The Most Common Symptoms of Spondylolisthesis
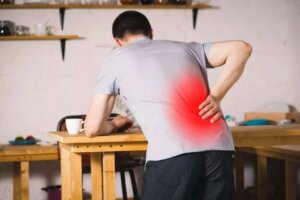
Spondylolisthesis is a condition that refers to the displacement of a vertebra so that it rests directly on the one below. It usually affects people over 40 years old. You might hear the term degenerative, congenital, or isthmic spondylolisthesis. However, the first case is currently the most common.
This term was coined by Newman in 1963 and, currently, there are different treatments depending on the severity of the disease that we’ll explain at the end of this article.
What is spondylolisthesis?
Its symptoms
Normally, spondylolisthesis affects the bones of the lumbar part of the back. There may be cases where the problem occurs in the middle part; however, this isn’t common.
But how can you identify it? Despite the fact that there are different symptoms that can alert you to its presence, it’s important to mention that many patients don’t feel anything.
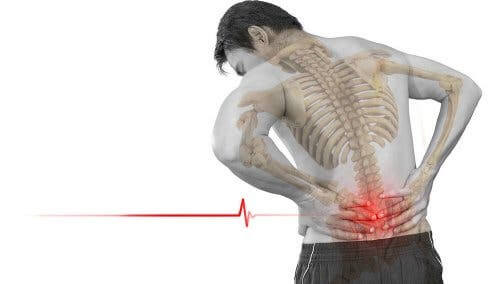
Thus, spondylolisthesis sometimes goes completely unnoticed, gets gradually worse and, many years later, presents more serious symptoms. Let’s take a look at some of the symptoms that some people with spondylolisthesis experience.
- Back pain: This is the most common symptom and appears as if it were a pulled muscle. It’s a sharp pain that spreads throughout the lower back.
- Weakness in the lower limbs: This can cause you to walk with your knees slightly bent and in short steps. It’s normal in these cases to feel tingling and numbness.
- Tense hamstrings: Another symptom of spondylolisthesis is the presence, for no reason, of tension in the back of the thighs. Sometimes it also produces spasms.
- Loss of sphincter control: This is an unusual symptom, but it can occur in some patients. Due to weakness in the lower limbs, sphincter control may be impaired.
Discover: 5 Health Problems that Cause Back Pain
Physical manifestations
The symptoms we mentioned aren’t the only ones that can alert you to the presence of this condition.Here are some other physical symptoms that could be a sign of this condition. Let’s see some examples:
- The abdomen protrudes
- The torso appears shorter
- Curves form in the lower back (sagging)
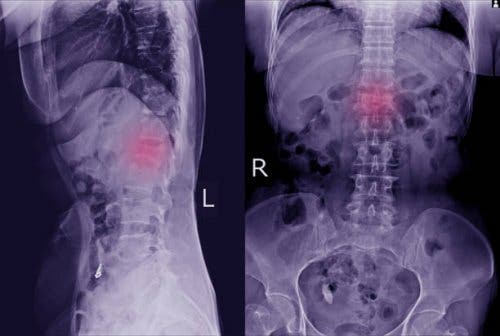
These physical manifestations are easy to overlook. However, paying attention to them will allow you to go to the doctor to perform one of the main tests that will allow their detection: x-rays. That way, it’ll be possible to see clearly if there’s a displaced vertebra.
In some cases, the doctor may require more specific tests, such as a computerized topography or an MRI scan. With these additional tests they can see more clearly if there’s spondylolisthesis and also if it has affected bones and nerves.
You may be interested in: How to Distinguish a Herniated Disc from Common Back Pain
Complications of spondylolisthesis
Despite the symptoms we noted, there are possible complications of this condition that can have serious effects on your quality of life. For example, persistent back pain can lead you to adopt a sedentary lifestyle, and this leads to weight gain.
Likewise, inactivity will only promote the loss of elasticity and muscle strength, as well as bone density.
Another consequence is stiffness. However, one fairly serious complication we should note is the possibility of permanently damaging the nerve that the slipped vertebra is pressing down on.
Despite all this, there are different treatments. The most conservative option is to undergo physiotherapy by strengthening the back area and correcting your posture. In other circumstances, you might need surgery. That way, doctors can put the vertebrae that slipped back in place and they can attach it with screws so that it doesn’t move again.
We recommend that, if you have any discomfort in your back, you should see a doctor immediately, especially if it happens on a daily basis. Likewise, adopting correct posture habits is important to help you avoid, or at least reduce, the presence of these types of problems if they aren’t congenital.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Gelosi, J. F., & Guyot, J. P. (2011). Espondilolistesis de alto grado. Revista de la Asociación Argentina de Ortopedia y Traumatología, 76(4), 330-335.
- Rivas Hernández, Rafael, & Santos Coto, Carlos A.. (2010). Manejo del síndrome doloroso lumbar. Revista Cubana de Medicina General Integral, 26(1) Recuperado en 25 de febrero de 2019, de http://scielo.sld.cu/scielo.php?script=sci_arttext&pid=S0864-21252010000100013&lng=es&tlng=es.
- Vázquez-Aguilar, A, Torres-Gómez, A, Atlitec-Castillo, PT, & León-Martínez, JE De. (2016). Espondilolistesis degenerativa. Influencia del índice de masa corporal en la evolución postquirúrgica. Acta ortopédica mexicana, 30(1), 13-16. Recuperado en 25 de febrero de 2019, de http://www.scielo.org.mx/scielo.php?script=sci_arttext&pid=S2306-41022016000100013&lng=es&tlng=es.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








