What is Kennedy's Terminal Ulcer?

Reviewed and approved by the doctor Mariel Mendoza
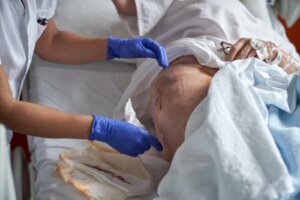
Kennedy’s terminal ulcer has the appearance of a sore, of a varied shape, with a color that can range from red and violet to black. Its evolution can be very rapid. Treatment is aimed at ensuring the patient’s well-being.
What is Kennedy’s terminal ulcer?
The name of this type of ulcer goes back to Karen Lou Kennedy, a nursing professional, who in 1983 made observations on some of her patients. These patients were in a terminal state and, for the most part, died within two weeks or less after the appearance of this sign.
However, according to research on the subject, the first description of Kennedy’s terminal ulcer (KTU) appeared in 1989 in the National Pressure Advisory Panel (nPUAP).
This is defined as a type of pressure injury that occurs in people who are nearing the end of their lives. Although it doesn’t necessarily appear in all those who are terminally ill. In fact, it tends to be less frequent in oncology patients.
In terms of incidence, one study found that more than 62.5% of palliative care patients had ulcers in the last weeks of life. Many of these were Kennedy’s.
Like this article? We think you may also like to read: Ewing’s Sarcoma: Symptoms and Treatments of This Rare Form of Cancer
What are its causes?
Regarding the exact causes of Kennedy’s terminal ulcer, there is no complete certainty about what they may be. However, some researchers think it is a sign of multi-organ failure.
In that sense, as the end of life approaches, vital organs (heart, lungs, liver, brain) and other systems may begin to fail. This is reflected in the skin, which is another organ.
The skin uses about one-third of the amount of blood that the heart pumps. In fact, one of the ways of manifesting this would be, precisely, Kennedy’s terminal ulcer.
Another explanation suggests that, in such circumstances, the body concentrates on directing blood and oxygen to the vital organs, leaving the skin unattended. Consequently, the skin becomes more susceptible to injury.
Patients with a chronic or degenerative condition are more likely to develop a Kennedy ulcer. However, the organ failure noted above can occur in anyone nearing the end of life.
This symptom may be indicative of a terminal, progressive, degenerative disease, including the following:
- Advanced pulmonary fibrosis
- Parkinson’s disease complications
- Cancer (although it’s said to be less frequent in the case of this condition)

The types and characteristics of Kennedy’s terminal ulcer
Two types of Kennedy’s terminal ulcer can be differentiated, according to their presentation. The unilateral one, as its name implies, appears on one side only, on one buttock. It is a small lesion, less than 1 centimeter, with irregular borders, darker, and of rapid development.
The bilateral one may have a purple tone and then darken more. Its appearance is erythematous or with epidermal erosion. It appears suddenly, but develops over a period ranging from 2 weeks to a few months before the patient’s death.
The appearance of Kennedy’s terminal ulcer may be similar to that of other pressure lesions. However, it has some distinguishing features:
- It usually appears in the skin area above the sacral bone. Also, it may appear on other bony prominences (e.g., the trochanter).
- The range of colors varies from shades of red and yellow to blue, violet, or black.
- The shape is variable. It often looks like a butterfly, horseshoe, or pear.
- It has irregular edges and is not very symmetrical.
- During the last stage, it begins to swell.
- The surrounding skin may appear more flaccid.
- Underneath the spot, the texture is soft.
Investigations indicate that it’s rapidly evolving. It appears and grows rapidly, even in a matter of hours.
It’s the latter that differentiates it from other pressure sores or pressure ulcers, also called bedsores. Bedsores take days to develop in people who spend a lot of time lying down and not moving.
Diagnosis, treatment, and prevention
Diagnosis of UTKs can be complicated because of the similarities to other types of injuries noted above. For this purpose, the healthcare professional should observe the signs and know the patient’s medical history.
Blood tests and other tests may be ordered, not for the Kennedy ulcer itself, but to find out how advanced the underlying condition is. However, in general, patients are usually under constant supervision at this time.
However, sometimes it’s a family member or caregiver who becomes aware of the problem. In these cases, it’s a good idea to take note of when it appeared and how the sore has changed.
After confirming a terminal Kennedy ulcer diagnosis, the physician will give recommendations for managing the situation, with a view to ensuring well-being. The goal of treatment is to keep the wounds in good condition, although this does not mean trying to promote healing.
Try to make the person comfortable and pain-free. To this end, analgesics should be administered, bandages should be applied to control odors, and postural changes and the use of cushions should be encouraged.
There is no way to prevent the appearance of Kennedy’s terminal ulcer. It’s due to the physiological deterioration of the body being close to death. The lesion will continue to progress, even if the patient receives all the necessary care.
We think you may like to read this article, too: How Many Types of Ulcers Are There?
Necessary support for Kennedy’s terminal ulcer
If someone close to you has Kennedy’s ulcer, it’s probably time to say goodbye and invite other family and friends to do so. If the doctor is not there, it may also be appropriate to call him or her.
It’s true that it’s not easy to see these signs appear and even less so if it’s the case of a loved one. However, whatever the circumstances, we must provide all emotional support to the terminally ill patient.
And, this support should also extend to those around him or her: parents, children, siblings, partner,s or friends. Those who care for a person with a serious illness should get help with their chores and tasks.
Remember that in order to care for others, we must also care for ourselves. If you feel very overwhelmed or discouraged, it may be necessary to seek counseling or support groups to help you cope with the outcome and eventual bereavement.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Alarcón Alfonso C. Plan de cuidados de enfermería de una paciente con úlcera terminal de Kennedy. Caso clínico Enfermería Clínica. 2022; 32(4): 284-290.
- Guinot Bachero J, Furió Vizcaino T. Poliulceración en paciente terminal: Úlceras de Kennedy. Plan de Cuidados Paliativos. Enferm Dermatol. 2014; 8(22): 32-40.
- Miller M. The Death of the Kennedy Terminal Ulcer. J Am Coll Clin Wound Spec. 2017; 8(1-3): 44-46. doi: 10.1016/j.jccw.2017.12.001.
- Raña Lama C, Rumbo Prieto J. Úlceras por presión inevitables, fallo cutáneo, úlceras terminales y cambios cutáneos al final de la vida. Eferm. 2018; 12(33): 7-9.
- Restrepo-Medrano J, Toro-Gonzales M, Salazar-Maya A. Úlceras terminales de Kennedy: una propuesta de cuidado desde enfermería. Enfermería Dermatológica. 2021; 15(44). DOI: 10.5281/zenodo.5812370
- Sarabia-Cobo C. Poly Ulceration patient terminal: Kennedy Terminal Ulcer (KTU). Journal of Palliative Care & Medicine. 2017; 07(01). DOI:10.4172/2165-7386.1000297
- Schank J. The Kennedy Terminal Ulcer – Alive and Well. J Am Coll Clin Wound Spec. 2018; 8(1-3): 54-55. doi: 10.1016/j.jccw.2018.02.002.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








