Symptoms and Causes of Sporotrichosis

Sporotrichosis is a long-term or chronic skin infection caused by a saprophytic fungus called Sporothrix schenckii. The infection develops when the fungus enters the body through scratches or cuts.
This condition usually appears as a skin infection and leads to swollen lymph nodes. However, it rarely affects the lungs, joints, bones, or other parts of the body.

This fungus grows on rose bushes, barberry bushes, sphagnum moss, and is present in some fertilizers. Unlike most fungal infections, this one penetrates the body through any skin wound, even the tiniest.
In most cases, infection occurs in farmers, rose growers, horticulturists, and nursery workers. Thus, one could say sporotrichosis is an occupational disease for people working in these sectors.
Widespread or disseminated sporotrichosis can develop in people with weakened immune systems when they inhale dust filled with fungus spores.
Symptoms
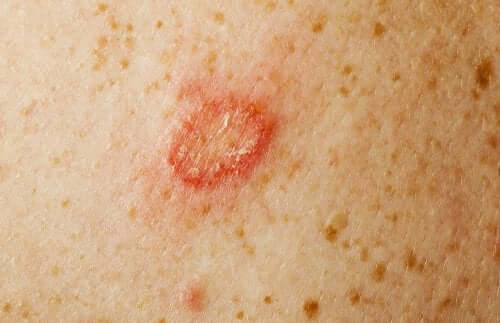
Most sores occur on the hands and forearms because these areas are commonly injured when handling plants.
The infection spreads through the lymph vessels in the finger, hand, and arm. Eventually, they reach the lymph nodes forming more nodes and open sores along the way.
There could be oozing pus from the lymph nodes. However, it’s hardly ever painful, even at this stage. These sores don’t heal unless you treat them and can last for years.
Find out how to Make your Own Natural Anti-Fungal Treatment for Nails
In addition, this fungal infection could affect the lungs and lead to pneumonia, with mild chest pain and cough. However, it usually only occurs in people with a history of lung disease. The inflammation in the joints makes movement painful, however.
Sporotrichosis rarely spreads throughout the body but it’s life-threatening when it does. Don’t worry unless you’re afflicted by an immunodeficiency.
Diagnosis
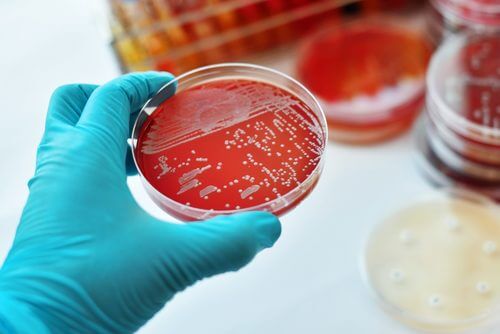
A proper diagnosis requires a culture of a sample of infected tissue to confirm if the Sporothrix fungus is present.
Treatment of sporotrichosis
The treatment of this skin infection is via antifungal drugs. Their active ingredient is oral itraconazole, which also helps prevent the recurrence of this disease. Full recovery is likely with treatment.
Treatment must go on for 2 to 4 weeks even if the skin sores have disappeared. You may also use terbinafine instead of itraconazole.
Disseminated sporotrichosis is more difficult to treat and requires several months of therapy. Infections that have spread or affect the entire body require intravenous amphotericin B. In this case, the duration of treatment could be up to 12 months.
This disease can be life-threatening for those with a weakened immune system. For instance, people with AIDS or other immunosuppressive diseases may need lifelong treatment, even if the disease is under control.
Check out The Best Six Remedies for Fungal Infections of the Scalp
Possible complications of sporotrichosis
People with a healthy immune system may experience discomfort and secondary skin infections such as staphylococcus or streptococcus.
Conversely, people with a weakened immune system could develop:
- Joint arthritis
- Bone infection
- Side effects from amphotericin B
- Breathing and lung problems such as pneumonia
- Brain infection
Finally, it’s possible to prevent or reduce the risk of skin injury by wearing thick gloves while gardening.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
-
Castro Alegria, L. A. (2013). Esporotricosis cutánea : experiencia de un hospital de tercer nivel en Cali , Colombia. Iatreia.
-
Bove-Sevilla, P. M., Mayorga-Rodríguez, J., & Hernández-Hernández, O. (2008). Esporotricosis transmitida por gato doméstico. Reporte de un caso. In Medicina Cutanea Ibero-Latino-Americana.
-
Carrada-Bravo, T. (2012). Esporotricosis: Avances recientes en el diagnóstico de laboratorio, histopatología y la epidemiología en México. Revista Latinoamericana de Patología Clínica y Medicina de Laboratorio.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








