How to Replace a Feeding Tube (PEG)
Written and verified by the doctor Nelton Abdon Ramos Rojas
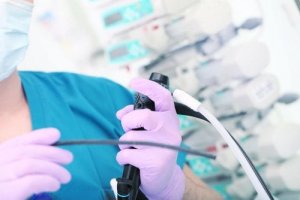
A percutaneous endoscopic gastrostomy (PEG) is a surgical procedure in which specialists place a feeding tube into the stomach. This intervention requires a non-invasive surgery that is done with endoscopy techniques.
The introduction of a tube into the stomach allows for the safe feeding of people who can’t properly carry out their digestive functions due to health problems.
Specialists commonly use this for people with dysphagia (typical of Amyotrophic lateral sclerosis). These people have difficulty swallowing the bolus (a ball-like mixture of food and saliva that forms in the mouth during the process of chewing). It’s also common in those who’ve had a stroke or some other form of neurological damage.
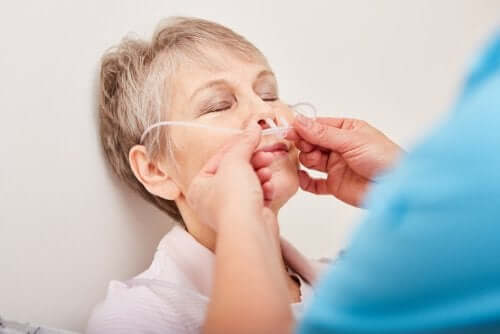
If we compare a percutaneous endoscopic gastrostomy with a nasogastric tube (the one placed from the nose to the stomach), there are many advantages to a PEG. For one, there’s a significant reduction of possible complications, in terms of infections or injuries associated with the pharynx due to breakages in the tube.
In addition, personal safety increases when we avoid most of the digestive tract. It also improves the psychological wellbeing of a patient, since a PEG is a lot more discreet. This is especially true in the case of young patients who are usually concerned about the aesthetic limitations of a nasogastric tube.
Changing a feeding tube
The feeding tube has huge advantages for the patient, both medically and aesthetically, in comparison to the alternative nasogastric tube. Let’s take a look at how it’s fitted.
How do they place it?
As we previously mentioned, this procedure is very simple. Below, we tell you how specialists fit the PEG, step by step, according to data supplied by the American Society of Gastrointestinal Endoscopy.
First, the doctor gives an intravenous solution to the patient in the endoscopy room to sedate them. Then, the doctor locates an appropriate region in the abdomen based on the results of the endoscopy, which is a way of looking inside the body, as explained by the United States’ National Library of Medicine. The doctor then carefully disinfects the area.
Next, the doctor locally anesthetizes the area and makes an incision to the abdominal wall. This is a small cut, about 1/2 an inch. Therefore, recovery is quick and there’s little risk of side effects.
Then, doctors insert an angiocath into the stomach with an endoscope wire as a guide. An angiocath is a kind of hollow needle capable of penetrating the stomach and reaching the inside of the organ.
Finally, they remove the endoscope by dragging the wire to the patient’s mouth. There, they place the tube that will come out through the abdominal incision. For added safety, manufacturers include an inflatable balloon to keep the probe from moving. So, they can easily fasten and cover it.
You may be interested in: Dangerous Diets and Their Warning Signs
When to replace a feeding tube
Percutaneous endoscopic gastrostomy is a fairly safe procedure. However, there may be complications that require its removal in patients who need prolonged enteral nutrition.
The most frequent complication of this procedure is an infection, although bleeding may also occur, as the Enciclopedia Médica MedlinePlus note.
The infection could come from the gastrostomy hole in the abdominal wall or from the tube of the probe itself. In these cases, it’s mandatory to remove it and start taking antibiotics to eliminate the infection. Otherwise, there’s a risk of septic shock.
Discover more: Acute Coronary Syndrome (ACS)
How to Replace a Feeding Tube
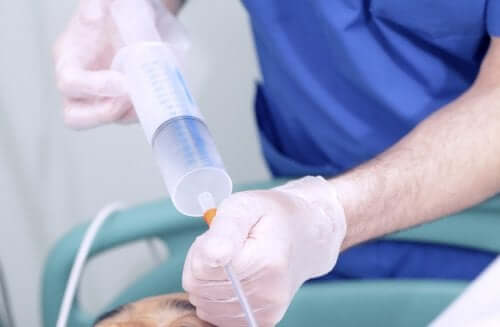
First, sterilize and disinfect the area on which you’re going to work. Then, disconnect the feeding mechanism so that the probe is clean.
Next, make sure the probe balloon is properly in place and that it works. For this, introduce sterilized water into the valve to inflate it. If it swells correctly and there are no leaks, then that means it’s functional.
Then, carefully clean the area around the hole in the patient’s stomach tube and make sure to deflate the balloon that holds the gastrostomy. As soon as the probe is no longer working and you’ve unattached it, you can remove it by pulling it firmly with one hand as you hold down the abdomen with the other.
Now, introduce the new probe through the same gastrostomy hole. Ideally, the tube will form a right angle to the abdomen to make it easier to place.
Finally, inflate the balloon until the new probe is in place and carefully pull it until it stops against the gastric wall. Always disinfect at the end of this process to prevent future infections in the new probe.
A force majeure decision
In conclusion, PEGs are used in force majeure cases when the patient can’t feed themselves for whatever reason. Often, this is due to a stroke.
Although it’s a simple procedure to fit a PEG, it still involves an operation and, as such, complications can arise. Of course, a doctor must evaluate whether it’s necessary to fit it or not, depending on the specific details of the case.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- American Society ofGastrointestinal Endoscopy. Cómo Comprender la Gastrostomía Endoscópica Percutánea. https://www.asge.org/home/for-patients/patient-information/c%C3%B3mo-comprender-la-gastrostom%C3%ADa-endosc%C3%B3pica-percut%C3%A1nea
- MedlinePlus. Endoscopia. https://medlineplus.gov/spanish/ency/article/003338.htm
- Nutrición Hospitalaria versión On-line ISSN 1699-5198versión impresa ISSN 0212-1611. Nutr. Hosp. vol.18 no.1 Madrid ene./feb. 2003. Nutrición enteral domiciliaria (NED): Registro Nacional del año 2000. http://scielo.isciii.es/scielo.php?script=sci_arttext&pid=S0212-16112003000100005
- MedlinePlus. Inserción de sonda de alimentación por gastrostomía. https://medlineplus.gov/spanish/ency/article/002937.htm
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








