Peripheral Venous Cutdown: Everything You Need to Know
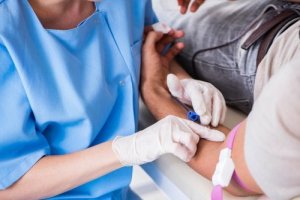
Peripheral venous cutdown is a surgical procedure that aims to expose the vein of an extremity or the neck. It seeks to introduce a cannula that may be short or that may reach the vena cava, or the right atrium.
The access consists of an implanted venous access port that provides patients with safe and permanent access to a vein.
Therefore, experts recommend peripheral venous cutdown to patients that require a cannula in their vein and where percutaneous vascular access is impossible.
Medical professionals often use it in patients who need continuous administration of injectable drugs such as, for example, patients who are getting chemotherapy. The procedure is also called phlebotomy.
Advantages of peripheral venous cutdown
A peripheral venous cutdown is an open surgical procedure. In the same process, the medical professional opens and accesses the cephalic vein.
It can be very favorable for the patient due to the following characteristics:
- Experts can introduce long catheters with direct visualization of the vein
- This way, they can administer chemotherapy, total parenteral nutrition, or also hypertonic solutions
- They can place the catheter tip in the center of the vein
- Using the catheter, the professional can record the central venous pressure
- Catheters can stay in place for long periods of time, even years
Also, it’s important to mention that since the professionals can place the tip into a large vein or the right atrium, they can also prevent the development of sclerosis and phlebitis.
Both conditions can develop when these treatments are passed through blood injection into a peripheral vein, using short catheters.
You should also read: Vascular Perforation and Central Venous Catheters
Peripheral venous cutdown technique
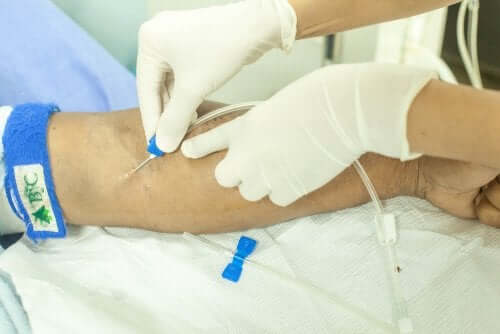
The first thing to consider for the proper execution of the technique is the patient’s position. It’ll depend on the place the medical professional chooses for the procedure.
When it comes to adults, the area medical professionals usually choose is the anteromedial part of the arm. Or, to put it in layman’s terms, above the elbow. The aim here is to work on the basilic vein. Other common places are also:
- External jugular veins of the neck
- The cephalic vein in the deltopectoral groove
- The saphenous arch at the thigh
If the patient is a child, then the process focuses on the saphenous vein. This means 0.4 inches (one centimeter) above and in front of the inner or medial malleolus of the ankle.
It’s essential to note that, if the patient’s condition allows it, then the surgeon should always explain the procedure and get their consent before starting.
After choosing the place where the medical professional will perform the procedure, they’ll then place the patient in the proper position. If the medical professional is going to perform it in the arm or deltopectoral groove, they’ll secure the arm in position the arm.
The professional must always wear the proper clothes, which consist of a cap, mask, sterile gown, and gloves.
Complications

Generally, the complications associated with this technique are based on the surgical procedure that will follow. Thus, the surgical risks are related to the catheter in situ or postoperative risks, which usually occur during postoperative care.
First of all, these are the most common surgical complications:
- Inability or difficulty in identifying or channeling a vein
- Venous rupture or arterial lesions – in this case, there can be really serious consequences
- Vein rupture, bruising, or arterial ligation
- Difficulty moving the catheter
In addition, postoperative complications are based on the catheter’s placement in the vein. This can happen due to a lack of care or it being there for prolonged periods. The risks are as follows:
- Venous thromboembolism
- Phlebitis – this problem arises when the catheter is left in the vein for a long time
- Accumulation of pus in the incision site – this is usually due to infected hematomas that, in the worst case, can lead to the development of generalized sepsis.
This article may interest you: Do You Know the Best Natural Antibiotics?
That’s why good postoperative care is fundamental. For example, professionals recommend handling the catheter with sterile gauze. This way, bacterial colonization is avoided and the catheter remains fixed during handling or when the patient is moved.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Selene Aideé, V. F., José Ángel, B. C., Jesús, T. J., José Luis, J. C., Wulfrano, R. A., & Eduardo E, M.-J. (2012). Modelo biológico no vivo para la enseñanza de la técnica de venodisección en alumnos de pregrado de la carrera de medicina. Cir. Gen.
- Rojas, G., Gerson, R., & Lázaro, M. (1992). Acceso vascular con catéteres Broviac-Hickman. Rev. Inst. Nac. Cancerol. (Méx.).
- Cabrera, C., Méndez, M., Fierro, F., Molina, I., Niño, J., & Beltrán, J. (2011). Catéteres parcialmente implantables en niños con enfermedades onco-hematológicas. CIRUPED.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








