What Are Uterine Fibroids and How Are They Treated?
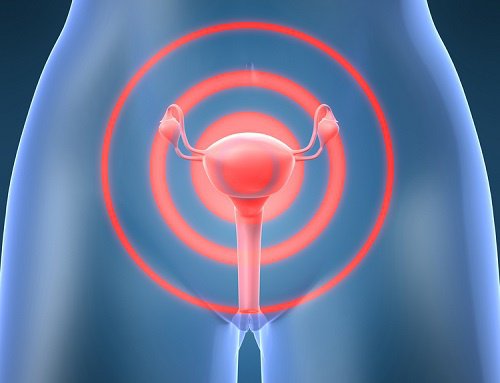
Uterine fibroids are benign (non-cancerous) tumors that grow in women’s uteruses. Between 20 and 50% of women of reproductive age have uterine fibroids and, usually, they do not present any symptoms.
However, women must undergo a medical exam to determine how serious the situation is and whether the fibroids must be removed.
The size of these fibroids can vary; they can be as small as a coin, or as large as a melon. In cases of large fibroids, they cause swelling in the uterus and can also make the woman look pregnant. Additionally, fibroids can grow alone or as a cluster.
Types of uterine fibroids
Fibroids in the uterus can be divided into three main groups, depending on their location:
- Subserosal: This type of fibroid grows in the outside part of the uterus and grows outwards.
- Intramural: This is the most common kind of fibroid, which grows within the uterine wall, making it expand more than normal. And so, this type of fibroid tends to produce the most symptoms.
- Submucosal: This type of fibroid grows under the uterine cavity, mainly causing more bleeding during the woman’s menstrual cycle, in addition to other problems such as infertility or miscarriages (in very serious cases).
Only about 20% of fibroids require treatment. However, that depends on the size, location, and a number of fibroids present in the patient. And so, the standard age when fibroids tend to appear is between 30 and 40 years old, and they are not related to whether or not the woman has had children.
Doctors have suggested that the appearance of fibroids is related to a female hormone called estradiol and the way in which it affects the myometrium, or, in other words, the uterine muscle.
This is why there are more cases of women with fibroids during perimenopause than in adolescence. They may also appear more aggressively during pregnancy.
You may also like to read:
Heart Health During Menopause
Symptoms of uterine fibroids
The most common signs of uterine fibroids are:
Changes in your menstrual cycle
You may end up bleeding more (hypermenorrhoea), your menstrual cycle may last longer (menometrorrhagia), or you may also bleed outside of your cycle (intermenstrual bleeding).
Pain
This pain tends to occur during the woman’s menstrual cycle (dysmenorrhoea), when she has sexual relations (dyspareunia), or any time of the day or month in her lower back or pelvis, without having done any physical effort or exercise.
Anemia
This can be determined with blood work, although other common symptoms of this condition are excess exhaustion, chronic fatigue, a lack of energy to get up in the morning, sleepiness, and general decline.
Tightness
The symptoms include difficulty urinating, pain when urinating, feeling that the bladder is full but urinating little, and also constipation.
Related to conception
Infertility, barrenness, miscarriages and premature birth are also some common symptoms.
If you only suffer from one of the above-mentioned symptoms, that does not necessarily mean that you have a fibroid. Thus, as we mentioned, in most cases, this problem does not have very visible symptoms.
A fibroid diagnosis is carried out by reviewing the patient’s clinical history, doing a routine gynecological exam and, if a fibroid is found, doing other studies such as a laparoscopy, hysteroscopy or ultrasound.
If the fibroids are small or do not grow, the recommended treatment is nothing more than annual gynecological exams. However, if the woman observes some of the symptoms of fibroids, she may need to undergo additional testing.
We recommend you also read:
If, on the other hand, the fibroid is large or does not respond to early treatments, the patient’s doctor may recommend performing surgery. This can be carried out in two ways: by performing a myomectomy (or laparoscopy) or by removing the uterus (called hysterectomy).
Homemade remedies for fibroids symptoms
It’s important to note that these treatments are not a replacement for medical treatment, but rather a way to reduce the symptoms of fibroids.
Recipe No. 1 for fibroids
Ingredients
- 2 tablespoons of sarsaparilla.
- 1 cup of boiling water (250 ml).
How do I make it?
Make a tea just like you would with a normal herb, cover and let it cool. Drink one cup before breakfast and another before dinner.
Recipe No. 2 for fibroids
Ingredients
- 1 apple.
- 1 carrot.
- 2 cabbage leaves.
How do I make it?
Wash, peel and chop the apple and carrot, and then place it all in a blender along with the cabbage leaves. Then, process the mixture for a few minutes and drink one cup per day.
Recipe No. 3 for fibroids
Ingredients
- 50 grams of milk thistle.
- 15 grams of pepper.
- 30 grams of nettle.
- 1 liter of water.
How do I make it?
Grind the milk thistle in a mortar and boil it in the liter of water. Then, remove the mixture from the stove and pour the rest of the ingredients in. Let it set for 20 minutes and then strain it. Drink three cups per day for 10 days straight.
Recipe No. 4 for fibroids
Ingredients
- 1 tablespoon of dandelion
- 1 cup of water
How do I make it?
Boil both ingredients for 5 minutes, then cover the mixture and let it cool. Then, drink it on an empty stomach to balance out your hormones and reduce the size of your fibroids.
Recipe No. 5 for fibroids
Ingredients
- 1/3 cups of castor oil
- 1 cloth
How do I make it?
Warm the oil and then soak the cloth in it. After, apply it to the abdomen and leave it there until it cools. This remedy is a great way to calm cramping and pelvic pain during your menstrual cycle.
Recipe No. 6 for fibroids
Ingredients
- 4 ounces of verbena leaves
- 6 liters of water
How do I make it?
Boil both ingredients until there are only 4 liters of water. Then, strain the mixture and drink 3 cups per day. Store the rest in the refrigerator.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Donnez, J., & Dolmans, M.-M. (2016). Uterine fibroid management: from the present to the future. Human Reproduction Update, 22(6), 665–686. https://doi.org/10.1093/humupd/dmw023
-
Farris, M., Bastianelli, C., Rosato, E., Brosens, I., & Benagiano, G. (2019). Uterine fibroids: an update on current and emerging medical treatment options. Therapeutics and Clinical Risk Management, 15, 157–178. https://doi.org/10.2147/tcrm.s147318
- Manta, L., Suciu, N., Toader, O., Purcărea, R. M., Constantin, A., & Popa, F. (2016). The etiopathogenesis of uterine fibromatosis. Journal of Medicine and Life, 9(1), 39–45. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5152611/
- Phelippeau, J., & Fernandez, H. (2016). Fibromas uterinos. EMC – Ginecología-Obstetricia, 52(4), 1–6. https://doi.org/10.1016/s1283-081x(16)80902-9
- Reis, F. M., Bloise, E., & Ortiga-Carvalho, T. M. (2016). Hormones and pathogenesis of uterine fibroids. Best Practice & Research Clinical Obstetrics & Gynaecology, 34, 13–24. https://doi.org/10.1016/j.bpobgyn.2015.11.015
- Zimmermann, A., Bernuit, D., Gerlinger, C., Schaefers, M., & Geppert, K. (2012). Prevalence, symptoms and management of uterine fibroids: an international internet-based survey of 21,746 women. BMC Women’s Health, 12(6). https://doi.org/10.1186/1472-6874-12-
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








