Gastric and Duodenal Ulcers


Written and verified by the pharmacist Fabiola Marín Aguilar
Gastric ulcers are erosions or wounds that appear on the lining of the stomach. When the erosions occur in the upper part of the small intestine, we call them duodenal ulcers.
What causes gastric and duodenal ulcers?
- Acid hypersecretion: loss of balance of stomach acid due to excessive production of hydrochloric acid (acid needed to help digestion) can cause the appearance of a peptic ulcer.
- Non-Steroidal Anti-Inflammatory Drugs (NSAIDs): Prolonged and excessive use of anti-inflammatory drugs to relieve pain, inflammation and fever such as ibuprofen increases the risk of gastrointestinal bleeding and ulcerative disease.
- Stress, tobacco and alcohol: promote the appearance of peptic ulcers.
On the other hand, we know that there’s a direct relationship between gastric or duodenal ulcers and infection with the bacteria Helicobacter pylori. In fact, the characteristic spiral morphology of this bacterium facilitates its penetration into the gastric mucosa, adhering to it and producing toxins that cause inflammation and the appearance of ulcers.
It’s estimated that approximately 50% of the world population may be infected with H. pylori, although only 15% of people infected with this microorganism will develop a gastric or duodenal ulcer throughout their lives.
Read more: Watch Out for These 9 Dangerous Bacteria That Are Harmful to Humans
What are the symptoms?

The most common symptoms related to gastric and duodenal ulcers are the following:
- Abdominal pain: the main symptom is a burning sensation in the pit of the stomach. It usually calms down after you eat food or after you take antacids. In the case of a gastric ulcer the pain is more characteristic immediately after meals.
- Heartburn or burning sensation in the esophagus.
- Nausea and vomiting.
- Changes in intestinal transit and abdominal swelling or bloating.
You can also experience an asymptomatic ulcer, where the discomfort is not as characteristic and is only diagnosed when more serious complications occur such as:
- Digestive hemorrhage: hematemesis occurs (the patient vomits blood) and melena (black stools due to blood in the stool).
- Perforation: the ulcer becomes deeper and deeper until the gastroduodenal mucosa is perforated.
- Pyloric stenosis: occurs when the area that joins the stomach and duodenum is narrowed and the patient has a feeling of satiety after hardly having eaten food.
How do you diagnose it?
The diagnosis of gastric and duodenal ulcers is made based on the patient’s medical history, the characteristic symptoms they show, a physical examination, and any additional tests the doctor considers appropriate.
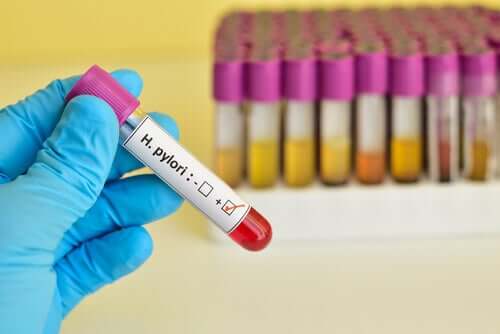
For diagnosis, doctors usually focus on visualization of the ulcer and detection of Helicobacter pylori bacteria.
- Methods focused on visualization of the ulcer:
- Oral digestive endoscopy: doctors do this by inserting a tube with a small camera through the mouth and esophagus. This allows them to see the entire digestive tract and detect any abnormalities. If they detect an ulcerative lesion, they’ll take a tissue sample (biopsy) for analysis.
- Methods focused on the detection of Helicobacter pylori:
- Serological tests to detect antibodies against this microorganism.
- Detection of helicobacter in stool samples.
- The breath test: this consists first of ingesting a liquid with carbon-marked urea and then of blowing a tube to determine if the exhaled CO2 contains marked carbon. This would indicate if the bacteria has metabolized it and therefore confirm the presence of helicobacter.
Discover: Overcome Bacterial Gastroenteritis in 5 Simple Steps
What does the treatment consist of?
Treatment is focused on relieving symptoms and reducing pain with pharmacological options.
Antacid drugs and gastric protectors
- Proton pump inhibitors: such as the well-known omeprazole, which is responsible for blocking acid secretion from the stomach.
- H2 receptor antagonists: An example is ranitidine.
Drugs indicated to treat Helicobacter pylori
The treatment to eradicate this microorganism consists of using a proton pump inhibitor to reduce acid secretion in combination with antibiotics that kill the bacteria.
You’ll take it for a few days and repeat the breath test after that, which will confirm if the infection has disappeared.
Treatment of complications from peptic ulcers such as bleeding or perforation requires finding the bleeding ulcer by endoscopy and cauterizing the hemorrhage. In the case of perforation, the patient will require urgent surgical intervention.
Prevent gastric ulcers
The prevention of ulcerative diseases is in your hands. Not abusing non-steroidal anti-inflammatory drugs, caffeine-rich drinks, avoiding tobacco, and eating a healthy diet reduce the risk of developing gastroduodenal ulcers.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Fundación Española del Aparato Digestivo (FEAD). Inicio. Enfermedades y síntomas. Úlcera péptica: https://www.saludigestivo.es/enfermedades-digestivas-y-sintomas/ulcera-peptica/#tratamien
- Shiotani A, Graham DY. Pathogenesis and therapy of gastric and duodenal ulcer disease. Med Clin North Am. 2002; 86: 1447-1466
- Agencia Española de Medicamentos y Productos Sanitarios. CIMA. Nexium mups 20 mg. Ficha técnica: https://cima.aemps.es/cima/dochtml/ft/63436/FT_63436.html
- Agencia Española de Medicamentos y Productos Sanitarios. CIMA. Alquen 150 mg. Ficha técnica: https://cima.aemps.es/cima/dochtml/ft/60298/FT_60298.html
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








