Postpartum Anemia: Causes and Treatments

Written and verified by the doctor Mariel Mendoza
Postpartum anemia is one of the most frequent complications that accompany the process of giving birth. According to the World Health Organization (WHO), anemia is a condition in which the number of red blood cells, or the concentration of hemoglobin within red blood cells, is lower than normal.
Hemoglobin is responsible for transporting oxygen to different tissues, so the main manifestations associated with anemia are related to decreased oxygen in the blood (hypoxemia) and tissues (hypoxia).
Treatment of postpartum anemia depends on its cause, severity, and associated maternal risk factors or illnesses.
Defining postpartum anemia
Postpartum anemia is defined as the presence of hemoglobin values less than 11 grams per deciliter in the first week postpartum or 12 grams per deciliter up to the eighth week postpartum. The prevalence is estimated to be 50% in the first 48 hours, and most cases usually resolve spontaneously.
Symptoms of postpartum anemia will depend on its severity. The mild form usually has no visible signs.
When anemia is symptomatic, its most common symptom is excessive fatigue and generalized weakness. It may also be associated with dizziness, lightheadedness, pale skin, weight loss, low blood pressure, palpitations, cold extremities, headache, insomnia, irritability, and depression.
Several blood tests are necessary to diagnose anemia. The most important thing is a complete blood count and measurement of blood iron levels. Vitamin B12, folic acid, and other vitamin levels may also be requested.
Find out more here: Iron-Deficiency Anemia Diet: The Foods to Include
Causes of postpartum anemia
Postpartum anemia is usually due to a combination of bleeding during childbirth along with chronic iron deficiency present since pregnancy. Iron deficiency is brought on in the third trimester of pregnancy due to increased nutrient expenditure for the growth of the baby.
On the other hand, the impact of blood loss will depend on the woman’s body mass and her estimated total blood volume. It also depends on any other conditions she may have. For example, a woman with a heart defect has greater decompensation with less blood loss.
Postpartum hemorrhage occurs in up to 15% of pregnant women and is bleeding greater than 500 milliliters after the third stage of labor (delivery) is completed. In a natural delivery, blood loss is estimated to be between 500 and 700 milliliters, while in a cesarean section it can be as much as 1000 milliliters.
The most common causes of postpartum hemorrhage are as follows:
- Uterine atony (the uterus doesn’t contract)
- Perineal tears during vaginal delivery
- Incidental injuries during cesarean section
Read more: How to Recognize Postpartum Depression and Treat it
Associated risk factors
The risk factors most associated with postpartum anemia are the presence of antepartum anemia and the type of delivery. Anemia is more common when forceps and vacuum extraction are used. The weight of the newborn baby, previous births, the woman’s ethnicity, perineal tears, and the cut made in the vagina to facilitate delivery also have an influence.
Treatment of postpartum anemia
The treatment of anemia will depend on its cause and severity. In the case of mild anemia, caused by iron deficiency, oral intake of iron will correct the defect. When the anemia is severe, intravenous iron may be needed, however, this isn’t the most common procedure.
When the origin is postpartum hemorrhage, bleeding should be stopped and volume replacement should be performed, depending on the severity of the bleeding. Immediate replacement with physiologic solutions may be required to maintain perfusion and subsequent transfusion of heterologous blood.
However, blood transfusions for postpartum anemia should be reserved for emergencies. That is, when the following circumstances are present:
- Severe blood loss after spontaneous delivery
- Severe anemia with signs of shock
- Severe anemia during pregnancy associated with maternal decompensation
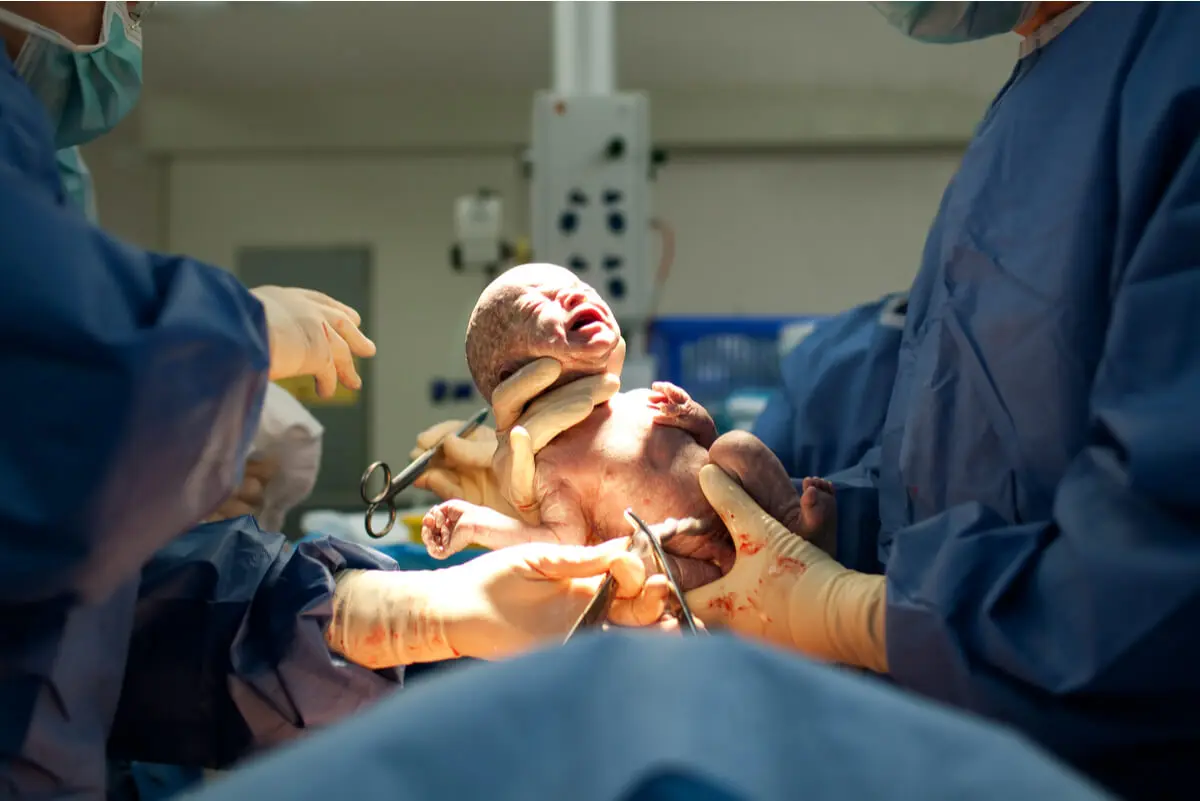
The best treatment is prevention
The main way of preventing postpartum anemia is adequate treatment and prevention of anemia in the third trimester of pregnancy. In addition to this, we can add timely therapy of hemorrhage during labor and the puerperium.
Ideally, low-dose oral iron supplements should be given during the second half of pregnancy and a balanced diet should be maintained. An iron-rich diet is recommended, with the consumption of red meat or well-cooked organ meats, as well as fruits and vegetables with vitamin C.
Maintaining adequate iron levels during pregnancy is the best prevention.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Dodd J, Dare M, Middleton P. Tratamiento de las mujeres con anemia ferropénica posparto. Cochrane Library 2004. Disponible en https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD004222.pub2/full/es.
- Karlsson H. Pérez C. Hemorragia postparto. Anales Sis San Navarra 2009;32(1):159-167. Disponible en http://scielo.isciii.es/scielo.php?script=sci_arttext&pid=S1137-66272009000200014&lng=es.
- Milman N. Postpartum anemia I: definition, prevalence, causes, and consequences. Ann Hematol 2011;90(11):1247-53. Disponible en https://pubmed.ncbi.nlm.nih.gov/21710167/.
- Urquizu X, Rodriguez M, García A, Pérez E. Anemia en el embarzo y el postparto inmediato. Prevalencia y factores de riesgo. Medicina Clínica 2016;146(10). Disponible en https://www.elsevier.es/es-revista-medicina-clinica-2-articulo-anemia-el-embarazo-el-posparto-S0025775316000646.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








