Types of Scars

Written and verified by the doctor Leonardo Biolatto
The skin can heal in different ways, because not all wounds are the same. How the injuries are caused can either produce deeper or more superficial wounds. This is what determines the different types of scars that form on our bodies.
It’s also important to consider which layer of the skin the wound has affected, since it’s formed by three layers: epidermis, dermis and hypodermis or subcutis. The epidermis is the most superficial layer and is the one in contact with the exterior, while the hypodermis is the deepest, in contact with the interior of the body.
The intermediate layer of the skin is the dermis and it can produce pathological scars when it’s affected by a wound deep enough to penetrate it. The dermis is a highly specialized tissue, and hence the difficulty when trying to repair it.
First, let’s see how the skin reacts to a wound to produce a scar, and then we’ll talk about the different types of scars.
Healing phases
When the skin is wounded, it triggers a series of successive phenomena to repair it. The way these phases are carried out is what determines the types of healing. There are five phases of healing:
1. Coagulation and vascular response
As soon as the injury occurs, the blood washes the wound. Foreign bodies are dragged out of place to avoid infection. Then, with the help of platelets, the vessels are closed to clot and stop bleeding.
2. Inflammation
The second phase is the inflammatory one. Although the skin becomes red, this isn’t an indication of an infection. The redness of the inflammation is from intense cellular movement and increased blood flow. A clear inflammatory fluid may even form in the wound, which isn’t a sign of infection either.
3. Granulation
Now the essence of the repair begins. The cells that are most involved are the fibroblasts, which travel to the site of the injury to produce collagen. Collagen is the main component of the dermis; therefore, it’s the one that replaces the lost tissue.
Discover more: 5 Natural Solutions to Treat Bruises
4. Epithelialization
A final function of wound repair is to restore the layer that separates the external from the internal. The skin has its barrier function thanks to the epidermis. Epithelialization consists of re-forming epidermis that disappeared through cells called keratinocytes.
5. Remodeling
Once the wound closes, the body’s healing process defines the scar’s final aspect. If the wound only affected the epidermis, there’s usually just cell regeneration and the scar is usually normal. On the other hand, if the wound was deep, there’s a greater possibility of having a pathological scar.
Types of healing
Skin healing phases are always the same in all wounds, but not all wounds are the same. That’s why three types of healing processes have been identified in the world of dermatology and surgery:
First intention
This is the process that occurs when the wound is small; it isn’t deep and the edges of the wound are close. It doesn’t usually leave a long-term scar.
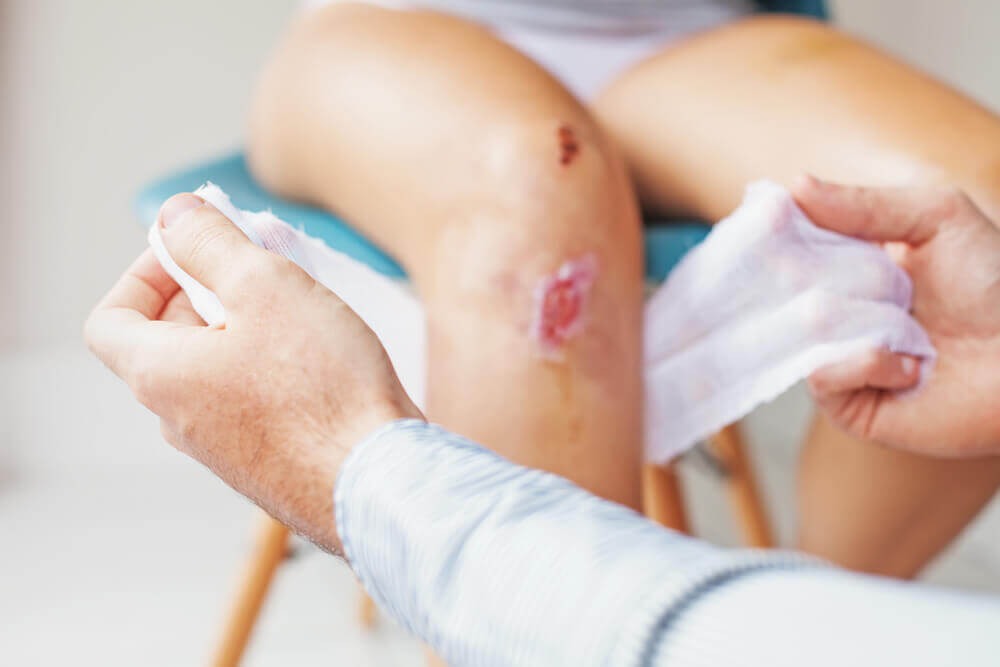
Second intention
This is the healing process of a deeper wound which affects the dermis. The result is usually a larger than usual scar with a striking appearance. The main cause is the loss of substance or the existence of a very large distance between the edges of the wound. When that happens, the dermis must form a lot of new tissue in the granulation stage, and that’s the reason for the final scar.
Third intention
This type of scarring is associated with medical intervention. This scarring appears when the surgeon places a second suture over an existing one, or when they add dermal grafts for repair. The medical intervention guides this final scar.
You may be interested in: 4 Natural Home Remedies to Eliminate Acne Scars
Types of scars
Although there are normal and expected scars, there are also scars that medicine considers pathological. Let’s see how they’re medically classified:
- Normal: appears after a routine process. The final result is a fine line.
- Atrophic: loss of substance in the skin, when there’s a small depression in the area where the wound was. This is something that’s very common with acne, for example.
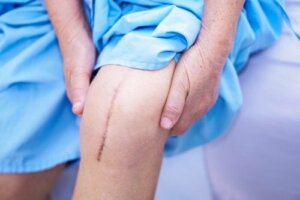
- Hypertrophic: scars caused by types of scarring with excessive collagen production. The resulting skin is thick and protrudes above the level of the normal epidermis. It usually occurs in areas of the skin with constant movement, such as the knee.
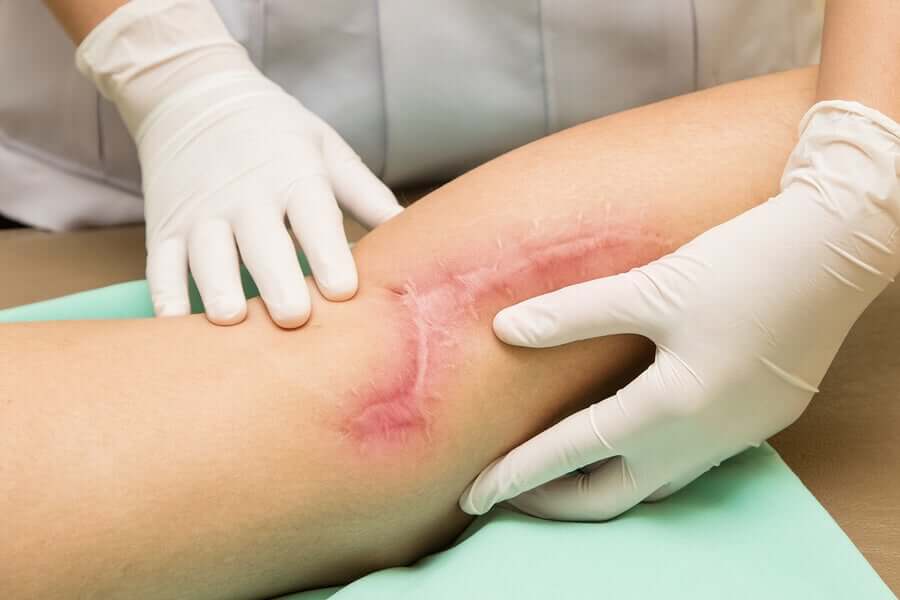
- Keloid: excessively large hypertrophic scar. It may itch and even cause some burning. It usually extends beyond the initial limits of the wound that originated it.
- Contracture: this is what scars that come from burns are called. The scar tissue contracts and deforms the affected area.
Each of these types of healing that result in different forms of scars have a medical approach. You can consult a surgeon or a dermatologist if you have a scar that concerns you. The professional will know and tell you the best approach for your case.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Andrades, Patricio, and Sergio Sepúlveda. “Cicatrización normal.” Cirugia Plástica Esencial Santiago: Universidad de Chile (2005).
- Basto, Carlos Valencia. “Cicatrización: proceso de reparación tisular. Aproximaciones terapéuticas.” Investigaciones Andina 12.20 (2010): 85-98.
- Yousef H, Alhajj M, Sharma S. Anatomy, Skin (Integument), Epidermis. [Updated 2019 Jun 12]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2019 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK470464/
- Senet, P. “Fisiología de la cicatrización cutánea.” EMC-Dermatología 42.1 (2008): 1-10.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








