Erysipelas Infection: Problems and Solutions

Written and verified by the doctor José Gerardo Rosciano Paganelli
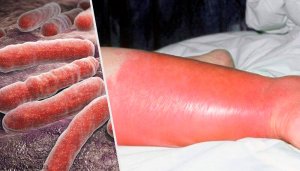
Erysipelas a cutaneous infection. It starts with the bacteria Streptococcus pyogenes and also Staphylococcus aureus. This condition has been on the increase in the last five years. And, this is especially true in places where these bacteria are common.
It can also take the form of a cellulite-like infection. At first, it appears on the surface. But then, it extends deeper into the skin, and spreads throughout.
The initial lesion is usually an erythematous papule that evolves. It increases rapidly in size. Then, it creates an unlimited and very painful erythematous plaque.
The gradual effects of the primary lesion change in the skin near the plaques. And, it looks like an orange peel. They’re also often accompanied by lymphangitis and other systemic symptoms of poor health. But a specialist clinic can address them.
Causes
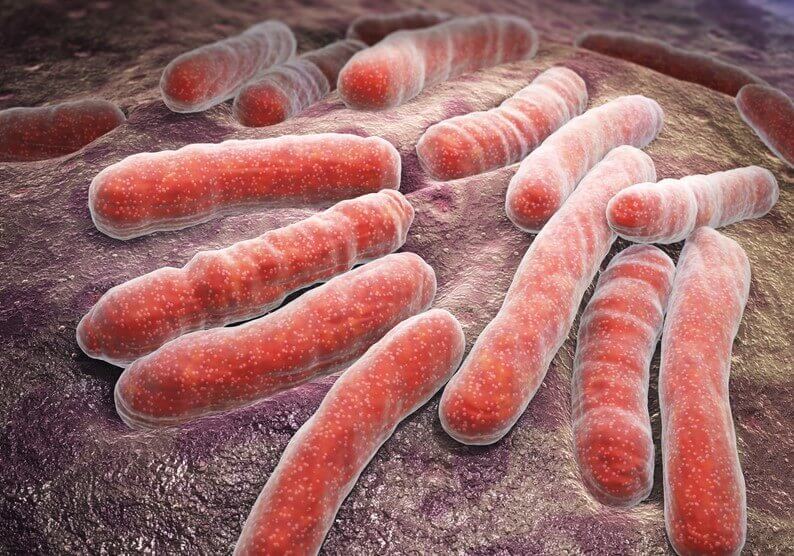
In general, the infection that causes erysipelas is not contagious. However, its direct bacterial origin is Streptococcus Pyogenes and Staphylococcus Aureus. The latter is the most common bacterium in skin lesions.
Also, these bacteria colonize from an entrance in the skin. Basically, this could be an open wound or an inflamed hair follicle. It can also occur through an infected pore. Or, it can start with an insect bite.
However, there are predisposing factors in each person. And, these factors can cause the bacteria to colonize the affected area much more quickly. In general, this is due to the ineffectiveness of the immune system itself. For instance, some of these predisposing factors are: nephrotic syndrome, venous or lymphatic obstruction and type 2 diabetes mellitus.
Symptoms
The symptoms are evident straight away. The local signs of phlogosis are evident, which are usually found in the lower extremities and in the malar region of the face, which is the favourite target.
Early signs
- Feeling hot
- Blushing
- Intense pain
- Functional limitation.
- Oedema of the affected area.
More serious symptoms
- Fever
- Weakness
- Lymphangitis
- Shivering
- General discomfort
Complications
- Post-streptococcal glomerulonephritis
- Thrombophlebitis
- Bacteraemia
- Toxic shock
Diagnosis
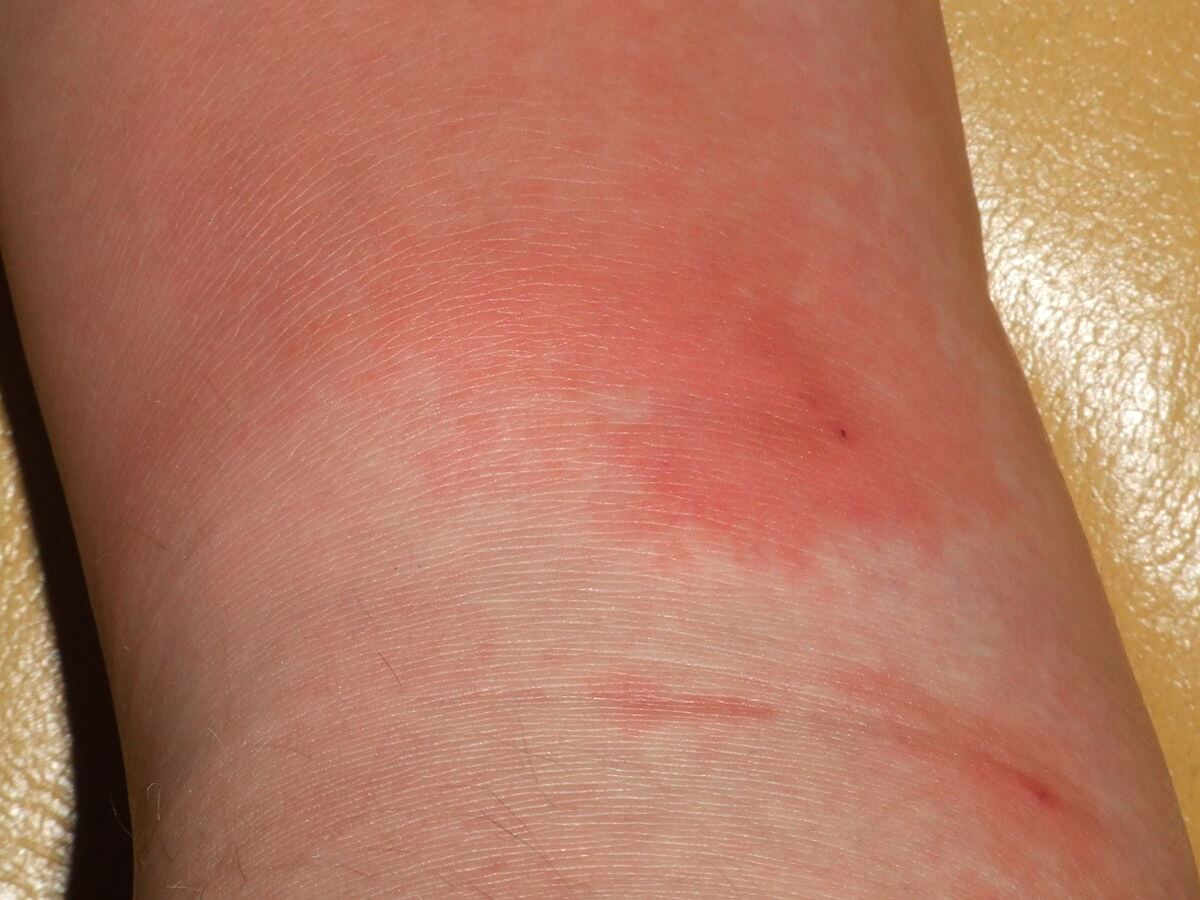
The onset of erysipelas is abrupt. And, it’s usually rapid. Additionally, elevation of the skin is notable in less than 24 hours. Because of this, the injury is usually in the lower extremities. The doctor will try to detect a body temperature of greater than 38 °C or, failing that, chills.
A diagnosis stats with the physical examination of the patient. And, it includes an interview with the patient and a review of the patient’s clinical history.
Erysipelas treatment
Erysipelas, being an infection that covers both layers of the skin, dermis and epidermis, cannot be treated with just pharmacological treatment. It’s a condition which requires care and hygiene measures in order that the lesion heals properly, and the pain may progressively recede until the lesion is completely healed.
Complementary care
- Good skin hygiene around the affected area.
- Absolute rest of whatever part of your body is injured.
- Elevation of the lesion to reduce oedema and help relieve pain.
- Thermotherapy with a cloth soaked in magnesium sulphate to reduce inflammation.
- Removal of secretions from open wounds with the help of sterile dressings hydrated with a physiological solution, three times a day.
Pharmacological Treatment
First-choice drugs
- Oxacillin: 1 – 2 grams IV every 4 hours at 6 hours for 10 days.
Paediatric dose: 200 mg / kg / day every 6 hours.
- Cephalexin: 500 mg VO every 6 hours for 7 days.
Paediatric dose: 25 mg / kg / day every 6 hours.
- Crystalline penicillin: 4 million IU IV every 4 hours for 7 days.
Second-choice drugs
- Ciprofloxacin: 200 mg IV every 12 hours for 7 days.
Its administration is not recommended in children under 10 years.
- Ceftriaxone: 1 gram IV OD for 10 days.
Paediatric dose: 50 – 100 mg / kg / day.
- Ampicillin/Sulbactam: 1.5 – 3 grams IV every 6 hours for 7 days.
Paediatric dose: 200mg / kg / day every 6 hours.
Tablets: 750mg VO every 12 hours for 7 days.
Recommendation
Patients affected by this type of injury should switch to oral treatment when the more serious symptoms subside. They should especially do this when there is no fever and there is a marked improvement in the skin. Of course, this usually takes 3 to 5 days, so the improvement will not be immediate.
Also, the total duration of the treatment is often a maximum of 10 to 14 days. But, as always, this depends on your body’s response.
References
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Erysipelas Infection: Problems and Solutions – Step To Health. (2009). Retrieved from https://steptohealth.com/erysipelas-infection-problems-solutions/
-
FICA, A. (2003). Celulitis y erisipela: Manejo en atención primaria. Revista chilena de infectología, 20(2), 104-110.
-
Skoknic, A., Díaz, I., Urcelay, S., Duarte, R., & Gonzales, O. (1981). Estudio de la Erisipela en Chile. Arch Med Vet, 13, 13-16.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








