Peptic Ulcers and Helicobacter Pylori
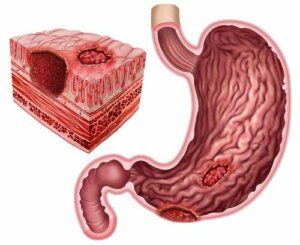
Peptic ulcers are a type of lesion that affects the gastroduodenal mucosa. Although the incidence of these ulcers is decreasing, it still affects a large part of the population.
More than 90% of peptic ulcer cases involve the presence of Heliobacter pylori. This is a type of bacteria that causes infections in the stomach.
Approximately two-thirds of the world’s population has this bacteria, which can spread through contaminated food and water.
Causes of peptic ulcers

In cases of peptic ulcers that involve Helicobacter, the eradication of the bacteria will diminish the relapses. However, only 10 to 20% of people infected with Helicobacter pylori will ever develop a peptic ulcer.
When there’s chronic consumption of NSAIDs, 50% of these people will have superficial gastric lesions. Also, the ulcers in these cases are usually asymptomatic.
The risk factors of peptic ulcers in people who consume NSAIDs are:
- History of peptic ulcer
- Age (older than 60 years)
- The use of anticoagulants or corticosteroids
- High doses of NSAIDs
- Infection by Helicobacter pylori
There are no studies that demonstrate that smoking, stress, or diet are factors that trigger peptic ulcers. However, smoking appears to negatively influence peptic ulcer healing.
Peptic ulcer symptoms and diagnosis
Most people affected that have ulcers present symptomatology of dyspepsia. Therefore, when patients present dyspepsia symptoms, doctors will suspect an ulcer. Symptoms include epigastric pain on an empty stomach that subsides with food or antacids.
Information on lifestyle, drug treatments, and personal history of ulcer or Helicobacter pylori infection is important for diagnosis.
In some people, ulcer and gastroesophageal reflux disease can coexist, which can make diagnosis difficult. However, the most sensitive and specific test to confirm the existence of an ulcer is upper endoscopy (gastroscopy).
You may also be interested in: 10 Symptoms of a Peptic Ulcer
Treatment of peptic ulcers

The goal of treatment is the relief of symptoms, healing of the ulcer, and the prevention of complications. Also, it’s a good idea to follow some hygienic-dietary measures, such as the following:
- Avoiding the consumption of NSAIDs
- Don’t eat or drink anything that causes the symptoms
- Don’t smoke, since tobacco delays the healing of the ulcer and increases relapses
Antisecretory treatment
Proton pump inhibitors (PPIs) are currently the drugs that achieve the highest mucosal healing rates. However, you should only take them if your doctor advises it.
They should be taken before meals. Also, some studies show greater effectiveness when taking them in the morning rather than late in the day. Proton pump inhibitor drugs need 3 to 5 days to achieve maximum effect. However, there’s variability in the clinical response of liver metabolism to the drug.
The duration of peptic ulcer treatment depends on the location of the peptic ulcer. In duodenal ulcers, it lasts 4 weeks, while in gastric ulcers it takes between 6 and 8 weeks.
Eradication of Helicobacter pylori
Eradication of the bacteria results in healing of the ulcer. Also, long-term ulcer complications are reduced.
The first choice of eradication treatment consists of administering a PPI and antibiotics (specifically clarithromycin, amoxicillin, and metronidazole) for at least ten days.
In penicillin-allergic patients, PPIs, clarithromycin, and metronidazole are used as the first choice for at least 10 days.
Recommendations for the use of NSAIDs for peptic ulcers
When risk factors for peptic ulcers exist, it’s advisable to consider the following recommendations before taking NSAIDs:
- Read the indications: If the effect you’re looking for is analgesia or fever reduction, it’s best to take paracetamol instead.
- Always take the minimum effective dose of NSAIDs and, also, the less toxic one.
- Avoid taking NSAIDs, corticoids, and anticoagulants all together.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
-
Ber Nieto, Y. (2012). Úlcera péptica. Medicine. https://doi.org/10.1016/S0304-5412(12)70275-5
-
Gamboa, J. L. (2003). Infección por Helicobacter pylori y enfermedad ulcerosa péptica. Bvs.Sld.Cu.
-
Truyols Bonet J, Martínez Egea A, G. H. A. (2014). Ulcera Gastrica Y Duodenal. Guía de Actuación Clínica En A. P.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








