Biological Therapy for Crohn's Disease: Advantages and Risks


Written and verified by the doctor Maryel Alvarado Nieto
Crohn’s disease is one of two recurrent conditions collectively referred to as inflammatory bowel disease, and biologic therapy options are the latest innovations in the field. Recent years have seen an increase in incidence, accelerating research to find effective approaches.
Due to the chronicity of Crohn’s disease symptomatology, it’s a difficult condition to cope with. That’s why establishing effective treatment is of vital importance for patients.
What is inflammatory bowel disease?
The term inflammatory bowel disease (IBD) groups together two distinct conditions that have a chronic course, but with recurrent symptoms. Crohn’s disease (CD) and ulcerative colitis (UC) are the conditions in question.
IBD affects both men and women in a similar way. It most commonly appears between 20 and 30 years of age, but can even be diagnosed in childhood.
Crohn’s disease
In this inflammatory process, various segments of the digestive tract are affected, including regions of mucosa with normal characteristics. It can be located in any part of the gastrointestinal tract, but is more frequent in the distal portion of the small intestine and colon.
Inflammation in Crohn’s disease usually involves all layers of the intestinal wall, which is why it is called transmural. In addition, ulcerative lesions of varying depth appear, giving it a cobblestone appearance.
When this condition is activated, the most common symptoms are diarrhea and abdominal pain. These may be accompanied by other clinical manifestations including fever, vomiting, and weight loss.
On the other hand, some people may develop alterations that affect other organs and systems, but are still linked to the pathological process of Crohn’s disease:
- Uveitis
- Arthropathies
- Stomatitis
- Erythema nodosum
It’s necessary to perform various studies that discover the inflammatory process and lesions that are causing any disease in the digestive tract. While the arsenal of complementary tests will depend on the intensity of the symptoms, some of these tests include the following:
- Detection of p-ANCA and anti-Saccharomyces antibodies
- Simple abdominal radiography
- Colonoscopy and ileoscopy
- Abdominal ultrasound
On the other hand, determining the exact nature of the condition is essential in the accurate diagnosis of Crohn’s disease. In particular, because it allows differentiating microscopic alterations from those caused by ulcerative colitis.
Ulcerative colitis
On the other hand, in the case of ulcerative colitis, the most common location is the rectum, with the condition often extending towards the colon. Likewise, in this inflammatory process, there are no areas with normal mucosa interposed on the altered ones.
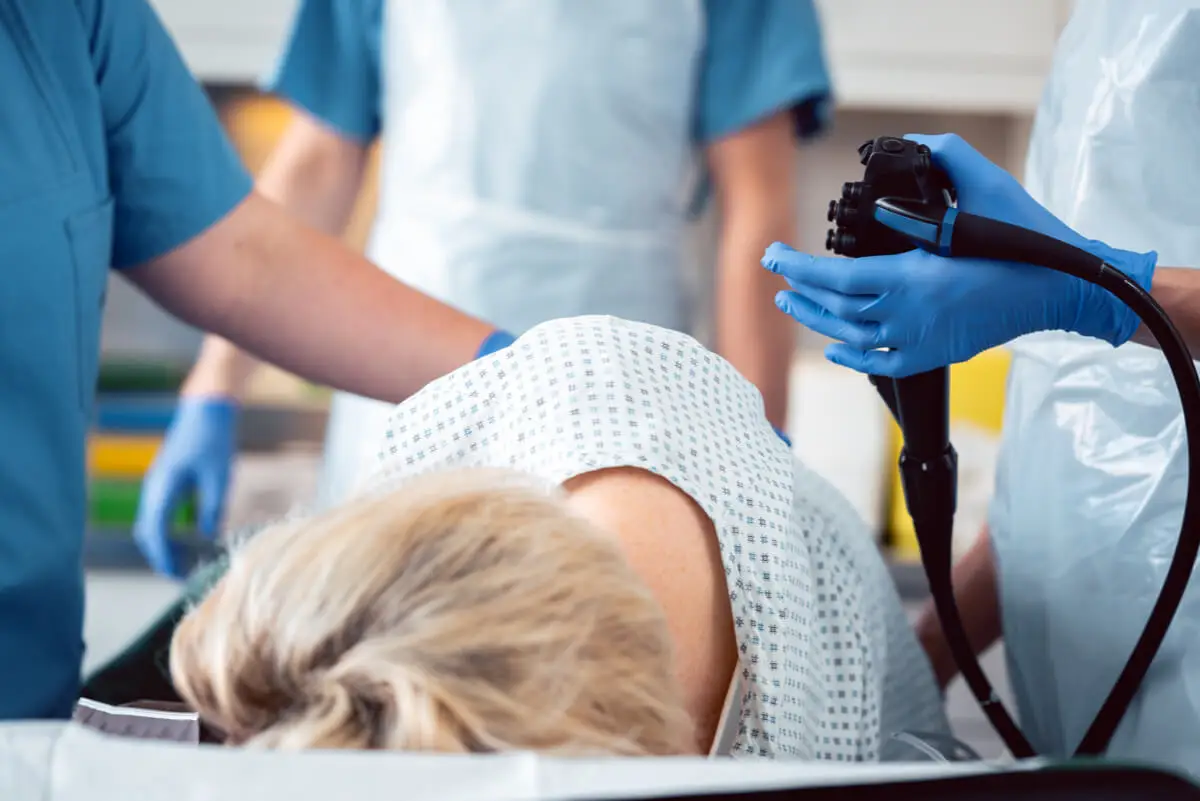
The multifactorial origin of Crohn’s disease has led to biological therapy
Specialists recognize that several environmental factors are necessary for a person with a vulnerable genetic component to develop Crohn’s disease. In addition, there’s a genetic factor involved. This has led specialists to think that genes are involved in the appearance of the condition.
There can be up to 201 loci involved in the genetic predisposition for the development of IBD.
On the other hand, with regard to environmental factors, smoking is linked to an increased risk for IBD. The diet of industrialized societies, with many processed foods high in fat and low in fiber, also appears to play a role in the onset of the disease.
Finally, abnormal immune response contributes to the development of IBD. Components of the intestinal wall and the normal bacterial flora residing in the digestive tract also trigger an exaggerated response that conditions the inflammatory process.
Like this article? You may also like to read: What Are Pro-Inflammatory Foods and What Are The Risks?
Treatment options for Crohn’s disease
Although there’s currently no therapeutic treatment that will cure Crohn’s disease, several approaches are available that control the underlying inflammatory process. Achieving complete remission is the ideal goal of current regimens.
Therefore, it’s necessary that doctors examine each case on an individual basis. This should take into account the severity and duration of symptoms, but also the location of the lesions.
Among the available therapeutic guidelines, the following scale is used:
- Aminosalicylate medications such as mesalazine
- Corticosteroid medications such as prednisone
- Immunosuppressants such as azathioprine and methotrexate
- Biological therapy with antibodies
- Surgery
It’s always necessary to assess the previous medication administered and the response obtained with it. This makes it possible to determine the degree of efficacy of a particular treatment. It’s therefore possible to make the right choice of regimen.
In mild to moderate conditions, the best option is to start with aminosalicylates. Then, doctors often suggest a person moves on to other regimens. Surgery should be the last option.
We think you may be interested in reading this, too: The Benefits of Ginger & Chamomile Tea for Irritable Bowel Syndrome
What is biological therapy for Crohn’s disease?
Biological therapy consists of a group of drugs whose active ingredient is obtained by processing material of biological origin, i.e. living organisms. This therapeutic option allows for the management of diseases that have an immune component.
In the treatment of Crohn’s disease with biological therapy, some compounds help control the inflammatory process. Among these schemes are the following:
- Anti-TNF antibodies, including infliximab and adalimumab
- Anti-integrin antibodies like Vedolizumab
- Anti-interleukin antibodies like Ustekinumab
Biological therapy is not the first line of treatment for Crohn’s disease.
However, there are special situations in which resorting to these drugs is a viable option. In particular, this may be recommended when high-dose steroid approaches don’t show an adequate response (corticoresistance). It may also be a good idea when a new flare-up (corticodependence) appears again after remission when the dose is reduced.
However, the current recommendation in these difficult-to-manage cases is to indicate immunosuppressive treatment before initiating biologic therapy. However, individualizing patients helps to determine who may have a real benefit.
The risks of biological therapy for Crohn’s disease
The main risk is the increased vulnerability to developing serious infections. This risk is seen in both steroid and immunosuppressant use.
Any infectious process, including the presence of asymptomatic tuberculosis, should be ruled out before starting biologic therapy.
Follow-up is key for inflammatory bowel disease
An increased risk of colorectal cancer has been discovered in patients with IBD compared to the general population. However, this risk also depends on the duration and extent of the condition, as well as on a history of colon cancer in the family.
Due to the chronic nature of this condition and this increased risk, a periodic review of the patient, beyond the established therapy, is advisable. This includes colonoscopies to demonstrate mucosal changes.
Although the location of the injuries usually remains constant, their severity may intensify over time. In fact, the usual inflammatory pattern at the onset of the disease may progress over the years.
Therefore, it’s important not to neglect your follow-up with your primary care provider if you have Crohn’s disease. Your healthcare team will be able to tell you whether or not you’re a good candidate for biologic therapy.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Mora, H.; Díaz, C.; Guedea, E.; Manejo de la Enfermedad de Crohn en la Era de la Terapia Biológica y Celular; Universidad de Zaragoza; 2019.
- Adegbola, S. O., Sahnan, K., Warusavitarne, J., Hart, A., & Tozer, P. (2018). Anti-TNF therapy in Crohn’s disease. International journal of molecular sciences, 19(8), 2244.
- Domarus, A.; Farreras, P.; Rozman, C.; Cardelach, F.; Nicolás, J; Cervera, R.; Farreras Rozman. Medicina Interna; 19na Edición; Elsevier; 2020.
- Sans, M.; Enfermedad de Crohn; Gastroenterología y Hepatología; 31 (Supl 4): 47 – 50; 2008.
- Comisión Regional de Farmacia y Terapéutica. Consejería de Sanidad y Política Social. Región de Murcia; Documento de Consenso sobre el Uso de Terapia Biológica en el Tratamiento de la Enfermedad de Crohn; 2015.
- Ginard, D.; Khorrami, S.; Pérez, L.; Tavio, E.; López, A.; García, M.; Muñoz, F.; Ibáñez, L.; Marín, I.; Guevara, J.; Casellas, F.; Eficacia y Efectividad de la Terapia Biológica en la Enfermedad Inflamatoria Intestinal. Estudio EFIFECT; Gastroenterología y Hepatología; 2016.
- Engel, T., Yung, D. E., Ma, C., Pariente, B., WIls, P., Eliakim, R., … & Kopylov, U. (2019). Effectiveness and safety of Ustekinumab for Crohn’s disease; systematic review and pooled analysis of real-world evidence. Digestive and Liver Disease, 51(9), 1232-1240.
- del Val, J. H., & Arce, N. M. (2005). Terapia biológica en el tratamiento de la enfermedad de Crohn fistulizante. Publicación de GETECCU para Formación Continuada, 102.
- Carrasco, G.; Histología en la Enfermedad Inflamatoria Intestinal; Revista Médica Clínica Las Condes; 30 (4); 2019.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








