The Rubella Vaccine: Everything You Need to Know

Written and verified by the biologist Samuel Antonio Sánchez Amador
The rubella vaccine is available on the market for purchase and administration, as well as being part of the official schedules of several countries for free administration. The importance of this vaccine is undisputed and it’s therefore key in public health approaches.
Rubella is an infectious disease caused by the rubella virus, a pathogen belonging to the Matonaviridae family. Due to its epidemiological importance, the World Health Organization (WHO) estimates that more than 250 million people are vaccinated against this pathology in the Americas alone.
Although this is an infection that’s usually mild in children and adults, during pregnancy, it poses a considerable risk of miscarriage and fetal death. For this reason, we’re going to tell you what the rubella vaccine is and when and why it’s necessary.
What is rubella?
As we’ve already mentioned, rubella is an infectious disease of viral origin. Several studies show us data that highlight the clinical importance of the disease. Some of them are the following:
- In the epidemic between 1964 and 1965, more than 20,000 children were born with birth defects due to rubella in the United States.
- During the same period, more than 10,000 spontaneous abortions occurred in infected mothers.
- Therefore, the WHO considers this disease to be the leading cause of vaccine-preventable birth defects in children.
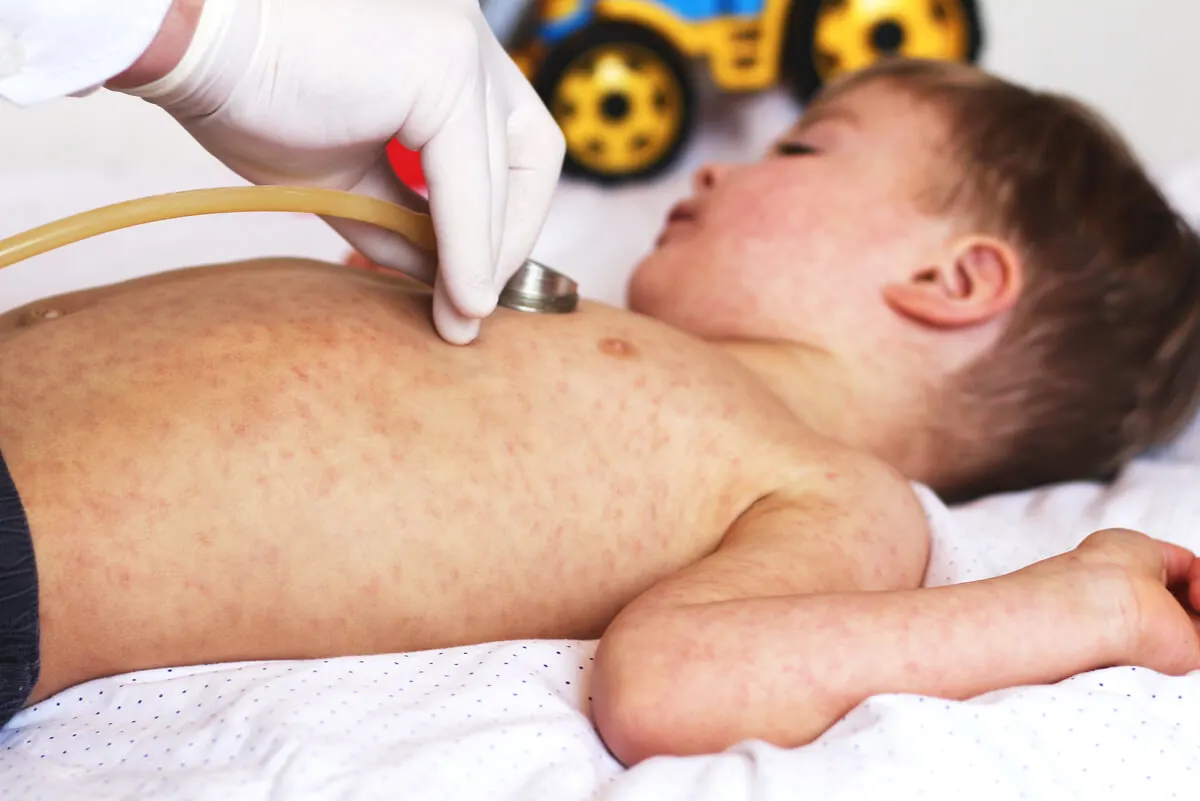
According to the Mayo Clinic, the signs and symptoms of rubella are difficult to diagnose due to their mildness. The patient may experience low-grade fever, rash, nausea, and mild conjunctivitis, although some infected patients don’t even develop any symptoms.
Transmission between adults and infants is through direct contact with the mucous membranes or sputum of the infected individual. On the other hand, it’s transmitted transplacentally from mother to child – that is, through the bloodstream.
We think you may be interested in reading this, too: The HPV Vaccine and Oral Health: How Are They Related?
What vaccines are available for rubella?
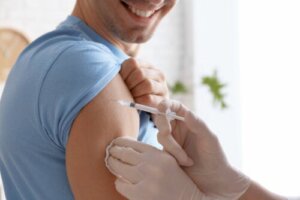
As the Centers for Disease Control and Prevention (CDC) tells us, the rubella vaccine is usually given as part of a combination vaccine called MMR. This MMR or MMR form is a cocktail of three attenuated viral components.
This allows the immune system to prepare for and act effectively against measles, mumps, and rubella. It’s administered by a combined application that often involves multiple injections.
On the other hand, there are also monovalent vaccines – i.e. unique vaccines for this condition alone. In any case, it’s an immunization without serious adverse effects, with an efficacy of 95 % after a single dose.
Who should be vaccinated for rubella?
The organization HealthyChildren organization tells us that the rubella vaccine should be administered during infancy. For the maximum degree of immunity possible, it’s necessary to distribute its dose in two events. These are as follows:
- The first dose: From 12 to 15 months of age.
- The second dose: Four to six years of age.
This is the ideal scenario, but in countries where the health structure is poor, a primary effort is usually made to vaccinate everyone under 40 years of age. If this is not possible, priority should be given to women of childbearing age.
According to WHO records, at least 80% of the population should be immune to rubella so that those who cannot be vaccinated can be indirectly protected. This creates a large non-susceptible group.
Who should not be vaccinated against rubella?
First of all, it’s essential to emphasize that vaccination is a civic obligation on behalf of any healthy individual. It is not a choice, but a responsibility.
Unfortunately, however, there are certain segments of the population that can’t be vaccinated against rubella. The following exceptions are listed in the sources cited above:
- Use of the vaccine should be avoided in persons who have a history of severe allergic reactions to MMR.
- Pregnant women cannot receive the rubella vaccine. It can only be given after the mother gives birth.
- People with a weakened immune system, either from infections such as HIV or from treatments such as chemotherapy, should avoid this type of vaccination.
Other exemptions exist, but vary on a case-by-case basis and are usually transient in nature. Unless otherwise indicated by a medical professional, vaccination against any disease is always the best option.
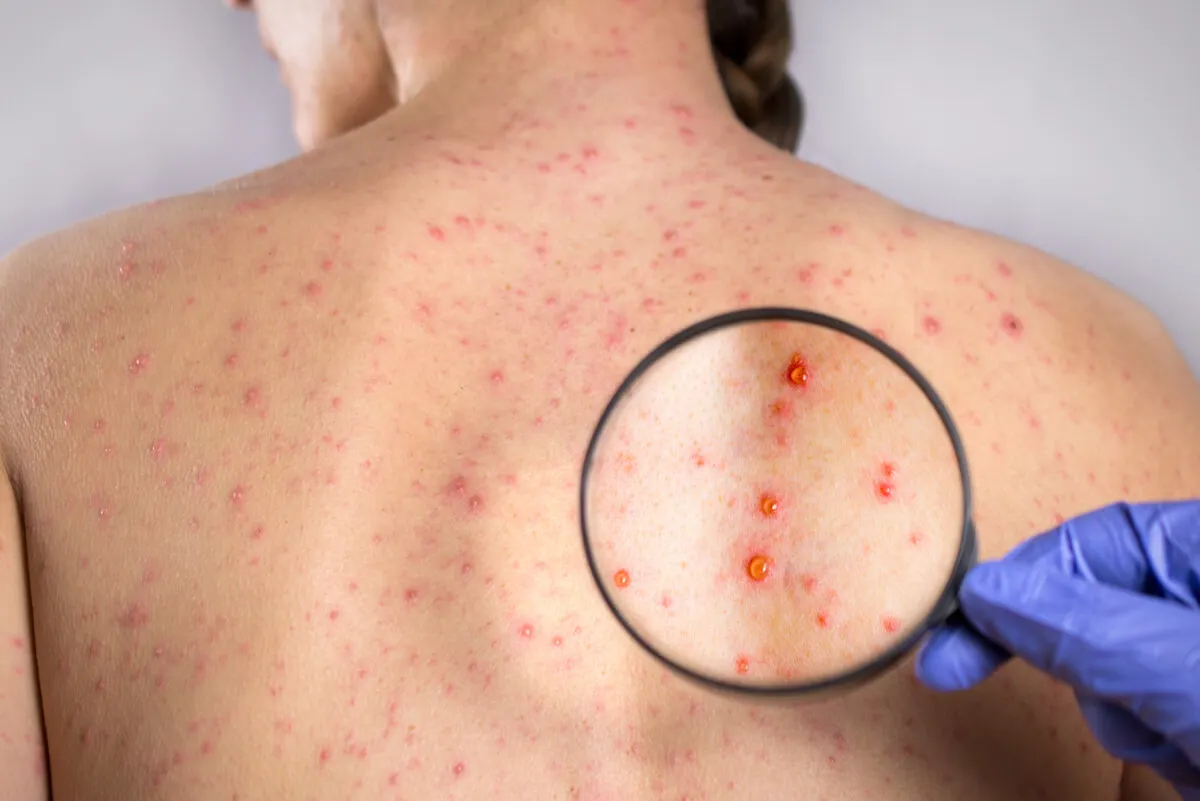
Possible side effects
According to the Spanish Association of Pediatrics (AEP), adverse effects are infrequent and mild. Mild fever or measles may appear 5 to 15 days after vaccination, although this clinical picture resolves on its own.
The patient may also experience coagulation disorders or an episode of swelling. However, these are very rare side effects.
Like this article? You may also like to read: Studies Show Efficacy of Pneumonia Vaccine in Older Adults
The rubella vaccine to protect pregnant women
As we have seen, the MMR vaccine is essential whenever the health of the infant or adult allows it. Thanks to it, the incidence of diseases such as measles has dropped to 1% in societies where the vaccine is widely administered.
Although rubella is a mild infection in children and adults, the fetuses of pregnant women are at serious risk if exposed to the pathogen. Therefore, it’s a civic obligation for all of us to prevent its spread.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Rubeola, Organización Mundial de la Salud (OMS). Recogido a 8 de octubre en https://www.who.int/es/news-room/fact-sheets/detail/rubella
- SUÁREZ-OGNIO, Luis et al. A rubella serosurvey in postpartum women in the three regions of Peru. Rev Panam Salud Pública [en línea]. 2007, v. 22, n. 2
- Rubeola, Mayo Clinic. Recogido a 8 de octubre en https://www.mayoclinic.org/es-es/diseases-conditions/rubella/symptoms-causes/syc-20377310
- Rubeola, CDC. Recogido a 8 de octubre en https://www.cdc.gov/spanish/especialescdc/rubeola/index.html#:~:text=La%20vacuna%20contra%20la%20rub%C3%A9ola%20generalmente%20es%20parte%20de%20una,hace%20m%C3%A1s%20de%2030%20a%C3%B1os.
- Las vacunas contra el sarampión, paperas y rubéola: lo que usted debe saber, Healthychildren.org. Recogido a 8 de octubre en https://www.healthychildren.org/Spanish/safety-prevention/immunizations/Paginas/Measles-Mumps-Rubella-Vaccines-What-You-Need-to-Know.aspx
- González Miranda, Felipe, and Elsa Paulina Abaca Castillo. Actualización clínica y epidemiológica de sarampión, rubéola, parotiditis y vacuna tres vírica en la región de las Américas ya nivel nacional. Diss. Universidad de Talca (Chile). Escuela de Tecnología Médica., 2019.
- Castillo González, William, et al. “Enfoque neuroinmunológico para la evaluación de la vacuna triple vírica contra el sarampión, la parotiditis y la rubéola.” Revista Cubana de Investigaciones Biomédicas 38.3 (2019).
- Mirlesse, V., F. Jacquemard, and F. Daffos. “Rubéola congénita.” EMC-Tratado de Medicina 4.2 (2000): 1-3.
- Weekly epidemiological record Relevé épidémiologique hebdomadaire, OMS. Recogido a 8 de octubre en https://web.archive.org/web/20160304201805/http://www.who.int/wer/2011/wer8629.pdf?ua=1
- VACUNA RUBEOLA, AEP. Recogido a 8 de octubre en https://vacunasaep.org/familias/vacunas-una-a-una/vacuna-rubeola
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








