9 Treatments for a Keloid Scar

Generally, a keloid scar isn’t harmful to a person’s health. However, these marks are considered unsightly and, in many cases, they’re located in visible areas that affect the self-esteem of those who have them.
Fortunately, nowadays, medicine has multiple alternatives to improve their appearance or even eliminate them completely. What are the options? In this article, we’ll take a closer look at the 9 most interesting ones.
What is a keloid scar, and what are its causes?
The Colombian Association of Dermatology and Dermatologic Surgery defines keloids as the excessive growth of fibrous tissue during the repair of an injury. Their appearance often exceeds the boundaries of the original wound.
They usually occur after a skin cut, but they’re also likely to appear spontaneously, especially if the person has some predisposition.
The journal Acta Médica Costarricense refers that disorders in the normal collagen structure are linked to the disproportionate thickening of the skin during healing, which leads to this undesirable effect.
On this point, the Pascua Dermatology Center Journal adds that the increase in fibroblasts and collagen matrix results in hypertrophic skin sequelae and pain.
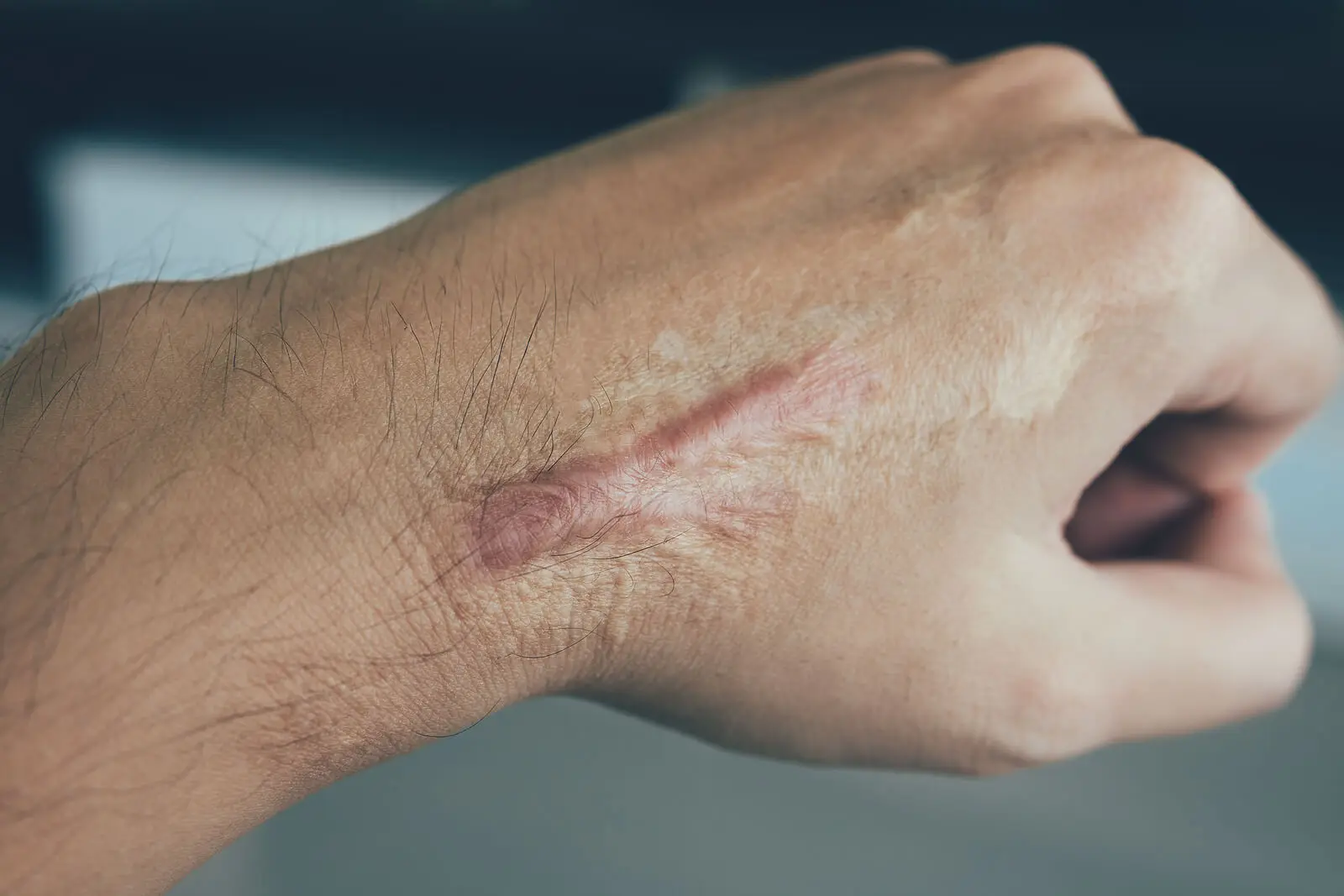
Symptoms of a keloid scar
The main symptom of keloids is a hardened, lumpy appearance. Other characteristics of this condition are as follows:
- Itching
- Pain
- Irritation
- Redness of the flesh
- A lump with ridges or nodular
- Altered sensation in the area
These scars tend to develop anywhere on the body, although the most common areas are the earlobe, neck, head, and chest.
Sometimes, over time, keloids minimize in size until they become less visible.
Can a keloid scar be prevented?
According to a publication by the U.S. National Library of Medicine, keloids are more common in blacks, Asians, Hispanics, and those under 30 years of age. They allude that the predisposition can be transmitted from parents to children.
All these factors affect the possibility of creating this type of scarring. However, certain precautions can help to avoid the deformation of the marks.
Among the advice given, it’s important to use sunscreen, cover the scar,and apply the medications prescribed by the doctor. In addition, for patients who are prone and fully aware of their condition, they suggest avoiding piercing procedures and surgeries that are not necessary.
Like this article? You may also like to read: 5 Treatments With Coconut Oil to Reduce Stretch Marks and Scars
Treatments to remove a keloid scar
According to the characteristics of the scar, the procedure for a keloid is determined by a dermatologist. There are conservative therapies such as camouflage makeup, for instance, which is a convenient method if the person prefers to avoid other techniques.
It may be necessary to combine several procedures to erase scars. Let’s take a look at what treatments are recommended.
1. Laser treatment
Several sessions with pulsed light lasers help to flatten a keloid bump. The interval between sessions is 1 to 2 months. For a better response, it’s best to couple the therapies with cortisone ampoules.
2. Corticosteroid injections
Corticosteroid injections exert anti-inflammatory and immunosuppressive effects. These doses reduce the swelling of the keloid. The objective is to make the mark look flatter.
To do this, the specialist diagnoses the type of substance to be infiltrated and the number of relevant sessions. In most cases, they establish three punctures, spacing them every month.
3. Surgery
Surgical intervention as a treatment for a keloid scar is controversial. Although resection and infiltration of the lump could reduce its recurrence, for some, it’s considered the last alternative.
In reality, the removal of these scars in people with a history of keloids increases the risk of new formations. The consensus on the operation is to resort to it only if minimally invasive aesthetic mechanisms do not offer results. In turn, the risks are believed to be decreased by combining surgery with other types of treatment.
4. Botulinum toxin
The Surgeon General newsletter reviews that the use of botulinum toxin type A (BAT) is an efficient therapeutic choice in cases of keloid scarring. In turn, the journal Cirugía Plástica Ibero-Latinoamericana highlights the influence of TBA on apoptosis and cell proliferation, which induces clinical and histological improvement of keloids.
TBA injections should be applied as soon as possible to relieve the tension caused by trauma or injury. With just two or three sessions, it’s already possible to notice a change. The total number of appointments necessary is established by the physician.
The Spanish Academy of Dermatology and Venereology notes that if there’s no improvement in the appearance of the scar, the botulinum toxin almost always heals the itching associated with keloids at a very minimum.
5. Ointments
Ointments promote scar concealment, soothe itching, prevent discomfort and relieve pain. They’re topical corticosteroids with anti-inflammatory, vasoconstrictive, antipruritic, antiproliferative, and apoptotic properties, according to the Fundación Piel Sana.
They’re usually formulations containing desoximetasone, fibrinolysis, and zinc and copper sulfate. Because of the delicacy of these topical medications, they must be prescribed by a healthcare professional.
6. Pressotherapy
Pressotherapy is a type of therapy that works by compressing keloid scars with insulating tapes and elastic bandages. It’s a reducing technique, argues the magazine Medicina Integral in a paper.
For this technique to be effective, the pressure must be 24 millimeters of mercury (mmHg). With this, it exceeds the normal capillary pressure, according to an analysis of the journal Cirugía Plástica Ibero-Latinoamericana.
It’s recommended that the pressotherapy lasts several months in periods of 12 to 19 hours.
7. Silicone
This treatment consists of covering the scar with a self-adherent and waterproof patch. Silicone patches are ideal for keeping the skin from reddening and for lowering the height of the bump.
Before placing it on the keloid, clean and dry the area. The patch should act for 12 hours over a period of three months. Leave it on while you carry out your daily activities; it doesn’t matter if it gets wet; the patches are ready to be reused for at least a week.
8. Radiotherapy
The Colombian Association of Dermatology states that radiotherapy is positive in the management of keloids and the prevention of recurrences. The procedure has shown better results if it’s preceded by surgery to destroy the keloid tissue.
In a maximum of three days after the operation, radiation advances to transform the keloid into a hypocellular tissue and prevent excessive proliferation of fibroblasts. This technique requires the joint participation of plastic surgeons, dermatologists, and radiologists.
9. Natural remedies
Natural medicine is less expensive than other scar treatments. There are home remedies that attenuate keloids. Aloe vera, honey, and rose water are among the organic options that conceal these unwanted marks.
These natural remedies have properties known to promote the overall health and appearance of the skin.

We think you may be interested in reading this, too: How to Get Rid of Acne Scars with 15 Natural Remedies
Is there a danger of complications from a keloid scar?
Keloid scars do not pose health hazards. In rare cases, doctors order biopsies in order to rule out other kinds of skin lesions.
As long as you follow the advice of specialists, the scarring does not get worse. Patches, moisturizers, topical serums, and sunscreen are important to help reduce the appearance of a keloid scar.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Arellano Arreguín J, Flores Hernández N, Flores Hernández U, Juárez Gutiérrez Z, Ramón Gamboa V, Zaragoza Álvarez C. Uso de toxina botulínica en cicatriz queloide. Cirujano General. Vol. 3. Núm. 2. pp. 76-81. México; 2014. https://www.mendeley.com/catalogue/378e787b-df50-378d-b551-38222770cc3b/?utm_source=desktop&utm_medium=1.19.4&utm_campaign=open_catalog&userDocumentId=%7Bdc451c3f-ffb8-4858-859c-794ac2d91a69%7D
- Citron Machón G, Poveda Xatruch J. La cicatrización queloide. Acta Médica Costarricense. Vol. 50. Núm. 2. Costa rica; 2009. https://www.mendeley.com/catalogue/27f27d1c-a4c7-3339-9024-0ace52d67f99/?utm_source=desktop&utm_medium=1.19.4&utm_campaign=open_catalog&userDocumentId=%7B98a2a98b-3ed1-46aa-bf48-8e329daf643b%7D
- Desoximetasone topical. Drugs.com. Estados Unidos; 2021. https://www.drugs.com/mtm_esp/desoximetasone-topical.html
- Enríquez Merino J, Martha C. Opciones terapéuticas para cicatrices queloides e hipertróficas. Revista del Centro Dermatológico Pascua. Vol. 16. Núm. 2. pp. 80-84. México; 2007. https://www.mendeley.com/catalogue/9b00e3cc-b2f8-3547-9044-505618c38426/?utm_source=desktop&utm_medium=1.19.4&utm_campaign=open_catalog&userDocumentId=%7B4ab57781-f546-46d8-889b-fc3cafc60808%7D
- Fibrinolisina. Diccionario Médico. Clínica Universidad de Navarra. España. https://www.cun.es/diccionario-medico/terminos/fibrinolisina
- Gavrilova M, Jordá Cuevas E, Martín Gorgojo A, Ramón Quiles D. Corticoides tópicos. Fundación Piel Sana. España; 2020. https://fundacionpielsana.es/wikiderma/corticoides-topicos
- Giorgianni Colmenares G, Higuerey Morao D, Soto Montenegro A. Toxina botulínica tipo A en el tratamiento del queloide. Cirugía Plástica Ibero-Latinoamericana. Vol. 47. Núm. 2. pp. 187-200. España; 2021. https://scielo.isciii.es/pdf/cpil/v47n2/1989-2055-cpil-47-02-0187.pdf
- Hernández C, Toro A. Enfoque y manejo de cicatrices hipertróficas y queloides. Revista Asociación Colombiana de Dermatología. Vol. 19. pp. 218-228. Colombia; 2011. https://revistasocolderma.org/sites/default/files/enfoque_y_manejo_de_cicatrices_hipertroficas_y_queloides.pdf
- Jaén Olasolo P. Toxina botulínica, usos revolucionarios. Fundación Piel Sana. Academia Española de Dermatología y Venereología. España; 2016. https://fundacionpielsana.es/estetica/toxina-botulinica-usos-revolucionarios
- Los queloides y las cicatrices hipertróficas. Medicina Integral. Vol. 38. Núm. 9. pp. 385-389. Año 2001. https://www.elsevier.es/es-revista-medicina-integral-63-articulo-los-queloides-cicatrices-hipertroficas-13022951#:~:text=Los%20queloides%20se%20distinguen%20de,en%20general%20no%20requieren%20tratamiento.
- Lozada Urbani J, Quintero Larróvere M, Soto Montenegro A. Uso de imanes en el tratamiento de queloides auriculares. Cirugía Plástica Ibero-Latinoamericana. Vol. 43. Núm. 2. España; 2017. https://medes.com/publication/123756
- Queloides. MedlinePlus. Biblioteca Nacional de Medicina. Estados Unidos; 2020. https://medlineplus.gov/spanish/ency/article/000849.htm#:~:text=Los%20queloides%20son%20m%C3%A1s%20comunes,que%20se%20formara%20el%20queloide.
- Rojas R. Tratamiento de queloides. Asociación Colombiana de Dermatología y Cirugía Dermatológica. Colombia; 2020. https://asocolderma.org.co/enfermedades-de-la-piel/tratamiento-de-queloides
-
Hekmatpou D, Mehrabi F, Rahzani K, Aminiyan A. The Effect of Aloe Vera Clinical Trials on Prevention and Healing of Skin Wound: A Systematic Review. Iran J Med Sci. 2019 Jan;44(1):1-9. PMID: 30666070; PMCID: PMC6330525.
- Martinotti S, Ranzato E. Honey, Wound Repair and Regenerative Medicine. J Funct Biomater. 2018 May 8;9(2):34. doi: 10.3390/jfb9020034. PMID: 29738478; PMCID: PMC6023338.
- Lee MH, Nam TG, Lee I, Shin EJ, Han AR, Lee P, Lee SY, Lim TG. Skin anti-inflammatory activity of rose petal extract (Rosa gallica) through reduction of MAPK signaling pathway. Food Sci Nutr. 2018 Oct 25;6(8):2560-2567. doi: 10.1002/fsn3.870. PMID: 30510758; PMCID: PMC6261181.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








