Acute Pancreatitis: Symptoms, Causes, and Treatments

Reviewed and approved by the doctor Leonardo Biolatto
Acute pancreatitis is a sudden inflammation of the pancreas. Typically, after the episode is over, the function of this gland comes back completely. These types of episodes occur more frequently among people 50 to 70 years old.
Anyone in good health can suffer an episode of acute pancreatitis. However, the most common situation it happens to those who have some health condition that predisposes them to suffer from this condition. Mainly, the most common risk factor is having gallstones (mineral deposits in the gallbladder). Another factor that can cause acute pancreatitis is alcohol consumption when ingested in large quantities or very regularly. Bad nutritional habits can also lead to the onset of this condition.
You might like: Cleanse Your Pancreas with These 5 Natural Remedies
What is acute pancreatitis?
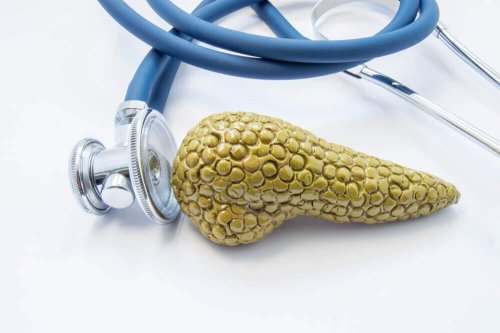
Pancreatitis is inflammation of the pancreas. The pancreas is a gland located in the upper abdomen, behind the stomach. It produces enzymes, which contribute to the digestive process, and hormones, which help to regulate the processing of sugar or glucose.
There are two types of pancreatitis:
- Acute pancreatitis appears suddenly and lasts only for a few days.
- Chronic pancreatitis can last for more than six months.
Acute pancreatitis can be serious, moderate, or mild. This classification depends on the effects it has on other body functions and the complications that it entails. Generally speaking, when pancreatitis is mild or moderate, it usually has no fatal consequences. However, if it’s serious, the risk of death higher.
Causes
The main causes of acute pancreatitis are the following:
- Gallstones: This condition makes up approximately 40% of cases. Although it’s not completely clear how this happens, the stones supposedly obstruct the pancreatic duct causing activation of the enzymatic process within the pancreas. This leads to the destruction of organ tissue.
- Alcohol consumption: This constitutes about 30% of cases. Systematic alcohol consumption, even if the intake is moderate, leads to chronic pancreatitis after a few years. It does not occur in all drinkers. Instead, other concurrent health conditions factor into the onset.
- Other factors: A genetic mutation was detected in the cationic trypsinogen gene that causes acute pancreatitis in 80% of the carriers. It is also a complication that appears in 5-10% of cases of those who receive an endoscopic retrograde cholangiopancreatography (ERCP) procedure.
You might like: 7 Foods to Fight Liver and Pancreas Inflammation
Symptoms of acute pancreatitis
The typical symptom of acute pancreatitis is severe pain in the abdomen. It’s present in more than 95% of cases. It has an intensity that ranges from moderate to severe, and the feeling resembles a dagger that goes through the back. The only way to slightly relieve this pain is by staying still. This pain appears suddenly and all at once.
Nausea and vomiting also appear in 80 or 90% of those who have an episode of this nature. At first, they may regurgitate food, and then bile or water. It’s also common to experience abdominal strain and fever.
In some cases, other symptoms appear that include respiratory or renal failure, heart failure, low blood pressure, and mental disorders. In the case of mild pancreatitis, the pain is much less intense and the other symptoms may go unnoticed.
Treatment
Typically, these types of episodes are treated in a hospital. First, the patient must fast for at least one to two days. When the inflammation subsides, a liquid diet begins and then a soft foods diet. Pain medications and intravenous fluids are also given to prevent dehydration.
After initial treatment, the patient will follow another specific treatment depending on the causes of their pancreatitis. This may include procedures for unblocking the bile ducts, gallbladder surgery, pancreas surgery or alcoholism treatment.
It’s important that after the patient recovers from the episode, they begin to follow a strict low-fact and high-liquid diet. Likewise, it’s crucial to stop drinking alcohol and avoid using tobacco.
The prognosis depends on the severity of the episode. The outlook is less optimistic if the patient is over 60 years old, has other health problems, is obese, has symptoms of hypovolemia (blood loss), systemic inflammatory response syndrome (SRIS), or pleural effusion, or shows signs of changes in his or her mental state.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Sánchez, A. C., & Aranda, J. A. G. (2012). Pancreatitis aguda. Boletín médico del Hospital Infantil de México, 69(1), 3-10.
- Salvador Moreno, E., & Ramírez Paesano, C. (2016). Pancreatitis aguda. DOLOR. https://doi.org/10.1016/j.med.2016.03.018
- Carneiro, M. C., Antônio, V. E., Siqueira-Batista, R., De Albuquerque, A. K. A. C., Gomes, A. P., Santos, S. S., & Nacif, M. S. (2008). Pancreatite aguda. Revista Brasileira de Medicina. https://doi.org/10.11606/issn.1679-9836.v49i2p93-119
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.