Polycythemia Vera: Causes, Symptoms, Diagnosis and Treatment

Reviewed and approved by the doctor Leonardo Biolatto
Red blood cells, or erythrocytes, are cells present in the blood, whose main function is to transport oxygen to the tissues. In this sense, when there are alterations in their number, such as with polycythemia vera, it can cause serious consequences.
Polycythemia vera is a neoplasm of the bone marrow, which causes an increase in the production of red blood cells. Other blood cells, such as platelets and leukocytes, may also be affected, but to a lesser extent.
The increased number of red blood cells makes the blood thicker, which explains the occurrence of long-term complications. Unfortunately, it’s a chronic disease, which is diagnosed many years after its onset, especially in people over 40 years of age.
Symptoms
The disease is asymptomatic in most cases, so people don’t know they have the disorder. Symptoms may be absent or very mild during the first few years.
The most characteristic symptoms appear when the number of red blood cells increases blood viscosity considerably. Among the main signs reported by people with polycythemia vera are the following:
- Loss of weight
- Blurred or double vision
- Headaches and dizziness
- Joint pain and swelling
- Difficulty breathing when lying down
- Redness of the face, hands and feet
- Itching or stinging, especially after a shower
- Tingling, numbness, or burning in the extremities
On the other hand, some studies state that up to 70% of people with polycythemia vera have splenomegaly or spleen enlargement. The spleen is the organ in charge of eliminating erythrocytes, and so it can increase in size if these changes occur.

You may be interested in: Oncological Blood Tests: What Are They and When Are They Done?
Causes of polycythemia vera
The main cause of the disorder is a genetic mutation in a specific gene that can occur at any time in life. The mutation responsible arises from unknown causes and isn’t inherited.
Multiple studies link polycythemia vera to an alteration in the JAK2 tyrosine kinase gene. The mutation occurs in a specific area, called exon 14, in up to 96% of cases. However, other sections may be affected, such as exon 12.
Nevertheless, some patients with polycythemia vera don’t have any mutation in this gene. Because of this, it’s a disease that may be idiopathic.
Risk factors
Anyone can be prone to the disease at some point in their lives. However, polycythemia vera tends to affect some population groups more frequently, and so there are risk factors.
The main ones are being male and being over 50 years old. However, it’s important to bear in mind that women and young people can also suffer from this condition.
Read also: 5 Most Common Diseases in Old Age
Possible complications
The complications of polycythemia vera appear as a result of an increase in blood viscosity. One of the main consequences is the formation of blood clots. Blood clots can obstruct the flow to organs such as the heart, brain, or lungs.
People may also develop gastrointestinal ulcers, due to the increased number of red blood cells. In addition, inflammation and joint pain are very common in this pathology.
Polycythemia vera can lead to other bone marrow disorders, such as myelofibrosis or replacement of the bone marrow with scar tissue. Myelofibrosis will cause a decrease in the production of blood cells, which can lead to anemia. In addition, some people with the disease develop acute myeloid leukemia.
Diagnosis of polycythemia vera
The diagnosis of the disease is made by chance in most cases, during a random blood test. Elevated erythrocyte levels are diagnostic, even if hemoglobin and hematocrit are normal.
The physician may also ask for a blood cell count to evaluate leukocyte and platelet levels, as well as the presence of low concentrations of a hormone called erythropoietin.
Specialists should use multiple laboratory tests to rule out the presence of other pathologies that may explain the blood abnormalities. A bone marrow biopsy may demonstrate increased red blood cell production. Finally, the presence of characteristic genetic changes should be looked for.
Treatment
Unfortunately, there’s no definitive cure for polycythemia vera. However, the therapeutic options available can alleviate the symptomatology presented by individuals and improve quality of life.
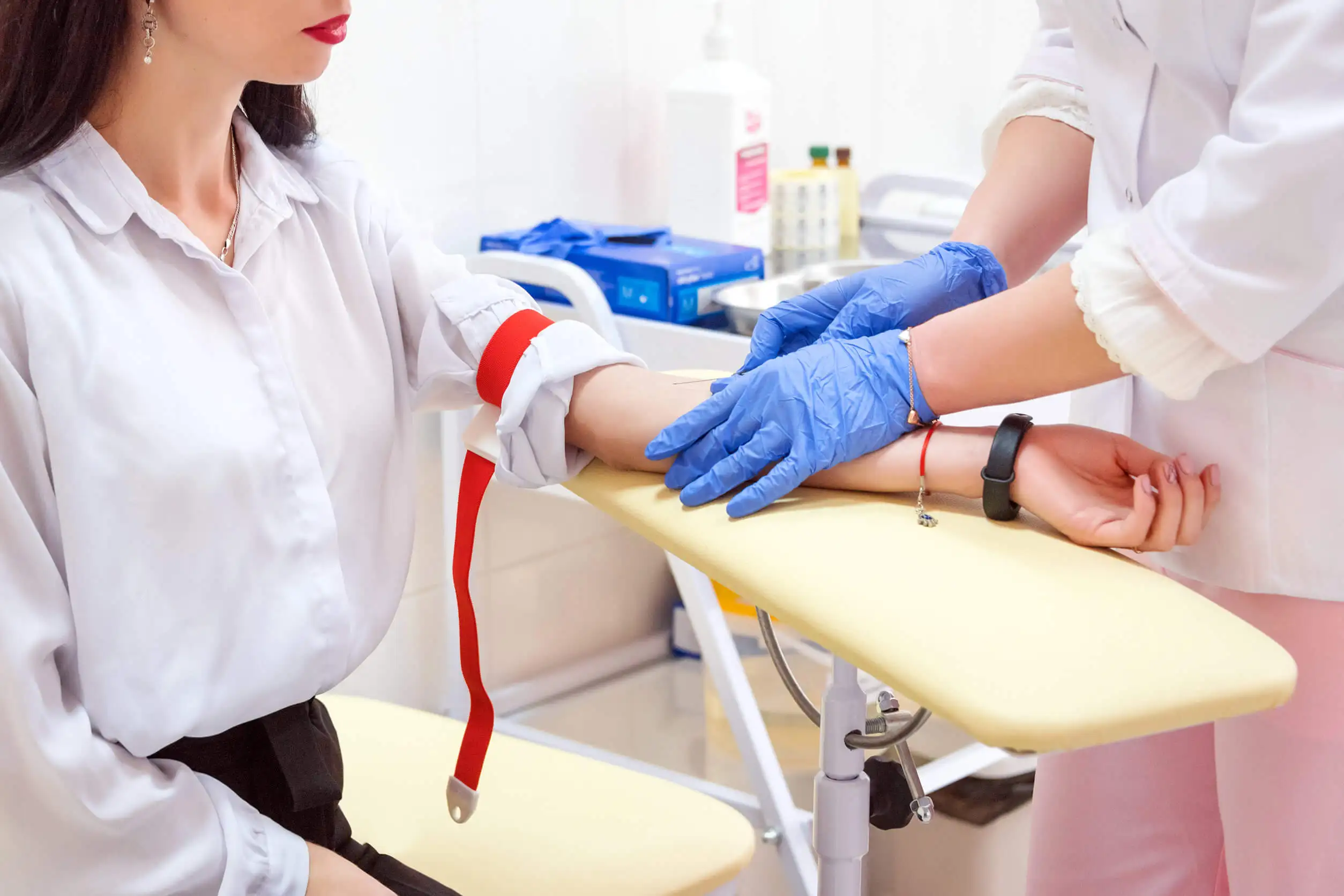
The main treatment available for the disease is a technique called phlebotomy. This consists of the insertion of a needle into a large caliber vein in order to extract varying amounts of blood. The extraction decreases volemia, the number of erythrocytes, and blood viscosity.
Phlebotomy should be performed periodically, although the frequency will depend on the severity of the condition. On the other hand, there are many drugs capable of decreasing red blood cell production. The use of these compounds offers favorable results, but they must be consumed under strict medical supervision.
Some symptoms, such as pruritus, can be very bothersome. In these cases, health personnel recommend antihistamines. Finally, some people should take low doses of aspirin to avoid blood clots.
How to live with polycythemia vera
The prognosis for people with polycythemia vera is good, provided they comply with their treatment properly. Life expectancy after diagnosis usually exceeds 20 years in most cases.
Living with any chronic disease is a real challenge for those who suffer from it and for their families.
People with polycythemia vera can follow some recommendations to improve their quality of life and reduce the impact of the disease. Among the recommended changes are the following:
- Not smoking
- Drinking plenty of fluids
- Avoiding cold and intense heat
- Taking cold or lukewarm baths
- Increasing the use of skin creams
- Exercising regularly, taking care of the possibility of traumatism
A chronic disease with serious consequences
Polycythemia vera is a pathology characterized by an increase in the number of red blood cells. The main cause is a specific genetic mutation, although there are also predisposing risk factors.
This pathology can produce fatal complications when not properly treated, so diagnosis and timely treatment are essential. In this sense, it’s important to see a physician in the presence of any abnormal symptomatology.
All cited sources were thoroughly reviewed by our team to ensure their quality, reliability, currency, and validity. The bibliography of this article was considered reliable and of academic or scientific accuracy.
- Correa Saavedra M, Ruiz Mejía C. Policitemia vera: presentación clínica, diagnóstico y nuevos abordajes terapéuticos. Archivos de Medicina (Manizales). 2018;18(2):421-431.
- Fernandez N, Fundora T, Macías I. Policitemia Vera. Experiencias en el diagnóstico y tratamiento en el Instituto de Hematología e Inmunología. Revista Cubana de Hematología Inmunología y Hemoterapia 2011:27(1)77-90.
- Fox S, Griffin L, Robinson Harris D. Polycythemia Vera: Rapid Evidence Review. Am Fam Physician. 2021 Jun 1;103(11):680-687.
- Silva-Vera M, Jiménez-González MJ, Moreno-Pérez NE, Moreno-Pizarro E, Máximo-Galicia P. Policitemia vera y neutropenia severa. Hematol Méx. 2020; 21 (3): 153-157.
- Spivak JL. How I treat polycythemia vera. Blood. 2019 Jul 25;134(4):341-352.
- Tremblay D, Mascarenhas J. Novel Therapies in Polycythemia Vera. Curr Hematol Malig Rep. 2020 Apr;15(2):133-140.
This text is provided for informational purposes only and does not replace consultation with a professional. If in doubt, consult your specialist.








