What is Pulmonary Tuberculosis and What Are Its Symptoms?
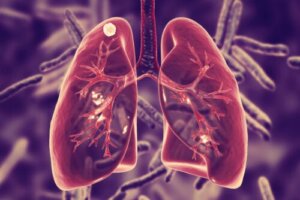
Pulmonary tuberculosis was a very serious public health problem in the early 20th century. In fact, an estimated 1 in 7 people died from it. Thanks to the development of certain drugs, the disease has been under control since the 1940s.
However, outbreaks of the infection occur from time to time. Pulmonary tuberculosis remains a problem, especially because of the emergence of a variety that’s been called multi-resistant, which is difficult to treat.
What is pulmonary tuberculosis?
Pulmonary tuberculosis is a disease caused by a bacterium called Mycobacterium tuberculosis. In most cases, this microorganism installs itself in the lungs. However, it can also affect other organs such as the brain and kidneys, as well as structures of the spine.
An important aspect is that the disease of pulmonary tuberculosis and latent infection are different. The first is the conventional pathology. The second is a condition where the bacteria is in the body, but doesn’t cause the pathology as such. It’s as if it were sleeping.
Most people who inhale the bacteria have an immune system that’s able to fight it and, as a result, prevent it from multiplying. However, the microorganism is still there, even if there are no signs.
These bacteria can remain inactive for many years or for a lifetime. However, if the immune system becomes weak, they become active, multiply and cause the potentially fatal disease of pulmonary tuberculosis.
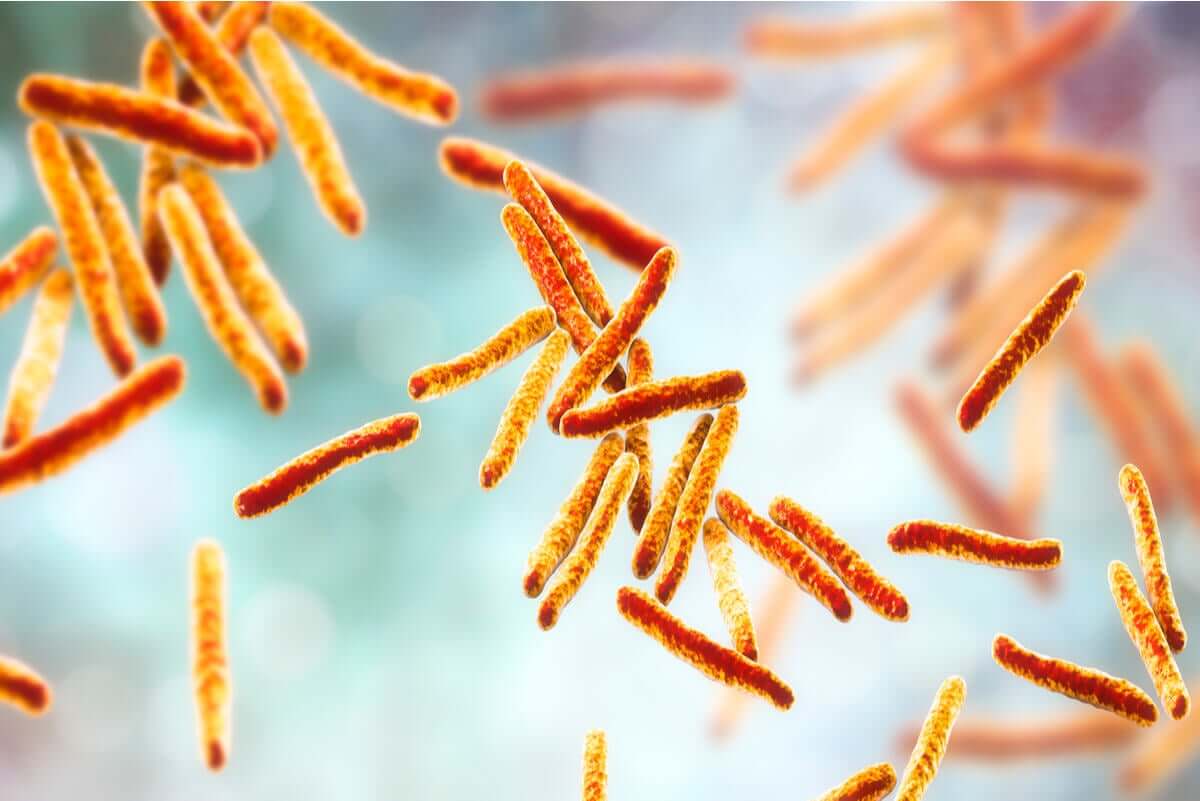
Causes of pulmonary tuberculosis
Pulmonary tuberculosis, as it’s caused by bacteria, is a contagious disease. This means that an infected person can spread it to someone else who doesn’t have the infection. If the infection is latent, there’s no spread.
Transmission occurs through water droplets from a cough or sneeze of a person with the disease. Many people recover from pulmonary tuberculosis without serious illness. However, in some cases, the infection reactivates only a few weeks after it’s occurred.
Find out more: Renal Tuberculosis: Diagnosis and Treatment
Risk Factors
Some people are at greater risk of developing pulmonary tuberculosis. These include the following groups:
- Infants: Under the age of 2 years old.
- Older people: Individuals over the age of 60.
- Weakened immune system: Either from diseases such as HIV and diabetes or from taking medications or chemotherapy
The risk of suffering from pulmonary tuberculosis increases if a person suffers from malnourishment, lives in unsanitary conditions, or is in contact with infected people. Also, outbreaks are more frequent in communities where there are more HIV patients, homeless people, or resistant strains.
You may also be interested in: All About Rifampicin and Tuberculosis
Factors that don’t produce risk
As we stated, a person with the latent infection doesn’t spread the disease to others. In the same way, tuberculosis doesn’t spread by contacts such as shaking hands or sharing personal items (toothbrush, silverware, etc).
Nor does it spread by sharing food or drinks, kissing, using the same toilet, or by coming into contact with an infected person’s bedding. It’s not necessary to disinfect surfaces that a person with pulmonary tuberculosis has touched.
Symptoms of pulmonary tuberculosis
The most conventional symptom of pulmonary tuberculosis is a severe cough that can last three weeks or more. This cough is usually accompanied by bloody sputum. The affected person feels great discomfort and has the following symptoms:
- Chest pain
- Weakness or fatigue with lack of appetite, leading to weight loss
- Fever and chills with night sweats
- Wheezing in the chest and difficulty breathing
Some people with pulmonary tuberculosis also have so-called Hippocratic fingers in the advanced stages. These have a widening, drum-stick shape, and a change in the angle of the nail growth.
It’s also common to have tender or swollen lymph nodes in the neck and other parts of the body. Similarly, there may be pleural effusion, that is, fluid around the lung. In some cases, complications appear such as liver inflammation, brown or orange tears and urine, rash, and vision changes.
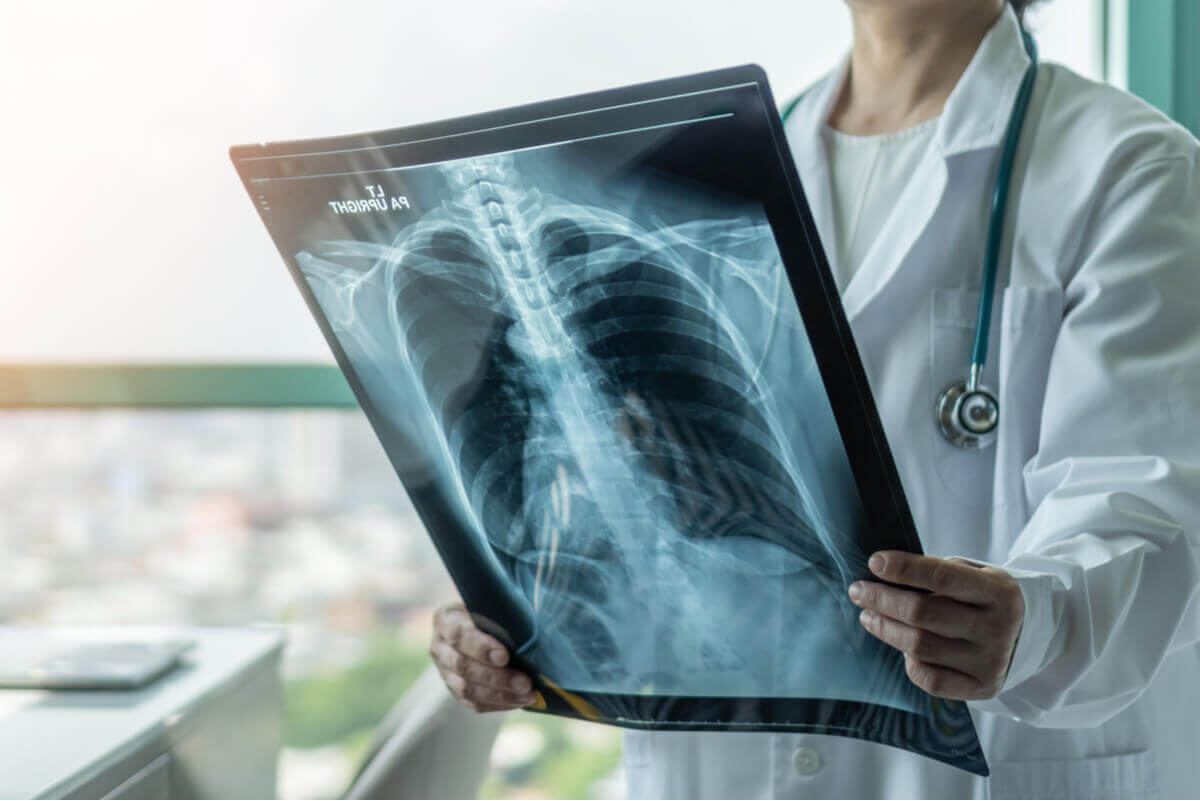
Early detection improves prognosis
Patients with the latent infection don’t have any symptoms or feel any discomfort. A skin test or blood test reveals that they are positive for TB when they undergo testing for another reason. Even if there are no symptoms, it’s important to initiate treatment to prevent progression of the disorder.
When the detection and treatment of pulmonary tuberculosis takes place early on, prognosis is excellent. Symptoms usually disappear within two to three weeks. Failure to treat the disease properly has fatal consequences.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Izurieta, M. (2014). La nutrición y la tuberculosis en los usuarios que acuden al centro de salud del canton Chillanes, provincia Bolívar.
- Grupo de Trabajo de Tuberculosis de la Sociedad Española de Infectología Pediátrica. (2006, January). Documento de consenso sobre el tratamiento de la exposición a tuberculosis y de la infección tuberculosa latente en niños. In Anales de Pediatría (Vol. 64, No. 1, pp. 59-65). Elsevier Doyma.
- Alpi, S. V., Quiceno, J. M., Fernández, H., Pérez, B. E., Sánchez, M. O., & Londoño, A. (2007). Calidad de vida relacionada con la salud y apoyo social percibido en pacientes con diagnóstico de tuberculosis pulmonar. Anales de Psicología/Annals of Psychology, 23(2), 245-252.
- Rincon Zuno, Joaquin. “Cual es la prueba de mayor utilidad diagnostica para tuberculosis en menores de dos años.” (2019).
- Paneque Ramos, Ena, Liana Yanet Rojas Rodríguez, and Maritza Pérez Loyola. “La Tuberculosis a través de la Historia: un enemigo de la humanidad.” Revista Habanera de Ciencias Médicas 17.3 (2018): 353-363.
- Barrios-Payán, Jorge A., et al. “Aspectos biológicos, clínicos y epidemiológicos de la tuberculosis latente.” salud pública de méxico 52.1 (2010): 70-78.
- Herrera, Tania. “Grupos de riesgo para tuberculosis en Chile.” Revista chilena de infectología 32.1 (2015): 15-18.
- Beijer, Ulla, Achim Wolf, and Seena Fazel. “Prevalence of tuberculosis, hepatitis C virus, and HIV in homeless people: a systematic review and meta-analysis.” The Lancet infectious diseases 12.11 (2012): 859-870.
- Smud, Astrid. “Eficacia del tratamiento de la infección latente por tuberculosis.” Evidencia, actualizacion en la práctica ambulatoria 22.2 (2019): e001095-e001095.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








