Skin Grafting: When Is It Used?

Written and verified by the doctor Maryel Alvarado Nieto
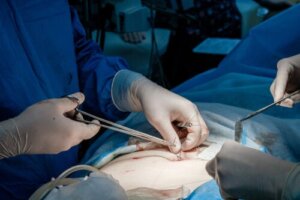
The skin is the organ that covers our body and serves as a barrier to the world around us. In this way, it protects us against infections and also protects us from the conditions of both our internal and external environments. Certain skin injuries are so extensive or complex that they require skin grafting to treat them.
The purpose of this type of surgical treatment is to confer indemnity to the tissue. In this way, the underlying structures are protected and the barrier effect of the skin is ensured. In the end, it not only covers the defect caused by the injury, but also aims to create aesthetic results. In this article, we’ll tell you more about it.
What is skin grafting?
A skin graft is a fragment of skin that is obtained through surgery. In this surgery, this piece is completely separated from a body region – called the donor region -, and then transplanted to the recipient site – that is, the place that has a defect or injury.
Since this place is separated from its donor site, the graft loses its blood flow. For this reason, the recipient tissue must be able to provide it with adequate irrigation. In this way, the transplanted skin can revascularize and therefore survive in its new location.
Skin layers
To understand the types of skin grafts that exist, it’s necessary to know the histological layers of the skin.
The epidermis is the most superficial layer. This structure lacks its own blood vessels and receives irrigation from the deeper portions of the skin. This causes epidermis-only grafts to fail and means that they are therefore useless.
On the other hand, the deepest layer of the skin is the dermis. In turn, this can be divided into two portions: the papillary dermis and the reticular dermis. The first is the most superficial layer, so its blood vessels are the ones that allow the nutrition of the overlying epidermis. Under the dermis is the subcutaneous cellular tissue, which is rich in fat.
Types of skin grafts
The most commonly used classification in skin grafts responds to the thickness of the skin involved. In general, two types are accepted: partial thickness grafts and full thickness skin grafts.
- Partial thickness grafts: In this case, the thickness is variable, but must always contain a portion of the dermis. This ensures the donation of the necessary elements for cell regeneration and nutrition of the overlying epidermis. Depending on the thickness of the dermis involved, the thickness of this tissue can be thinner or thinner.
- Full-thickness grafts: The sectioned skin fragment has both the epidermis and the entire dermis. The tissue must be devoid of subcutaneous fat to allow for neovascularization.
Grafts according to the form in which the skin graft is used
According to the need to cover the defect, the grafts can be continuous – that is, those formed by one or several fragments that manage to cover all the loss of substance when joined together.
Similarly, there are also discontinuous skin grafts, in which the defect is not covered in its entirety. Among these are the following options:
- Tanner and Vandeput mesh
- Plurifragmented grafts
- Trueba banded grafts
- Gabarro seals
- Davis or lozenge grafts
Special situations
The choice of one type of graft over another responds to several issues. The location of the loss of substance is of utmost importance, as is the selection of the donor site.
Also, the extent of the injury will help to determine which type of graft a person needs. Meanwhile, the cause of the loss of substance helps the surgeon choose the most appropriate thickness.
The characteristics of skin grafting
Depending on the thickness of the fragment, each type of graft has some advantages over others. In addition, the injured tissue also plays an important role in the “catching” of the graft, i.e., in making the technique successful. Some of the characteristics to consider are described below.
Donor and recipient skin
Since skin has a high antigenicity, skin grafts can only come from the same person. This is because the immune system is not able to recognize elements other than its own. Therefore, an immune response is triggered that ends up rejecting the grafted tissue.
This type of transplant – in which the donor is the same individual as the recipient – is known as “autografting”. However, there are situations (such as major burns) in which the use of cadaveric or even pig skin grafts may be useful.
We think you may also enjoy reading this article: 5 Tips to Protect the Skin Against the Effects of Air Conditioning
Donor tissue conditions
The choice of the site from which the skin graft will be taken must be careful to ensure the best possible result. Therefore, fragments are usually taken from sites close to the injury. In general, the following recommendations are suggested:
- It must have a similar color to the recipient site.
- In cases of tumor resection, it’s advisable to choose the contralateral limb to take the graft.
- The tissue must be free of infection.
- The texture and hair distribution between both sites (donor-recipient) is recommended to be similar.
Injured tissue conditions
The recipient bed is the background to which the skin graft should be attached. This must have abundant vascularization to allow the new tissue to survive. However, the presence of infection or hemorrhage decreases the success rate and must be treated first.
Situations in which skin grafting is useful
Despite representing a solution for complex skin injuries, not all body locations allow skin grafts to be the best option. Despite this issue, the main situations in which they are used are the following:
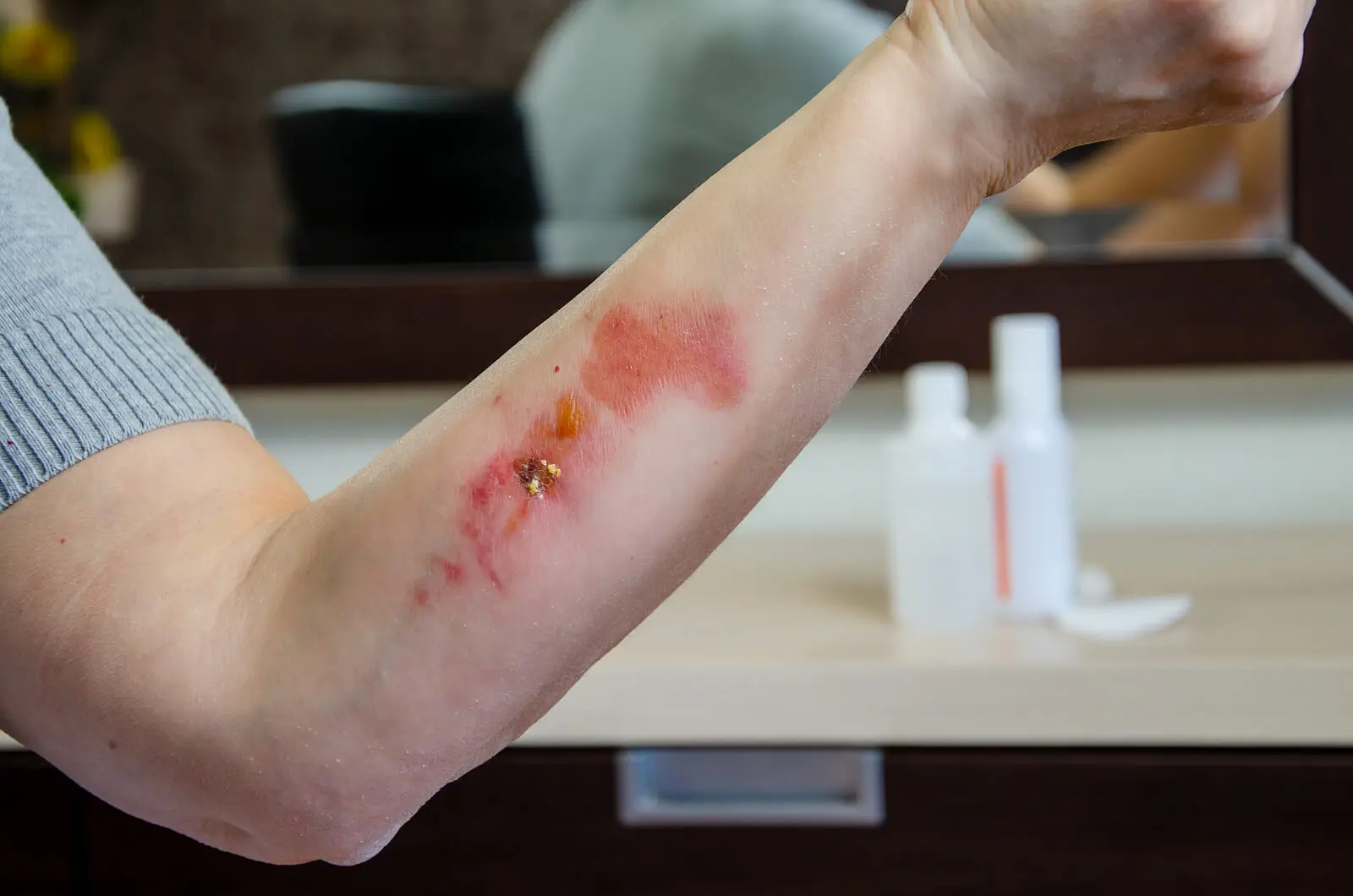
- Large burns
- Extensive wounds
- Resection of skin tumors
- Ulcers in lower limbs
- Defects of mucosal areas
- Fasciotomies
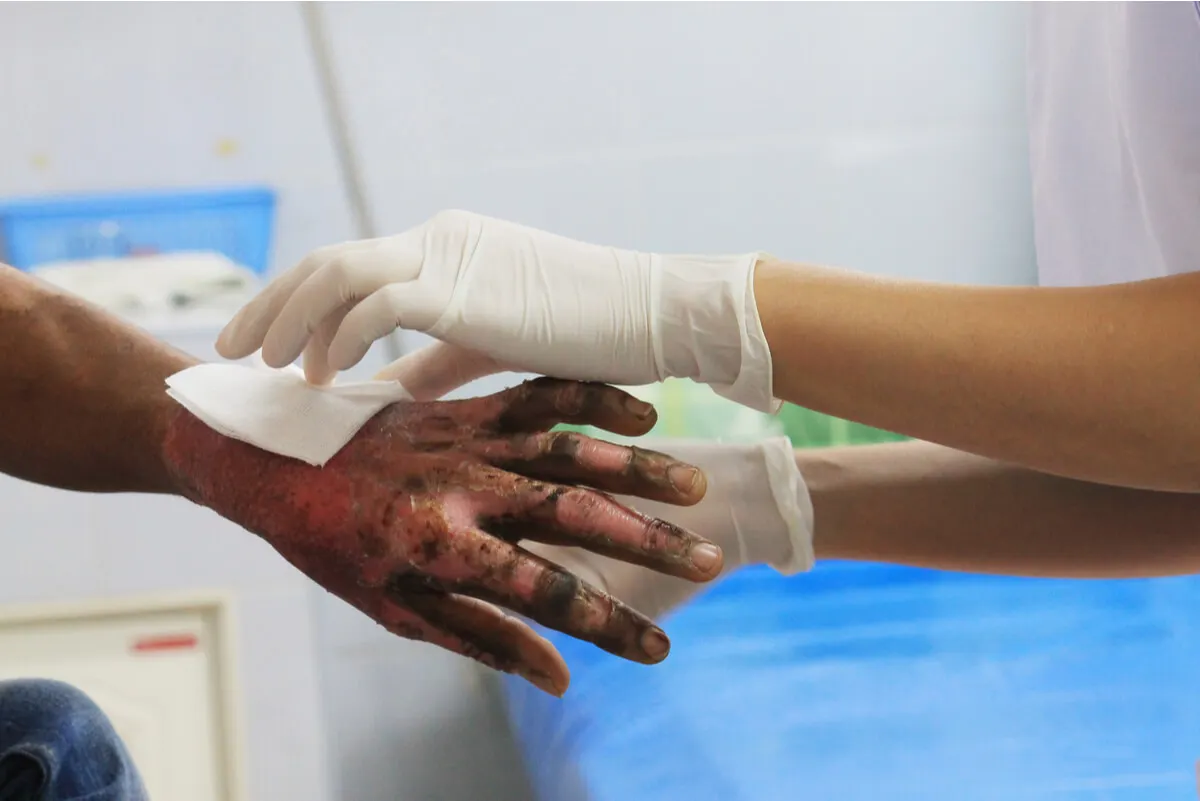
Skin grafts can only come from the same person; otherwise, there’s an immune response that rejects the tissue.
Healing of the injury
In addition to providing vascularization of the tissue, the recipient bed can produce retractions in the skin graft, especially if it’s of partial thickness. For this reason, it’s recommended that full-thickness grafts be used in esthetic areas such as the face, since they allow for better coverage and have less retraction.
On the other hand, when the loss of substance is very extensive, it’s more appropriate to use partial-thickness fragments, which are also discontinuous. Meshing, for example, makes it possible to increase the size of a continuous skin graft by up to three times. This increases the coverage capacity of the fragment, although it represents less esthetic results.
Like this article? You may also like to read: 10 Beauty Treatments that Can Regenerate Skin Collagen
Complications of skin grafting
As in any surgical treatment, there are some risks in skin grafting. The most frequent include the following:
- Hemorrhages
- Hematomas
- Seromas
On the other hand, retractions, scarring, and pigmentation changes may affect the final appearance of the skin graft. In these cases, additional dermatologic procedures may be recommended to improve the final appearance.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Prohaska J, Cook C. Skin Grafting. [Updated 2022 May 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK532874/
- Revol; M.; Servant.; Injertos Cutáneos; Cirugía Plástica Reparadora y estética; 45 – 070; 2010.
- Avellaneda, E.; Coberturas Especiales I: Injertos de Piel; Proyecto Lumbre; 7 – 18;
- Avellaneda, E.; González, A.; González, S.; Palacios, P.; Rodríguez, E.; Bugallo, J.; Injertos en Heridas; Heridas y Cicatrización; 2 (8); 2018.
-
Braza ME, Fahrenkopf MP. Split-Thickness Skin Grafts. [Updated 2022 May 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK551561/
-
Ramsey ML, Walker B, Patel BC. Full Thickness Skin Grafts. [Updated 2022 May 2]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK532875/
- Blatière, V.; injertos Cutáneos: Injertos de Piel de Grosor Variable y Total; EMC – Dermatología; 55 (1) 2021.
- Castillo. P.; Villafranca, A.; Injertos de Davis; Cuad. Cir.; 16: 64 – 68; 2002.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








