What Is Diabetic Gastroparesis and How Is it Treated?

Written and verified by the doctor Mariel Mendoza
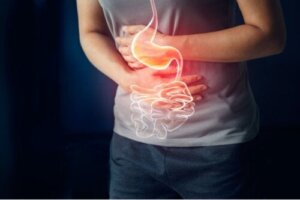
Diabetic gastroparesis is a syndrome characterized by a delay in gastric emptying in the absence of any mechanical obstruction of the stomach. It can be asymptomatic up to 50% of the time. However, the most frequent symptoms, when present, are early satiety (postprandial fullness), nausea, and vomiting.
The main cause of gastroparesis is diabetes mellitus. Because its symptomatology can be nonspecific, it tends to be a diagnosis of exclusion.
Diabetes and nerve involvement
In diabetes mellitus, nerve involvement occurs in up to 50% of patients. This condition is known as “diabetic neuropathy”.
Although the most common diabetic neuropathy is distal symmetric polyneuropathy, which affects the motor and sensory nerves in the hands and feet, there are also dysautonomias. The latter occur due to involvement of the autonomic nervous system. The symptoms, then, are cardiac, gastrointestinal, and genitourinary.
Find out more about: Essential Oils for Neuropathy in Diabetic Patients
Diabetic gastroparesis as neuropathy
Although gastroparesis, defined as a paralysis of the stomach muscles, is not exclusive to diabetes mellitus, this is its most frequent cause. The first to describe it was Kassander in 1958. He used the term gastroparesis diabeticorum to describe the process of atony and loss of gastric emptying in some diabetic patients.
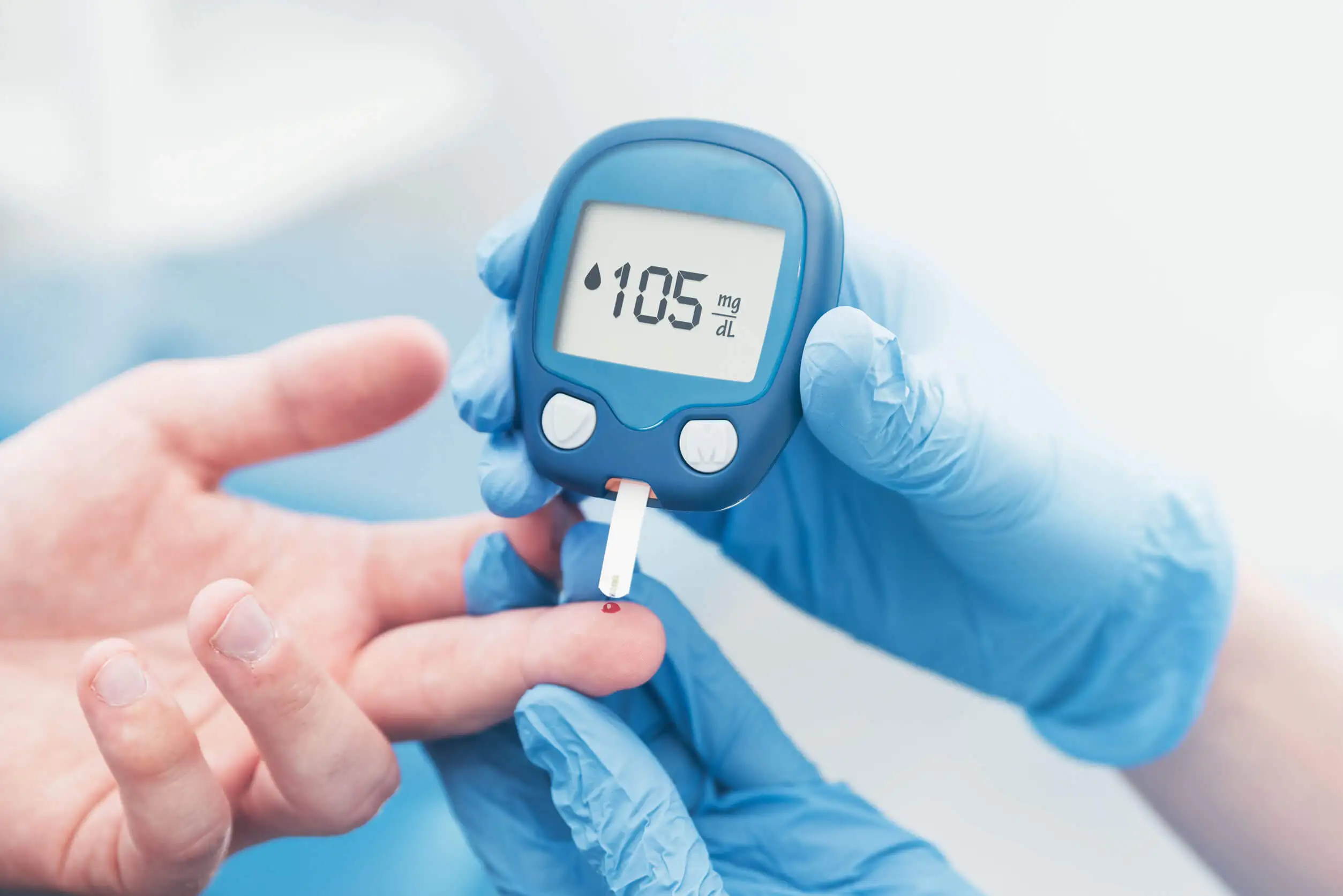
Its prevalence among people with diabetes isn’t well defined and is estimated to be between 10% and 76% of patients. However, although it usually occurs after suffering from the disease for a long time, it’s more associated with poor glycemic control.
Causes
In diabetic gastroparesis, as in other neuropathies, the causes are multifactorial. They are based on the nervous and vascular alteration produced by sustained hyperglycemia, in conjunction with the decrease in insulin concentration.
These alterations produce changes in the motor activity of the stomach, resulting in the following:
- Problems in the adaptive relaxation of the stomach to receive the alimentary bolus.
- Decreased or increased frequency of intrinsic electrical activity of the stomach.
- Decreased contraction of the antrum of the stomach, with difficulty in crushing large food particles.
- Increased pyloric sphincter tone, which slows the emptying of gastric contents into the duodenum.
- Atrophy or fibrosis of the smooth muscle of the organ.
The alteration is considered an autonomic neuropathy, because it leads to the involvement of the vagus nerve (the main effector of the parasympathetic nervous system) and increased activity of the sympathetic system. The result is gastric dysrhythmias.
Find out more: How Diabetes Affects The Digestive System
Symptoms of diabetic gastroparesis
Due to the paralysis of the stomach muscles, in diabetic gastroparesis there’s delayed gastric emptying. It manifests with the following:
- Nausea and vomiting
- Loss of appetite
- Postprandial fullness
- Abdominal distension
- Abdominal pain in the epigastrium
These symptoms are non-specific and are shared with other intestinal pathologies, such as ulcer disease, gastric obstruction, stomach cancer, and functional dyspepsia.
In addition, delayed gastric emptying leads to alterations in post-meal blood glucose. Thus, poor blood sugar control is further aggravated.
The complications identified are as follows:
- Weight loss
- Poor glycemic control
- Hydroelectrolyte disorders
- Decreased absorption of some medications
- Increased risk of bronchoaspiration in procedures requiring anesthesia
How is it diagnosed?
The American Gastroenterological Association recommends, when diabetic gastroparesis is suspected, performing an initial evaluation with questions and a physical examination. Then, a complete blood count, glycosylated hemoglobin, and metabolic profile are requested to evaluate glycemic control.
Amylasemia is also requested.
To continue to rule out mechanical obstruction or other gastrointestinal diseases, a serial upper gastrointestinal radiologic study with barium and ultrasound is performed in case of biliary symptoms or associated abdominal pain. Upper GI endoscopy is used to rule out mucosal lesions.
The ideal diagnostic standard is scintigraphy, in which radioisotope-labeled food is ingested to determine gastric emptying at 15-minute intervals for 4 hours. When more than 10% of food is retained at the end of 4 hours, this is considered indicative of gastroparesis.
Treatment
After excluding other causes, gastroparesis is treated by assessing severity and correcting complications. The goal of the approach is to optimize glycemic control and maintain adequate nutritional status.
Consumption of homogenized food and nutritional supplements is usually necessary in cases of severe gastroparesis. In patients with mild and moderate manifestations, prokinetics and antiemetics are indicated. These include cisapride, domperidone, ondansetron, and metoclopramide.
Medications that exacerbate gastric motility disorder, such as antacids, calcium channel blockers, histamine receptor antagonists, proton pump inhibitors, opioid analgesics, beta-adrenergic receptor agonists, diphenhydramine, sucralfate and tricyclic antidepressants, should be eliminated.
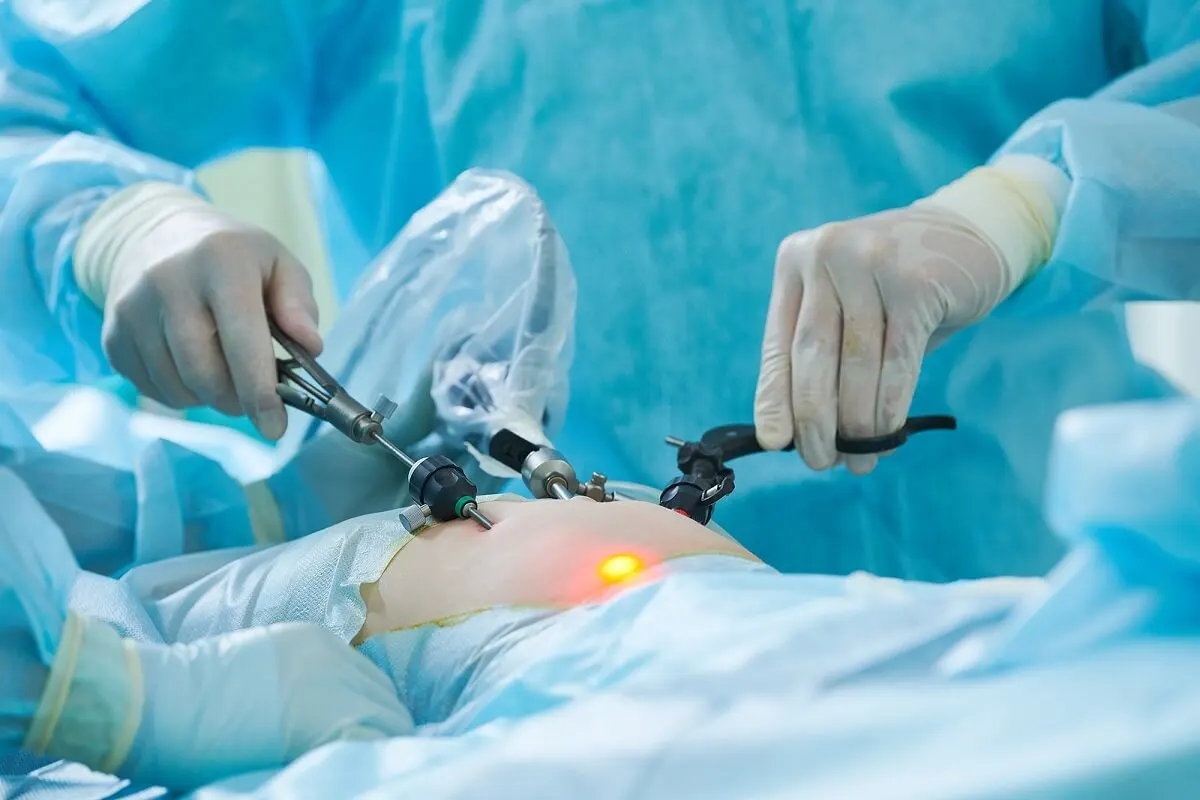
In cases of severe, drug-resistant gastroparesis, gastric electrical stimulation can be attempted (electrodes are implanted in the gastric muscular layer by laparotomy or laparoscopy). Or proceed to surgery with resection of part of the stomach.
A problem without specific treatment
For mild cases of diabetic gastroparesis, diet modification and low doses of antiemetics or prokinetics are recommended. As there is a slowing in the movement of food, the ideal thing is to have 6 small meals throughout the day instead of 3 large meals.
Foods with high fat content shouldn’t be consumed, because this nutrient further delays gastric emptying. The same happens with foods high in insoluble fiber, because they hinder digestion.
Undigested food ferments in the stomach and leads to bacterial proliferation. On the other hand, it can also harden and form a mass called bezoar, which can cause gastric obstruction. A balanced and adequate diet is essential in the treatment of diabetes and its complications.
Diabetic gastroparesis is a rare diagnosis that negatively impacts the lives of those who suffer from it. This is why it should be suspected for a timely diagnostic and therapeutic approach.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Barney C, Parra J, Meza L. Gastroparesia diabética: revisión corta con viñeta clínica ilustraiva. Actualización y puntos más relevantes para la práctica clínica. Revista Colombiana de Endocrinología, Diabetes y Metabolismo 2020;7(4). Disponible enhttps://revistaendocrino.org/index.php/rcedm/article/view/653/843
- Carpio-Deheza G, Almendras MC. Diabe . Diabetic gastroparesis: a gastrointestinal complication underdiagnosed in diabetic neuropathy. Rev Méd-Cient “Luz Vida”. 2011;2(1):46-50.
- Cundulle K, Cedeño S. Neuropatía gastrointestinal diabética. Una revisión de la literatura. Anatomía Digital 2022;5(3.2):34-45.
- Mayor V, et al. Diagnóstico y tratamiento actual de la gastroparesia: una revisión sistemática de la literatura. Rev. colomb. Gastroenterol. 2020;35(4). Disponible en www.scielo.org.co/scielo.php?script=sci_arttext&pid=S0120-995720200 0400471
- Reyes P, Rojs W. Gastroparesia diabética: comparación del vaciamiento gástrico de pacientes tratados con eritromicina o cisaprida. Repertorio de Medicina y Cirugía 2000. Disponible en https://www.fucsalud.edu.co/sites/default/files/2017-01/1_22.pdf
- Parkan M, Hasler W, Fisher R. Asociación Americana de Gastroenterología. Revisión técnica sobre el diagnóstico y tratamiento de la gastroparesia. Gastroenterology 2004;127. Disponible en https://www.medigraphic.com/pdfs/gastro/ge-2005/ge053n.pdf
- Parkman H, Camilleri M, Farrugia G, et al. Gastroparesis and functional dyspepsia: excerpts from the AGA/ANMS meeting. Neurogastroenterol Motil 2010;22.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








