What Is a Malignant Melanoma?
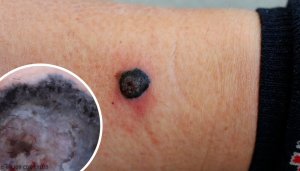
A malignant melanoma is a cancerous tumor that normally develops on the skin. Sometimes it can also appear on a mucous membrane or on other areas of the body. It’s the most deadly form of skin cancer because it spreads easily to other parts of the body.
This type of tumor appears when melanocytes, skin cells that produce melanin, acquire cancerous characteristics. It is the third most common type of skin cancer; in fact, its worldwide diagnosis has increased in recent decades. The mortality rate associated with the disease has also increased.
It’s common for doctors to have appointments for skin lesions that have pigmentation. In order to prevent melanoma, it’s recommended that we assume that any mark with these characteristics is a malignant melanoma. Early diagnosis is fundamental for the good prognosis of the disease.
Risk factors and types of malignant melanomas
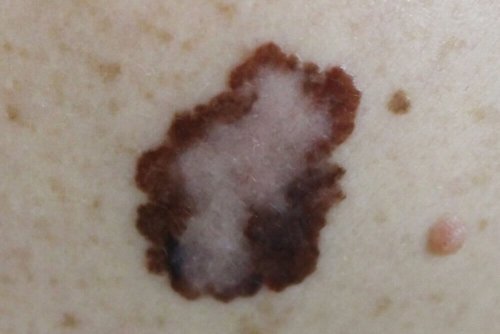
People with a higher risk of developing a malignant melanoma are redheaded people with fair skin, people with a lot of moles, or those who frequently get sunburn. Only 25% of malignant melanomas are from a pre-existing mole.
In general, men tend to get malignant melanomas on the back, while in women, the most common area is on their the legs. In general, malignant melanomas initially resemble a normal mole, which changes little by little, increasing in size and acquiring a more irregular shape.
We can distinguish up to four types of malignant melanomas:
- Extensive and superficial: This applies to 70% of cases. They show up mainly on the legs and on the abdomen. It’s a flat lesion, with some elevated areas. It grows slowly and has a variety of colors (gray, red, black, blue or brown).
- Nodular: This applies to 15% of cases. It’s a raised lesion and black, blue or colorless and they grow very quickly.
- Lentiginous: This covers about 5% to 10% of cases. This malignant melanoma has a papule or nodule appearance and usually appears in elderly people. It is brown, black, blue or without pigment. It grows slowly.
- Lentigo maligna: This type covers around 5% of cases. It appears in older people on their faces, necks or the backs of their hands. It’s a flat lesion, with smaller bulky areas. It has blue or gray tones and grows very slowly.
Diagnosis of malignant melanoma

As mentioned before, when a strange mole appears on the skin or something that resembles it, we should assume that it’s a malignant melanoma. There is an acronym – the “ABCDE rule“- that’s used to accurately detect this type of tumor. Evaluate each skin lesion to see if it has the following characteristics:
- A: Asymmetric, that is, with an irregular shape.
- B: Irregular edges.
- C: Irregular coloration.
- D: Diameter is greater than 6 mm.
- E: Evolution, that is, it changes over time.
When a lesion meets these characteristics, a doctor will order a biopsy or the removal of the lesion. In both cases, the doctor carries out a histopathological study. This means that, to determine if it’s malignant melanoma, the tissue that was removed will be studied. They also measure the depth of it.
The main measure of prevention against a malignant melanoma is to protect your skin from ultraviolet radiation, both natural and artificial. We must avoid exposing our skin to the sun’s rays, especially during the hottest hours of the day. On the other hand, an early diagnosis considerably increases the chances of a cure.
Complications and prognosis

If the melanoma is deeper, the problem is usually more serious. With this melanoma, it must be determined if the sentinel lymph node has been reached, meaning the nearest lymph node to the melanoma.
The prognosis of malignant melanoma depends on several factors:
- Localization
- Thickness
- Mitotic index, that is, how often cancer cells multiply
- Level of invasion
- Infiltration of lymphoid
- Ulceration
Doctors will take the growth of the melanoma into account. However, the factor that influences the prognosis most is whether the melanoma remains in the same area or if, on the contrary, it has spread. In the first case, the prognosis is very positive, while the second case usually leads to serious forecasts.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Calderón, M. B., & Martín, R. L. (2011). Factores de riesgo y detección temprana del melanoma maligno en pacientes con nevus melanocíticos. Más Dermatología. https://doi.org/10.5538/1887-5181.2011.14.5
- Carbajosa-Martìnez, J., & García-de Acevedo, B. (2017). Melanoma maligno. Dermatologia Revista Mexicana.
https://doi.org/10.1016/S1134-2072(07)71533-5 - Moreira, J., Moreira, E., Azevedo, F., & Mota, A. (2014). Melanoma maligno cutâneo: Estudo retrospetivo de sete anos (2006-2012). Acta Medica Portuguesa.
https://doi.org/10.20344/amp.5211 -
Schadendorf, D., van Akkooi, A. C. J., Berking, C., Griewank, K. G., Gutzmer, R., Hauschild, A., … Ugurel, S. (2018, September 15). Melanoma. The Lancet. Lancet Publishing Group.
https://doi.org/10.1016/S0140-6736(18)31559-9 -
Gershenwald, J. E., Giacco, G. G., & Lee, J. E. (2013). Cutaneous melanoma. In 60 Years of Survival Outcomes at the University of Texas MD Anderson Cancer Center (Vol. 9781461451976, pp. 153–165). Springer New York.
https://doi.org/10.1007/978-1-4614-5197-6_15
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








