Physical Signs that Psychological Violence Leaves Behind

Violence is a type of social or personal interaction in which there is a clear intention to cause harm or damage to the other party. It can be so subtle to the point of going unnoticed. Psychological violence, although it isn’t physical, can also leave signs in the body.
So, below we’ll tell you about some of their effects on your body and the health problems they can lead to.
What’s psychological violence?
Psychological violence is a type of verbal abuse (not physical) where the perpetrator tries to subdue another person by abusing their power over them. It manifests itself through humiliation, disqualifications, harassment, insults, isolation, or bullying that discriminates against the dignity of the victim.
Since there’s no physical evidence such as bumps, scratches, or bruises, sometimes it can be difficult to prove, since it’s the word of one person against the other.
Signs left on the body by psychological violence
1. Sleeping disorders
Psychological abuse usually results in sleeping disorders. The high doses of pressure and verbal violence cause psychological states of anxiety and stress, which are often associated with insomnia or poorer quality rest.
As a study by the Netherlands Institute for Neuroscience points out, these states of constant alertness are associated with sleep problems, which, in turn, have an impact on the discomfort experienced during the day.
In other words, in these circumstances, sleep doesn’t repair the stressful situation that the victim is experiencing, and the victim becomes even weaker, unable to cope with the pain effectively.
This initiates a whole chain of alterations in which other systems of the body are ultimately involved. This occurs at both the metabolic and cardiovascular levels, according to a recent review conducted by researchers at the University of Seoul (South Korea).
Read about Restful Sleep – How Much Do We Really Need?
2. Hypertension
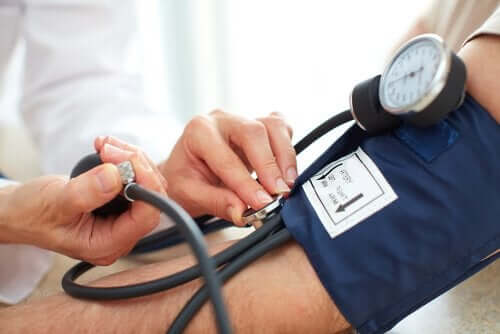
Learn about Candesartan: Common Treatment for Hypertension
3. Eating disorders
As explained in a paper by Dr. Markus J. Rantala and his team, eating disorders are mediated by the stress response of each individual.
If it becomes chronic, one of the possible consequences is the variation of basic habits such as diet. Thus it happens that victims of psychological violence suffer disturbances such as:
- Loss of appetite
- Lack of control
- Insecurity and disregard for what one eats
There are factors that can lead to these eating disorders, such as feelings of loneliness, frustration, contained anger or emotional distress. These are features that often characterize the pain experienced and make the emotional stress even more intense.
4. Depression
There are many signs of psychological violence that result in illness or mental disorder:
- Blackmail
- Uncontrolled jealousy
- Deprivation of liberty
- Invasion of privacy
- Dominance and submission
- Insulting and humiliating nicknames
- Non-consensual sexual relations
- Screams, insults, and disparagements
- Total control of money, clothing or social relations
In the face of these attacks, the affected person comes to present some of the symptoms that are characteristic of depression. Furthermore, if these symptoms persist over a long period of time, the deterioration of the victim’s self-esteem can be devastating and lead to significant mood disorders.
For all this, it isn’t strange that the victim. This is because even without presenting symptoms of physical violence, falls into a state of desolation. Furthermore, the person can get to the point of becoming suicidal as the only way out.
In addition, the aggravating factor is that, usually, the aggressor is usually the partner or a close member of the family.

Tips to prevent psychological violence
The signs that psychological violence leaves behind may not be obvious to the naked eye. However, if you pay a little attention, you can see that they’re there and that they affect the person’s quality of life.
Therefore, if you detect that you’re in a situation of this type and, in addition, you identify certain signs such as those mentioned above, asking for help is a priority.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Coker, A. L., Davis, K. E., Arias, I., Desai, S., Sanderson, M., Brandt, H. M., & Smith, P. H. (2002). Physical and mental health effects of intimate partner violence for men and women. American Journal of Preventive Medicine, 23(4), 260–268. https://doi.org/10.1016/s0749-3797(02)00514-7
- Dokkedahl, S., Kok, R. N., Murphy, S., Kristensen, T. R., Bech-Hansen, D., & Elklit, A. (2019). The psychological subtype of intimate partner violence and its effect on mental health: protocol for a systematic review and meta-analysis. Systematic Reviews, 8(1), 198. https://doi.org/10.1186/s13643-019-1118-1
- Kimber, M., McTavish, J. R., Couturier, J., Boven, A., Gill, S., Dimitropoulos, G., & MacMillan, H. L. (2017). Consequences of child emotional abuse, emotional neglect and exposure to intimate partner violence for eating disorders: a systematic critical review. BMC Psychology, 5(1), 33. https://doi.org/10.1186/s40359-017-0202-3
- Koo, D. L., Nam, H., Thomas, R. J., & Yun, C. H. (2018). Sleep Disturbances as a Risk Factor for Stroke. Journal of Stroke, 20(1), 12–32. https://doi.org/10.5853/jos.2017.02887
- Mwakanyamale, A. A., & Yizhen, Y. (2019). Psychological maltreatment and its relationship with self-esteem and psychological stress among adolescents in Tanzania: a community based, cross-sectional study. BMC Psychiatry, 19(1), 176. https://doi.org/10.1186/s12888-019-2139-y
- Rantala, M. J., Luoto, S., Krama, T., & Krams, I. (2019). Eating Disorders: An Evolutionary Psychoneuroimmunological Approach. Frontiers in Psychology, 10, 2200. https://doi.org/10.3389/fpsyg.2019.02200
- Rivera, P. M., Fincham, F. D., & Bray, B. C. (2018). Latent Classes of Maltreatment: A Systematic Review and Critique. Child Maltreatment, 23(1), 3–24. https://doi.org/10.1177/1077559517728125
- Simmons, J., Wijma, B., & Swahnberg, K. (2015). Lifetime co-occurrence of violence victimisation and symptoms of psychological ill health: a cross-sectional study of Swedish male and female clinical and population samples. BMC Public Health, 15, 979. https://doi.org/10.1186/s12889-015-2311-3
- Wassing, R., Benjamins, J. S., Dekker, K., Moens, S., Spiegelhalder, K., Feige, B., Riemann, D., van der Sluis, S., Van Der Werf, Y. D., Talamini, L. M., Walker, M. P., Schalkwijk, F., & Van Someren, E. J. (2016). Slow dissolving of emotional distress contributes to hyperarousal. Proceedings of the National Academy of Sciences of the United States of America, 113(9), 2538–2543. https://doi.org/10.1073/pnas.1522520113
- Wilkins, N., Myers, L., Kuehl, T., Bauman, A., & Hertz, M. (2018). Connecting the Dots: State Health Department Approaches to Addressing Shared Risk and Protective Factors Across Multiple Forms of Violence. Journal of Public Health Management and Practice, 24, S32–S41. https://doi.org/10.1097/phh.0000000000000669; texto completo
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








