Basal Insulin: Everything You Need to Know

Written and verified by the doctor Maryel Alvarado Nieto
Insulin is a hormone secreted by the pancreas, whose main function is to stimulate cells to take up glucose circulating in the bloodstream. Continuous secretion generates a concentration known as basal insulin, which maintains normal blood sugar levels during the period in between meals.
Additionally, when food is consumed, extra insulin loads are released from the pancreas to cope with the increased glucose from the diet. This produces levels of the hormone higher than basal insulin, called postprandial.
How important is basal insulin?
In some patients, insulin levels may be increased, predisposing them to the development of type 2 diabetes mellitus. This situation is known as insulin resistance.
For various reasons, the usual concentration of the hormone is not sufficient to maintain adequate blood glucose levels. Therefore, the pancreas tries to compensate for this defect by releasing even more insulin molecules.
In contrast, in patients with type 1 diabetes mellitus, the pancreas stops producing insulin, resulting in decreased levels of the hormone. In these cases, it’s necessary to implement treatments with exogenous insulin to prevent diabetes complications. It’s here that basal insulin as medication becomes important.
We think you may also enjoy reading this article: Insulin Overdose: What Are The Consequences?
The types of insulin available
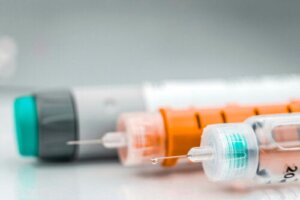
Currently, there are several insulin options available, which are classified depending on the duration of the effect they produce. Short-acting insulin, also called regular insulin, has analogs: lispro, apart, and glulisine. They prevent post-meal blood glucose peaks, resembling the effect of postprandial insulin.
Intermediate-acting (NPH) and long-acting (glargine, detemir, and degludec) types of insulin seek to maintain insulin values during fasting periods. Because of this, this group of substances is considered the basal insulin of diabetic patients. The purpose of this treatment is to allow the cells a constant input of glucose as a source of energy, but without causing hypoglycemia.
It’s important to note that there are devices designed to administer insulin continuously and automatically (insulin pumps). These devices are small in size and use rapid-acting insulin. However, since they provide constant concentrations throughout the day and night, they’re often considered part of basal insulin.
Basal insulin characteristics
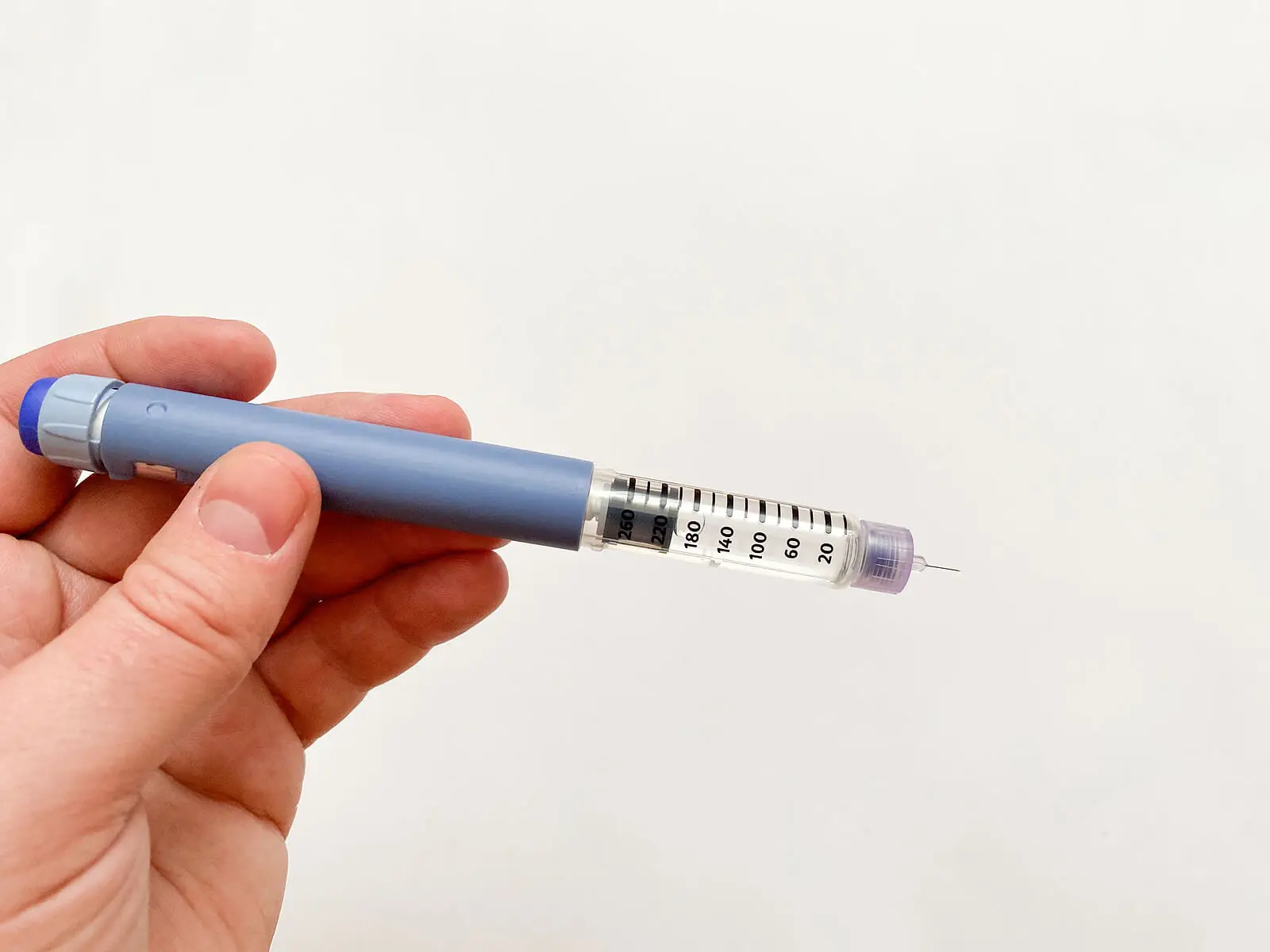
As a long-acting drug, basal insulin is usually prescribed once or twice daily. The choice of administration schedule depends on the characteristics of each type of insulin and the intrinsic factors of each patient.
Therefore, insulin therapy and adjustments should always be performed by a specialist physician. Better, with a professional who has experience in the management of diabetes mellitus.
NPH (neutral protamine Hagedorn): The intermediate-acting insulin
NPH insulin is an off-white suspension containing zinc and protamine. The latter molecule slows the absorption of insulin, prolonging its effect.
The duration of action can be extended up to 16 hours, which is why it’s usually prescribed twice a day. However, nocturnal administration has not shown good blood glucose values the following morning.
Long-acting human insulin analogues
Human insulin analogues have modifications in some amino acids of the hormone, which produce a prolonged effect. In general, they don’t have a peak action, thus reducing the risk of hypoglycemia.
The most relevant characteristics are described below:
- Insulin glargine is dissolved in an acidic medium, giving it a crystalline appearance, like that of regular insulin. Subcutaneous administration provides an adequate basal insulin concentration, so it can be indicated only once a day. It should never be mixed with other types of insulin.
- Detemir is a type of insulin that has a fatty acid in one of its chains. This molecule binds to blood proteins when absorbed, prolonging its action. It has the advantage of producing less hypoglycemia than glargine. It should generally be administered twice a day.
- Insulin degludec, on the other hand, creates large molecules that slowly break apart when injected into the subcutaneous tissue, producing a prolonged effect. In addition, it also binds to albumin, delaying its effect. It can only be administered once a day.
Insulin treatment therapy: What you should know
Generally speaking, about 50% of the daily insulin dose in a patient with type 1 diabetes should be administered as basal insulin, while the other 50% should be covered by meals. However, some factors should be taken into consideration. The main objective is to maintain adequate blood glucose levels.
Similarly, the calculation of the daily dose advised by the American Diabetes Association (ADA) ranges from 0.4 to 1 international unit (IU) per kilogram of the patient’s weight. The choice of the dose is also individualized, since it depends on age and the presence of any associated condition.
In those patients with type 2 diabetes mellitus who are indicated for insulin therapy, the ADA advises that the hormone requirements be covered with basal insulin associated with an oral hypoglycemic agent. In these individuals, the dose is estimated to be between 0.1 and 0.2 IU per kilogram of weight per day.
Important factors to consider with basal insulin
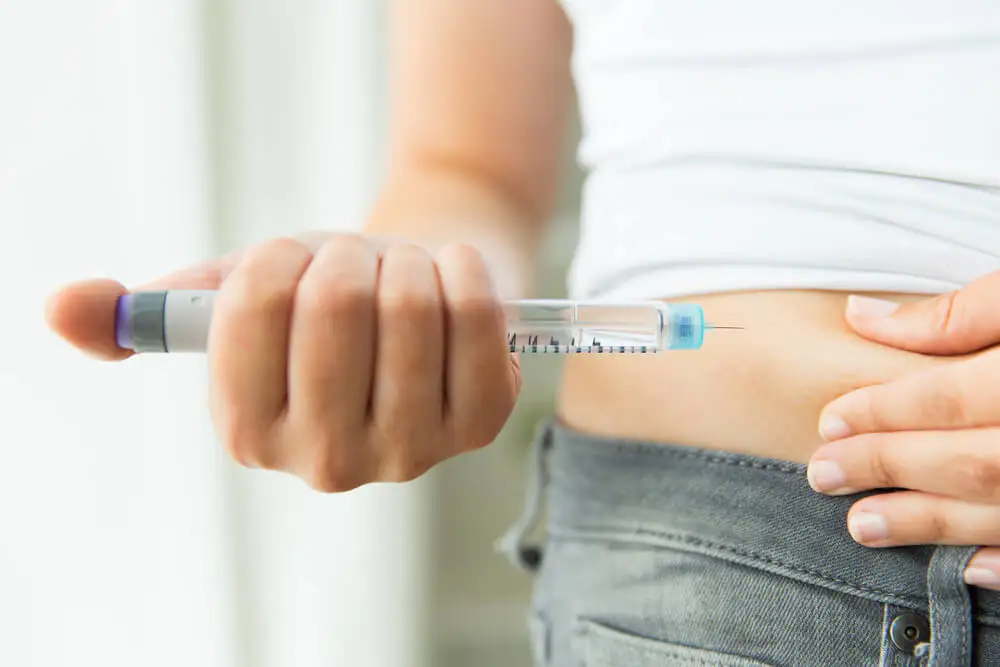
The route of administration of insulin is subcutaneous, requiring multiple injections during treatment. The preferred site is the adipose tissue of the abdomen, but the thighs, buttocks, and arms are also suitable.
It’s important to change the location frequently to avoid the development of lipohypertrophy. Likewise, special insulin needles, which are short, should be used in order to prevent intramuscular administration.
On the other hand, improvements in the patient’s lifestyle should be encouraged. Incorporating a balanced diet with adequate nutritional advice and regular exercise has been shown to have a positive effect on glycemic control.
Like this article? You may also like to read: Does Turmeric Help Prevent Diabetes? This is What Science Says
What is the follow-up of insulin therapy like?
Diabetic patients should be educated about their condition so that they’re able to actively participate in their treatment. Capillary blood glucose monitoring is an indispensable resource since it allows close, real-time monitoring of the effect of insulin on the patient.
Likewise, regular detection of glycosylated hemoglobin serves to evaluate the effectiveness of insulin treatment in the medium term. Today, it’s an essential method for deciding whether to maintain or modify the insulin treatment regimen.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Diabetes Care ® The Journal of Clinical and Applied Research and Education; Standards of Medical Care in Diabetes – 2022; American Diabetes Association; 45 (Supplement 1); 2022.
- Brunton, L.; Hilal, R.; Knollmann, B.; Powers, A.; D’Alessio, D.; Goodman & Gilman Las Bases Farmacológicas de la Terapéutica; Capítulo 47; Decimotercera Edición; McGraw Hill; 2018.
- Katzung, B.; Vanderah, T.; Masharani, U.; Kroon, L.; Farmacología Básica y Clínica; Capítulo 41; Decimoquinta Edición; 2022.
- Domarus, A.; Farreras, P.; Rozman, C.; Cardelach, F.; Nicolás, J; Cervera, R.; Farreras Rozman. Medicina Interna; 19na Edición; Elsevier; 2020.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








