What Is Rapid Sequence Induction?
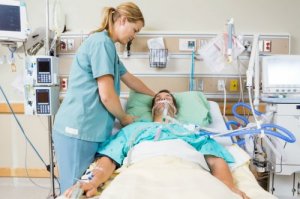
Changes in a person’s airways can lead to death. However, rapid sequence induction can be the key to saving many lives.
Rapid sequence induction refers to an orotracheal intubation. This procedure is normally performed in the emergency room. However, in order for it to be successful, it’s necessary to follow a series of orderly steps that, if skipped, can put the patient’s life at risk.
As one study states: ‘for the medical specialist in emergency medicine, the management of the airways in the Pre-Hospital Care Units and Emergency Services is a fundamental part of their basic competencies.’
Therefore, it’s essential that doctors know how to perform a rapid sequence induction. This will reduce the risk of pulmonary aspiration in some patients.
When do doctors perform rapid sequence induction?

People need rapid sequence inductions when they arrive at the emergency room with an imminent risk of ventilatory failure. A quick evaluation will prevent the doctors from carrying out the procedure without precision.
The consequences of performing a rapid sequence induction can range from hypoxemia to causing an injury in the airway when the orotracheal tube is inserted. Therefore, it’s important to stay calm and to follow the steps exactly.
In some cases it’s not clear when orotracheal intubation should be carried out. However, when there’s a possibility that the patient may need it, the doctor will perform it.
However, the following symptoms should be taken into account. They can clearly indicate the need for a rapid sequence induction:
- Swollen hematoma in the neck
- Thoracic trauma with hypotension
- Extensive burns
- Obstruction of the airway
- Heart attack
If, in addition to all this, the patient is agitated because they can’t breathe normally, then they’ll need immediate sedation. After that, the doctor should perform the rapid sequence induction as soon as possible.
Discover: 6 Habits that Damage your Lung Health
Correct procedure
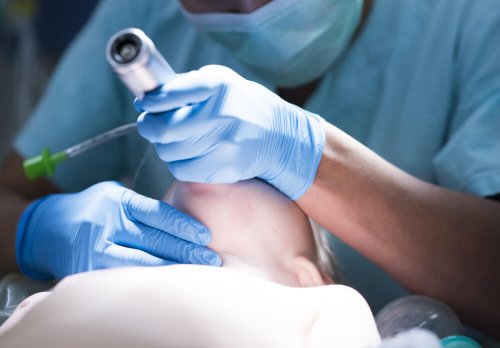
In order to perform a successful intubation, a series of steps must be followed. The doctors will carry out these steps in an agile, quick, and precise manner. That way, they’ll be able to avoid some of the consequences that we mentioned previously.
Pre-intubation actions
- Raise the patient’s head by placing a pillow underneath it.
- Lift their jaw by pushing it up and forward.
- Remove any foreign bodies from the oropharyngeal cavity.
- Aspirate all secretions (blood, vomit).
Rapid sequence induction
- Hold the laryngoscope with one hand and insert through the corner of the mouth, moving the tongue and bringing the laryngoscope forward and up.
- Place the tip of the instrument in the epiglottis.
- To reduce the risk of aspiration or regurgitation, another professional must perform the Sellick maneuver. They must do this within the duration of the intubation.
- In the event that the glottis or vocal cords aren’t very visible, another person should perform the BURP maneuver to expose them. This will allow the doctors to properly place the laryngoscope without damaging the airway.
- When the doctor inserts the tube correctly, they will remove the laryngoscope without moving the tube. They will then fix and connect it to the oxygen source.
Although we recommended using the Sellick and BURP maneuvers, these should never be used if the patient is suffering from trauma or has a foreign body in the trachea. This is very important to keep in mind.
Read this article: Thiopental: How it’s Administered and Precautions for Use
Medications
In general, the use of medications isn’t necessary when performing rapid sequence induction. However, there are cases where, without these medications, it would be impossible to intubate the patient.
When a patient is restless, it’s necessary to give them a sedative. In other cases, when the patient is in severe pain, you should also give them an analgesic in addition to a sedative.
There are a few circumstances in which emergency room doctors have to provide patients with a micro-relaxant. This is essential when the tube cannot pass through the trachea due to pressure.
As you can see, induction is a procedure that all professionals who work in the emergency room should know how to carry out correctly. That way, they can ensure their patients will experience the least possible damage to their airways.
Additionally, it’s important to know the medicines they should use in certain situations. Rapid sequence induction is definitely an essential first aid measure.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Almarales, J. R., Saavedra, M. Á., Salcedo, Ó., Romano, D. W., Morales, J. F., Quijano, C. A., & Sánchez, D. F. (2016). Inducción de secuencia rápida para intubación orotraqueal en Urgencias. Repertorio de Medicina y Cirugía, 25(4), 210-218.
- Calvache, J. A., Sandoval, M. X., & Vargas, W. A. (2013). Fuerza aplicada por el personal de salud sobre un simulador del cartílago cricoides durante la realización de la maniobra de Sellick en la intubación de secuencia rápida. Revista Colombiana de Anestesiología, 41(4), 261-266.
- Carrillo-Esper, R., Vinay-Ramírez, B., & Bahena, A. (2008). Maniobra BURP. Revista mexicana de Anestesiología, 31(1), 63-65.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








