is common for the teeth neighboring the gap to have been mobilized in an attempt to close the gap. In these cases, it’s usually necessary to resort to orthodontic movements prior to surgery. With this, the crooked teeth straighten and the space necessary for the insertion of the implant fills in.
The absence of infections
Many times, dentists pull out teeth due to some type of infection. Before placing a dental implant inside the bone, it’s necessary to make sure that there are no infectious remains in the bone tissue.
If there is any type of infection in the area, it must be properly cleaned. This prevents the presence of germs that could jeopardize osseointegration and lead to the failure of dental implants.
The size, type, and exact position of the implant
When planning the surgery for the placement of dental implants, the dentist must choose the type and size of screw to be used and the exact site where it will be placed. The dentist’s experience and the right technology allow the surgery to be precise.
Intraoral scans and 3D CT scans provide information about the anatomy of the mouth to help plan the surgery. The computer-guided surgery technique helps to place the screws accurately without any issues.
Like this article? We think you may also like to read: Dental Apicoectomy: What Is It and What Are Its Benefits?
The patient’s medical history
Knowing the patient’s medical history is a very important aspect of dental surgeries. Knowing if he/she suffers from any chronic disease, what medications he/she takes, his/her pathological history, or if he/she suffers from allergies are essential data for the adequate development of the treatments.
Assessing the patient’s state of health and seeking his/her stabilization is necessary to reduce the risks during the intervention and in the osseointegration process of dental implants. Interdisciplinary work and the use of certain drugs or antibiotics can help to avoid complications.
How long does osseointegration of dental implants take?
A dental implant takes 3 or 4 months to fully osseointegrate.
During these months, several changes take place inside the bone until after the final fixation:
- In the first 3 to 4 weeks after placing the screw, it’s hard to tell if the healing process has begun.
- After 2 months, the screw begins to compact with the bone structure. Contact between the bone and the implant is visible. In addition, there seems to be greater resistance and strength of union between both.
- At 3 or 4 months, the bone and the implant are integrated with each other, forming a solid and stable unit. A well-osseointegrated screw functions just like the root of a natural tooth.
From this moment on, it’s possible to place the crown or the definitive dental prosthesis, which will restore functionality and esthetics to the mouth. Until this moment, the person can wear a cover or temporary denture so as not to affect the appearance of the smile.

Why can osseointegration of dental implants fail?
The osseointegration process of dental implants has a high success rate, estimated at 95% in general terms. However, there are some factors that can cause the healing to fail and they are the following:
- Smoking: Smoking is a very harmful habit for oral health that interferes with the osseointegration process of dental implants. Tobacco and nicotine hinder and slow down the healing process and increase the risk of infections.
- Systemic problems: Certain systemic and chronic diseases, such as diabetes, can pose a risk to the correct osseointegration of dental implants. In these cases, controls should be more exhaustive and periodic to avoid complications.
- Oral hygiene: If there’s no adequate cleaning of the mouth, oral bacteria might impair healing. Diseases such as mucositis or peri-implantitis are often due to poor oral hygiene.
We think you may also like to read this article: 7 Consequences of Poor Dental Hygiene for Your Health
Possible complications in implant treatments
There are situations that can lead to bone loss, accompanied by inflammatory processes, infections, and overloads. In these cases, a lack of action will increase the risk of treatment failure.
One of the possible complications during osseointegration of dental implants is bone loss due to inflammation of the gums in the peri-implant area. This happens due to the presence of bacteria and their toxins that activate the osteoclasts in the bone and cause its destruction.
Bone loss can also arise as a consequence of a traumatic process or overload in the implant area that affects the physiological balance of the bone. Receiving inadequate or excessive force in the area where healing is taking place can complicate this process.
To prevent these problems, it’s important to avoid overloading the implants during the osseointegration process and to stop peri-implant inflammation through proper oral hygiene. Regular check-ups are just as important, since they make it possible to detect problems early and anticipate possible complications.
Regular check-ups are key
Osseointegration is the process that allows dental implants to become firmly fixed to the bone. These immovable screws in the thickness of the bone tissue give this type of treatment a degree of stability, functionality, and durability that other therapies cannot match.
Regular visits to the implantologist allow you to check that the osseointegration process of dental implants is going as expected. Attending the check-ups scheduled by the professional will help you prevent complications that may arise during the treatment.
With proper care and frequent controls, the healing of the implants will go smoothly. After a few months, you will be able to recover the function and aesthetics of your mouth…and smile with confidence.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Carrión Vidal Víctor Josué, V. J. (2021). Biología de la oseointegración en implantes dentarios (Bachelor’s thesis, Universidad de Guayaquil. Facultad Piloto de Odontología).
- Ruben Carlos, M. M. (2021, December). BREVE HISTORIA DE LA ODONTOLOGIA. In I Jornada Virtual de Estomatología 2022. Ciego de Ávila.
- Martínez Álvarez, O., Barone, A., Covani, U., Fernández Ruíz, A., Jiménez Guerra, A., Monsalve Guil, L., & Velasco Ortega, E. (2018). Injertos óseos y biomateriales en implantología oral. Avances en odontoestomatología, 34(3), 111-119.
- Morante Carriel, A. F. (2021). Criterios de éxito y fracaso de implantes dentales oseointegrados (Bachelor’s thesis, Universidad de Guayaquil. Facultad Piloto de Odontología).
- Padrón, A. P., Quiñones, J. A. P., Martell, Y. D., Fuentes, R. B., & Matheu, L. C. (2020). Revisión Bibliográfica sobre la implantología: causas y complicaciones. Revista Médica Electrónica, 42(2).
- Tamez, J. E. B., Zilli, F. N., Fandiño, L. A., & Guizar, J. M. (2017). Factores relacionados con el éxito o el fracaso de los implantes dentales colocados en la especialidad de Prostodoncia e Implantología en la Universidad de La Salle Bajío. Revista Española de Cirugía Oral y Maxilofacial, 39(2), 63-71.
- Noboa Fernández, D. S. (2022). Fracasos en implantes dentales asociados a la diabetes (Bachelor’s thesis, Universidad de Guayaquil. Facultad Piloto de Odontología).
- Pérez Padrón, A., Pérez Quiñones, J. A., Cid Rodriguez, M. D. C., Díaz Martell, Y., Saborit Carvajal, T., & García Martí, C. D. (2018). Causas y complicaciones de los fracasos de la implantología dental. Matanzas. Revista Médica Electrónica, 40(4), 1023-1031.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








