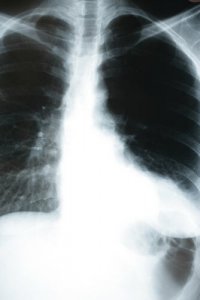
How Pneumonia Affects the Body

Written and verified by the doctor Leonardo Biolatto
There are an estimated 2 to 10 cases of pneumonia per 1,000 inhabitants per year. Of those cases, between 20 and 35% require hospitalization. In patients with other illnesses, mortality is 1%, but it can increase to 40% in hospitalized patients, especially those in intensive care. Depending on a patient’s situation, pneumonia can be fatal.
In this article, we’ll explain the process your body goes through from the moment of infection up until illness occurs. In doing so, we’ll reveal how pneumonia affects the body.
How pneumonia affects the body
Pneumonia is the consequence of two separate conditions that occur simultaneously:
- The arrival of microorganisms in the alveoli and their subsequent proliferation.
- An inflammatory response from the host, which will condition the clinical manifestations and seriousness of the illness.
How do these microorganisms reach the lungs?
Bacteria, viruses, fungi, and parasites are all capable of causing pneumonia, but bacteria and viruses are usually to blame. Currently, experts are identifying more and more viruses and the causal agents of pneumonia. There are two types of pneumonia that can occur:
- Pneumonia resulting from a viral infection: This is called primary pneumonia. For example, pneumonia associated with SARS-COV-2 (COVID-19) falls into this category.
- Bacterial pneumonia following a viral infection of the respiratory tract. For example, bacterial pneumonia is a common complication of the flu.

You may also want to read: Coronavirus Treatments Currently in Use
Our airways are constantly exposed to microorganisms. Bacterias, viruses, and other microorganisms can form colonies in our lungs in the following ways:
1. Breathing in microorganisms in the throat
Our respiratory and digestive apparatuses are intimately connected thanks to the pharynx. The pharynx connects the nose and the mouth to the larynx (respiratory apparatus) and the esophagus (digestive apparatus).
The foods that we eat, after passing through the pharynx, should only enter the esophagus. At the same time, only air can enter the larynx. Therefore, we possess a structure known as the epiglottis that closes the larynx and directs food towards the esophagus.
All people have bacterias and sometimes even viruses in our nasal or oral cavities that don’t normally cause damage. However, the larynx, the trachea, the bronchial tubes, and the lungs must remain sterile. In other words, they should not contain any microorganisms because this can lead to an infection. Therefore, as we have explained, only air must enter the larynx.
While we are sleeping, the muscles of the throat and the epiglottis relax, which can allow for microaspirations. This refers to the passing of small contents of saliva, food, etc. from the pharynx to the larynx. These microaspirations can contain microorganisms that, after passing through the larynx, reach the lungs. This is the mechanism that occurs in the great majority of individuals that develop pneumonia as well as healthy people with no illness.
At the same time, some people don’t have adequate control over their epiglottis. This causes them to have massive aspirations of foods, drinks, or saliva towards their larynx. As a result, colonization occurs in their lungs.
You may also want to read: Learn All about Swallowing Disorders
2. Inhalation dissemination
People regularly inhale small amounts of microorganisms from the air, which can make their way to our airways. These microorganisms can come tom an infected person who coughs or sneezes without protection, contaminating those in the area.
3. Hematogenous dissemination
This mechanism of infection normally occurs in people with a compromised immune system, also known as immunosuppressed individuals. In other words, their body doesn’t have a strong defense mechanism to fight against infections.
These people may, for example, have bacteria circulating in their blood. Then, these bacteria may pass to their airways, later affecting their lungs. Overall, hematogenous dissemination involves the passing of microorganisms from the blood to the lungs. Fortunately, this type of contagion is very uncommon.
4. As the result of an infection in the pleura or the mediastinum
The lungs are surrounded by a layer known as the pleura. This membrane can become infected and, consequently, the infection can spread to the lungs. What’s more, between the lungs we find different structures that make up the mediastinum, where we find, for example, the lung.
Sometimes this zone can also suffer from infections that can spread to the lungs.
5. Hospital-acquired pneumonia
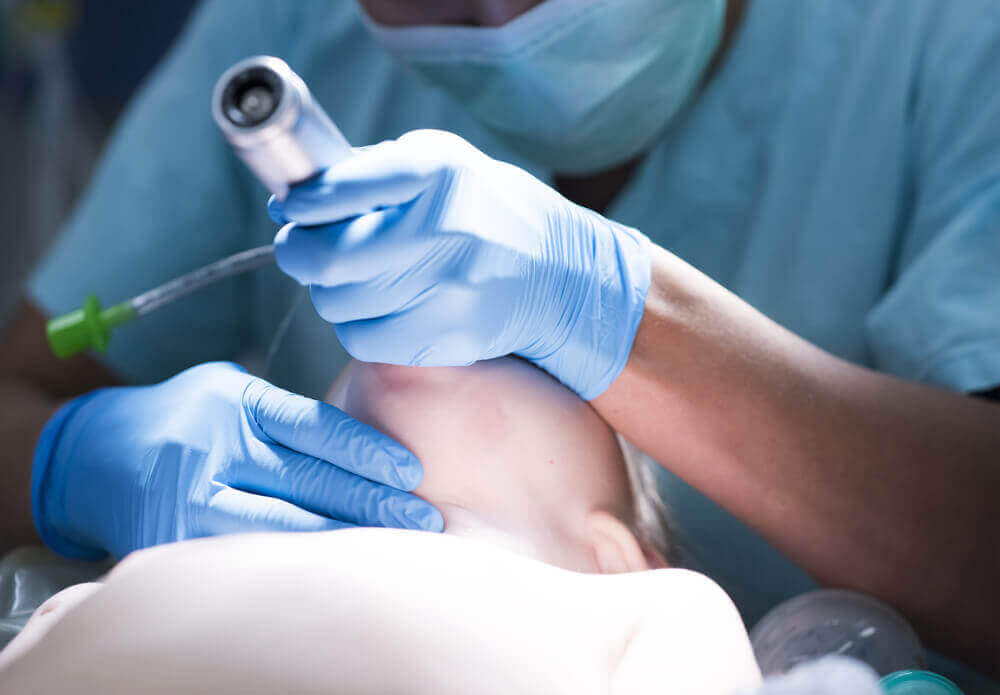
In the hospital, people who are admitted due to other illnesses can end up catching pneumonia. The most common mechanism of contagion of this type of pneumonia has to do with ventilators. In other words, it occurs in intubated patients or those with respirators.
Intubation consists of passing a tube directly from the exterior of the larynx. This prevents the epiglottis from doing its job to keep the airways free of microorganisms. Pathogens from the exterior then find it easier to enter the lungs and cause infection.
Therefore, intubation should only take place in special situations where the life of a patient is at risk and he or she is unable to breathe by any other means.
Defense mechanisms
Normally, if these microorganisms enter the lungs, they are easily eliminated by our body’s defense mechanisms, which include:
- The cough reflex, which helps to expel mucous and foreign substances.
- The cilia of the cells that cover the pulmonary airways, which prevent microorganisms from invading the lungs. These cilia are small mobile filaments that push mucous and foreign substances upwards to be expelled through sneezing.
- The cells of the lungs produce substances that attack microorganisms and destroy them.
- In the lungs, there are cells from the body’s defense system. These cells are there naturally and protect the alveoli. They are called alveolar macrophages and their function is to “eat” microorganisms and kill them.
When these defense mechanisms fail, then either the microorganism is very potent or the person inhaled a large quantity of the microorganism. As a result, pneumonia develops.
How does the body respond?
If the primary defense mechanisms have been unable of expelling the microorganism, our bodies process an inflammatory response. This inflammatory response is caused by the release of substances by the alveolar macrophages:
- Substances that produce fever. The body produces this response because higher temperatures can cause the deactivation of microorganisms and destroy them more easily.
- Substances that attract other defense cells, like neutrophils. At the same time, neutrophils produce purulent secretions. These can cover the alveoli and keep them from performing the gas exchange. This produces a sensation of suffocation because oxygen doesn’t reach the blood.
To understand this better, we’ll use the following analogy. The alveolar macrophages are soldiers on the frontlines of the battle. However, if they realize that they’re losing, they call for reinforcements to help them overcome the enemy. These reinforcements will be the rest of the defense cells.
However, the reinforcements that the macrophages attract can lead to clinical manifestations that are harmful to the host. Therefore, to stop the body from producing this defense response, the patient must receive proper treatment to eliminate the microorganism.
Conclusion: How pneumonia affects the body
In conclusion, we need to understand that the clinical manifestations of pneumonia are not caused by the pathogen agent itself. Rather, they are the result of a person’s inflammatory response.
Therefore, people with a stronger immune system will have more symptoms that a person with a compromised immune system.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Pérez-Deago, B., Alonso-Porcel, C., Elvira-Menendez, C., Murcia-Olagüenaga, A., & Martínez-Ibán, M. (2018). Epidemiology and management of community acquired pneumonia: more than 10 years experience. Semergen, 44(6), 389–394. https://doi.org/10.1016/j.semerg.2018.01.008
- Neumonía: Síntomas, diagnóstico y tratamiento. Clínica Universidad de Navarra. (n.d.). Retrieved April 8, 2020, from https://www.cun.es/enfermedades-tratamientos/enfermedades/neumonia
- Generalidades sobre la neumonía – Trastornos pulmonares – Manual MSD versión para profesionales. (n.d.). Retrieved April 10, 2020, from https://www.msdmanuals.com/es/professional/trastornos-pulmonares/neumonía/generalidades-sobre-la-neumonía
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








