The Causes and Symptoms of Hereditary Angioedema


Written and verified by the pharmacist Fabiola Marín Aguilar
Quincke’s edema, angioneurotic edema, or hereditary angioedema is a hereditary genetic disease that causes painful inflammation and edema in the lower layer of the skin, the subcutaneous tissue, the mucous membranes, and even in some viscera.
Sometimes, this genetic disease is life-threatening if it affects the airways. Learn more about the causes and symptoms of hereditary angioedema in this article!
Types of hereditary angioedema
There are two types of hereditary angioedema:
- Type 1 (the most common). Characterized by diminished levels of the C1-inhibitor protein. This protein regulates the inhibition of the complement system in order to prevent spontaneous immune system activation. It’s a bridge between innate and acquired immunity that helps us defend ourselves against infections.
- Type 2. This type causes dysfunctional forms of the C1-inhibitor protein.
The first symptoms of hereditary angioedema usually appear during childhood or adolescence. In older ages, and when patients have an associated disorder, the C1 inhibitor deficiency may be caused by:
- Complement system depletion due to a neoplastic disorder (B-cell lymphoma).
- Antibodies are produced against the C1 inhibitor. This occurs in autoimmune diseases such as systemic lupus erythematosus.
What can trigger hereditary angioedema?
Mild trauma, a viral illness, eating certain foods, stress, and even exposure to cold can trigger this condition.
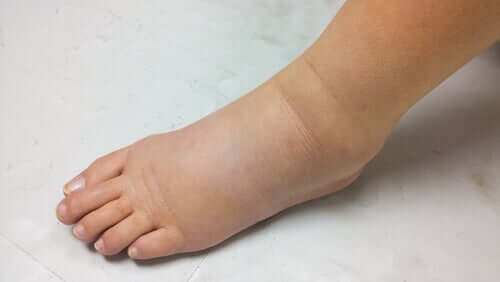
The symptoms of hereditary angioedema
The characteristic symptoms of this condition are very similar to those that appear in other forms of bradykinin-mediated angioedema:
- Asymmetric painful swelling of the face, lips, and tongue
- Swelling on the back of the hands, feet, and genitals
- Bowel obstruction
- Nausea
- Vomiting
- This condition doesn’t cause hives or itching
This article may interest you: How to Treat Hives in Children
Diagnosis
Experts believe that bradykinin, a powerful vasodilator, is responsible for most of the symptoms of hereditary angioedema.
To diagnose the condition, doctors request laboratory tests that measure serum complement levels. For example, the concentrations of C4, inhibitor of C1 and C1q, which is a component of C1:
- Hereditary angioedema (types 1 and 2). Low C4 levels.
- Type 1. Low levels of C1 inhibitor and normal C1q levels.
- Hereditary angioedema type 2. Normal or high C1 inhibitor levels and normal C1q levels.
- Acquired C1 inhibitor deficiency. Low C1q levels.
Therefore, if the swelling isn’t accompanied by hives and recurs with no clear cause, then doctors will suspect hereditary angioedema or acquired C1 inhibitor deficiency.
Read on to learn more: Strengthen Your Immune System with 6 Habits
Treatment
Bradykinin-mediated angioedema is often resistant to standard therapies used to treat other types of angioedema. Epinephrine, glucocorticoids, or antihistamines aren’t effective in these cases.
- For acute life-threatening attacks that compromise the airways, medical professionals intravenously administer human plasma-derived C1 esterase inhibitor concentrate.
- Long-term prevention. Treatment is based on a C1-esterase inhibitor (ecallantide or icatibant). If none of these drugs is available, tranexamic acid is used in the European Union.
- Attenuated androgens (danazol) are also used as a preventive measure. These stimulate the hepatic synthesis of C1 inhibitor.
- In case of surgery, intubation, or a procedure involving trauma to the cervico-facial region, a possible acute attack should be prevented in the short term. Medical professionals usually use C1-esterase inhibitor concentrate thirty minutes before the invasive procedure.
- To relieve symptoms. Some options are pain relievers, antiemetics, and hydration.
Conclusion
Although it isn’t a common condition, hereditary angioedema can compromise the patient’s life if it isn’t diagnosed in time.
The clinical signs and symptoms of this disease can lead people to erroneously suspect that it could be another pathology. Therefore, if you suspect this condition, you should consult a specialist.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Memon RJ, Tiwari V. Angioedema. StatPearls [Internet], 2019. https://www.ncbi.nlm.nih.gov/books/NBK538489/.
- Manual MDS. Versión para profesionales. Angioedema hereditario y adquirido, 2018. https://www.msdmanuals.com/es-es/professional/inmunolog%C3%ADa-y-trastornos-al%C3%A9rgicos/enfermedades-al%C3%A9rgicas,-autoinmunitarias-y-otros-trastornos-por-hipersensibilidad/angioedema-hereditario-y-adquirido.
- Moellman JJ, Bernstein JA, Lindsell C et al. American College of Allergy, Asthma & Immunology (ACAAI). Society for Academic Emergency Medicine (SAEM). A consensus parameter for the evaluation and management of angioedema in the emergency department. Acad Emerg Med. 2014 Apr;21(4):469-84. https://www.ncbi.nlm.nih.gov/pubmed/24730413.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








