Is Leishmaniasis Contagious?


Written and verified by the doctor Leonardo Biolatto
Leishmaniasis is a disease worth learning about. Its contagious characteristic has turned it into a great public health problem. It appears frequently in 88 countries of the world. It affects 14 million people globally, with 2 million new cases each year.
For one, many consider leishmaniasis one of the seven most important tropical diseases globally. Despite that, this disorder is quite neglected and forgotten. According to a study by the National Epidemiology Center, to take Spain as an example, there were 1,359 autochthonous cases spread over 15 autonomous communities between 2014 and 2017.
Leishmaniasis: what exactly is it?
Leishmaniasis is a contagious infection produced by different species of protozoa of the genus Leishmania. These protozoa, also called parasites, are microscopic organisms that need a vector in order to be transmitted.
Now, a vector is an animal that transmits pathogens from an infected person or infected animal to a healthy person. In other words, the disease isn’t spread by direct contact, there’s a second organism that carries the microorganism.
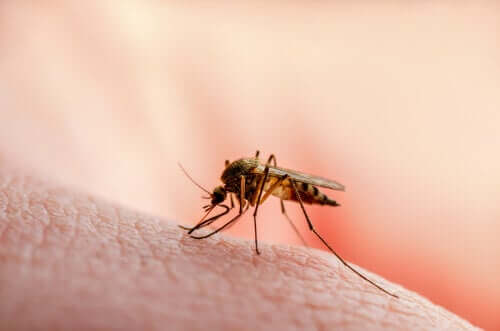
Usually, these vectors are invertebrates, such as mosquitoes, fleas, lice, and ticks. In the case of the pathology we’re talking about in this article, the Leishmania protozoan is transmitted by the bite of the sandfly mosquito.
Read also: 3 natural and homemade mosquito repellents
The mosquito becomes infected when it ingests blood from an infected person or animal. Once inside, the parasite doesn’t cause any symptoms to the vector, it just develops and divides.
When there are a sufficient number of parasites, they go to the mouth and pharynx of the mosquito and are injected at the next bite. The infected sandfly bites another human or animal, injects it with Leishmania, and that’s when contagion occurs.
Despite the human body’s defenses, the pathogen doesn’t die. Instead, it reproduces inside macrophages in the blood and tissues, which end up breaking down and releasing protozoa into the blood, where other macrophages become infected and the cycle continues.
Where are these vectors found?
Sandflies love humidity and heat. For that reason, it’s easy to find them in tropical and subtropical areas. However, it also lives in the Mediterranean basin.
According to the World Health Organization (WHO), leishmaniasis has everything to do with environmental changes. Let’s see some of its risk factors.
- Socio-economic conditions: poverty implies poor housing conditions and poor household sanitation. For that reason, this condition increases the risk of leishmaniasis. This encourages the breeding and resting development of the transmitting mosquitoes.
- Malnutrition: the deficit of proteins, iron, vitamins, and minerals causes an individual to have a weak defense system. This, of course, allows the disease to advance and spread.
- Population mobility: population settlements in formerly wooded areas (which are the mosquito’s habitat) lead to a rapid increase in cases.
- Environmental changes: deforestation, dam construction, irrigation systems, and urbanization cause mosquitoes to have more contact with humans.
- Climate change: Leishmania is very sensitive to changes in weather conditions. Variations in temperature and humidity in different areas make mosquitoes migrate to places where they didn’t live before.
Read also: Find out why viruses are getting stronger
What are the symptoms of leishmaniasis?
There are at least 20 species of protozoa of the genus Leishmania that can be transmitted by vectors. Depending on the species and its degree of invasion in the body, people may present different symptoms. Because of that, this pathology has several varieties.
The three common ways are as follows:
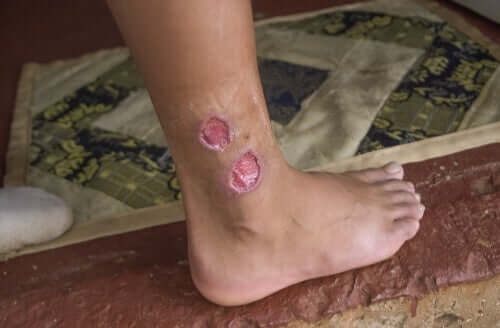
- Cutaneous leishmaniasis: Cutaneous leishmaniasis occurs when the infection occurs only to the area of the bite. Many individuals know it as botón del Oeste and it usually appears on the Mediterranean coast. On the area of the bite, an ulcerated protrusion appears, which sometimes heals automatically, leaving a scar.
- Muco-cutaneous leishmaniasis: the parasite can spread from the skin to the mucous membranes, especially affecting the upper respiratory tract. It occurs with swelling, redness, and ulceration of the mucous membranes.
- Visceral leishmaniasis: in addition to the type of infecting protozoan, it’s also important to bear in mind the immunity of the infected person. When their defenses fail, the parasite migrates into the viscera. The internal organs most affected are the bone marrow, lymph nodes, liver, and spleen.
How can you prevent catching leishmaniasis?
Leishmaniasis is contagious as long as the vector exists. No one really knows if there’s actually a human-to-human transmission, except for specific cases that have been recorded, for example, with people who share syringes to inject drugs. However, regular blood transfusions are totally safe since they go through many controls.
However, it’s true that there will be more mosquitoes in a place where there are infected people. Evidently, this increases the likelihood that the people around you will be infected. Talking about leishmaniasis as a contagious disease is possible considering the participation of the vector.
Therefore, the main prevention begins with avoiding mosquito bites, especially in people who travel to countries where the disease is common. Let’s see some good tips to avoid bites.
- Use insect repellents on exposed skin.
- Wear mosquito nets on clothing and treat clothing with medications, such as permethrin.
- Wear socks, long-sleeved shirts, pants, and tucked-in shirts to prevent mosquitoes from having access to the skin.
- Avoid outdoor activities from dusk to dawn in tropical areas, which is when mosquitoes are most active.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Weiss, Pedro. “Epidemiología y clínica de las leishmaniosis tegumentarias en el Perú.” Revista Perúana de Medicina Experimental y Salud Publica 2.3 (1943): 209-248.
- Chang, Patricia, et al. “Lip Leishmaniasis.” Dermatología Cosmética, Médica y Quirúrgica 17.1 (2019): 30-35.
- Martínez, B. Fernández, D. Gómez Barroso, and R. Cano Portero. “La leishmaniasis en España: evolución de los casos notificados a La Red Nacional de Vigilancia Epidemiológica desde 2005 a 2017 y resultados de la vigilancia de 2014 a 2017.” Boletín epidemiológico semanal 27.2 (2019): 15-27.
- Javier, Sosa Ávila Ediel, Caro Lozano Janett, and Zúñiga Carrasco Iván Renato. “Perfil epidemiológico de la leishmaniasis: una enfermedad olvidada en México.” Enfermedades infecciosas y microbiología 34.1 (2014): 31.
- Boelaert, M., et al. “The poorest of the poor: a poverty appraisal of households affected by visceral leishmaniasis in Bihar, India.” Tropical medicine & international health 14.6 (2009): 639-644.
- Matía Hernando, Belén. “Impacto de un brote de leishmaniasis en población inmunosuprimida no VIH.” (2019).
- Vera-Izaguirre, Diana S., et al. “Leishmaniasis. A review.” Dermatología Cosmética, Médica Y Quirúrgica 4.4 (2006): 252-260.
- Domínguez-Ugalde, María Guadalupe, et al. “Chronic localized cutaneous leishmaniasis.” Dermatología Revista Mexicana 63.6 (2020): 600-605.
- Tovar, Catalina, and María Yasnot. “Visceral Leishmaniasis in Latin America and therapy perspectives.” Revista MVZ Córdoba 22 (2017).
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








