7 Common Causes of Itchy Testicles

Written and verified by the doctor Maryel Alvarado Nieto
In today’s article, we’ll take a look at some of the most common causes of itchy testicles. Many times, a man feels embarrassed to seek medical help for this condition, delaying a possible solution.
The clinical term used to describe the itching sensation in a certain part of the body is localized pruritus. The genitals are one of those regions where the symptom causes great discomfort and concern.
Bearing this in mind, let’s take a closer look at some of the possible causes of itchy testicles.
1. Problems with intimate hygiene and lifestyle
Whether by defect or excess, one of the main reasons for itching of the testicles is body hygiene. The presence of sweat and secretions in the genital area triggers maceration processes that allow microorganisms to grow. Thus, bad odor, and irritation appear.
Similarly, vigorous and repetitive intimate hygiene causes dryness and itching. Therefore, the best option is to have proper hygiene in a timely manner.
Underwear and itchy testicles
On the other hand, because it’s usually covered, the genital area is an area prone to humidity and heat. If, in addition to this vulnerability, synthetic fibers and tight underwear are chosen, the situation is aggravated.
These types of materials don’t allow for perspiration and lead to the accumulation of sweat since it can’t be eliminated through evaporation. Also, the local temperature with these fabrics increases. For this reason, the recommendation is to choose loose-fitting underwear made of natural fibers, such as cotton.
We think you may also enjoy reading this article: Testicular Cancer: The Disease that Borussia Dortmund’s Sebastien Haller Has
Intimate shaving can cause itchy testicles
Another common trigger of itching in the testicles is genital shaving. Shavers generate micro-injuries that trigger inflammatory processes in the irritated area, especially if the razors are worn or if they are applied dry or without prior hygiene.
The consequent release of certain proinflammatory substances is responsible for causing redness and itching in the shaved area. Similarly, the inflammatory process also acts on the hair follicles, generating folliculitis.
This condition can become superinfected with bacteria from the normal flora of the skin, aggravating the situation. For this reason, it’s recommended to cut unwanted hair instead of shaving it. If you do shave, it’s important to use razors in good condition and to wash the area well before performing the procedure.

2. Can parasites cause itching of the testicles?
The term ectoparasitosis refers to the infestation of the skin and its annexes by various organisms. In humans, the two most frequent types of parasites that can cause testicular itching are pediculosis and scabies.
In this section, we’ll focus only on lice affecting the genital region, as they can also occur in other locations. Pediculosis and scabies are contagious entities and are often associated with poor hygienic conditions.
Pediculosis pubis (pubic lice)
Pubic lice are small insects that invade the genital region in humans, although they can sometimes be found in other areas with coarse hair. The infestation is caused by Pthirus pubis and intimate contact is the real form of contagion, so sexually transmitted infections (STIs) should also be ruled out.
The bite of the insect is the trigger for itching, leaving small spots on the skin.
Like this article? You may also like to read: Why Does a Kick to The Testicles Hurt So Much?
Scabies
In the case of scabies, a mite called Sarcoptes scabiei penetrates the skin to invade it, creating tiny tunnels in its path. These can be seen on the skin surface as small, thin, curved elevations, known as acarine furrows. The lesions are very itchy, and it’s common for the patient to report that the itching is worse at night.
Although they often cover various parts of the body, scabies can sometimes present as nodules located in the genital region. The mite spreads very easily, both by direct physical contact and by surfaces where they’re found, since they’re capable of unleashing epidemics in vulnerable communities.
Therefore, in addition to treatment, hygienic measures should be reinforced if scabies is the cause of the itching.
3. Dermatitis as a cause of itchy testicles
A skin condition that’s also linked to itching is dermatitis or eczema. In this type of inflammatory skin condition, lesions appear that tend to become chronic and trigger severe itching.
Atopic dermatitis usually appears in childhood as a consequence of an alteration of the skin barrier function. The areas of involvement depend on the age of the child, but it’s quite unusual that it affects the genital area.
However, in the presence of thickened, scaly, and pruritic plaques on the scrotum and base of the penis in an atopic patient, it’s necessary to suspect this cause. This is especially the case when other conditions, such as fungi and allergic processes, have already been ruled out.
In addition, systemic disorders should also be investigated. The follow-up of these cases should be prolonged always at the hands of a specialist.
Contact dermatitis, on the other hand, can generate itching in the testicles in the presence of an irritant agent. Among the most frequent are deodorants, perfumes, spermicides, and condoms.
Previous sensitization with the triggering agent will produce an immediate reaction or after a few hours. However, in the case of first contact there may be no lesions, or they may only appear after a few days. Elimination of the causal agent is enough to prevent future episodes.
4. Mycosis
Fungal infections can also cause itching of the testicles. Candidal intertrigo appears as reddened, circular plaques that cause itching and stinging of the genitals.
The causative agent is an opportunistic fungus that is part of the normal flora, called Candida albicans. Similarly, seborrheic dermatitis is related to infection by yeasts of the genus Malassezia. In this condition, yellowish plaques are observed on the scrotum and penis.
Tinea cruris is a clinical entity in which very pruritic plaques appear in the inguinal folds, perianal region, and perineum. The lesions have raised, erythematous borders, while the center of the lesions may be lighter. The hot and humid environment favors the development of mycoses, so obesity and profuse sweating are both predisposing factors.
5. Itching of the testicles due to STIs
Some sexually transmitted infections are associated with itching, although this isn’t usually an isolated manifestation. In the case of herpes, itching precedes the appearance of the typical vesicles, which, when ruptured, take on a yellowish crusty appearance.
The location of these lesions in men is usually on the glans and foreskin. Less frequently, they are located on the scrotum and thighs.
In the case of human papillomavirus (HPV), infection is usually asymptomatic. Depending on their location, lesions may be accompanied by mild pruritus.
Human immunodeficiency virus (HIV), on the other hand, has diverse cutaneous manifestations, which usually go unnoticed because they are nonspecific. Among them, we often find pruritus.
Maintaining safe sex is the only effective measure to reduce the risk of STI transmission.
6. Itching of the testicles as a manifestation of other diseases
Itching in this area of the body may also be the manifestation of other health problems that require specialized review, especially if the symptom is maintained over time. It’s important to perform the corresponding complementary tests to rule out any other disease.
Among the main diseases that can cause testicular itching are the following:
- Diabetes mellitus
- Extramammary Paget’s disease
- Psoriasis
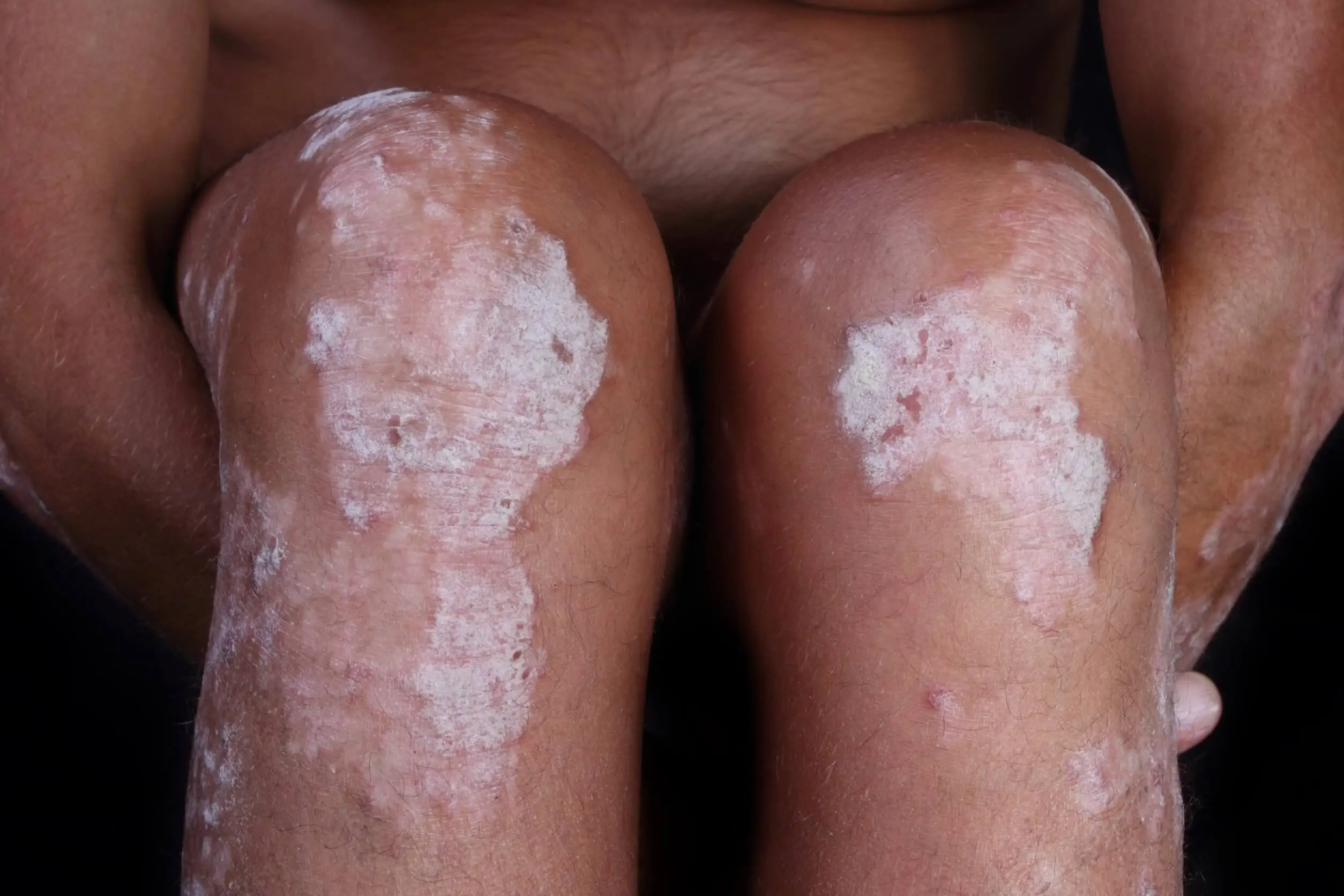
7. Red scrotum syndrome
Finally, there’s also a condition in which redness, itching, and burning appear in the scrotum, secondary to the use of topical corticosteroids in the genital area. Usually, the person reports great anxiety due to the manifestations, often fearing an infectious or malignant origin. In this case, other processes should be ruled out, the steroid should be eliminated, and the case should be closely monitored.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Jinich, H.; Lifshitz, A.; García, J.; Ramiro, M.; Síntomas y Signos Cardinales de las Enfermedades; Sexta Edición; Editorial El Manual Moderno S.A. de C.V.; 2013.
- Díaz, C.; Enfermedades Cutáneas no Infecciosas de los Genitales Masculinos; Revista de la Asociación Colombiana de Dermatología y Cirugía Dermatológica; 12 (1): 35 – 46; 2004.
- Chaine, B.; Janier, M.; Dermatosis Genitales Masculinas; EMC – Dermatología; 48 (1): E – 98-834-A-10; 2014.
- Suárez, R.; Guía Dermatológica para Atención Primaria; Primera Edición; ICG Marge S.L.; 2013.
- Cayuela, A.; Luna, C.; Gómez, M.; Prurito localizado; Atención Primaria; 52 (3): 206 – 207; 2020.
- Bonet, R.; Garrote, A.; Higiene Íntima Masculina y Femenina; Ámbito Farmacéutico Dermofarmacia; 29 (1): 59 – 63; 2010.
- Wendel, K.; Rompalo, A.; Scabies and Pediculosis Pubis: An Update of Treatment Regimens and General Review; Clinical Infectious Diseases; 35 (Issue Supplement 2): S146 – S151; 2002.
- Prieto, L.; Torredo, A.; Dermatitis Atópica y Otras Erupciones Eczematosas; Pediatría Integral; 20 (4): 216 – 226; 2016.
- Molina, A.; Aspectos Clínicos, Diagnósticos y Terapéuticos de las Dermatofitosis; Enfermedades Infecciosas y Microbiología Clínica; 29 (Suplemento 3): 33 – 39; 2011.
- Moya, L.; Fernández, M.; Aldanondo, I.; Muñoz, E.; Protocolo Diagnóstico de Infecciones Fúngicas; Protocolo de Práctica Asistencial; Medicine; 9 (47): 3101 – 3104; 2006.
- Cerantola, Y.; Vaucher, L.; Secco, M.; Tillou, X.; Doerfler, A.; Patología Inflamatoria del Escroto; EMC – Urología; 46 (1); 2014.
- Ríos, A.; Enfermedades de Transmisión Sexual; Tópicos en Urología; Capítulo 35; Editorial Ateproca; 2002.
- Potenziani, J.; Martín, M.; Virus del Papiloma Humano en el Hombre; Tópicos en Urología; Capítulo 36; Editorial Ateproca; 2002.
- Navarrete, C.; Ortega, R.; Concha, M.; Manifestaciones Dermatológicas Asociadas a la Infección por VIH/SIDA; Revista Chilena de Infectología; 32 (Suplemento 1); 2015.
- Poletti, E.; Muñoz, R.; Morales, A.; Síndrome de Enrojecimiento Genital y Corticodependencia; Dermatología Cosmética, Médica y Quirúrgica; 2011.
- González, E.; González, A.; Un Varón con Síndrome del Escroto Rojo; Más Dermatología; 29: 13 – 15; 2017.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








