Diagnosis and Treatment of Uveitis

Written and verified by the biologist Samuel Antonio Sánchez Amador
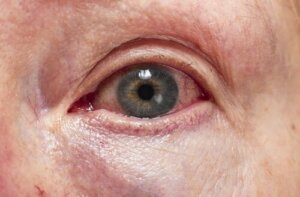
Uveitis is a pathology characterized by inflammation of the uvea — the intermediate layer of ocular tissue located between the sclera and the retina. According to the Mayo Clinic, this disease manifests as redness, blurry vision, and pain. Also, it tends to worsen rather quickly.
Some medical studies reveal that the chronic form of this disorder leads to complications such as glaucoma and retinal detachment. Therefore, it’s a good idea to be familiar with the signs, diagnosis, and treatment.
What’s uveitis?
Uveitis is a form of eye inflammation. The uvea is the intermediate lamina cribrosa of the human eye and highly irrigated with blood capillaries. In fact, it’s precisely through these channels that the immune cells that provoke the undesirable inflammatory response can enter.
The Portal Clínic Barcelona medical page provides some interesting data regarding the distribution of uveitis. Some of them are:
- This eye disorder is considered a rare disease by the World Health Organization (WHO).
- Uveitis is the main cause of blindness in the active working-age group together with diabetes mellitus. Therefore, it translates into a high socio-economic impact.
- 10% of all cases of blindness in the USA are caused by uveitis. In fact, estimates indicate that 47,000 people are affected by this disease in some countries.
All these figures reveal it’s a much more widespread disorder than one would think in the first place. In addition, the aforementioned portal points out there are different types of uveitis depending on the affected area.
For example:
- Iritis. This condition affects the front of the eye and manifests as redness, pain, and photophobia (light sensitivity).
- Intermediate uveitis. In this one the gelatinous substance that gives the structure to the eye and that fills the vitreous cavity (vitreous humor) becomes inflamed. Thus, clusters of “snowballs” form in this substance — clusters of floating inflammatory cells, that is.
- Posterior uveitis. This one is an inflammation of the retina or choroids.
- Panuveitis. This condition happens when the disease manifests in both the front and back of the eye.
We’ve described the incidence of this disease in the general population and the possible subtypes. Now it’s time to dive into the diagnosis and treatment of this pathology.
Check out these Natural Remedies for Dry Eyes
Diagnosis and treatment of uveitis
We must be familiar with the causes of uveitis in order to address the disease. The National Eye Institute (NIH) indicates the possible reasons that drive the appearance of uveitis. Some of them are:
- Self-attacks by the body’s own immune system (autoimmune disorders)
- Infectious processes within the eye
- Tumors associated with the ocular apparatus
- Eye damage and injuries
- The entry of toxic substances into the eye
- Certain diseases, such as HIV, toxoplasmosis, tuberculosis, and many others
Diagnosis
The diagnosis of uveitis requires a detailed medical history of the patient. This is because there may be multiple causes that have little to nothing to do with each other. An eye examination is usually the first step, as the pathology is linked to loss of vision.
Therefore, the eye doctor may suggest various tests such as:
- Visual acuity
- Funduscopic examination [of the back of the eye]
- Measurement of eye pressure
- Eye inspection using a slit lamp
Unfortunately, tests aimed at evaluating the central nervous system in people with intermediate uveitis may be necessary. Why? Because several studies already identified it as a symptom of multiple sclerosis in its early stages.
The Mayo Clinic also states that a blood test can facilitate the diagnosis of this disease. In fact, there can be various complications when detected. However, the first step must always be to differentiate whether it’s an infectious or non-infectious cause.
Treatment
The treatment of uveitis is based on eliminating the inflammation of the uvea, relieving local pain, and preventing further tissue damage. Still, the cause will determine the drug of choice. This is because a bacterial infection in the eye has nothing to do with an autoimmune disorder. Thus, there are three groups of drugs generally used for this purpose:
- Anti-inflammatory drugs are prescription steroidal drugs usually in the form of eye drops
- Antibiotics or antivirals focus on fighting and eliminating the viral or bacterial source of infection that causes pain
- Immune system modulators are immunosuppressive drugs that target specific elements of a patient’s immune system

You might like to know these Five Effective Remedies for Eye Infections
Things to keep in mind about uveitis
As you can see, uveitis is an ocular disorder characterized by an inflammatory process with multiple causes. One can explain this pathology by infectious processes such as bacterial colonization in the eye, and neurodegenerative diseases as complex as multiple sclerosis, among others.
It’s for this reason that the diagnosis and treatment of this disease can be complex. In any case, consult your doctor if your eye pain doesn’t go away.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Uveítis, mayoclinic.org. Recogido a 23 de agosto en https://www.mayoclinic.org/es-es/diseases-conditions/uveitis/symptoms-causes/syc-20378734
- SALMEN, Siham, BERRUETA, Lisbeth, SANCHEZ, Nelly et al. Nongranulomatous Anterior Uveitis Associated with Alendronate Therapy. Invest. clín. [online]. mar. 2002, vol.43, no.1, p.49-52.
- Uveítis, Clínica Barcelona.org. Recogido a 23 de agosto en https://www.clinicbarcelona.org/asistencia/enfermedades/uveitis/definicion#:~:text=La%20uve%C3%ADtis%20est%C3%A1%20considerada%20por,prevenible%20en%20el%20mundo%20desarrollado.
- Uveítis, National Eye Institute. Recogido a 23 de agosto en https://www.nei.nih.gov/learn-about-eye-health/eye-conditions-and-diseases/uveitis
- Díaz-Valle, D., Méndez, R., Arriola, P., Cuiña, R., & Ariño, M. (2008). Enfermedades sistémicas no infecciosas y uveítis Non-infectious systemic diseases and uveitis. An. Sist. Sanit. Navar, 31(Suplemento 3).
- Uveítis, Mayoclinic.org. Recogido a 23 de agosto en https://www.mayoclinic.org/es-es/diseases-conditions/uveitis/diagnosis-treatment/drc-20378739
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








