What is Barodontalgia and How Can You Prevent It?


Written and verified by the dentist Vanesa Evangelina Buffa
Do you swim frequently and discover that your teeth hurt after diving? If so, you may be suffering from barodontalgia.
This little-known condition can really affect the quality of life of certain people who are active at altitude or in deep water. Mountaineers, divers, pilots, or employees who have to travel constantly by plane are also all susceptible to barodontalgia.
But it isn’t only the profession or the sporting activity that can be responsible. A primary risk factor is poor oral hygiene or neglect of oral cavity pathologies, such as cavities. The latter, without a proper approach, increase the chances of having pain when the atmospheric pressure changes.
Considering that no one wants to have discomfort in the mountains, on board an airplane, or submerged in the ocean, we tell you why barodontalgia occurs and what you can do to prevent it. Don’t miss it.
What is barodontalgia?
The term barodontalgia is composed of two parts. The first is baro, which means ‘pressure’. On the other hand, odontalgia means ‘toothache.’
In this way, we understand that the concept refers to pain in the teeth and mouth caused by a change in atmospheric pressure. This change in pressure can be caused by an ascent to high altitudes or by a descent to considerable depths underwater and then a return to the surface.
The expression tooth squeeze is sometimes used to describe the phenomenon and the patients’ sensations. This is because of the common sensation that this causes, as if the mouth were being “squeezed.”
We think you may also enjoy reading this article: What Does it Mean to Dream of Your Teeth Falling Out?
Who can suffer from barodontalgia?
Barodontalgia can appear at any age and affect any person. In any case, the requirement of going through a change in atmospheric pressure must be met for it to be diagnosed. That is to say, if there’s pain in a tooth without being at a high altitude or without being submerged, then it’s not this disorder.
In this sense, there are population groups that are more exposed due to their work or recreational activities. Among them we can mention the following:
- Mountaineers, hikers, and rock climbers
- Aircraft pilots, flight attendants, and aircrews
- Soldiers and military personnel performing aviation or diving tasks
- Professional or hobby divers
- People whose work requires them to travel frequently in airplanes to perform tasks in different destinations
However, as we mentioned in the introduction, within these more exposed groups there are risk factors that increase the possibility of suffering from barodontalgia. That is to say, not everyone who gets on an airplane will have pain in their teeth.
Those who present any of the following conditions are more likely to be affected:
- Gingivitis or gum inflammation
- Dental fillings or repairs
- Cavities
This greater susceptibility is explained by the exposure of the dental pulp in these patients. It’s in this tissue that the dental nerve can be found, which is ultimately responsible for registering the change in atmospheric pressure and reacting with pain when faced with it.

The mechanism of pain is due to physics
To understand why there’s dental pain when faced with a change in atmospheric pressure, we must refer to a basic principle of physics, which is the Boyle-Mariotte law. It states that the volume of a gas trapped in a closed container, at a constant temperature, changes according to the variations in the pressure it receives.
This change is inverse. If the surrounding pressure increases, the enclosed gas decreases in volume. On the contrary, if the pressure decreases, then the gas increases its volume.
In the case of barodontalgia, this applies to the gas inside the dental elements (especially if there are cavities). When ascending in altitude above sea level, the atmospheric pressure decreases, and this causes the gas contained in a tooth to expand, increasing its volume and pushing outward.
In diving, the same thing happens when ascending back to the surface. The diver is subjected to more atmospheric pressure as he descends, but as she or he rises out of the water, the opposite process begins, which would be equivalent to ascending a mountain.
Now, why is gas trapped inside the tooth? The routes by which air reaches the interior of the pulp chamber are varied. Although the cause may not be determined, it’s most likely that some factor has played a role in causing the gas to come into contact with the dental nerve.
If there’s been a death in some part of the pulp tissue, the gas could find a place to occupy. In the same way, it may find it difficult to exit through the blood because the vascularization is poor due to necrosis of the area.
In the case of having suffered a fracture in a tooth, the fissure serves as a channel for the gas to move inward and find it difficult to exit. It’s as if it were a unidirectional path for the air to enter, but not to leave. The same explanation applies to a misfit filling or one that presents leakage spaces.
Again, we want to emphasize that in the case of barodontalgia, having a previous dental condition is a risk factor. In this case, what the change in atmospheric pressure does is stimulate the trapped gas to modify its volume. And that’s when the pain appears.
That is why it’s understood that this process is a symptom, but not a disease in itself. If the pain appears due to a change in pressure, a dentist should be consulted to determine which underlying clinical condition is to blame.
The symptoms of barodontalgia
Of course, the cardinal symptom of barodontalgia is a toothache or the feeling of squeezing from within the tooth when the atmospheric pressure changes. But there are associated signs that can suggest the underlying condition.
For example, the most acute and intense pain is associated with cavites. On the other hand, when small hemorrhages appear around the affected tooth, they are usually the result of recent oral surgery.
It’s rare and infrequent for the gas to cause a dental fracture when it expands. However, it can complicate or aggravate a clinical condition that is already present in the patient beforehand.
There is a classification for barodontalgia that considers the symptoms and the possible underlying condition. It’s as follows:
- Class 1: The pain appears suddenly when ascending, but the patient feels nothing when descending. This is most likely acute or irreversible pulpitis.
- Class 2: The throbbing and dull pain when ascending, which appears progressively, but without symptoms when descending. It could be due to chronic pulpitis.
- Class 3: The presence of the same pain as in class 2, but occurring when descending and not when ascending, is indicative of necrotic pulpitis.
- Class 4: Finally, intense pain, both when ascending and descending, leads to the suspicion of apical periodontitis.
Like this article? You may also like to read: 9 Natural and Effective Tips for Taking Care of Your Teeth
How to prevent it
Preventing barodontalgia is relatively simple. It’s necessary to take some precautions when we know that we will be in situations of atmospheric pressure changes. This is especially the case of people with cavities, pulpitis, dental fractures, or who have recently received oral surgery. They should take extreme measures.
Therefore, it’s logical to emphasize that the main prevention lies in good oral hygiene. As long as the factors that affect the production of conditions in the mouth are reduced, there will be less risk of pressure pain.
It’s also necessary to have regular check-ups with a trusted dentist. If you have had oral surgery, a tooth extraction, or dental work done and you have to get on a plane, you can ask the professional about the safety of taking the flight.
Similarly, if you frequently practice sports activities such as mountaineering or diving, you will also have to receive the authorization of the dentist and medical clearance to resume these disciplines. The dentist’s office will be able to give you a tentative date to return to practice after surgery.
For divers attending diving schools, it’s essential that the instructors are aware of your oral health. They will also be able to recommend or not to dive according to their experience with the subject.
Equalizing pressures
There are two natural and simple methods that can contribute to equalizing a little the pressures between the outside and the inside of the body when we change altitude. They will not always prevent barodontalgia, and may not be of much use if there are serious pathologies of the teeth, but in mild cases, they make a difference.
One option is to chew gum. The act of chewing mobilizes the air inside the mouth and generates changes in the Eustachian tube, which is an anatomical structure that connects the pharynx with the ears. In this way, the internal and external pressures tend to equalize.
The Valsalva maneuver pursues the same objective. It consists of trying to exhale air with the nose and mouth blocked. The most practical is to close the mouth, cover your nose with your hands, and forcefully expel the air.
The role of a dentist in the prevention of barodontalgia
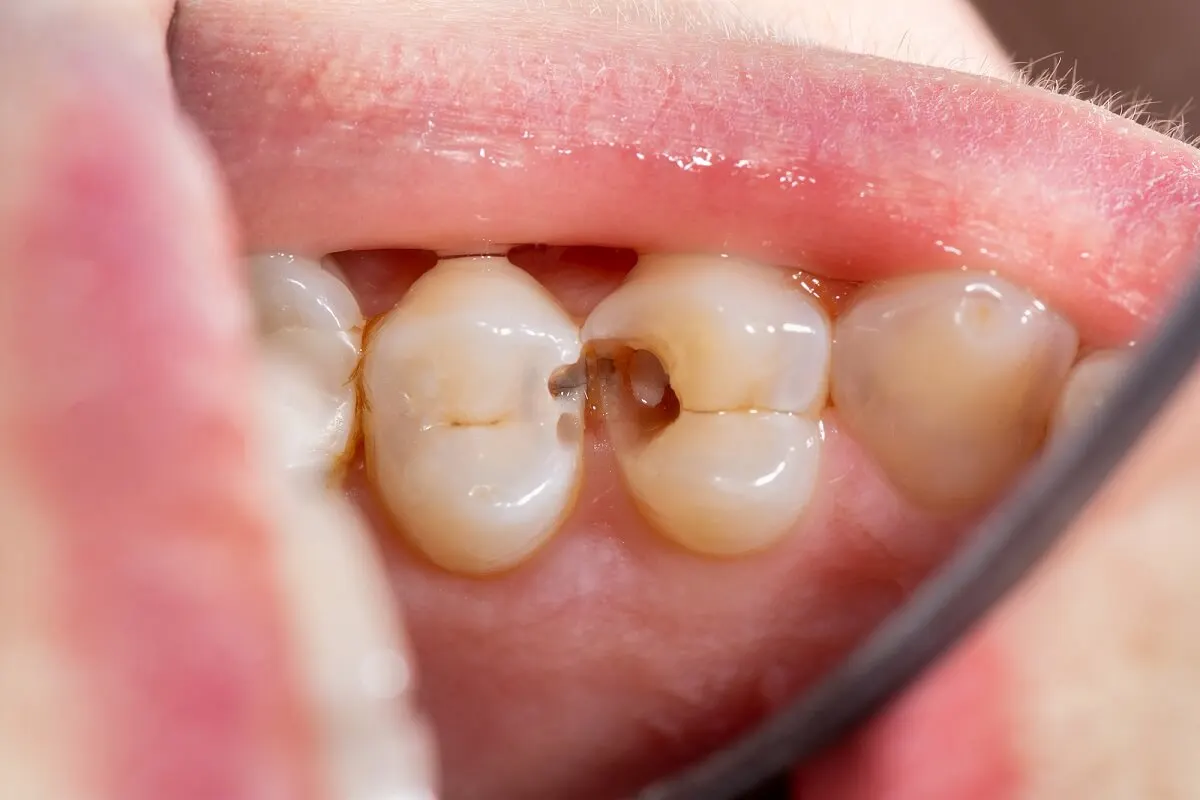
The prevention of barodontalgia also depends on the dental professional. Since pain often occurs in pre-existing oral conditions or due to air leaking into previously operated tooth elements, it should be recognized that poor fillings or wrong approaches in the dental office can be risk factors for patients.
Dentists should be aware that some materials used in clinical practice are more effective in preventing periodontalgia. This is the case of resin versus zinc phosphate and glass ionomers. This substance better withstands changes in atmospheric pressure, so it should be the first choice for treatment in airline pilots or divers, for example.
In turn, if the practitioner knows that his or her patient has frequent activities at high altitudes or practices diving, then they should take the initiative to reduce risk factors. This involves checking old arrangements and not letting signs of decay evolve untreated.
Barodontalgia is a sign of something else
It’s important to be clear that barodontalgia is a condition in the mouth. So, if you suffer from it frequently or it has happened to you in recent time, it’s crucial to consult a dentist.
There are probably cavities, pulpitis, or dental fractures that need to be addressed immediately. This will prevent new episodes of pressure pain, but will also limit the complications of the disease in question.
In short, oral health and dental hygiene are the pillars of the prevention of barodontalgia. If you like mountaineering or scuba diving, or if you have to spend a lot of time in airplanes for work reasons, then make sure you brush your teeth and visit your dentist regularly.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Zadik, Y. Aviation dentistry: current concepts and practice. Br Dent J 206, 11–16 (2009). https://doi.org/10.1038/sj.bdj.2008.1121
- Robichaud, Roland, and Mary E. McNally. “Barodontalgia as a differential diagnosis: symptoms and findings.” J Can Dent Assoc 71.1 (2005): 39-42.
- Saboowala, Hakim, ed. “What is Barodontalgia/Aerodontalgia? A Concise Review.” (2020).
- SohaibArshad, Soha Shawqi Albayat, et al. “Flyers Tooth Squeeze-Current Concepts and Future Needs-A Review.” (2021).
- Gaur, Tarun K., and Tarun V. Shrivastava. “Barodontalgia: a clinical entity.” J Oral Health Comm Dent 6.1 (2012): 18-20.
- Stoetzer, Marcus, et al. “Pathophysiology of barodontalgia: a case report and review of the literature.” Case reports in dentistry 2012 (2012).
- Zadik, Yehuda. “Barodontalgia.” Journal of endodontics 35.4 (2009): 481-485.
- González Santiago, María del Mar, Angel Martinez-Sahuquillo Marquez, and Pedro Bullón Fernández. “Prevalencia de las barodontalgias y su relación con el estado bucodental en el personal con responsabilidad en vuelo militar.” Medicina Oral, Patología Oral y Cirugía Bucal (Ed. impresa) 9.2 (2004): 92-105.
- Isis, Rojas Herrera, and Menendez LLera Dianela. “Barodontalgia: Manejo actualizado en la atención primaria de salud.” Congreso Internacional de Estomatología 2015. 2015.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








