Chocolate Allergy: Causes, Treatment and Prevention


Written and verified by the doctor María Irene Benavides Guillém
Chocolate allergy is a controversial and complex subject. Allergic symptoms are attributed to ingredients such as milk, nuts, peanuts, or nickel, and not to the cocoa itself.
Cocoa is the basic ingredient in chocolate. In 100 grams (4 oz) of cocoa, there are 20.4 grams (0.8 oz) of proteins, 25.6 grams (1 oz) of lipids, 11.5 grams (0.5 oz) of carbohydrates, and minerals such as phosphorus, calcium, and iron, among other substances.
However, there are different types of chocolate ranging from dark chocolate, with more than 80% of its weight in cocoa, to white chocolate, without pure cocoa, with milk and sugar. All these elements are potential sources of allergy.
How does chocolate allergy occur?
Foods generate a tolerance response. In an allergic person, they will be recognized as pathogens, triggering an inflammatory response.
This susceptibility to developing food allergy involves factors such as genetics and the microbes we have in our intestines. We speak of allergies when exposure to chocolate or its components always triggers an abnormal immune system response. The best-known form is that in which immunoglobulin E antibodies are produced.
In classical allergies, immunoglobulin E molecules released in response to the food bind to receptors on cells such as mast cells and basophils. This results in the release of substances such as histamine. This is what causes the rapid onset of allergic manifestations, ranging from a skin rash to anaphylaxis.
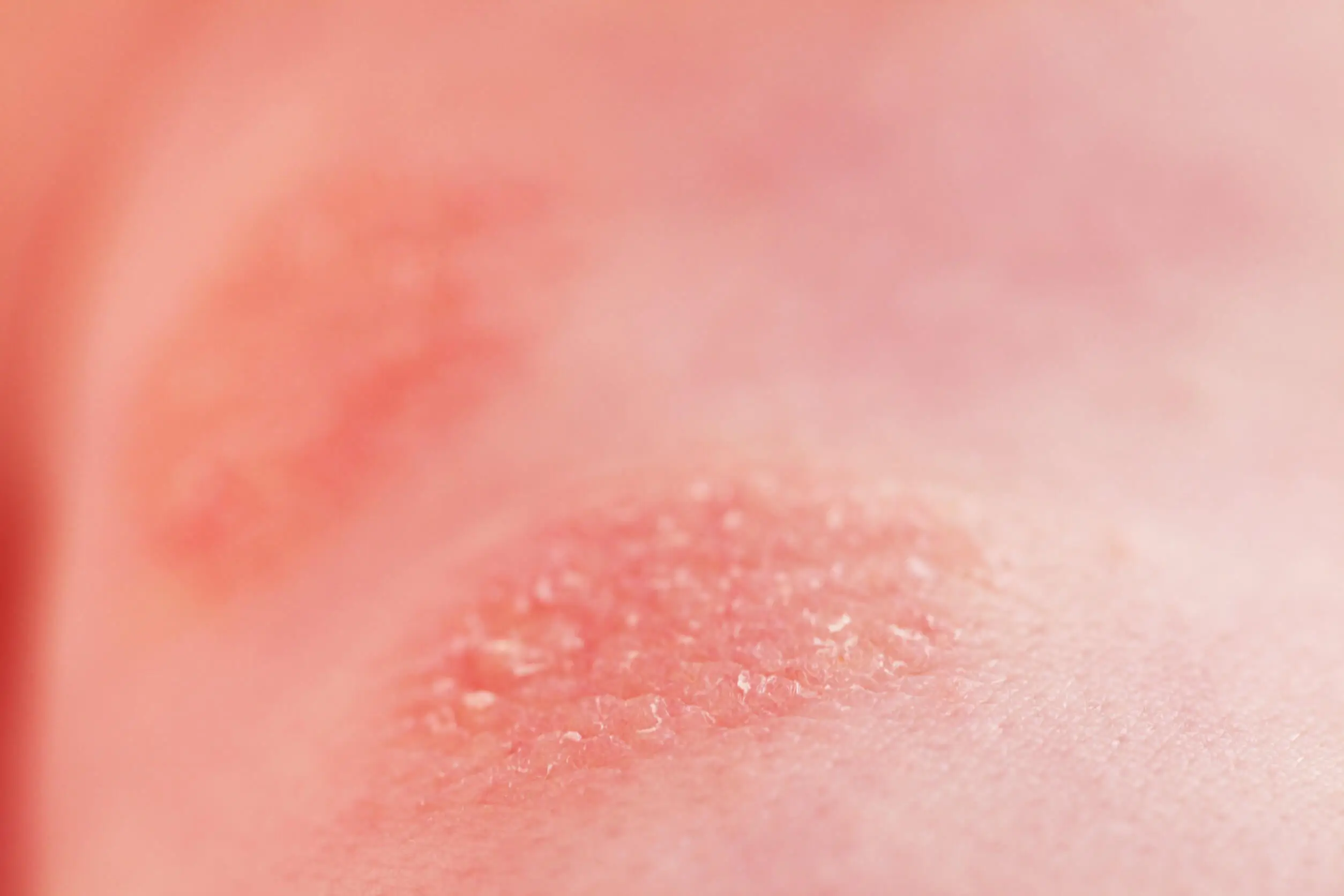
Symptoms
Symptoms of food allergies, including chocolate, involve almost every organ of the body. Hives may occur on the skin, with itching and redness of varying extents.
In more severe cases there may be edema or generalized swelling, called “angioedema”. This can be life-threatening when it affects the respiratory system.
Gastrointestinal symptoms are frequent, starting with nausea and mild abdominal pain. Vomiting and diarrhea follow.
Signs of allergic rhinitis, such as increased nasal secretions and itching of the nose, are accompanied by coughing. Moreover, there may be cardiovascular complications, such as a sudden drop in blood pressure and circulatory collapse.
Find out more here: Keys to Recognizing a Ginger Allergy
Allergies associated with chocolate
The most common allergy-causing foods are milk, egg, peanuts, nuts, shellfish, wheat, soy, and fish. In turn, products containing these ingredients will cause reactions.
Milk, peanuts and tree nuts are regularly found in chocolate.
People with nickel allergy may develop systemic nickel allergy syndrome or chronic dermatitis when ingesting chocolate. Less well described is cocoa allergy. There are reports of sensitization through occupational exposure.
In parallel, Lopes et al. report 3 patients with immunoglobulin E-mediated allergic immune response to cocoa. In all 3 cases, there was a positive oral challenge test. The patients manifested pruritus, edema, and respiratory symptoms, requiring treatment with antihistamines and adrenaline.
How to treat chocolate allergy
The treatment of chocolate allergy has several aspects. Medications such as antihistamines and corticosteroids are useful for symptom relief. However, in the case of anaphylaxis, the first-line treatment is epinephrine or adrenaline.
In the long term, the most important thing is to avoid the allergy-causing food. As diet can be problematic, the help of a nutritionist is always advisable.
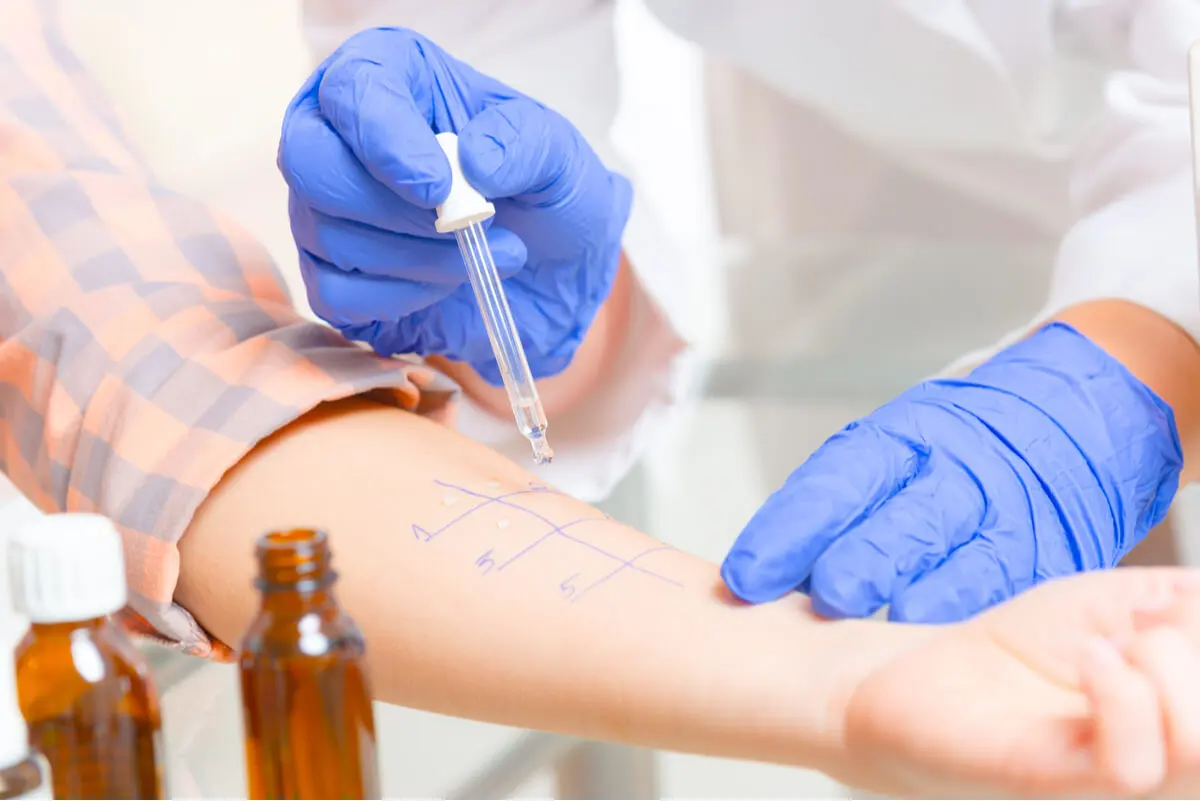
Another option is immunotherapy. The patient will be put in contact with small increasing amounts of the food causing the allergy, until tolerance is achieved.
Can I prevent chocolate allergy?
Due to the multifactorial nature of food allergies, their prevention is a constant subject of research. Preventive measures are focused on childhood, as this is when there’s more scientific evidence.
In the year 2021, the recommendations of the American Academy of Allergy, Asthma and Immunology, the American College of Allergy, Asthma and Immunology, and the Canadian Society of Allergy and Clinical Immunology were published. The entities indicate that it’s important to introduce peanuts and boiled eggs at 6 months of age. Along with this, a young child’s diet must include a great diversity of foods.
On the other hand, the European Academy of Allergy and Clinical Immunology guideline, also published in 2021, suggests avoiding the regular use of cow’s milk formula with cow’s milk protein to supplement breastfeeding during the first week of life.
Read more: The Difference Between Milk Allergy and Lactose Intolerance
What do I do if I already have an allergy?
If the person is already allergic to chocolate, additional precautions will need to be taken to avoid complications:
- Read the labels of the products you eat
- Be cautious when eating food for the first time
- Be careful when eating products bought on the street
- Talk about the allergy with the people around you.
.Remember that it will always be necessary to consult a trusted doctor in case of any questions and follow their recommendations.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Lopes JP, Kattan J, Doppelt A, Nowak-Węgrzyn A, Bunyavanich S. Not so sweet: True chocolate and cocoa allergy. J Allergy Clin Immunol Pract. 2019;7(8):2868-2871.
- Montagna MT, Diella G, Triggiano F, Caponio GR, De Giglio O, Caggiano G et al. Chocolate, “Food of the Gods”: History, Science, and Human Health. Int J Environ Res Public Health. 2019;16(24):4960.
- Anvari S, Miller J, Yeh CY, Davis CM. IgE-Mediated Food Allergy. Clin Rev Allergy Immunol. 2019 ;57(2):244-260.
- Shu SA, Yuen AWT, Woo E, Chu KH, Kwan HS, Yang GX, Yang Y, Leung PSC. Microbiota and Food Allergy. Clin Rev Allergy Immunol. 2019;57(1):83-97.
- Muthukumar J, Selvasekaran P, Lokanadham M, Chidambaram R. Food and food products associated with food allergy and food intolerance – An overview. Food Res Int. 2020;138(Pt B):109780.
- Cianferoni A. Non-IgE Mediated Food Allergy. Curr Pediatr Rev. 2020;16(2):95-105.
- Fleischer DM, Chan ES, Venter C, Spergel JM, Abrams EM, Stukus D et al. A Consensus Approach to the Primary Prevention of Food Allergy Through Nutrition: Guidance from the American Academy of Allergy, Asthma, and Immunology; American College of Allergy, Asthma, and Immunology; and the Canadian Society for Allergy and Clinical Immunology. J Allergy Clin Immunol Pract. 2021;9(1):22-43.e4.
- Halken S, Muraro A, de Silva D, Khaleva E, Angier E, Arasi S et al ; European Academy of Allergy and Clinical Immunology Food Allergy and Anaphylaxis Guidelines Group. EAACI guideline: Preventing the development of food allergy in infants and young children (2020 update). Pediatr Allergy Immunol. 2021;32(5):843-858.
- Rishor-Olney CR, Gnugnoli DM. Nickel Allergy. En: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022. Disponible en: https://www.ncbi.nlm.nih.gov/books/NBK557638/.
- Jacob SE, Hamann D, Goldenberg A, Connelly EA. Easter egg hunt dermatitis: systemic allergic contact dermatitis associated with chocolate ingestion. Pediatr Dermatol. 2015;32(2):231-3.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








