Pope Francis' Symptomatic Diverticular Stenosis


Written and verified by the doctor Leonardo Biolatto
The symptomatic diverticular stenosis affecting Pope Francis made headlines around the world as it landed him in the hospital. It wasn’t an emergency, however, but only a scheduled procedure to improve the man’s quality of life.
This affectation of the digestive system is common in the elderly. Thus, the older one gets, the more frequent its incidence. Indeed, most cases are asymptomatic although some manifest as abdominal pain or changes in bowel movements.
In the case of Pope Francis, the condition is the result of a somewhat more complex evolution than normal. This is why he required surgery, although it isn’t a major intervention.
Today’s article will discuss this disease in more detail.
Symptomatic diverticular stenosis and diverticulosis
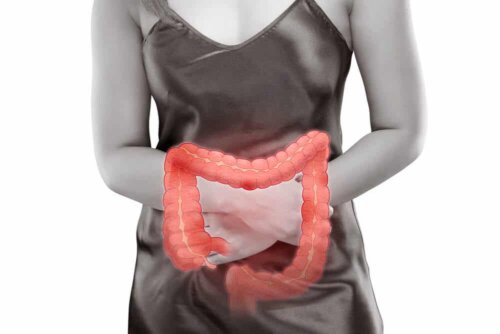
Colon diverticula are small pouches that form in the wall of this organ. The colon is the large intestine, that is, the final part of the digestive tract responsible for dehydrating the fecal bolus to form the waste (feces).
These pockets in the wall protrude outwards and create a space that can receive substances, become infected, or even perforate. These complications are rare, but some risk factors increase the chances.
A person with several diverticula has diverticulosis. It isn’t common in people under 40 but its incidence increases as people age. To such an extent that half of all human beings over 60 years of age have it.
The mechanism that explains the formation refers to the pressure inside the digestive tract. An increase of this force in the lumen of the colon, the mucosa, and the submucosa of the organ wall prolapse outwards. Thus, the small sac forms, usually in areas where the anatomical structure is weaker.
Risk factors for diverticulosis
Clearly, age is a risk factor for the formation of diverticula in the colon. Thus, it’s also logical to think there are circumstances added to aging. These refer to asymptomatic diverticulosis as such and not necessarily to symptomatic diverticular stenosis — that’s the case with Pope Francis’ disease.
- Dietary fiber stimulates peristalsis (bowel movements), so a diet with few vegetable components will lead to constipation and this will increase the pressure inside the colon. In general, those who eat this type of diet consume more animal products and these contain saturated fats. They’re linked to a higher incidence of constipation.
- The lack of physical activity also reduces peristalsis and has the same effect as the lack of fiber.
- Being overweight is closely linked to diverticulosis. It can be due to two habits mentioned above: a diet low in fiber and a sedentary lifestyle.
- One of the many negative effects of smoking on health is the increased risk of diverticula. This is because it increases the incidence of infections. The name for this condition is diverticulitis.
Learn about the Habits that Damage Your Intestines
Symptomatic diverticular stenosis as a complication of diverticulitis
Pope Francis underwent surgery for symptomatic diverticular stenosis over his preexisting diverticulosis. Most patients have no signs of diverticula and many are never aware of the condition.
The most common complication is diverticulitis. This is the inflammation of the existing pouches due to local irritation, impaction of fecal matter, or infection. Approximately a quarter of patients with diverticulitis experience complications due to one of the following processes:
- Some of the pus will surround the large intestine and might generate a larger collection if the diverticulum becomes infected and perforates.
- A fistula is a communication between two hollow organs or between an internal part of the body and the outside. Infected perforated diverticula can generate an abnormal duct that joins the large intestine with the small intestine or the colon with the bladder.
- The inflammation of the peritoneum is a serious condition. The pus from the infected diverticula can reach the abdominal cavity and generate a clinical condition requiring urgent attention if an encapsulated abscess fails to form or a fistula doesn’t complete.
- Finally, obstruction or stenosis, such as the one Pope Francis had, is the closure of the lumen of the colon due to inflammation or scarring of the bowel wall. This usually manifests with pain, changes in bowel rhythm. Also, there may even be some fever if the complication develops while there’s an active infection.
Treatment of symptomatic diverticular stenosis
Doctors decided to perform scheduled surgery to fix it after they determined that Pope Francis had symptomatic diverticular stenosis. This becomes necessary when symptoms are noticeable and physicians can predict there won’t be any spontaneous resolution to the obstruction.
In turn, it’s likely for a doctor to prescribe antibiotics to resolve any ongoing infection. This way, they cover all fronts and the patient recovers their normal intestinal transit.
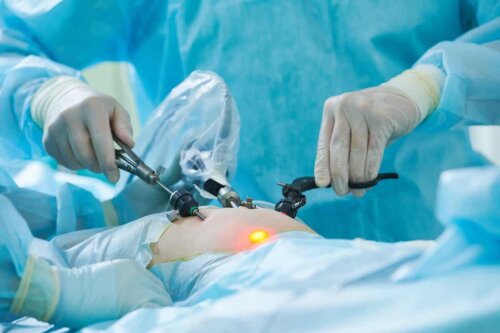
These surgeries are laparoscopic nowadays so the intervention is minimally invasive and recovery doesn’t take too long afterward. Of course, hygienic and dietary support measures are necessary throughout the following days as well as the application of some changes in lifestyle habits.
Finally, the prognosis is good when the patient has no comorbidities and their immune system functions properly. Indeed, there may be recurrences and the rest of the diverticula will still be present. However, only a small proportion of those affected undergo repeated episodes of obstruction.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Bae HJ, Kim ST, Hong SG, Lee H, Choi HS, Cho YK, Kim TH, Chung SH. Risk Factors for Asymptomatic Colon Diverticulosis. Korean J Gastroenterol. 2019 Sep 25;74(3):142-148. doi: 10.4166/kjg.2019.74.3.142. PMID: 31554029.
- Bakopoulos A, Tsilimigras DI, Syriga M, Koliakos N, Ntomi V, Moris D, Bistarakis D, Schizas D. Diverticulitis of the transverse colon manifesting as colocutaneous fistula. Ann R Coll Surg Engl. 2018 Aug 16;100(8):e1-e3. doi: 10.1308/rcsann.2018.0130. Epub ahead of print. PMID: 30112933; PMCID: PMC6204519.
- Camilleri M, Sandler RS, Peery AF. Etiopathogenetic Mechanisms in Diverticular Disease of the Colon. Cell Mol Gastroenterol Hepatol. 2020;9(1):15-32. doi: 10.1016/j.jcmgh.2019.07.007. Epub 2019 Jul 25. PMID: 31351939; PMCID: PMC6881605.
- Tănase I, Păun S, Stoica B, Negoi I, Gaspar B, Beuran M. Epidemiology of diverticular disease — systematic review of the literature. Chirurgia (Bucur). 2015 Jan-Feb;110(1):9-14. PMID: 25800310.
- Tursi A, Scarpignato C, Strate LL, Lanas A, Kruis W, Lahat A, Danese S. Colonic diverticular disease. Nat Rev Dis Primers. 2020 Mar 26;6(1):20. doi: 10.1038/s41572-020-0153-5. Erratum in: Nat Rev Dis Primers. 2020 Apr 29;6(1):35. Erratum in: Nat Rev Dis Primers. 2020 Jun 17;6(1):50. PMID: 32218442; PMCID: PMC7486966.
- Lanas A, Abad-Baroja D, Lanas-Gimeno A. Progress and challenges in the management of diverticular disease: which treatment? Therap Adv Gastroenterol. 2018 Jul 23;11:1756284818789055. doi: 10.1177/1756284818789055. PMID: 30046356; PMCID: PMC6056793.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








